Abstract
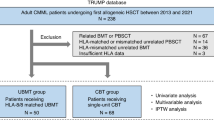
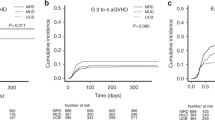
Cord blood transplantation (CBT) is an alternative donor transplantation method and has the advantages of rapid availability and the possibility of inducing a more potent graft-versus-leukemia effect, leading to a lower relapse rate for patients with non-remission relapse and refractory acute myeloid leukemia (R/R AML). This study aimed to investigate the impact of CBT, compared to human leukocyte antigen-matched related donor transplantation (MRDT). This study included 2451 adult patients with non-remission R/R AML who received CBT (1738 patients) or MRDT (713 patients) between January 2009 and December 2018. Five-year progression-free survival (PFS) and the prognostic impact of CBT were evaluated using a propensity score (PS) matching analysis. After PS matching, the patient characteristics were well balanced between the groups. The five-year PFS was 25.2% (95% confidence interval [CI]: 21.2–29.5%) in the CBT group and 18.1% (95% CI: 14.5–22.0%) in the MRDT group (P = 0.009). The adjusted hazard ratio (HR) was 0.83 (95% CI: 0.69–1.00, P = 0.045); this was due to a more pronounced decrease in the relapse rate (HR: 0.78, 95% CI: 0.69–0.89, P < 0.001) than an increase in the NRM (1.42, 1.15–1.76, P = 0.001). In this population, CBT was associated with a better 5-year PFS than MRDT after allogeneic HSCT.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
DeWolf SE, Tallman MS. How I treat relapsed or refractory AML. Blood. 2020. https://doi.org/10.1182/blood.2019001982.
Döhner H, Weisdorf DJ, Bloomfield CD. Acute myeloid leukemia. N Engl J Med. 2015;373:1136–52.
Wattad M, Weber D, Döhner K, Krauter J, Gaidzik VI, Paschka P, et al. Impact of salvage regimens on response and overall survival in acute myeloid leukemia with induction failure. Leukemia. 2017;31:1306–13.
Nagler A, Savani BN, Labopin M, Polge E, Passweg J, Finke J, et al. Outcomes after use of two standard ablative regimens in patients with refractory acute myeloid leukaemia: a retrospective, multicentre, registry analysis. Lancet Haematol. 2015;2:e384–392.
Brissot E, Labopin M, Ehninger G, Stelljes M, Brecht A, Ganser A, et al. Haploidentical versus unrelated allogeneic stem cell transplantation for relapsed/refractory acute myeloid leukemia: a report on 1578 patients from the Acute Leukemia Working Party of the EBMT. Haematologica. 2019;104:524–32.
Brissot E, Labopin M, Stelljes M, Ehninger G, Schwerdtfeger R, Finke J, et al. Comparison of matched sibling donors versus unrelated donors in allogeneic stem cell transplantation for primary refractory acute myeloid leukemia: a study on behalf of the Acute Leukemia Working Party of the EBMT. J Hematol Oncol. 2017;10:130.
Baron F, Labopin M, Ruggeri A, Ehninger G, Bonifazi F, Stelljes M, et al. Umbilical cord blood versus unrelated donor transplantation in adults with primary refractory or relapsed acute myeloid leukemia: a report from Eurocord, the Acute Leukemia Working Party and the Cord Blood Committee of the Cellular Therapy and Immunobiology Working Party of the EBMT. Blood Cancer J. 2019;9:46.
Konuma T, Kato S, Ooi J, Oiwa-Monna M, Ebihara Y, Mochizuki S, et al. Single-unit cord blood transplantation after granulocyte colony-stimulating factor–combined myeloablative conditioning for myeloid malignancies not in remission. Biol Blood Marrow Transpl. 2014;20:396–401.
Ballen KK, Lazarus H. Cord blood transplant for acute myeloid leukaemia. Br J Haematol. 2016;173:25–36.
Dholaria B, Savani BN, Hamilton BK, Oran B, Liu HD, Tallman MS, et al. Hematopoietic cell transplantation in the treatment of newly diagnosed adult acute myeloid leukemia: an evidence-based review from the American Society of Transplantation and Cellular Therapy. Transpl Cell Ther. 2021;27:6–20.
Milano F, Gooley T, Wood B, Woolfrey A, Flowers ME, Doney K, et al. Cord-blood transplantation in patients with minimal residual disease. N Engl J Med. 2016;375:944–53.
Barker JN, Kurtzberg J, Ballen K, Boo M, Brunstein C, Cutler C, et al. Optimal practices in unrelated donor cord blood transplantation for hematologic malignancies. Biol Blood Marrow Transpl. 2017;23:882–96.
Brunstein CG, Fuchs EJ, Carter SL, Karanes C, Costa LJ, Wu J, et al. Alternative donor transplantation after reduced intensity conditioning: results of parallel phase 2 trials using partially HLA-mismatched related bone marrow or unrelated double umbilical cord blood grafts. Blood. 2011;118:282–8.
Chen Y-B, Aldridge J, Kim HT, Ballen KK, Cutler C, Kao G, et al. Reduced-intensity conditioning stem cell transplantation: comparison of double umbilical cord blood and unrelated donor grafts. Biol Blood Marrow Transpl. 2012;18:805–12.
Sharma P, Purev E, Haverkos B, Pollyea DA, Cherry E, Kamdar M, et al. Adult cord blood transplant results in comparable overall survival and improved GRFS vs matched related transplant. Blood Adv. 2020;4:2227–35.
Sorror ML, Maris MB, Storb R, Baron F, Sandmaier BM, Maloney DG, et al. Hematopoietic cell transplantation (HCT)-specific comorbidity index: a new tool for risk assessment before allogeneic HCT. Blood. 2005;106:2912–9.
Giralt S, Ballen K, Rizzo D, Bacigalupo A, Horowitz M, Pasquini M, et al. Reduced-intensity conditioning regimen workshop: defining the dose spectrum. Report of a workshop convened by the center for international blood and marrow transplant research. J Am Soc Blood Marrow Transpl. 2009;15:367–9.
Bacigalupo A, Ballen K, Rizzo D, Giralt S, Lazarus H, Ho V, et al. Defining the intensity of conditioning regimens: working definitions. J Am Soc Blood Marrow Transpl. 2009;15:1628–33.
Austin PC. The performance of different propensity score methods for estimating marginal hazard ratios. Stat Med. 2013;32:2837–49.
Breems DA, Van Putten WLJ, Huijgens PC, Ossenkoppele GJ, Verhoef GEG, Verdonck LF, et al. Prognostic index for adult patients with acute myeloid leukemia in first relapse. J Am Soc Clin Oncol. 2005;23:1969–78.
Chevallier P, Labopin M, Turlure P, Prebet T, Pigneux A, Hunault M, et al. A new Leukemia Prognostic Scoring System for refractory/relapsed adult acute myelogeneous leukaemia patients: a GOELAMS study. Leukemia. 2011;25:939–44.
Duval M, Klein JP, He W, Cahn J-Y, Cairo M, Camitta BM, et al. Hematopoietic stem-cell transplantation for acute leukemia in relapse or primary induction failure. J Am Soc Clin Oncol. 2010;28:3730–8.
Battipaglia G, Ruggeri A, Labopin M, Volin L, Blaise D, Socié G, et al. Refined graft-versus-host disease/relapse-free survival in transplant from HLA-identical related or unrelated donors in acute myeloid leukemia. Bone Marrow Transpl. 2018;53:1295–303.
Davies SM, Kollman C, Anasetti C, Antin JH, Gajewski J, Casper JT, et al. Engraftment and survival after unrelated-donor bone marrow transplantation: a report from the national marrow donor program. Blood. 2000;96:4096–102.
Akpek G, Pasquini MC, Logan B, Agovi M-A, Lazarus HM, Marks DI, et al. Effects of spleen status on early outcomes after hematopoietic cell transplantation. Bone Marrow Transpl. 2013;48:825–31.
Sullivan KM, Agura E, Anasetti C, Appelbaum F, Badger C, Bearman S, et al. Chronic graft-versus-host disease and other late complications of bone marrow transplantation. Semin Hematol. 1991;28:250–9.
Przepiorka D, Weisdorf D, Martin P, Klingemann HG, Beatty P, Hows J, et al. 1994 consensus conference on acute gVHD grading. Bone Marrow Transpl. 1995;15:825–8.
Kanda J, Hayashi H, Ruggeri A, Kimura F, Volt F, Takahashi S, et al. Prognostic factors for adult single cord blood transplantation among European and Japanese populations: the Eurocord/ALWP-EBMT and JSHCT/JDCHCT collaborative study. Leukemia. 2020;34:128–37.
Shouval R, Fein JA, Labopin M, Kröger N, Duarte RF, Bader P, et al. Outcomes of allogeneic haematopoietic stem cell transplantation from HLA-matched and alternative donors: a European Society for Blood and Marrow Transplantation registry retrospective analysis. Lancet Haematol. 2019;6:e573–e584.
Yanada M, Konuma T, Yamasaki S, Kuwatsuka Y, Masuko M, Tanaka M, et al. Time-varying effects of graft type on outcomes for patients with acute myeloid leukemia undergoing allogeneic hematopoietic cell transplantation. Biol Blood Marrow Transpl. 2020;26:307–15.
Liu H, Sun Z, Geng L, Wang X, Ding K, Tong J, et al. Similar survival, but better quality of life after myeloablative transplantation using unrelated cord blood vs matched sibling donors in adults with hematologic malignancies. Bone Marrow Transpl. 2014;49:1063–9.
Tong J, Xuan L, Sun Y, Huang D, Liu H, Zheng C, et al. Umbilical cord blood transplantation without antithymocyte globulin results in similar survival but better quality of life compared with unrelated peripheral blood stem cell transplantation for the treatment of acute leukemia—a retrospective study in China. Biol Blood Marrow Transpl. 2017;23:1541–8.
Mehta RS, Holtan SG, Wang T, Hemmer MT, Spellman SR, Arora M, et al. Composite GRFS and CRFS outcomes after adult alternative donor HCT. J Clin Oncol. 2020;38:2062–76.
Inamoto Y, Kimura F, Kanda J, Sugita J, Ikegame K, Nakasone H, et al. Comparison of graft-versus-host disease-free, relapse-free survival according to a variety of graft sources: antithymocyte globulin and single cord blood provide favorable outcomes in some subgroups. Haematologica. 2016;101:1592–602.
Miyawaki S. JSH guideline for tumors of hematopoietic and lymphoid tissues: leukemia 1. Acute myeloid leukemia (AML). Int J Hematol. 2017;106:310–25.
Labopin M, Ruggeri A, Gorin NC, Gluckman E, Blaise D, Mannone L, et al. Cost-effectiveness and clinical outcomes of double versus single cord blood transplantation in adults with acute leukemia in France. Haematologica 2014;99:535–40.
Preussler JM, Denzen EM, Majhail NS. Costs and cost-effectiveness of hematopoietic cell transplantation. J Am Soc Blood Marrow Transpl 2012;18:1620–8.
Kiernan J, Damien P, Monaghan M, Shorr R, McIntyre L, Fergusson D, et al. Clinical studies of ex vivo expansion to accelerate engraftment after umbilical cord blood transplantation: a systematic review. Transfus Med Rev. 2017;31:173–82.
Wagner JE, Brunstein CG, Boitano AE, DeFor TE, McKenna D, Sumstad D, et al. Phase I/II trial of StemRegenin-1 expanded umbilical cord blood hematopoietic stem cells supports testing as a stand-alone graft. Cell Stem Cell. 2016;18:144–55.
Horwitz ME, Wease S, Blackwell B, Valcarcel D, Frassoni F, Boelens JJ, et al. Phase I/II study of stem-cell transplantation using a single cord blood unit expanded ex vivo with nicotinamide. J Am Soc Clin Oncol. 2019;37:367–74.
Acknowledgements
The authors thank all the physicians and data managers of the centers, who contributed to the collection of data on transplantation for the Japanese Data Center for Hematopoietic Cell Transplantation and the Transplant Registry Unified Management Program 2. We would like to express our gratitude to the Japan Society of Clinical Research for their support.
Author information
Authors and Affiliations
Contributions
YS designed the study, analyzed the data, performed the statistical analysis, and wrote the first draft of the manuscript. TS, SH, TK, SM, JK, TF, KK and MY critically reviewed the manuscript and analyzed data. All the other authors contributed to data collection. All authors approved the final version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Shimomura, Y., Sobue, T., Hirabayashi, S. et al. Comparing cord blood transplantation and matched related donor transplantation in non-remission acute myeloid leukemia. Leukemia 36, 1132–1138 (2022). https://doi.org/10.1038/s41375-021-01474-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41375-021-01474-0
This article is cited by
-
Updated comparable efficacy of cord blood transplantation for chronic myelomonocytic leukaemia: a nationwide study
Bone Marrow Transplantation (2024)
-
Different effects of thymoglobulin on acute leukemia with pre-transplant residual blasts in HLA mismatch transplantation
International Journal of Hematology (2023)
-
Unrelated cord blood transplantation vs. HLA-matched sibling transplantation for adults with B-cell acute lymphoblastic leukemia in complete remission: superior OS for patients with long-term survival
Stem Cell Research & Therapy (2022)
-
Improved trends in survival and engraftment after single cord blood transplantation for adult acute myeloid leukemia
Blood Cancer Journal (2022)