Abstract
Natural killer/T-cell lymphoma (NKTL) is a sub-type of Epstein–Barr virus (EBV)-related non-Hodgkin lymphomas common in Asia and Latin America but rare elsewhere. Its pathogenesis is complex and incompletely understood. Lymphoma cells are transformed from NK- or T-cells, sometimes both. EBV-infection and subsequent genetic alterations in infected cells are central to NKTL development. Hemophagocytic syndrome is a common complication. Accurate staging is important to predict outcomes but there is controversy which system is best. More than two-thirds of NKTL lympohmas are localized at diagnosis, are frequently treated with radiation therapy only and have 5-year survival of about 70 percent. Persons with advanced NKTLs receive radiation therapy synchronously or metachronously with diverse multi-drug chemotherapy typically including l-asparginase with 5-year survival of about 40 percent. Some persons with widespread NKTL receive chemotherapy only. There are few data on safety and efficacy of high-dose therapy and a haematopoietic cell autotransplant. Immune therapies, histone deacetylase (HDAC)-inhibitors and other drugs are in early clinical trials. There are few randomized controlled clinical trials in NKTLs and no therapy strategy is clearly best; more effective therapy(ies) are needed. Some consensus recommendations are not convincingly evidence-based. Mechanisms of multi-drug resistance are considered. We discuss these issues including recent advances in our understanding of and therapy of NKTLs.
Similar content being viewed by others
Introduction
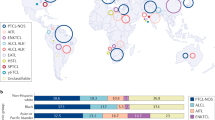
Natural killer/T-cell lymphoma (NKTL), an Epstein–Barr virus (EBV) associated lympho-proliferative disease, accounts for <2 percent of T-cell lymphomas. It develops from transformation of natural killer (NK)-cells or cytotoxic T-cells, rarely both. NKTL is relatively common in Asia and, to lesser extent, in Latin America, but rare in Europe and North America. NKTLs can be nodal (nNKTL) or extra-nodal (eNKTL), forms which differ substantially in clinical, patho-physiological and genetic features [1,2,3].
In 2016 WHO scheme NKTLs are classified as EBV-associated T- and NK-cell lympho-proliferative diseases [4]. Most eNKTLs occur in the nasal cavity and are termed nasal-type eNKTL but can occur at any site. Localized NKTL is curable but most persons with advanced disease have a poor prognosis [5,6,7].
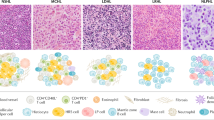
Diagnosis of NKTL depends on histology including T- and/or NK-cells expressing CD3ε, granzyme B, perforin, TIA1, and EBV [8]. Cytogenetic abnormalities include del(6), del(8) and del(14). Commonly mutated genes include TP53, DDX3X, STAT3, JAK3, MGA, BCOR, ECSIT, and MCL1 [9, 10].
Several prognostic and predictive models of NKTLs are proposed including International Prognostic Index (IPI), Korean Prognostic Index (KPI), Prognostic Index of Natural Killer Lymphoma (PINK), and Nomogram-revised Risk Index (NRI). None is sufficiently accurate to predict outcomes at the patient level [11,12,13,14].
Localized NKTL is often treated with radiation therapy with 5-year survival of about 70% [5]. Advanced and recurrent NKTLs are typically treated with radiation therapy and multi-drug chemotherapy regimens including l-asparaginase with 5-year survival only about 40% [7]. High-dose therapy and autologous hematopoietic cell transplants are sometimes used but mostly ineffective and better therapies are needed [15, 16]. Immune therapies directed against NKTL-associated targets such as immune checkpoint inhibitors, anti-CD30 and -CD38 monoclonal antibodies and against EBV-related targets are increasingly used [17,18,19,20]. We use a question-and-answer format to summarize major issues in the biology and therapy of NKTLs.
Why the geographic diversity of NKTLs?
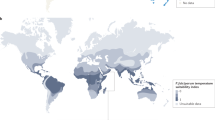
NKTL is relatively common in Asia and Latin America compared with Europe and North America [21,22,23]. Why is incompletely understood but important considerations include EBV type and genetic susceptibility, probably both [24,25,26,27,28].
EBV is divided into two major strains or clades, EBV strain or type -1 and EBV strain or type-2 which have different EBNA-2 and -3A, 3B, and 3C genes with different transforming and reactivation activities [29, 30]. EBV type-1 is dominant globally [30,31,32,33]. EBV starin-1 is common in NKTLs compared with EBV strain-2 [25, 34]. These data mean geographic differences in EBV type prevalences only partly explain differences in geographic incidences of NKTLs. Several other EBV strains and inter-starin viruses have been isolated from human cancers, especially nasopharyngeal cancinomas, and lymphomas including NKTLs. EBV strains associated with nasopharyngeal cancinomas include GD1, GD2, HKNPC1, C666-1, and M81 [29, 35,36,37,38,39,40]. whereas EBV viruses associated with Burkitt lymphoma include AG876, Akata, and Mutue [29, 41,42,43,44].
Many EBV strains identified in different geographic areas differ mainly in LMP1 genes [29, 34]. The Asian EBV strains were isolated from samples in East and South Asia and clearly differ from strains from other parts of the world [29]. Recent phylogenetic analyses indicate EBV genomes sequenced from Asians with NKTL are closer to the Asian than non-Asian strains indicating an association between Asian strains and NKTL and a potential explanation of the geographic diversity of NKTLs [29, 45].
Genomic analyses indicate several variants of EBV derived from NKTLs [38, 46, 47]. The frequent single nucleotide variant was located at BPLE1 gene [47]. A 30 base pair deletion in EBV LMP1 gene C terminus region was common and associated with oncogenicity of EBV strain-2 in NKTLs [30, 46, 48]. Transcriptome analyses indicate differential expression of latent and lytic genes and variations of T-cell epitopes in EBV strains from NKTLs suggesting some specific EBV variants are more likely to cause NKTL [47].
Studies on race-related genetic predisposition to NKTL have been done in east Asia [28, 49]. Bei et al. reported correlations between the HLADPB1 rs9277378 single nucleotide polymorphism locus and immune response to EBV-infection and likelihood of developing NKTL [49]. These authors also reported different IL18RAP rs13015714 genotypes promote cell proliferation and are associated with developing NKTL [28]. Another association with developing NKTL is rs9271588 at GRCh38 38.1/142 [28]. More studies of genetic predisposition to NKTL are needed.
Are NK/T-cell lymphomas T- or NK-cell cancers or both?
NK- and T-cells derive from the same lymphoid progenitor cell which develops into different lineages because of expression of different transcription factors [50]. Most NKTLs originate in NK-cells with germline T-cell receptor (TCR) genes [1]. Rarely, NKTLs arise in T-cells with rearranged TCR genes. A study of 67 subjects with NKTL reported more than two-thirds of cases were of NK-cell origin [51]. NK-cells express perforin, granzyme B, TIA1, CD2, cytoplasmic CD3ε, and CD56, expressed in most extra-nodal NKTLs [8, 52]. Granzyme B, TIA1, CD2, CD56 are also sometimes expressed in T-cell-derived cases. However, TCR protein is only expressed in T-cell cases [51, 53]. Del(14q11.2) is a potential indicator of a T-cell origin of nodal NKTLs [2, 54]. NKTLs of NK-cell origin often have STAT3, DDX3X mutations whereas those of T-cell origin often have TP53 and EPHA1 mutations [9]. Clinical features and therapy response of NK- and T-cell origin NKTLs are similar [4, 51, 53, 54]. Nodal NKTLs are included into EBV-positive variant of peripheral T-cell lymphoma not otherwise specified (NOS) [3].
What is the most accurate NKTL staging system?
The Ann Arbor staging system is the most widely used for staging NKTL. Although useful for planning radiation therapy it fails to consider the prognostic impact of certain anatomical sites such as the aero-digestive tract, local invasion, and regional lymph node involvement [55].
The TNM staging system is based on a single-center study of anthracycline chemotherapy in persons with nasal NKTL. Although it emphasizes the prognostic impact of regional lymph node involvement it is not intended for extra-nasal NKTLs and is not validated in persons receiving l-asparaginase therapy [56].
The Chinese Southwest Oncology Group and Asia Lymphoma Study Group ENKTL (CA) staging system considers site, local invasion, regional lymph node involvement and metastasis and is validated in persons receiving l-asparaginase [13]. This system seems more accurate than others in estimating survival and operates under different therapies. Table 1 summarizes the details of the CA system. Other co-variates which may improve the accuracy of staging systems include measures of circulating EBV-DNA and positron emission tomography/computed tomography scanning [5, 57,58,59].
Which is the best survival prognostic/predictive model?
The IPI, KPI, and the PINK are the most widely used NKTL prognostic and/or predictive models. Accuracy of the IPI was confirmed in many studies of low-and high-grade lymphomas including studies which included l-asparaginase therapy but accuracy in NKTL is controversial [11]. Although most persons with stage-I/-II NKTL are classified as low-risk in the IPI some have a poor prognosis [12, 60].
Accuracy of the KPI model is validated in persons receiving l-asparginase. However, there is no preditive discrimaination between persons in the IPI low- and low-intermediate risk cohorts or between persons in the IPI high-intermediate and high-risk cohorts [60]. A multi-variable Cox regression analyses which included local invasion and the KPI reported local invasion was a better survival predictor than the KPI only [12]. An important limitation is the IPI and KPI models were developed before l-asparginase was widely used [60, 61]. In contrast, the PINK model was developed and validated in persons receiving l-asparginase-based therapy and more accurately identifies prognoses of persons in the same risk cohorts in the IPI and KPI models but is also far from accurate [13, 62].
Li et al. used Ann Arbor stage, age, Eastern Cooperative Oncology Group performance score, lactate dehydrogenase (LDH) and local invasion to develop a predictive nomogram and NRI for NKTL [14, 63]. The NRI is more accurate compared with the IPI, KPI, or PINK models [14]. These models are compared in Table 2.
What is the best therapy of early-stage NKTL?
Data from 2 recent retrospective studies indicate radiation therapy alone is effective therapy of early-stage NKTL with no benefit of adding chemotherapy. In these studies outcomes with different therapies were compared using a propensity score-matched analysis [6, 64]. Subjects in the low-risk cohort had favorable outcomes with radiation therapy alone with 5-year survival of about 90 percent [6, 64, 65]. Similar data are reported for subjects staged using the CA system [13]. Others suggest risk-adapted therapy for early-stage NKTL where chemotherapy is given only persons with an adverse prognosis despite being low-risk [5,65,66,67].
What is the best therapy of advanced NKTL?
There are consensus persons with advanced NKTL benefit from combined radiation therapy and chemotherapy. For example, in a study using the NRI subjects in the intermediate-/high-risk cohorts benefited from combined radiation therapy and chemotherapy compared with radiation therapy only with 5-year survivals of about 75% versus 60% [6, 65, 68].
Similar data are reported for subjects staged using the CA system [13]. The conclusion adding chemotherapy to radiation benefits intermediate/high stage subjects are not from a randomized controlled trial and should be viewed cautiously.
Combined therapy can be given synchronously or given metachronously in either order [5]. In the synchronous format radiation therapy is given with reduced doses of DeVIC (dexamethasone, etoposide, ifosfamide, and carboplatin), ESHAP (etoposide, dexamethasone, high-dose cytarabine, and cisplatin), or DEP (dexamethasone, etoposide, and cisplatin) [69,70,71,72]. Also, radiation therapy can be given with weekly cisplatin followed by VIPD (etoposide, ifosfamide, cisplatin, and dexamethasone) or VIDL (etoposide, ifosfamide, dexamethasone, and l-asparaginase) [73, 74]. Data from metachronous format include DDGP (pegaspargase, gemcitabine, cisplatin, and dexamethasone) followed by radiation therapy with little toxicity [75]. SMILE (dexamethasone, methotrexate, ifosfamide, l-asparaginase, and etoposide) followed by radiation therapy is also effective [7]. Another metachronous format is to sandwich radiation between chemotherapy courses. Examples include MESA (methotrexate, etoposide, dexamethasone, and pegaspargase) followed by radiation and radiation therapy combined with GELOX (gemcitabine, l-asparaginase and oxaliplatin) or PGEMOX (gemcitabine, pegaspargase, and oxaliplatin) [76,77,78].
Persons with widespread NKTL are sometimes receive chemotherapy only. Most trials had few, selected subjects with wide confidence intervals precluding critical interpretation or comparison. Regimens tested included SMILE, PEMD (pegylated-L-asparginase, etoposide, methotrexate, and dexamethasone), AspaMetDex (l-asparaginase, methotrexate, and dexamethasone), PGEMOX, and GDP (gemcitabine, dexamethasone, and cisplatin) [79,80,81,82,83]. A randomized controlled trial compared outcomes of DDGP and SMILE. DDGP had better survival with less severe adverse events [84]. These regimens are displayed in Table 3. SMILE, PGEMOX, and DDGP are recommended in the NCCN guidelines with AspaMetDex is recommended for persons unable to tolerate intensive therapy [16].
Most data we cite for therapy of advanced NKTL are from retrospective or uncontrolled studies and report similar outcomes with synchronous and metachronous therapy and with diverse radiation therapy and chemotherapy regimens, formats, schedules etc [54, 85, 86]. There are also a myriad of radiation therapy doses, fields, and schedules. The many formats for radiation therapy and diverse chemotherapy regimens suggest no convincing data any strategy is best. Curiously, the NCCN guidelines recommend radiation therapy combined with DeVIC, VIPD, modified SMILE, or PGEMOX [16]. We think this recommendation is not evidence-based and should be viewed cautiously.
Is there a role for high-dose therapy and a haematopoietic cell autotransplant in NKTL?
There are several small studies of high-dose chemotherapy followed by a haematopoietic cell autotransplant in persons with advanced NKTL. The largest included 31 subjects receiving an autotransplant as initial therapy. 3-year progression-free survival (PFS) and survival were 40% (95% Confidence Interval [CI], 22, 58%) and 52% (34, 71%) [87]. The largest retrospective study in subjects from Western countries reported comparable survival to Asian subjects with 2-year PFS of 33% (13, 84%) and survival of 40% (19, 86%) [15]. These data are largely uninterpretable because of huge confidence intervals. A multi-center phase-2 study evaluated VIDL followed by an autotrasplant in 27 subjects with advance NKTL. 8 of 17 responders after induction chemotherapy maintained a complete remission posttransplant but there were no controls [88]. These limited data from uncontrolled clinical trials provide no basis for recommending or not recommending autotransplants in advanced NKTL and are displayed in Table 4. Surprisingly, NCCN guidelines recommend haematopoietic cell_transplants for persons with advanced NKTL in complete remission or a biopsy-negative partial remission after first-line therapies. This recommendation seems based on few, data and is unconvincing.
What is the mechanism of multi-drug resistance (MDR) in NKTL?
Most NKTLs express MDR1 which encodes the P-glycoprotein which mediates cell efflux of doxorubicin and vincristine from cells and may explain resistance of NKTLs to anthracycline-based therapy [89]. Response rates of MDR1-negative subjects to CHOP (cyclophosphamide, doxorubicin, vincristine, and prednisone) is significantly higher than those MDR1-positive in 1 study but not others [90]. Interleukin-13 (IL-13) and ABCC4 are highly expressed in NKTLs and also contributes to doxorubicin resistance [91]. Wang et al. reported a higher concentration of IL-2 receptors α (IL-2R α) on NKTL cell lines compared with normal NK-cells [92]. Over-expression of IL-2R α is associated with resistance to killing by gemcitabine, doxorubicin, and l-asparaginase. MYC expression promotes expression of SNHG12, the small nucleolar RNA host gene 12 of long non-coding RNAs which mediates resistance of NKTL cells to cisplatin [93]. Clinical translation of these data are lacking.
Why is NKTL prone to hemophagocytic syndrome (HPS)?
HPS is an immune-mediated syndrome characterized by systemic activation of macrophages resulting in a hyper-inflammatory response and widespread tissue and organ damage. HPS is classified as primary or secondary. People with haematopoietic cancers, especially NKTLs, are at risk to develop secondary HPS. NKTL and HPS are associated with EBV infection [94]. In persons with EBV-associated NKTL TNF-α expression is increased activating monocyte/macrophage phagocytosis and cytokine secretion. ECSITT419C is common in NKTL [10]. A mutation in ECSIT, ECSITV140A combines with the S100A8/S100A9 hetero-dimer which promotes stable binding of arachidonic acid to S100A9 and contributes to the assembly of NADPH oxidase followed by activation of NF-κB pathway. These steps promote secretion of TNF-α and IFN-γ which activate macrophages and precipitate cytokine storm resulting in secondary HPS. Also, persons with advanced NKTL have high interleukin-18 (IL-18) concentrations which also correlate with high TNF-α and IFN-γ concentrations and are associated with lymphoma-associated hemophagocytic syndrome (LAHPS) [95]. One study reported bone marrow infiltration, hepato-splenomegaly, and high LDH levels were risk factors for LAHPS. The incidence of LAHPS in people with two or three risk factors was >60 percent [96].
Is there a role for immune therapy of NKTL?
PD-L1 is expressed frequently on NKTL cells and is associated with poor prognosis making anti-PD-L1/PD-1 antibodies an attractive therapy [19, 97]. Pembrolizumab is reported effective in persons with advanced NKTL and there are encouraging results with nivolumab [98,99,100,101]. Other active drugs include sintilimab, CS-001, and avelumab [102,103,104,105]. These data are summarized in Table 5. Although pembrolizumab and nivolumab are recommended in the NCCN guidelines for advanced NKTL the strength of evidence is weak and they should probably only be used in the context of a clinical trial [16].
CD38 and CD30 are expressed in about one-half of NKTLs [106, 107]. There is a case report of efficacy of daratumumab, an anti-CD38 antibody, in advanced NKTL [108]. Preliminary safety and efficacy data are also reported from a multi-center phase-2 study (NCT02927925) [18]. Another study claimed efficacy of brentuximab vedotin, an anti-CD30 antibody, in 2 subjects [109, 110]. A phase-2 study of 7 subjects reported responses [17]. These data without controls are insufficient to comment critically on safety and efficacy of this approach and it should be used only in the context of clinical trials.
EBV-infection is associated with NKTLs and provides a therapy target. In one study 10 subjects in complete remission after diverse therapies received autologous cytotoxic T-cells against EBV latent membrane protein (LMP)-1/-2a with encouraging results. However, controls were lacking [20]. Kim et al. reported responses in four subjects with advanced NKTL receiving autologous EBV-specific T-cells [111]. Transfusing allogeneic EBV-specific T-cells from donors was reported to improve survival in persons at high risk of relapse compared with historical cohorts [112]. These few data and absent controls preclude critical analyses of safety and efficacy and suggest use only in the context of a clinical trial.
Are histone deacetylase (HDAC)-inhibitors active in NKTL?
Chidamide, a selective inhibitor of HDAC1, 2, 3, and 10 was tested in a phase-2 study in 16 subjects with advanced NKTL. Three responded with one complete remission [113]. In another study subjects with advanced NKTL received chidamide only (N = 19) or with chemotherapy (N = 18). Responses were reported in five subjects receiving chidamide only and eight receiving combined therapy [114]. A phase-2 study reported data of 15 subjects with advanced NKTL receiving chidamide with 6 responders [115]. There were 21 responders among 37 subjects with advanced NKTL receiving chidamide in a phase 1b/−2 study [116]. Another study reported a response in a subject with advanced NKTL receiving panobinostat with bortezomib [117]. Other HDAC-inhibitors such as romidepsin and belinostat were used in phase-2 trials with too few subjects to comment critically [118,119,120,121,122]. Other data suggest vorinostat and valproic acid are active against NKTL cells in vitro and in animal models [123, 124]. Studies of HDAC-inhibitors are displayed in Table 6. These few data and absent controls preclude critical analyses of safety and efficacy and suggest use only in the context of a clinical trial.
Conclusion
There is substantial recent progress in understanding the biology of NKTLs combined with modest therapy advances. Staging and predictive and prognostic scoring models have improved but greater accuracy and precision are needed. Risk-adapted therapy is proposed but unvalidated. Radiation therapy has proved effective in localized NKTL whereas l-asparaginase based chemotherapy is effective in persons with advanced disease. No therapy format is proved best and randomized controlled trials are lacking. New therapy strategies including immune and targeted therapies are advancing in clinical trials. Progress, but more is needed.
References
Tse E, Kwong Y-L. Diagnosis and management of extranodal NK/T cell lymphoma nasal type. Expert Rev Hematol. 2016;9:861–71.
Ng S-B, Chung T-H, Kato S, Nakamura S, Takahashi E, Ko Y-H, et al. Epstein-Barr virus-associated primary nodal T/NK-cell lymphoma shows a distinct molecular signature and copy number changes. Haematologica. 2018;103:278–87.
Jeon YK, Kim J-H, Sung J-Y, Han JH, Ko Y-H. Epstein-Barr virus-positive nodal T/NK-cell lymphoma: an analysis of 15 cases with distinct clinicopathological features. Hum Pathol. 2015;46:981–90.
Swerdlow SH, Campo E, Pileri SA, Harris NL, Stein H, Siebert R, et al. The 2016 revision of the World Health Organization classification of lymphoid neoplasms. Blood. 2016;127:2375–90.
Kim SJ, Yoon SE, Kim WS. Treatment of localized extranodal NK/T cell lymphoma, nasal type: a systematic review. J Hematol Oncol. 2018;11:140.
Yang Y, Zhu Y, Cao J-Z, Zhang Y-J, Xu L-M, Yuan Z-Y, et al. Risk-adapted therapy for early-stage extranodal nasal-type NK/T-cell lymphoma: analysis from a multicenter study. Blood 2015;126:1424–32.
Kwong Y-L, Kim WS, Lim ST, Kim SJ, Tang T, Tse E, et al. SMILE for natural killer/T-cell lymphoma: analysis of safety and efficacy from the Asia Lymphoma Study Group. Blood. 2012;120:2973–80.
Hue SS-S, Oon ML, Wang S, Tan S-Y, Ng S-B. Epstein-Barr virus-associated T- and NK-cell lymphoproliferative diseases: an update and diagnostic approach. Pathology. 2020;52:111–27.
Xiong J, Cui B-W, Wang N, Dai Y-T, Zhang H, Wang C-F, et al. Genomic and transcriptomic characterization of natural killer T cell lymphoma. Cancer Cell. 2020;37:403–419.e6.
Wen H, Ma H, Cai Q, Lin S, Lei X, He B, et al. Recurrent ECSIT mutation encoding V140A triggers hyperinflammation and promotes hemophagocytic syndrome in extranodal NK/T cell lymphoma. Nat Med. 2018;24:154–64.
Chim C-S, Ma S-Y, Au W-Y, Choy C, Lie AKW, Liang R, et al. Primary nasal natural killer cell lymphoma: long-term treatment outcome and relationship with the International Prognostic Index. Blood. 2004;103:216–21.
Wang L, Xia Z-j, Huang H-q, Lu Y, Zhang Y-j. Cyclophosphamide, doxorubicin, vincristine, and prednisone (CHOP) in the treatment of stage IE/IIE extranodal natural killer/T cell lymphoma, nasal type: 13-year follow-up in 135 patients. Int J Hematol. 2012;96:617–23.
Hong H, Li Y, Lim ST, Liang C, Huang H, Yi P, et al. A proposal for a new staging system for extranodal natural killer T-cell lymphoma: a multicenter study from China and Asia Lymphoma Study Group. Leukemia. 2020;34:2243–8.
Chen S-Y, Yang Y, Qi S-N, Wang Y, Hu C, He X, et al. Validation of nomogram-revised risk index and comparison with other models for extranodal nasal-type NK/T-cell lymphoma in the modern chemotherapy era: indication for prognostication and clinical decision-making. Leukemia. 2020;35:130–42.
Fox CP, Boumendil A, Schmitz N, Finel H, Luan JJ, Sucak G, et al. High-dose therapy and autologous stem cell transplantation for extra-nodal NK/T lymphoma in patients from the Western hemisphere: a study from the European Society for Blood and Marrow Transplantation. Leuk Lymphoma. 2015;56:3295–3300.
NCCN Guidelines T-Cell Lymphomas Version 1.2021. https://www.nccn.org/professionals/physician_gls/pdf/t-cell.pdf. Accessed 24 Nov 2020.
Kim SJ, Yoon DH, Kim JS, Kang HJ, Lee HW, Eom H-S, et al. Efficacy of brentuximab vedotin in relapsed or refractory high-CD30-expressing non-Hodgkin lymphomas: results of a multicenter, open-labeled phase II trial. Cancer Res Treat: Off J Korean Cancer Assoc. 2020;52:374–87.
Huang H-q, Kim W-S, Yao M, Kim TM, Yoon D, Cho S-G, et al. Daratumumab monotherapy for patients with relapsed or refractory (R/R) natural killer/T-cell lymphoma (NKTCL), nasal type: updated results from an open-label, single-arm, multicenter phase 2 study. Blood. 2019;134:1568–1568.
Nagato T, Ohkuri T, Ohara K, Hirata Y, Kishibe K, Komabayashi Y, et al. Programmed death-ligand 1 and its soluble form are highly expressed in nasal natural killer/T-cell lymphoma: a potential rationale for immunotherapy. Cancer Immunol Immunother. 2017;66:877–90.
Cho S-G, Kim N, Sohn H-J, Lee SK, Oh ST, Lee H-J, et al. Long-term outcome of extranodal NK/T cell lymphoma patients treated with postremission therapy using EBV LMP1 and LMP2a-specific CTLs. Mol Ther. 2015;23:1401–9.
Lima M. Aggressive mature natural killer cell neoplasms: from epidemiology to diagnosis. Orphanet J Rare Dis. 2013;8:95.
Aozasa K, Ohsawa M, Tajima K, Sasaki R, Maeda H, Matsunaga T, et al. Nation-wide study of lethal mid-line granuloma in Japan: frequencies of Wegener’s granulomatosis, polymorphic reticulosis, malignant lymphoma and other related conditions. Int J Cancer. 1989;44:63–66.
Quintanilla-Martínez L, Lome-Maldonado C, Ott G, Gschwendtner A, Gredler E, Angeles-Angeles A, et al. Primary intestinal non-Hodgkin’s lymphoma and Epstein-Barr virus: high frequency of EBV-infection in T-cell lymphomas of Mexican origin. Leuk Lymphoma. 1998;30:111–21.
Midgley RS, Bell AI, Yao QY, Croom-Carter D, Hislop AD, Whitney BM, et al. HLA-A11-restricted epitope polymorphism among Epstein-Barr virus strains in the highly HLA-A11-positive Chinese population: incidence and immunogenicity of variant epitope sequences. J Virol. 2003;77:11507–16.
Gualco G, Domeny-Duarte P, Chioato L, Barber G, Natkunam Y, Bacchi CE. Clinicopathologic and molecular features of 122 Brazilian cases of nodal and extranodal NK/T-cell lymphoma, nasal type, with EBV subtyping analysis. Am J Surg Pathol. 2011;35:1195–203.
Montes-Mojarro IA, Chen B-J, Ramirez-Ibarguen AF, Quezada-Fiallos CM, Pérez-Báez WB, Dueñas D, et al. Mutational profile and EBV strains of extranodal NK/T-cell lymphoma, nasal type in Latin America. Mod Pathol. 2020;33:781–91.
Saleem A, Natkunam Y. Extranodal NK/T-Cell Lymphomas: The Role of Natural Killer Cells and EBV in Lymphomagenesis. Int J Mol Sci. 2020;21:1501.
Lin G-W, Xu C, Chen K, Huang H-Q, Chen J, Song B, et al. Genetic risk of extranodal natural killer T-cell lymphoma: a genome-wide association study in multiple populations. Lancet Oncol. 2020;21:306–16.
Palser AL, Grayson NE, White RE, Corton C, Correia S, Ba Abdullah MM, et al. Genome diversity of Epstein-Barr virus from multiple tumor types and normal infection. J Virol. 2015;89:5222–37.
Montes-Mojarro IA, Fend F, Quintanilla-Martinez L EBV and the Pathogenesis of NK/T Cell Lymphoma. Cancers. 2021;13:1414.
Correa RM, Fellner MD, Alonio LV, Durand K, Teyssié AR, Picconi MA. Epstein-Barr virus (EBV) in healthy carriers: distribution of genotypes and 30 bp deletion in latent membrane protein-1 (LMP-1) oncogene. J Med Virol. 2004;73:583–8.
Neves M, Marinho-Dias J, Ribeiro J, Esteves M, Maltez E, Baldaque I, et al. Characterization of Epstein-Barr virus strains and LMP1-deletion variants in Portugal. J Med Virol. 2015;87:1382–8.
Halabi MA, Jaccard A, Moulinas R, Bahri R, Al Mouhammad H, Mammari N, et al. Clonal deleted latent membrane protein 1 variants of Epstein-Barr virus are predominant in European extranodal NK/T lymphomas and disappear during successful treatment. Int J Cancer. 2016;139:793–802.
Kanda T, Yajima M, Ikuta K. Epstein-Barr virus strain variation and cancer. Cancer Sci. 2019;110:1132–9.
Zeng MS, Li DJ, Liu QL, Song LB, Li MZ, Zhang RH, et al. Genomic sequence analysis of Epstein-Barr virus strain GD1 from a nasopharyngeal carcinoma patient. J Virol. 2005;79:15323–30.
Liu P, Fang X, Feng Z, Guo YM, Peng RJ, Liu T, et al. Direct sequencing and characterization of a clinical isolate of Epstein-Barr virus from nasopharyngeal carcinoma tissue by using next-generation sequencing technology. J Virol. 2011;85:11291–9.
Tsai MH, Raykova A, Klinke O, Bernhardt K, Gärtner K, Leung CS, et al. Spontaneous lytic replication and epitheliotropism define an Epstein-Barr virus strain found in carcinomas. Cell Rep. 2013;5:458–70.
Neves M, Marinho-Dias J, Ribeiro J, Sousa H. Epstein-Barr virus strains and variations: geographic or disease-specific variants? J Med Virol. 2017;89:373–87.
Feederle R, Klinke O, Kutikhin A, Poirey R, Tsai MH, Delecluse HJ. Epstein-Barr Virus: from the detection of sequence polymorphisms to the recognition of viral types. Curr Top Microbiol Immunol. 2015;390:119–48.
Depledge DP, Palser AL, Watson SJ, Lai IY, Gray ER, Grant P, et al. Specific capture and whole-genome sequencing of viruses from clinical samples. PLoS ONE. 2011;6:e27805.
Dolan A, Addison C, Gatherer D, Davison AJ, McGeoch DJ. The genome of Epstein-Barr virus type 2 strain AG876. Virology. 2006;350:164–70.
Lin Z, Wang X, Strong MJ, Concha M, Baddoo M, Xu G, et al. Whole-genome sequencing of the Akata and Mutu Epstein-Barr virus strains. J Virol. 2013;87:1172–82.
Kwok H, Wu CW, Palser AL, Kellam P, Sham PC, Kwong DL, et al. Genomic diversity of Epstein-Barr virus genomes isolated from primary nasopharyngeal carcinoma biopsy samples. J Virol. 2014;88:10662–72.
Lei H, Li T, Li B, Tsai S, Biggar RJ, Nkrumah F, et al. Epstein-Barr virus from Burkitt Lymphoma biopsies from Africa and South America share novel LMP-1 promoter and gene variations. Sci Rep. 2015;5:16706.
Lin N, Ku W, Song Y, Zhu J, Lu Z. Genome-wide analysis of Epstein-Barr virus isolated from extranodal NK/T-cell lymphoma, nasal type. Oncologist. 2019;24:e905–13.
Chiang AK, Wong KY, Liang AC, Srivastava G. Comparative analysis of Epstein-Barr virus gene polymorphisms in nasal T/NK-cell lymphomas and normal nasal tissues: implications on virus strain selection in malignancy. Int J Cancer. 1999;80:356–64.
Peng R-J, Han B-W, Cai Q-Q, Zuo X-Y, Xia T, Chen J-R, et al. Genomic and transcriptomic landscapes of Epstein-Barr virus in extranodal natural killer T-cell lymphoma. Leukemia. 2019;33:1451–62.
Quintanilla-Martinez L, Franklin JL, Guerrero I, Krenacs L, Naresh KN, Rama-Rao C, et al. Histological and immunophenotypic profile of nasal NK/T cell lymphomas from Peru: high prevalence of p53 overexpression. Hum Pathol. 1999;30:849–55.
Li Z, Xia Y, Feng L-N, Chen J-R, Li H-M, Cui J, et al. Genetic risk of extranodal natural killer T-cell lymphoma: a genome-wide association study. Lancet Oncol. 2016;17:1240–7.
Sun JC, Lanier LL. NK cell development, homeostasis and function: parallels with CD8+ T cells. Nat Rev Immunol. 2011;11:645–57.
Pongpruttipan T, Sukpanichnant S, Assanasen T, Wannakrairot P, Boonsakan P, Kanoksil W, et al. Extranodal NK/T-cell lymphoma, nasal type, includes cases of natural killer cell and αβ, γδ, and αβ/γδ T-cell origin: a comprehensive clinicopathologic and phenotypic study. Am J Surg Pathol. 2012;36:481–99.
Parham P. MHC class I molecules and KIRs in human history, health and survival. Nat Rev Immunol. 2005;5:201–14.
Jhuang J-Y, Chang S-T, Weng S-F, Pan S-T, Chu P-Y, Hsieh P-P, et al. Extranodal natural killer/T-cell lymphoma, nasal type in Taiwan: a relatively higher frequency of T-cell lineage and poor survival for extranasal tumors. Hum Pathol. 2015;46:313–21.
Tse E, Kwong Y-L. The diagnosis and management of NK/T-cell lymphomas. J Hematol Oncol. 2017;10:85.
Kim TM, Park YH, Lee S-Y, Kim J-H, Kim D-W, Im S-A, et al. Local tumor invasiveness is more predictive of survival than International Prognostic Index in stage I(E)/II(E) extranodal NK/T-cell lymphoma, nasal type. Blood. 2005;106:3785–90.
Yan Z, Huang H-q, Wang X-x, Gao Y, Zhang Y-j, Bai B, et al. A TNM staging system for nasal NK/T-cell lymphoma. PLoS ONE. 2015;10:e0130984.
Kwong YL, Pang AWK, Leung AYH, Chim CS, Tse E. Quantification of circulating Epstein-Barr virus DNA in NK/T-cell lymphoma treated with the SMILE protocol: diagnostic and prognostic significance. Leukemia. 2014;28:865–70.
Kim SJ, Choi JY, Hyun SH, Ki C-S, Oh D, Ahn YC, et al. Risk stratification on the basis of Deauville score on PET-CT and the presence of Epstein-Barr virus DNA after completion of primary treatment for extranodal natural killer/T-cell lymphoma, nasal type: a multicentre, retrospective analysis. Lancet Haematol. 2015;2:e66–e74.
Tse E, Kwong Y-L. Nasal NK/T-cell lymphoma: RT, CT, or both. Blood. 2015;126:1400–1.
Lee J, Suh C, Park YH, Ko YH, Bang SM, Lee JH, et al. Extranodal natural killer T-cell lymphoma, nasal-type: a prognostic model from a retrospective multicenter study. J Clin Oncol. 2006;24:612–8.
International Non-Hodgkin’s Lymphoma Prognostic Factors Project. A predictive model for aggressive non-Hodgkin’s lymphoma. N. Engl J Med. 1993;329:987–94.
Kim SJ, Yoon DH, Jaccard A, Chng WJ, Lim ST, Hong H, et al. A prognostic index for natural killer cell lymphoma after non-anthracycline-based treatment: a multicentre, retrospective analysis. Lancet Oncol. 2016;17:389–400.
Yang Y, Zhang YJ, Zhu Y, Cao JZ, Yuan ZY, Xu LM, et al. Prognostic nomogram for overall survival in previously untreated patients with extranodal NK/T-cell lymphoma, nasal-type: a multicenter study. Leukemia. 2015;29:1571–7.
Liu X, Wu T, Zhu S-Y, Shi M, Su H, Wang Y, et al. Risk-Dependent Conditional Survival and Failure Hazard After Radiotherapy for Early-Stage Extranodal Natural Killer/T-Cell Lymphoma. JAMA Netw Open. 2019;2:e190194.
Qi S-N, Yang Y, Zhang Y-J, Huang H-Q, Wang Y, He X, et al. Risk-based, Response-adapted Therapy for Early-stage Extranodal Nasal-type NK/T-cell Lymphoma in the Modern Chemotherapy Era: A China Lymphoma Collaborative Group (CLCG) Study. Am J Hematol. 2020;95:1047–56.
Li YX, Yao B, Jin J, Wang WH, Liu YP, Song YW, et al. Radiotherapy as primary treatment for stage IE and IIE nasal natural killer/T-cell lymphoma. J Clin Oncol. 2006;24:181–9.
Kim GE, Cho JH, Yang WI, Chung EJ, Suh CO, Park KR, et al. Angiocentric lymphoma of the head and neck: patterns of systemic failure after radiation treatment. J Clin Oncol. 2000;18:54–63.
Qi F, Chen B, Wang J, Lin X, Qi S, Yang J, et al. Upfront radiation is essential for high-risk early-stage extranodal NK/T-cell lymphoma, nasal type: comparison of two sequential treatment modalities combining radiotherapy and GDP (gemcitabine, dexamethasone, and cisplatin) in the modern era. Leuk Lymphoma. 2019;60:2679–88.
Yamaguchi M, Tobinai K, Oguchi M, Ishizuka N, Kobayashi Y, Isobe Y, et al. Phase I/II study of concurrent chemoradiotherapy for localized nasal natural killer/T-cell lymphoma: Japan Clinical Oncology Group Study JCOG0211. J Clin Oncol. 2009;27:5594–5600.
Yamaguchi M, Tobinai K, Oguchi M, Ishizuka N, Kobayashi Y, Isobe Y, et al. Concurrent chemoradiotherapy for localized nasal natural killer/T-cell lymphoma: an updated analysis of the Japan clinical oncology group study JCOG0211. J Clin Oncol. 2012;30:4044–6.
Michot J-M, Mazeron R, Danu A, Lazarovici J, Ghez D, Antosikova A, et al. Concurrent Etoposide, Steroid, High-dose Ara-C and Platinum chemotherapy with radiation therapy in localised extranodal natural killer (NK)/T-cell lymphoma, nasal type. Eur J Cancer. 2015;51:2386–95.
Tsai H-J, Lin S-F, Chen C-C, Chen T-Y, Su W-C, Hwang W-L, et al. Long-term results of a phase II trial with frontline concurrent chemoradiotherapy followed by consolidation chemotherapy for localized nasal natural killer/T-cell lymphoma. Eur J Haematol. 2015;94:130–7.
Kim SJ, Kim K, Kim BS, Kim CY, Suh C, Huh J, et al. Phase II trial of concurrent radiation and weekly cisplatin followed by VIPD chemotherapy in newly diagnosed, stage IE to IIE, nasal, extranodal NK/T-Cell Lymphoma: Consortium for Improving Survival of Lymphoma study. J Clin Oncol. 2009;27:6027–32.
Kim SJ, Yang D-H, Kim JS, Kwak J-Y, Eom H-S, Hong DS, et al. Concurrent chemoradiotherapy followed by L-asparaginase-containing chemotherapy, VIDL, for localized nasal extranodal NK/T cell lymphoma: CISL08-01 phase II study. Ann Hematol. 2014;93:1895–901.
Zhang L, Wang Y, Li X, Li L, Wang X, Sun Z, et al. Radiotherapy vs sequential pegaspargase, gemcitabine, cisplatin and dexamethasone and radiotherapy in newly diagnosed early natural killer/T-cell lymphoma: A randomized, controlled, open-label, multicenter study. Int J Cancer. 2021;148:1470–7.
Xu PP, Xiong J, Cheng S, Zhao X, Wang CF, Cai G, et al. A phase II study of methotrexate, etoposide, dexamethasone and pegaspargase sandwiched with radiotherapy in the treatment of newly diagnosed, stage IE to IIE extranodal natural-killer/T-cell lymphoma, nasal-type. EBioMedicine. 2017;25:41–49.
Wang L, Wang Z-h, Chen X-q, Li Y-j, Wang K-f, Xia Y-f, et al. First-line combination of gemcitabine, oxaliplatin, and L-asparaginase (GELOX) followed by involved-field radiation therapy for patients with stage IE/IIE extranodal natural killer/T-cell lymphoma. Cancer. 2013;119:348–55.
Wang L, Wang Z-H, Chen X-Q, Wang K-F, Huang H-Q, Xia Z-J. First-line combination of GELOX followed by radiation therapy for patients with stage IE/IIE ENKTL: An updated analysis with long-term follow-up. Oncol Lett. 2015;10:1036–40.
Yamaguchi M, Kwong Y-L, Kim WS, Maeda Y, Hashimoto C, Suh C, et al. Phase II study of SMILE chemotherapy for newly diagnosed stage IV, relapsed, or refractory extranodal natural killer (NK)/T-cell lymphoma, nasal type: the NK-Cell Tumor Study Group study. J Clin Oncol. 2011;29:4410–6.
Liang JH, Wang L, Peter Gale R, Wu W, Xia Y, Fan L, et al. Efficacy of pegaspargase, etoposide, methotrexate and dexamethasone in newly diagnosed advanced-stage extra-nodal natural killer/T-cell lymphoma with the analysis of the prognosis of whole blood EBV-DNA. Blood Cancer J. 2017;7:e608.
Jaccard A, Gachard N, Marin B, Rogez S, Audrain M, Suarez F, et al. Efficacy of L-asparaginase with methotrexate and dexamethasone (AspaMetDex regimen) in patients with refractory or relapsing extranodal NK/T-cell lymphoma, a phase 2 study. Blood. 2011;117:1834–9.
Wang J-H, Wang L, Liu C-C, Xia Z-J, Huang H-Q, Lin T-Y, et al. Efficacy of combined gemcitabine, oxaliplatin and pegaspargase (P-gemox regimen) in patients with newly diagnosed advanced-stage or relapsed/refractory extranodal NK/T-cell lymphoma. Oncotarget. 2016;7:29092–101.
Wang J-J, Dong M, He X-H, Li Y-X, Wang W-H, Liu P, et al. GDP (gemcitabine, dexamethasone, and cisplatin) is highly effective and well-tolerated for newly diagnosed stage IV and relapsed/refractory extranodal natural killer/T-cell lymphoma, nasal type. Medicine. 2016;95:e2787.
Li X, Cui Y, Sun Z, Zhang L, Li L, Wang X, et al. DDGP versus SMILE in newly diagnosed advanced natural killer/T-cell lymphoma: a randomized controlled, multicenter, open-label study in China. Clin Cancer Res. 2016;22:5223–8.
Kwong YL, Kim SJ, Tse E, Oh SY, Kwak JY, Eom HS, et al. Sequential chemotherapy/radiotherapy was comparable with concurrent chemoradiotherapy for stage I/II NK/T-cell lymphoma. Ann Oncol. 2018;29:256–63.
Li J, Li Y, Zhong M, Liu W, Liu X, Li J, et al. A multicenter retrospective comparison of sequential versus sandwich chemoradiotherapy for stage IE-IIE extranodal natural killer/T-cell lymphoma, nasal type. J Cancer. 2018;9:1598–606.
Yhim HY, Kim JS, Mun YC, Moon JH, Chae YS, Park Y, et al. Clinical outcomes and prognostic factors of up-front autologous stem cell transplantation in patients with extranodal natural killer/T cell lymphoma. Biol Blood Marrow Transpl. 2015;21:1597–604.
Song GY, Yoon DH, Suh C, Moon JH, Baek DW, Kim JS, et al. Open-label, single arm, multicenter phase II study of VIDL induction chemotherapy followed by upfront autologous stem cell transplantation in patients with advanced stage extranodal NK/T-cell lymphoma. Bone Marrow Transplant. 2021;56:1205–8.
Yamaguchi M, Kita K, Miwa H, Nishii K, Oka K, Ohno T, et al. Frequent expression of P-glycoprotein/MDR1 by nasal T-cell lymphoma cells. Cancer. 1995;76:2351–6.
Kim GE, Yang W-I, Lee S-W, Rha SY, Chung HC, Kim JH, et al. Lack of correlation between P-glycoprotein and chemotherapy resistance in nasal NK/T-cell lymphomas. Leuk Lymphoma. 2004;45:1857–64.
Ni M, Qin B, Xie L, Zhang X, Yang J, Lv H, et al. IL-13 contributes to drug resistance of NK/T-cell lymphoma cells by regulating ABCC4. Biomed Res Int. 2018;2018:2606834.
Wang L, Bi X-W, Zhu Y-J, He Y-Z, Lai Q-Y, Xia Z-J, et al. IL-2Rα up-regulation is mediated by latent membrane protein 1 and promotes lymphomagenesis and chemotherapy resistance in natural killer/T-cell lymphoma. Cancer Commun. 2018;38:62.
Zhu L, Zhang X, Fu X, Li Z, Sun Z, Wu J, et al. c-Myc mediated upregulation of long noncoding RNA SNHG12 regulates proliferation and drug sensitivity in natural killer/T-cell lymphoma. J Cell Biochem. 2019;120:12628–37.
Liapis K, Apostolidis J, Delimpasis S. EBV-associated hemophagocytic syndrome. Am J Hematol. 2011;86:422.
Lim SW, Ryu KJ, Lee H, Ko YH, Kim WS, Kim SJ. Serum IL18 is associated with hemophagocytosis and poor survival in extranodal natural killer/T-cell lymphoma. Leuk Lymphoma. 2019;60:317–25.
Li N, Zhang L, Liu J, Zhang J, Weng H-W, Zhuo H-Y, et al. A clinical study of 21 patients with hemophagocytic syndrome in 295 cases diagnosed with nasal type, extranodal nature killer/T cell lymphoma. Cancer Biol Ther. 2017;18:252–6.
Muhamad H, Suksawai N, Assanasen T, Polprasert C, Bunworasate U, Wudhikarn K. Programmed cell death 1 and programmed cell death ligands in extranodal natural killer/T cell lymphoma: expression pattern and potential prognostic relevance. Acta Haematol. 2020;143:78–88.
Kwong Y-L, Chan TSY, Tan D, Kim SJ, Poon L-M, Mow B, et al. PD1 blockade with pembrolizumab is highly effective in relapsed or refractory NK/T-cell lymphoma failing l-asparaginase. Blood. 2017;129:2437–42.
Li X, Cheng Y, Zhang M, Yan J, Li L, Fu X, et al. Activity of pembrolizumab in relapsed/refractory NK/T-cell lymphoma. J Hematol Oncol. 2018;11:15.
Kim S-J, Hyeon J, Cho I, Ko YH, Kim WS. Comparison of Efficacy of Pembrolizumab between Epstein-Barr Virus‒Positive and ‒Negative Relapsed or Refractory Non-Hodgkin Lymphomas. Cancer Res Treat. 2019;51:611–22.
Chan TSY, Li J, Loong F, Khong P-L, Tse E, Kwong Y-L. PD1 blockade with low-dose nivolumab in NK/T cell lymphoma failing L-asparaginase: efficacy and safety. Ann Hematol. 2018;97:193–6.
Cai Q, Huang H, Liu P, Zhou H, Li Y, Zhang Y, et al. Safety and preliminary efficacy of sintilimab Plus P-Gemox (pegaspargase, gemcitabine and oxaliplatin) regimen as first-line treatment for patients with advanced extranodal natural killer/T cell lymphoma, nasal type: an open-label, multicenter, phase 2 study. Blood. 2020;136:26–7.
Tao R, Fan L, Song Y, Hu Y, Zhang W, Wang Y, et al. Sintilimab for relapsed/refractory (r/r) extranodal NK/T-cell lymphoma (ENKTL): a multicenter, single-arm, phase 2 trial (ORIENT-4). 2019;37:7504.
Huang H-q, Tao R, Zou L, Cen H, Guo Y, Huang Y, et al. Preliminary results from a multicenter, single-arm, phase 2 study of CS1001, an anti-programmed death-ligand 1 (PD-L1) human monoclonal antibody (mAb), in patients (pts) with relapsed or refractory extranodal natural killer/T cell lymphoma (rr-ENKTL). Blood. 2019;134:2833.
Kim SJ, Lim JQ, Laurensia Y, Cho J, Yoon SE, Lee JY, et al. Avelumab for the treatment of relapsed or refractory extranodal NK/T-cell lymphoma: an open-label phase 2 study. Blood. 2020;136:2754–63.
Wang L, Wang H, Li P-f, Lu Y, Xia Z-j, Huang H-q, et al. CD38 expression predicts poor prognosis and might be a potential therapy target in extranodal NK/T cell lymphoma, nasal type. Ann Hematol. 2015;94:1381–8.
Feng Y, Rao H, Lei Y, Huang Y, Wang F, Zhang Y, et al. CD30 expression in extranodal natural killer/T-cell lymphoma, nasal type among 622 cases of mature T-cell and natural killer-cell lymphoma at a single institution in South China. Chin J Cancer. 2017;36:43.
Hari P, Raj RV, Olteanu H. Targeting CD38 in refractory extranodal natural killer cell-T-cell lymphoma. N. Engl J Med. 2016;375:1501–2.
Kim HK, Moon SM, Moon JH, Park JE, Byeon S, Kim WS. Complete remission in CD30-positive refractory extranodal NK/T-cell lymphoma with brentuximab vedotin. Blood Res. 2015;50:254–6.
Poon L-M, Kwong Y-L. Complete remission of refractory disseminated NK/T cell lymphoma with brentuximab vedotin and bendamustine. Ann Hematol. 2016;95:847–9.
Kim WS, Ardeshna KM, Lin Y, Oki Y, Ruan J, Jacobsen ED, et al. Autologous EBV-specific T cells (CMD-003): early results from a multicenter, multinational phase 2 trial for treatment of EBV-associated NK/T-cell lymphoma. Blood. 2017;130:4073.
Long HM. Targeting EBV-positive B- and T/NK-cell lymphomas. Blood. 2018;132:2315–6.
Shi Y, Dong M, Hong X, Zhang W, Feng J, Zhu J, et al. Results from a multicenter, open-label, pivotal phase II study of chidamide in relapsed or refractory peripheral T-cell lymphoma. Ann Oncol. 2015;26:1766–71.
Shi Y, Jia B, Xu W, Li W, Liu T, Liu P, et al. Chidamide in relapsed or refractory peripheral T cell lymphoma: a multicenter real-world study in China. J Hematol Oncol. 2017;10:69.
Yan G, Huang H-q, Li P, Bing B, Xiaoxiao W, Qixiang R, et al. Chidamide, oral subtype-selective histone deacetylase inhibitor (HDACI) monotherapy was effective on the patients with relapsed or refractory extranodal natural killer (NK)/T-cell lymphoma. Blood. 2017;130:2797.
Gao Y, Huang H, Wang X, Bai B, Zhang L, Xiao Y, et al. Anti-PD-1 antibody (sintilimab) plus histone deacetylase inhibitor (chidamide) for the treatment of refractory or relapsed extranodal natural killer/T cell lymphoma, nasal type (r/r-ENKTL): preliminary results from a prospective, multicenter, single-arm, phase Ib/II trial (SCENT). Blood. 2020;136:39–40.
Tan D, Diong CP, Loh Y, Goh YT. Histone deacetylase (HDAC) inhibitors when combined with a proteasome inhibitor are safe and effective in patients with extranodal natural killer/T-cell lymphoma (ENKTL). Ann Oncol. 2016;27:1811–2.
Coiffier B, Pro B, Prince HM, Foss F, Sokol L, Greenwood M, et al. Results from a pivotal, open-label, phase II study of romidepsin in relapsed or refractory peripheral T-cell lymphoma after prior systemic therapy. J Clin Oncol. 2012;30:631–6.
O’Connor OA, Falchi L, Lue JK, Marchi E, Kinahan C, Sawas A, et al. Oral 5-azacytidine and romidepsin exhibit marked activity in patients with PTCL: a multicenter phase 1 study. Blood. 2019;134:1395–405.
O’Connor OA, Horwitz S, Masszi T, Van Hoof A, Brown P, Doorduijn J, et al. Belinostat in patients with relapsed or refractory peripheral T-cell lymphoma: results of the pivotal phase II BELIEF (CLN-19) study. J Clin Oncol. 2015;33:2492–9.
Amengual JE, Lichtenstein R, Lue J, Sawas A, Deng C, Lichtenstein E, et al. A phase 1 study of romidepsin and pralatrexate reveals marked activity in relapsed and refractory T-cell lymphoma. Blood. 2018;131:397–407.
Mehta-Shah N, Moskowitz AJ, Lunning M, Lynch P, Scheuerman M, Kumar A, et al. A phase Ib/IIa trial of the combination of romidepsin, lenalidomide and carfilzomib in patients with relapsed/refractory lymphoma shows complete responses in relapsed and refractory T-cell lymphomas. Blood. 2016;128:2991.
Siddiquey MNA, Nakagawa H, Iwata S, Kanazawa T, Suzuki M, Imadome K-I, et al. Anti-tumor effects of suberoylanilide hydroxamic acid on Epstein-Barr virus-associated T cell and natural killer cell lymphoma. Cancer Sci. 2014;105:713–22.
Iwata S, Saito T, Ito Y, Kamakura M, Gotoh K, Kawada J-I, et al. Antitumor activities of valproic acid on Epstein-Barr virus-associated T and natural killer lymphoma cells. Cancer Sci. 2012;103:375–81.
Funding
YL was supported by Sun Yat-sen University Start-up Funding (Grant no. 201603), the Program for Guangdong Introducing Innovative and Entrepreneurial Teams (2017ZT07S096), and National Natural Science Foundation of China (Grant number: 81873428). HW was supported by National Natural Science Foundation of China (Grant number: 81700148). RPG acknowledges support from the National Institute of Health Research (NIHR) Biomedical Research Centre funding scheme.
Author information
Authors and Affiliations
Contributions
YL, HW, and RPG designed the review. HW and BBF searched databases and processed analysis. HW and BBF drafted the paper. YL, RPG, and HW revised the typescript. YL and RPG are responsible for the typescript.
Corresponding author
Ethics declarations
Conflict of interest
RPG is a consultant to BeiGene Ltd., Fusion Pharma LLC, LaJolla NanoMedical Inc., Mingsight Parmaceuticals Inc. and CStone Pharmaceuticals; advisor to Antegene Biotech LLC, Medical Director, FFF Enterprises Inc.; partner, AZAC Inc.; Board of Directors, Russian Foundation for Cancer Research Support; and Scientific Advisory Board: StemRad Ltd. All other authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wang, H., Fu, Bb., Gale, R.P. et al. NK-/T-cell lymphomas. Leukemia 35, 2460–2468 (2021). https://doi.org/10.1038/s41375-021-01313-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41375-021-01313-2
This article is cited by
-
Full-spectral genome analysis of natural killer/T cell lymphoma highlights impacts of genome instability in driving its progression
Genome Medicine (2024)
-
The RNA sequencing results revealed the expression of different genes and signaling pathways during chemotherapy resistance in peripheral T-cell lymphoma
BMC Medical Genomics (2024)
-
Clinical epidemiology of Epstein-Barr virus-associated Lymphoproliferative Disorders (EBV-LPDs) in hospitalized children: A six-year multi-institutional study in China
Italian Journal of Pediatrics (2024)
-
Genomic features reveal potential benefit of adding anti-PD-1 immunotherapy to treat non-upper aerodigestive tract natural killer/T-cell lymphoma
Leukemia (2024)
-
Increased coexpression of PD-L1 and IDO1 is associated with poor overall survival in patients with NK/T-cell lymphoma
Leukemia (2024)