Abstract
Objective
Evaluate the relationship of neonatal unit level of care (LOC) and volume with mortality or morbidity in moderate-late preterm (MLP) (32–36 weeks’ gestation) infants.
Design
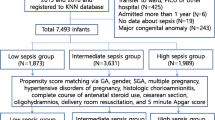
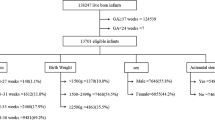
Retrospective cohort study of 650,865 inborn MLP infants in 4976 hospitals-years using 2003–2015 linked administrative data from 4 states. Exposure was combined neonatal LOC and MLP annual volume. The primary outcome was death or morbidity (respiratory distress syndrome, severe intraventricular hemorrhage, necrotizing enterocolitis, sepsis, infection, pneumothorax, extreme length of stay) with components as secondary outcomes. Poisson regression models adjusted for patient characteristics with a random effect for unit were used.
Results
In adjusted models, high-volume level 2 units had a lower risk of the primary outcome compared to low-volume level 3 units (aIRR 0.90 [95% CI 0.83–0.98] vs. aIRR 1.13 [95% CI 1.03–1.24], p < 0.001)
Conclusion
MLP infants had improved outcomes in high-volume level 2 units compared to low-volume level 3 units in adjusted analysis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
Deidentified individual participant data cannot be made available by the authors due to restrictions in the data use agreements by which the data were obtained. Access to these data and associated code must be requested via a data use agreement with the respective states.
References
Shapiro-Mendoza CK, Lackritz EM. Epidemiology of late and moderate preterm birth. Semin Fetal Neonatal Med. 2012;17:120–5.
Trembath AN, Payne AH, Colaizy TT, Bell EF, Walsh MC. The problems of moderate preterm infants. Semin Perinatol. 2016;40:370–3. https://doi.org/10.1053/j.semperi.2016.05.008.
Lindström K, Winbladh B, Haglund B, Hjern A. Preterm infants as young adults: A Swedish national cohort study. Pediatrics. 2007;120:70–7.
American Academy of Pediatrics Committee on Fetus and Newborn. Levels of neonatal care. Pediatrics. 2012;130:587–97.
Stark AR, Pursley DM, Papile LA, Eichenwald EC, Hankins CT, Buck RK, et al. Standards for Levels of Neonatal Care: II, III, and IV. Pediatrics. 2023;151:e2023061957.
Chung JH, Phibbs CS, Boscardin WJ, Kominski GF, Ortega AN, Gregory KD, et al. Examining the effect of hospital-level factors on mortality of very low birth weight infants using multilevel modeling. J Perinatol J Calif Perinat Assoc. 2011;31:770–5. https://pubmed.ncbi.nlm.nih.gov/21494232/.
Phibbs CS, Baker LC, Caughey AB, Danielsen B, Schmitt SK, Phibbs RH. Level and volume of neonatal intensive care and mortality in very-low-birth-weight infants. N Engl J Med. 2007;356:2165–75.
Lasswell SM, Barfield WD, Rochat RW, Blackmon L. Perinatal regionalization for very low-birth-weight and very preterm infants a meta-analysis. JAMA. 2010;304:992–1000.
Cifuentes J, Bronstein J, Phibbs CS, Phibbs RH, Schmitt SK, Carlo WA. Mortality in low birth weight infants according to level of neonatal care at hospital of birth. Pediatrics. 2002;109:745–51.
Lorch SA, Baiocchi M, Ahlberg C, Small D. The differential impact of delivery hospital on the outcomes of premature infants. Pediatrics. 2012;130:270–8. https://pubmed.ncbi.nlm.nih.gov/22778301/.
Phibbs C, Bronstein J, Buxton E, Phibbs R. The effects of patient volume and level of care at the hospital of birth on neonatal mortality. JAMA. 1996;276:1054–9.
Salazar EG, Handley SC, Greenberg LT, Edwards EM, Lorch SA. Association Between Neonatal Intensive Care Unit Type and Quality of Care in Moderate and Late Preterm Infants. JAMA Pediatr. 2023;177:278–85. https://pubmed.ncbi.nlm.nih.gov/36648939/.
Herrchen B, Gould J, Nesbitt T. Vital statistics linked birth/infant death and hospital discharge record linkage for epidemiological studies. Comput Biomed Res. 1997;30:290–305.
von Elm E, Altman D, Egger M, Pocock S, Gøtzsche P, Vandenbroucke J, et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Ann Intern Med. 2007;147:573–7.
Yannekis G, Passarella M, Lorch S. Differential effects of delivery hospital on mortality and morbidity in minority premature and low birth weight neonates. J Perinatol. 2020;40:404–11. https://doi.org/10.1038/s41372-019-0423-9.
Gyamfi-Bannerman C, Thom E, Blackwell S, Tita A, Reddy U, Saade G, et al. Antenatal betamethasone for women at risk for late preterm delivery. N Engl J Med. 2016;374:1311–20.
Clapp M, Melamed A, Freret T, James K, Gyamfi-Bannerman C, Kaimal A. US Incidence of Late-Preterm Steroid Use and Associated Neonatal Respiratory Morbidity After Publication of the Antenatal Late Preterm Steroids Trial, 2015-2017. JAMA Netw Open. 2022;2022:e2212702.
Roberts D, Brown J, Medley N, Dalziel SR. Antenatal corticosteroids for accelerating fetal lung maturation for women at risk of pretemr birth. Cochrane Database Syst Rev. 2017;3:CD004454.
Salazar EG, Handley SC, Greenberg LT, Edwards EM, Lorch SA, Greenbery LT, et al. Measuring Quality of Care in Moderate and Late Preterm Infants. J Perinatol. 2022;42:1294–1300.
Duong HH, Mirea L, Shah PS, Yang J, Lee SK, Sankaran K. Pneumothorax in neonates: Trends, predictors and outcomes. J Neonatal-Perinat Med. 2014;7:29–38.
Altman M, Vanpée M, Cnattingius S, Norman M. Moderately preterm infants and determinants of length of hospital stay. Arch Dis Child Fetal Neonatal Ed. 2009;94:414–8.
Escobar GJ, McCormick MC, Zupancic JAF, Coleman-Phox K, Armstrong MA, Greene JD, et al. Unstudied infants: Outcomes of moderately premature infants in the neonatal intensive care unit. Arch Dis Child Fetal Neonatal Ed. 2006;91:238–44.
Profit J, McCormick MC, Escobar GJ, Richardson DK, Zheng Z, Coleman-Phox K, et al. Neonatal intensive care unit census influences discharge of moderately preterm infants. Pediatrics. 2007;119:314–9.
Lukacs SL, Schrag SJ. Clinical sepsis in neonates and young infants, United States, 1988-2006. J Pediatr. 2012;160:960–965.e1. https://doi.org/10.1016/j.jpeds.2011.12.023.
Cleary-Goldman J, Malone F, Vidaver J, Ball R, Nyberg D, Comstock C, et al. Impact of maternal age on obstetric outcome. Obstet Gynecol. 2005;105:983–90.
Howell E, Hebert P, Chatterjee S, Kleinman L, Chassin M. Black/white differences in very low birth weight neonatal mortality rates among New York City hospitals. Pediatrics. 2008;121:e407–15.
McBride C, Bernstein I, Badger G, Horbar J, Soll R. The effect of maternal hypertension on mortality in infants 22-29 weeks gestation. Pregnancy Hypertens. 2005;5:362–6.
Kozhimannil K, Shippee T, Adegoke O, Vemig BA. Trends in hospital-based childbirth care: the role of health insurance. Am J Manag Care. 2013;19:e125–32.
Korb D, Goffinet F, Seco A, Chevret S, Deneux-Tharaux C. Risk of severe maternal morbidity associated with cesarean delivery and the role of maternal age: a population-based propensity score analysis. CMAJ. 2019;191:E352–60.
Tyson J, Parikh N, Langer J, Green C, Higgins R, Network NI of CH and HDNR. Intensive care for extreme prematurity-moving beyond gestational age. N Engl J Med. 2008;358:1672–81.
Clausson B, Gardosi J, Francis A, Cnattingius S. Perinatal outcome in SGA births defined by customised versus population-based birthweight standards. BJOG. 2001;108:830–4.
Stoll B, Hansen N, Bell E, et al. Trends in Care Practices, Morbidity, and Mortality of Extremely Preterm Neonates, 1993-2012. JAMA. 2015;314:1039–51.
Shapiro-Mendoza CK, Tomashek KM, Kotelchuck M, Barfield W, Nannini A, Weiss J, et al. Effect of late-preterm birth and maternal medical conditions on newborn morbidity risk. Pediatrics. 2008;121:e223–32. https://pubmed-ncbi-nlm-nih-gov.proxy.library.upenn.edu/18245397/.
Fenton TR. A new growth chart for preterm babies: Babson and Benda’s chart updated with recent data and a new format. BMC Pediatr. 2003;3:13. https://pubmed.ncbi.nlm.nih.gov/14678563/.
Linden A, Mathur MB, VanderWeele TJ. Conducting sensitivity analysis for unmeasured confounding in observational studies using E-values: The evalue package. Stata J. 2020;20:162–75. https://doi.org/10.1177/1536867X20909696.
Jensen EA, Lorch SA. Effects of a Birth Hospital’s Neonatal Intensive Care Unit Level and Annual Volume of Very Low-Birth-Weight Infant Deliveries on Morbidity and Mortality. JAMA Pediatr. 2015;169:e151906.
Chung JH, Phibbs CS, Boscardin WJ, Kominski GF, Ortega AN, Needleman J. The effect of neonatal intensive care level and hospital volume on mortality of very low birth weight infants. Med Care. 2010;48:635–44. https://pubmed.ncbi.nlm.nih.gov/20548252/.
Acknowledgements
PA: The Pennsylvania Health Care Cost Containment Council (PHC4) is an independent state agency responsible for addressing the problem of escalating health costs, ensuring the quality of health care, and increasing access to health care for all citizens regardless of ability to pay. PHC4 has provided data to this entity in an effort to further PHC4’s mission of educating the public and containing health care costs in Pennsylvania. PHC4, its agents, and staff, have made no representation, guarantee, or warranty, express or implied, that the data -- financial, patient, payor, and physician specific information -- provided to this entity, are errorfree, or that the use of the data will avoid differences of opinion or interpretation. This analysis was not prepared by PHC4. This analysis was done by the aforementioned authors. PHC4, its agents and staff, bear no responsibility or liability for the results of the analysis, which are solely the opinion of this entity. MO: The data used in this document/presentation was acquired from the Missouri Department of Health and Senior Services (DHSS). The contents of this document including data analysis, interpretation or conclusions are solely the responsibility of the authors and do not represent the official views of DHSS. SC: This information is from the records of the Revenue and Fiscal Affairs Office, Health and Demographics Section, South Carolina. Our authorization to release this information does not imply endorsement of this study or its findings by either the revenue and fiscal affairs office or the data oversight council.
Funding
T32HL098054 (to EGS). R01HD084819 (to CSP, SAL). K23HD109426 (to SCH).
Author information
Authors and Affiliations
Contributions
Dr. Elizabeth Salazar designed the study, drafted the initial manuscript, reviewed, and revised the manuscript. Dr. Sara Handley conceptualized and designed the study, critically reviewed, and revised the manuscript. Brielle Formanowski and Molly Passarella carried out the analyses, critically reviewed and revised the manuscript. Dr. Scott Lorch conceptualized and designed the study, obtained grant funding for the creation of the data source for the project, as well as critically reviewed and revised the manuscript. Dr. Ciaran Phibbs provided critical feedback on study methodology, obtained grant funding for the creation of the data source for the project, as well as reviewed and revised the manuscript. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Salazar, E.G., Passarella, M., Formanowski, B. et al. The impact of volume and neonatal level of care on outcomes of moderate and late preterm infants. J Perinatol (2024). https://doi.org/10.1038/s41372-024-01901-x
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41372-024-01901-x