Abstract
Objective
We aimed to reduce the time interval between an infant’s admission to the Neonatal Intensive Care Unit (NICU) and first maternal interaction.
Methods
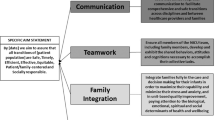
We identified three key drivers: 1. Collaboration with Labor and Delivery, 2. Education of staff and parents, and 3. Improved documentation of maternal presence. We measured the time interval from NICU admission to the initial maternal presence. We followed length of stay as a balancing measure to assay whether use of remote televisitation impeded efficient parental teaching and delayed discharge.
Results
We reduced the time interval from an average of 19.7 h in February 2020 to 12.3 h in June 2021. We expanded an already existing televisitation program as a surrogate to in-person interaction during COVID-19 pandemic. Televisitation did not affect in-person parental presence or LOS.
Conclusion
Our multidisciplinary efforts resulted in a significantly accelerated time to initial maternal presence and did not prolong LOS.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
After de-identification, individual participant data that underlie the results reported in this paper will be available to researchers who provide a methodologically sound proposal. To gain access, data requestors will need to sign a data access agreement.
References
Mulder EJ, Robles de Medina PG, Huizink AC, Van den Bergh BR, Buitelaar JK, Visser GH. Prenatal maternal stress: effects on pregnancy and the (unborn) child. Early Hum Dev. 2002;70:3–14.
Pineda RG, Stransky KE, Rogers C, Duncan MH, Smith GC, Neil J, et al. The single-patient room in the NICU: maternal and family effects. J Perinatol. 2012;32:545–51.
Harris R, Gibbs D, Mangin-Heimos K, Pineda R. Maternal mental health during the neonatal period: Relationships to the occupation of parenting. Early Hum Dev. 2018;120:31–9.
Lasiuk GC, Comeau T, Newburn-Cook C. Unexpected: an interpretive description of parental traumas' associated with preterm birth. BMC Pregnancy Childbirth. 2013;13:S13.
Greene MM, Rossman B, Patra K, Kratovil A, Khan S, Meier PP. Maternal psychological distress and visitation to the neonatal intensive care unit. Acta Paediatr. 2015;104:e306–13.
Pineda R, Bender J, Hall B, Shabosky L, Annecca A, Smith J. Parent participation in the neonatal intensive care unit: Predictors and relationships to neurobehavior and developmental outcomes. Early Hum Dev. 2018;117:32–8.
Lewis TP, Andrews KG, Shenberger E, Betancourt TS, Fink G, Pereira S, et al. Caregiving can be costly: A qualitative study of barriers and facilitators to conducting kangaroo mother care in a US tertiary hospital neonatal intensive care unit. BMC Pregnancy Childbirth. 2019;19:227.
Sigurdson K, Mitchell B, Liu J, Morton C, Gould JB, Lee HC, et al. Racial/Ethnic Disparities in Neonatal Intensive Care: A Systematic Review. Pediatrics. 2019;144:e20183114.
Greene MM, Rossman B, Meier P, Patra K. Elevated maternal anxiety in the NICU predicts worse fine motor outcome in VLBW infants. Early Hum Dev. 2018;116:33–9.
Muinga N, Abejirinde IO, Paton C, English M, Zweekhorst M. Designing paper-based records to improve the quality of nursing documentation in hospitals: A scoping review. J Clin Nurs. 2021;30:56–71.
Kroth PJ, Dexter PR, Overhage JM, Knipe C, Hui SL, Belsito A, et al. A computerized decision support system improves the accuracy of temperature capture from nursing personnel at the bedside. AMIA Annu Symp Proc. 2006;2006:444–8.
Caraballo PJ, North F, Peters S, Puffer M, Nyman M, Epps S, et al. Use of decision support to prevent errors when documenting height and weight in the hospital electronic medical record. AMIA Annu Symp Proc 2008:890.
Mastrianni A, Sarcevic A, Chung LS, Zakeri I, Alberto EC, Milestone ZP, et al. Designing Interactive Alerts to Improve Recognition of Critical Events in Medical Emergencies. DIS (Des Interact Syst Conf). 2021;2021:864–78.
Cimino JJ, Farnum L, Cochran K, Moore SD, Sengstack PP, McKeeby JW. Interpreting nurses' responses to clinical documentation alerts. AMIA Annu Symp Proc. 2010;2010:116–20.
Author information
Authors and Affiliations
Contributions
PN, JC- conceptualization, implementation, data collection and data analysis. AB, DS, JM, AA, SS- implementation and data collection. TS, KW- conceptualization, information technology support, implementation. MG- conceptualization and data analysis. MH- conceptualization and implementation.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nandula, P.S., Buckelew, A., Cortez, J. et al. A quality improvement initiative to reduce the time to initial maternal visit in the neonatal intensive care unit. J Perinatol 44, 446–451 (2024). https://doi.org/10.1038/s41372-023-01726-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-023-01726-0