Abstract
Objective
To understand the perspectives and perceived facilitators of and barriers to following safe infant sleeping practices among mothers with opioid use disorder (OUD).
Study design
Using the Theory of Planned Behavior (TPB) framework, we conducted qualitative interviews with mothers with OUD regarding infant sleep practices. We created codes and generated themes, concluding data collection upon achieving thematic saturation.
Results
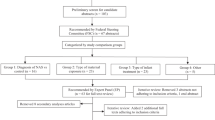
Twenty-three mothers with infants 1–7 months of age were interviewed from 08/2020 to 10/2021. Mothers chose sleeping practices they perceived made their infants safer, more comfortable, and minimized infant withdrawal symptoms. Mothers in residential treatment facilities were influenced by facility infant sleep rules. Hospital sleep modeling and varied advice by providers, friends and family influenced maternal decisions.
Conclusions
Mothers reported factors unique to their experience with OUD that influenced their decisions about infant sleep that should be considered when developing tailored interventions to promote safe infant sleep in this population.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
The code book and de-identified transcripts are available upon reasonable request.
References
Hwang SS, Parker MG, Colvin BN, Forbes ES, Brown K, Colson ER. Understanding the barriers and facilitators to safe infant sleep for mothers of preterm infants. J. Perinatol. 2021;41:1992–9.
The Centers for Disease Control and Prevention. Sudden unexpected infant death and sudden infant death syndrome: data and statistics. https://www.cdc.gov/sids/data.htm. Accessed 27 July, 2022.
Zipursky J, Juurlink DN. Opioid use in pregnancy: an emergin health crisis. Obstet Med. 2021;14:211–9.
Patrick SW, Barfield WD, Poindexter BP, Cummings J, Hand, Adams-Chapman I, et al. Neonatal opioid withdrawal syndrome. Pediatrics 2020;146:e2020029074.
Kandall SR, Gaines J. Maternal substance use and subsequent sudden infant death syndrome (SIDS) in offspring. Neurotoxicol Teratol. 1991;13:235–40.
Ward SL, Bautista D, Chan L, Derry M, Lisbin A, Durfee MJ, et al. Sudden infant death syndrome in infants of substance abusing mothers. J. Pediatr. 1990;117:876–81.
Moon, RY. How to keep your sleeping baby safe: AAP policy explained. [internet]. American Academy of Pediatrics: Baby Safe Sleep Coalition. c2014-2023 [updated 2022 Jun; cited 2022 September]. Available from https://www.babysafesleep.org/how-to-keep-your-sleeping-baby-safe-aap-policy-explained.org/.
Moon RY, Corwin MJ, Kerr S, Heeren T, Colson E, Kellams A, et al. Mediators of improved adherence to infant safe sleep using a mobile health intervention. Pediatrics. 2019;143:e20182799.
Glanz K, Rimer BK, Viswanath K. Health Behavior: Theory, Research, and Practice. 5th Edition. https://www.wiley.com/en-us/Health+Behavior:+Theory,+Research,+and+Practice,+5th+Edition-p-9781118628980.
Ajzen, I. The Theory of planned Behavior. [internet]. University of Massachusetts Amherst. c2019 [updated 2019; cited 2022 Sept 9]. Available from https://www.peopleumass.edu/aizen/tpb.diag.html.
Ajzen I. The Theory of Planned Behavior. Organ Behav Hum Decis Process. 1991;50:179–211. https://doi.org/10.1016/0749-5978(91)90020-T.
Montano DE, Kasprzyk D. Theory of Reasoned Action, Theory of Planned Behavior, and the Integrated Behavioral Model. In: Glanz K, Rimer BK, Viswanath K, editors. Health Behavior and Health Education, 4th ed. San Francisco, CA: Jossey-Bass, 2002. p. 67–96.
Denzin N, Kal YS. The Sage Handbook of Qualitative Research. 3rd ed. Thousand Oaks, CA: Sage Publications; 2006.
Archibald MM. Investigator triangulation: a collaborative strategy with potential for mixed methods research. 2016;10. https://doi.org/10.1177/1558689815570092.
Carter N, Bryant-Lukosius D, DiCenso A, Blythe J, Neville AJ. The use of triangulation in qualitative research. Oncol Nurs Forum. 2014;41:545–7.
Farmer T, Robinson K, Elliott SJ, Eyles J. Developing and implementing a triangulation protocol for qualitative health research. Qual Health Res. 2006;16:377–94.
Colson ER, Levenson S, Rybin D, Calianos C, Margolis A, Colton T, et al. Barriers to following the supine sleep recommendation among mothers at four centers for Women, Infants, and Children Program. Pediatrics 2006;118:e243–e250.
Oden RP, Joyner BL, Ajao TI, Moon RY. Factors influencing African American mothers’ decisions about sleep position: a qualitative study. J. Natl Med Assoc. 2010;102:870–80.
De Sousa Machado T, Chur-Hansen A, Due C. First-time mothers’ perceptions of social support: recommendations for best practice. Health Psychol Open. 2002; https://doi.org/10.1177/2055102919898611.
Velez M, Jansson LM. The opioid dependent mother and newborn dyad: nonpharmacologic care. J. Addict Med (200*). 2008;2:113–20. https://doi.org/10.1097/ADM.0b013e31817e6105.
McHugo GJ, Caspi Y, Kammerer N, Mazelis R, Jackson EW, Russell L, et al. The assessment of trauma history in women with co-occurring substance abuse and mental disorders and a history of interpersonal violence. J. Behav Health Serv Res. 2005;32:113–27.
Velez ML, Montoya ID, Jansson LM, Walters V, Svikis D, Jones HE, et al. Exposure to violence among substance-dependent pregnant women and their children. J. Subst Abus Treat. 2006;30:31–8.
Rutherford HJV, William SK, Moy S, Mayes LC, Johns JM. Disruption of maternal parenting circuitry by addictive process: rewiring of reward and stress systems. Front Psychiatry. 2011;2:1–17. https://doi.org/10.3389/fpsyt.2011.00037.
Wachman EM, Grossman M, Schiff DM, Philipp BL, Minear S, Hutton E, et al. Quality improvement initiative to improve inpatient outcomes for Neonatal Abstinence Syndrome. J. Perinatol. 2018;38:1114–22.
Grossman MR, Berkwitt AK, Osborn RR, Xu Y, Esserman DA, Shapiro ED, et al. An Initiative to Improve the Quality of Care of Infants With Neonatal Abstinence Syndrome. Pediatrics 2017;139:e20163360.
Ghertner, R, Groves, L. The opioid crisis and economic opportunity: geographic and economic trends [internet]. U.S. Dept of Health and Human Services. [updated 2018 Sept 11; cited September 2022]. Available from https://aspe.hhs.gov/sites/default/files/private/pdf/259261/ASPEEconomicOpportunityOpioidCrisis.pdf.
Acknowledgements
We acknowledge all mothers who participated in this study. We also acknowledge the Harvard Neonatal-Perinatal Medicine Fellowship Program for supporting Dr TM.
Funding
This study was supported by grant funding from the American SIDS Institute. PI MP.
Author information
Authors and Affiliations
Contributions
Dr TM composed the first draft and edited all subsequent drafts of the paper. She reviewed and coded transcripts and was involved in all discussions regarding theme development. Dr KS and AW made significant revisions to the paper. They reviewed and coded transcripts and were involved in all discussions regarding theme development. LC conducted all interviews with study participants and participated in code book development. CBS reviewed transcripts and participated in codebook development. She reviewed and made significant contributions to this paper. Drs BC, HF, DS and EW participated in our process of expert triangulation and made significant contributions to the development of this paper. Drs EC and M-LD participated in interview guide development, code development, generation of themes. They provided meaningful feedback that contributed to the development of the paper. Dr MP is the principal investigator of this research. She developed the study question, designed the study, participated in interview guide development, code book development and the generation of themes. She provided significant oversight of this work and extensive review of all drafts of this paper. All authors approved the final paper as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Morrison, T.M., Standish, K.R., Wanar, A. et al. Drivers of decision-making regarding infant sleep practices among mothers with opioid use disorder. J Perinatol 43, 923–929 (2023). https://doi.org/10.1038/s41372-023-01701-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-023-01701-9