Abstract
Objective
To analyze and compare perspectives on antenatal consultation and decision-making from participants with varying degrees of prematurity experience and clinician-experts.
Study design
Open-ended interviews structured around topics previously identified by recognized clinician-experts were conducted with participants having different levels of prematurity experience. Analysis used mixed methods (thematic and mental models analysis). Secondary sub-group comparisons were performed, based on degree of experience.
Results
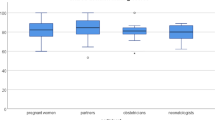
Non-clinician participants’ (n = 80) perspectives differed regarding: amount and content of information desired, decision-making strategies, and who – parent or clinician – should direct consultations. Most wanted to retain decisional authority, all recognized their emotional limitations and many advocated for deliberation support. Participants worried parents’ would regret choosing palliative care contrary to clinicians. Bereaved parents often saw issues differently.
Conclusions
Parents approach risk and decision-making for extremely premature infants in a personal fashion. They need personalized support tailored to their unique circumstances, decision-making preferences, and emotions.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Janvier A, Lorenz JM, Lantos JD. Antenatal counselling for parents facing an extremely preterm birth: limitations of the medical evidence. Acta Paediatr. 2012;101:800–4.
Gaucher N, Payot A. Focusing on relationships, not information, respects autonomy during antenatal consultations. Acta Paediatr. 2017;106:14–20.
Kim UO, Basir MA. Informing and educating parents about the risks and outcomes of prematurity. Clin Perinatol. 2014;41:979–91.
Guillén Ú, Suh S, Munson D, Posencheg M, Truitt E, Zupancic JA, et al. Development and pretesting of a decision-aid to use when counseling parents facing imminent extreme premature delivery. J Pediatr. 2012;160:382–7.
Haward MF, Gaucher N, Payot A, Robson K, Janvier A. Personalized decision making: practical recommendations for antenatal counseling for fragile neonates. Clin Perinatol. 2017;44:429–45.
Grobman WA, Kavanaugh K, Moro T, DeRegnier RA, Savage T. Providing advice to parents for women at acutely high risk of periviable delivery. Obstet Gynecol. 2010;115:904–9.
Payot A, Gendron S, Lefebvre F, Doucet H. Deciding to resuscitate extremely premature babies: how do parents and neonatologists engage in the decision? Soc Sci Med. 2007;64:1487–500.
Fischhoff B, Barnato AE. Value awareness: a new goal for end-of-life decision making. MDM Policy Pr. 2019;4:2381468318817523.
Haward MF, Janvier A, Lorenz JM, Fischhoff B. Counseling parents at risk of delivery of an extremely premature infant: Differing strategies. AJOB Empir Bioeth. 2017;8:243–52.
Morgan MGFB, Bostrom A, Atman C. Risk communication: a mental models approach. Cambridge UK: Cambridge University Press; 2002.
Bruine de Bruin W, Bostrom A. Assessing what to address in science communication. Proc Natl Acad Sci USA 2013;110:14062–8.
Haward MF, Lorenz JM, Janvier A, Fischhoff B. Bereaved parents: insights for the antenatal consultation. Am J Perinatol. 2021. https://doi.org/10.1055/s-0041-1731651. Epub ahead of print.
Bourque CJ, Dahan S, Mantha G, Robson K, Reichherzer M, Janvier A. Improving neonatal care with the help of veteran resource parents: an overview of current practices. Semin Fetal Neonatal Med. 2018;23:44–51.
Janvier A, Bourque CJ, Dahan S, Robson K, Barrington KJ. Integrating parents in neonatal and pediatric research. Neonatology 2019;115:283–91.
Gaucher N, Nadeau S, Barbier A, Janvier A, Payot A. Personalized antenatal consultations for preterm labor: responding to mothers’ expectations. J Pediatr. 2016;178:130–4.e7.
Lantos JD. Ethical problems in decision making in the neonatal ICU. N Engl J Med. 2018;379:1851–60.
Goggins KM, Wallston KA, Nwosu S, Schildcrout JS, Castel L, Kripalani S. Health literacy, numeracy, and other characteristics associated with hospitalized patients’ preferences for involvement in decision making. J Health Commun. 2014;19:29–43.
Reyna VF, Nelson WL, Han PK, Dieckmann NF. How numeracy influences risk comprehension and medical decision making. Psychol Bull. 2009;135:943–73.
Lipkus IM, Samsa G, Rimer BK. General performance on a numeracy scale among highly educated samples. Med Decis Mak. 2001;21:37–44.
Kaemingk BD, Carroll K, Thorvilson MJ, Schaepe KS, Collura CA. Uncertainty at the limits of viability: a qualitative study of antenatal consultations. Pediatrics. 2021;147:e20201865.
Kharrat A, Moore GP, Beckett S, Nicholls SG, Sampson M, Daboval T. Antenatal consultations at extreme prematurity: a systematic review of parent communication needs. J Pediatr. 2018;196:109–15.e7.
Arnolds M, Xu L, Hughes P, McCoy J, Meadow W. Worth a try? Describing the experiences of families during the course of care in the neonatal intensive care unit when the prognosis is poor. J Pediatr. 2018;196:116–22.e3.
Dahan S, Bourque CJ, Reichherzer M, Prince J, Mantha G, Savaria M, et al. Community, hope, and resilience: parental perspectives on peer support in neonatology. J Pediatr. 2022;243:85–90.e2.
Thivierge E, Luu TM, Bourque CJ, Duquette LA, Pearce R, Jaworski M, Barrington KJ, et al. Guilt and regrets experienced by parents of children born extremely preterm. J Pediatr. 2022:S0022-3476(22)01019-8. https://doi.org/10.1016/j.jpeds.2022.10.042. Epub ahead of print.
Hynan MT, Steinberg Z, Baker L, Cicco R, Geller PA, Lassen S, et al. Recommendations for mental health professionals in the NICU. J Perinatol. 2015;35:S14–8.
Snaman JM, Kaye EC, Torres C, Gibson DV, Baker JN. Helping parents live with the hole in their heart: The role of health care providers and institutions in the bereaved parents’ grief journeys. Cancer 2016;122:2757–65.
Zaal-Schuller IH, Geurtzen R, Willems DL, de Vos MA, Hogeveen M. What hinders and helps in the end-of-life decision-making process for children: Parents’ and physicians’ views. Acta Paediatr. 2022;111:873–87.
Fischhoff B. Hindsight foresight: the effect of outcome knowledge on judgment under uncertainty. J Exp Psychol Hum Percept Perform. 1975;1:288–99.
Baron J, Hershey JC. Outcome bias in decision evaluation. J Pers Soc Psychol. 1988;54:569–79.
Geurtzen R, van Heijst AFJ, Draaisma JMT, Kuijpers L, Woiski M, Scheepers HCJ, et al. Development of nationwide recommendations to support prenatal counseling in extreme prematurity. Pediatrics. 2019;143:e20183253.
Levetown M, Committee on B. Communicating with children and families: from everyday interactions to skill in conveying distressing information. Pediatrics. 2008;121:e1441–e60.
Acknowledgements
We thank Rosie Ferrara, Sandra Sandve for additional help with transcriptions. The authors are grateful for the participants in these interviews, who shared their views and experiences with us on these difficult topics.
Funding
Marron-Manginello Endowment of the Valley Hospital Foundation and Division of Neonatology, Albert Einstein College of Medicine, Children’s Hospital at Montefiore.
Author information
Authors and Affiliations
Contributions
All authors participated equally in the following: 1- conceived and designed the work that led to the submission, acquired data, and played an important role in interpreting the results 2- Drafted or revised the manuscript. 3- Approved the final version.4- Agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Haward, M.F., Lorenz, J.M., Janvier, A. et al. Antenatal consultation and deliberation: adapting to parental preferences. J Perinatol 43, 895–902 (2023). https://doi.org/10.1038/s41372-023-01605-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-023-01605-8