Abstract
Objective
To assess the educational and clinical impact of a tiny baby intubation team (TBIT).
Study design
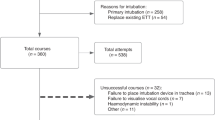
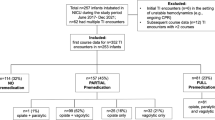
Retrospective study comparing endotracheal intubation (ETI) performed: pre-implementation of a TBIT (T1), 6 months post-implementation (T2), and 4 years post-implementation (T3).
Results
Post-implementation (T2), first-attempt success rate in tiny babies increased (44% T1; 59% T2, p = 0.04; 56% T3, p = NS) and the proportion of ETIs performed by residents decreased (53% T1; 37% T2, p = 0.001; 45% T3, p = NS). After an educational quality improvement intervention (prioritizing non-tiny baby ETIs to residents, systematic simulation training and ETI using videolaryngoscopy), in T3 residents’ overall (67% T1; 60% T2, p = NS; 79% T3, p = 0.02) and non-tiny baby ETI success rate improved (72% T1; 60% T2, p = NS; 82% T3, p = 0.02).
Conclusion
A TBIT improves success rate of ETIs in ELBW infants but decreases educational exposure of residents. Educational strategies may help maintain resident procedural competency without impacting on quality of care.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Raju TN, Vidyasagar D, Torres C, Grundy D, Bennett EJ. Intracranial pressure during intubation and anesthesia in infants. J Pediatr. 1980;96:860–2.
Friesen RH, Honda AT, Thieme RE. Changes in anterior fontanel pressure in preterm neonates during tracheal intubation. Anesth Analg. 1987;66:874–8.
Marshall TA, Deeder R, Pai S, Berkowitz GP, Austin TL. Physiologic changes associated with endotracheal intubation in preterm infants. Crit Care Med. 1984;12:501–3.
Hatch LD, Grubb PH, Lea AS, Walsh WF, Markham MH, Whitney GM, et al. Endotracheal intubation in neonates: a prospective study of adverse safety events in 162 infants. J Pediatr. 2016;168:62–66.e66.
Stow PJ, McLeod ME, Burrows FA, Creighton RE. Anterior fontanelle pressure responses to tracheal intubation in the awake and anaesthetized infant. Br J Anaesth. 1988;60:167–70.
Miller KE, Singh N. Association of multiple tracheal intubation attempts with clinical outcomes in extremely preterm infants: a retrospective single-center cohort study. J Perinatol. 2022;42:1216–20.
Wallenstein MB, Birnie KL, Arain YH, Yang W, Yamada NK, Huffman LC, et al. Failed endotracheal intubation and adverse outcomes among extremely low birth weight infants. J Perinatol. 2016;36:112–5.
Johnston L, Sawyer T, Ades A, Moussa A, Zenge J, Jung P, et al. Impact of physician training level on neonatal tracheal intubation success rates and adverse events: a report from National Emergency Airway Registry for Neonates (NEAR4NEOS). Neonatology. 2021;118:434–42.
Sanders RC Jr, Giuliano JS Jr, Sullivan JE, Brown CA III, Walls RM, Nadkarni V, et al. Level of trainee and tracheal intubation outcomes. Pediatrics. 2013;131:e821–e828.
Morris M, Cleary JP, Soliman A. Small baby unit improves quality and outcomes in extremely low birth weight infants. Pediatrics. 2015;136:e1007–e1015.
O’Donnell CP, Kamlin CO, Davis PG, Morley CJ. Endotracheal intubation attempts during neonatal resuscitation: success rates, duration, and adverse effects. Pediatrics. 2006;117:e16–e21.
Gozzo YF, Cummings CL, Chapman RL, Bizzarro MJ, Mercurio MR. Who is performing medical procedures in the neonatal intensive care unit? J Perinatol. 2011;31:206–11.
Moussa A, Luangxay Y, Tremblay S, Lavoie J, Aube G, Savoie E, et al. Videolaryngoscope for teaching neonatal endotracheal intubation: a randomized controlled trial. Pediatrics. 2016;137:1–8.
Assaad MA, Lachance C, Moussa A. Learning neonatal intubation using the videolaryngoscope: a randomized trial on mannequins. Simul Health. 2016;11:190–3.
Foglia EE, Ades A, Sawyer T, Glass KM, Singh N, Jung P, et al. Neonatal intubation practice and outcomes: an international registry study. Pediatrics. 2019;143:e20180902.
Downes KJ, Narendran V, Meinzen-Derr J, McClanahan S, Akinbi HT. The lost art of intubation: assessing opportunities for residents to perform neonatal intubation. J Perinatol. 2012;32:927–32.
Haubner LY, Barry JS, Johnston LC, Soghier L, Tatum PM, Kessler D, et al. Neonatal intubation performance: room for improvement in tertiary neonatal intensive care units. Resuscitation. 2013;84:1359–64.
Wyckoff MH, Aziz K, Escobedo MB, Kapadia VS, Kattwinkel J, Perlman JM. et al. Part 13: neonatal resuscitation: 2015 American Heart Association Guidelines update for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation. 2015;132:S543–S560.
Donoghue AJ, Ades AM, Nishisaki A, Deutsch ES. Videolaryngoscopy versus direct laryngoscopy in simulated pediatric intubation. Ann Emerg Med. 2013;61:271–7.
Sawyer T, Foglia E, Hatch LD, Moussa A, Ades A, Johnston L, et al. Improving neonatal intubation safety: a journey of a thousand miles. J Neonatal Perinat Med. 2017;10:125–31.
Mills DM, Williams DC, Dobson JV. Simulation training as a mechanism for procedural and resuscitation education for pediatric residents: a systematic review. Hosp Pediatr. 2013;3:167–76.
Finan E, Bismilla Z, Campbell C, Leblanc V, Jefferies A, Whyte HE. Improved procedural performance following a simulation training session may not be transferable to the clinical environment. J Perinatol. 2012;32:539–44.
Surcouf JW, Chauvin SW, Ferry J, Yang T, Barkemeyer B. Enhancing residents’ neonatal resuscitation competency through unannounced simulation-based training. Med Educ Online. 2013;18:1–7.
O’Shea JE, Thio M, Kamlin CO, McGrory L, Wong C, John J, et al. Videolaryngoscopy to teach neonatal intubation: a randomized trial. Pediatrics. 2015;136:912–9.
Volz S, Stevens TP, Dadiz R. A randomized controlled trial: does coaching using video during direct laryngoscopy improve residents’ success in neonatal intubations? J Perinatol. 2018;38:1074–80.
Lingappan K, Arnold JL, Fernandes CJ, Pammi M. Videolaryngoscopy versus direct laryngoscopy for tracheal intubation in neonates. Cochrane Database Syst Rev. 2018;6:Cd009975.
Vlatten A, Aucoin S, Litz S, Macmanus B, Soder C. A comparison of the STORZ video laryngoscope and standard direct laryngoscopy for intubation in the Pediatric airway—a randomized clinical trial. Paediatr Anaesth. 2009;19:1102–7.
Hodgson KA, Owen LS, Kamlin COF, Roberts CT, Newman SE, Francis KL, et al. Nasal high-flow therapy during neonatal endotracheal intubation. N Engl J Med. 2022;386:1627–37.
Author information
Authors and Affiliations
Contributions
LG-A has contributed to conception and design, acquisition of data, analysis and interpretation of data. She has co-written (with MJ) the first draft of this specific article and modified subsequent drafts until all authors approved the final version of the article. MJ has contributed to conception and design, acquisition of data, analysis and interpretation of data. She has co-written (with LG-A) the first draft of this specific article and revised the article critically for important intellectual content. GE and KJB have contributed to analysis and interpretation of data; and revised the article critically for important intellectual content. TP has contributed to acquisition of data, analysis and interpretation of data; and revised the article critically for important intellectual content. AM has contributed to conception and design, acquisition of data, analysis and interpretation of data. He helped LG-A and MJ write the first draft of this specific article and revised the article critically for important intellectual content. All authors agree to be accountable for all aspects of the work. They ensure that questions relating to accuracy or integrity of any part of the work are appropriately investigated and resolved. All authors have approved the final version of the article as sent to Journal of Perinatology.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
This study was approved by the Sainte-Justine University Hospital institutional review board (Reference number: 2016-1209) and performed in accordance with the Declaration of Helsinki.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gariépy-Assal, L., Janaillac, M., Ethier, G. et al. A tiny baby intubation team improves endotracheal intubation success rate but decreases residents’ training opportunities. J Perinatol 43, 215–219 (2023). https://doi.org/10.1038/s41372-022-01546-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-022-01546-8