Abstract
Objective
To perform an external validation of a publicly available model predicting extubation success in very preterm infants.
Study design
Retrospective study of infants born <1250 g at a single center. Model performance evaluated using the area under the receiver operating characteristic curve (AUROC) and comparing observed and expected probabilities of extubation success, defined as survival ≥5 d without an endotracheal tube.
Results
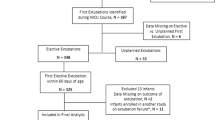
Of 177 infants, 120 (68%) were extubated successfully. The median (IQR) gestational age was 27 weeks (25–28) and weight at extubation was 915 g (755–1050). The model had acceptable discrimination (AUROC 0.72 [95% CI 0.65–0.80]) and adequate calibration (calibration slope 0.96, intercept -0.06, mean observed-to-expected difference in probability of extubation success −0.08 [95% CI −0.01, −0.15]).
Conclusions
The extubation success prediction model has acceptable performance in an external cohort. Additional prospective studies are needed to determine if the model can be improved or how it can be used for clinical benefit.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The corresponding author can be contacted for source data.
References
Walsh MC, Morris BH, Wrage LA, Vohr BR, Poole WK, Tyson JE, et al. Extremely low birthweight neonates with protracted ventilation: mortality and 18-month neurodevelopmental outcomes. J Pediatr. 2005;146:798–804.
Chawla S, Natarajan G, Shankaran S, Carper B, Brion LP, Keszler M, et al. Markers of successful extubation in extremely preterm infants, and morbidity after failed extubation. J Pediatr. 2017;189:113–9.e2.
Gupta D, Greenberg RG, Sharma A, Natarajan G, Cotten M, Thomas R, et al. A predictive model for extubation readiness in extremely preterm infants. J Perinatol. 2019;39:1663–9.
Collins GS, Reitsma JB, Altman DG, Moons KG. Transparent reporting of a multivariable prediction model for individual prognosis or diagnosis (TRIPOD): the TRIPOD statement. BMJ 2015;350:g7594.
Jensen EA, Dysart K, Gantz MG, McDonald S, Bamat NA, Keszler M, et al. The diagnosis of bronchopulmonary dysplasia in very preterm infants. an evidence-based approach. Am J Respir Crit Care Med. 2019;200:751–9.
Alba AC, Agoritsas T, Walsh M, Hanna S, Iorio A, Devereaux PJ, et al. Discrimination and calibration of clinical prediction models: users’ guides to the medical literature. JAMA 2017;318:1377–84.
Altman DG, Vergouwe Y, Royston P, Moons KG. Prognosis and prognostic research: validating a prognostic model. BMJ 2009;338:b605.
Kidman AM, Manley BJ, Boland RA, Davis PG, Bhatia R. Predictors and outcomes of extubation failure in extremely preterm infants. J Paediatr Child Health. 2021;57:913–9.
Perkins NJ, Schisterman EF. The Youden Index and the optimal cut-point corrected for measurement error. Biom J. 2005;47:428–41.
Swets JA. Measuring the accuracy of diagnostic systems. Science. 1988;240:1285–93.
Mandrekar JN. Receiver operating characteristic curve in diagnostic test assessment. J Thorac Oncol. 2010;5:1315–6.
Giaccone A, Jensen E, Davis P, Schmidt B. Definitions of extubation success in very premature infants: a systematic review. Arch Dis Child Fetal Neonatal Ed. 2014;99:F124–7.
Kent DM, van Klaveren D, Paulus JK, D’Agostino R, Goodman S, Hayward R, et al. The predictive approaches to treatment effect heterogeneity (PATH) statement: explanation and elaboration. Ann Intern Med. 2020;172:W1–25.
Ferguson KN, Roberts CT, Manley BJ, Davis PG. Interventions to improve rates of successful extubation in preterm infants: a systematic review and meta-analysis. JAMA Pediatr. 2017;171:165–74.
Author information
Authors and Affiliations
Contributions
BD conceived of and designed the study, acquired data and drafted the manuscript, AS and VS acquired data and critically revised the manuscript for important intellectual content, RG, MR, and SC guided analyses and interpretation of data and critically revised the manuscript for important intellectual content and RP conceived of and designed the study, analyzed the data, drafted the manuscript and provided study supervision.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
41372_2022_1517_MOESM2_ESM.pdf
Supplementary Table 2. Sensitivity, Specificity, Youden’s J and Euclidean Distance at Various Extubation Success Probability Thresholds
41372_2022_1517_MOESM5_ESM.pdf
Supplementary Figure 2. Optimal Cut-Point of Predicted Probability of Extubation Success using Youden’s J and Euclidean distance
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dryer, R.A., Salem, A., Saroha, V. et al. Evaluation and validation of a prediction model for extubation success in very preterm infants. J Perinatol 42, 1674–1679 (2022). https://doi.org/10.1038/s41372-022-01517-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-022-01517-z
This article is cited by
-
Peri-extubation settings in preterm neonates: a systematic review and meta-analysis
Journal of Perinatology (2024)