Abstract
Objective
To identify the relationship between prophylactic indomethacin (PI) administration and incidence of intraventricular hemorrhage.
Study design
A retrospective analysis of extremely premature infants <27 weeks gestational age born between January 2014 and September 2020.
Results
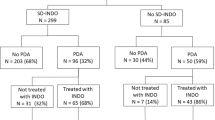
A total of 421 infants were included from three of Nationwide Children’s Hospital delivery centers. Of those 255 (61%) received PI. After adjustment by inverse proportionality treatment weighting (IPTW), no differences were found in incidence of intraventricular hemorrhage (IVH) at the time of the first ultrasound, 31% vs. 33% in PI and control groups respectively (p = 0.68). The rate of rise of serum creatinine from baseline to day of life four was significantly higher in the PI group (0.14 mg/dl PI and 0.03 mg/dl control, p < 0.001).
Conclusion
PI was not associated with any benefit in prevention of IVH, but is associated with adverse effects including acute rise in creatinine.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are not publicly available due patient privacy but are available from the corresponding author on reasonable request.
References
Leijser LM, de Vries LS. Chapter 8—Preterm brain injury: Germinal matrix–intraventricular hemorrhage and post-hemorrhagic ventricular dilatation. In: de Vries LS, Glass HC, editors. Handbook of clinical neurology. Vol 162. Elsevier: Cambridge, MA, 2019, pp 173–99.
Abdi HH, Backes CH, Ball MK, Barber MM, Klebanoff MA, Jadcherla SR, et al. Prophylactic Indomethacin in extremely preterm infants: association with death or BPD and observed early serum creatinine levels. J Perinatol. 2021;41:749–55.
Ballabh P. Intraventricular hemorrhage in premature infants: mechanism of disease. Pediatr Res. 2010;67:1–8.
Szpecht D, Szymankiewicz M, Nowak I, Gadzinowski J. Intraventricular hemorrhage in neonates born before 32 weeks of gestation-retrospective analysis of risk factors. Childs Nerv Syst. 2016;32:1399–404.
Ment LR, Oh W, Ehrenkranz RA, Philip AG, Vohr B, Allan W, et al. Low-dose indomethacin and prevention of intraventricular hemorrhage: a multicenter randomized trial. Pediatrics. 1994;93:543–50.
Schmidt B, Davis P, Moddemann D, Ohlsson A, Roberts RS, Saigal S, et al. Long-term effects of indomethacin prophylaxis in extremely-low-birth-weight infants. N Engl J Med. 2001;344:1966–72.
McCrea HJ, Ment LR. The diagnosis, management, and postnatal prevention of intraventricular hemorrhage in the preterm neonate. Clin Perinatol. 2008;35:777–92.
Ment LR, Stewart WB, Ardito TA, Huang E, Madri JA. Indomethacin promotes germinal matrix microvessel maturation in the newborn beagle pup. Stroke. 1992;23:1132–7.
Ment LR, Stewart WB, Duncan CC, Scott DT, Lambrecht R. Beagle puppy model of intraventricular hemorrhage. Effect of indomethacin on cerebral blood flow. J Neurosurg. 1983;58:857–62.
Fowlie PW, Davis PG. Prophylactic indomethacin for preterm infants: a systematic review and meta-analysis. Arch Dis Child Fetal Neonatal Ed. 2003;88:F464–6.
Nelin TD, Pena E, Giacomazzi T, Lee S, Logan JW, Moallem M, et al. Outcomes following indomethacin prophylaxis in extremely preterm infants in an all-referral NICU. J Perinatol. 2017;37:932–7.
Harris PA, Taylor R, Minor BL, Elliott V, Fernandez M, O’Neal L, et al. The REDCap consortium: building an international community of software platform partners. J Biomed Inf. 2019;95:103208.
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap)—a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inf. 2009;42:377–81.
Schmidt B, Asztalos EV, Roberts RS, Robertson CM, Sauve RS, Whitfield MF. Impact of bronchopulmonary dysplasia, brain injury, and severe retinopathy on the outcome of extremely low-birth-weight infants at 18 months: results from the trial of indomethacin prophylaxis in preterms. JAMA. 2003;289:1124–9.
Sardesai S, Biniwale M, Wertheimer F, Garingo A, Ramanathan R. Evolution of surfactant therapy for respiratory distress syndrome: past, present, and future. Pediatr Res. 2017;81:240–8.
Liebowitz M, Clyman RI. Prophylactic indomethacin compared with delayed conservative management of the patent ductus arteriosus in extremely preterm infants: effects on neonatal outcomes. J Pediatr. 2017;187:119–26.
Dipak NK, Nanavat RN, Kabra NK, Srinivasan A, Ananthan A. Effect of delayed cord clamping on hematocrit, and thermal and hemodynamic stability in preterm neonates: a randomized controlled trial. Indian Pediatr. 2017;54:112–5.
Roberts D, Brown J, Medley N, Dalziel SR. Antenatal corticosteroids for accelerating fetal lung maturation for women at risk of preterm birth. Cochrane Database Syst Rev. 2017;3:Cd004454.
Charpak N, Tessier R, Ruiz JG, Uriza F, Hernandez JT, Cortes D, et al. Kangaroo mother care had a protective effect on the volume of brain structures in young adults born preterm. Acta Paediatr. 2022;00:1–11.
Selewski DT, Charlton JR, Jetton JG, Guillet R, Mhanna M, Askenazi D, et al. Neonatal acute kidney injury. Pediatrics. 2015;136:e463–73.
Couser RJ, Ferrara TB, Wright GB, Cabalka AK, Schilling CG, Hoekstra RE, et al. Prophylactic indomethacin therapy in the first twenty-four hours of life for the prevention of patent ductus arteriosus in preterm infants treated prophylactically with surfactant in the delivery room. J Pediatr. 1996;128:631–7.
Akima S, Kent A, Reynolds G, Gallagher M, Falk M. Indomethacin and renal impairment in neonates. Pediatr Nephrol. 2004;19:490–3.
Shaffer CL, Gal P, Ransom JL, Carlos RQ, Smith MS, Davey AM, et al. Effect of age and birth weight on indomethacin pharmacodynamics in neonates treated for patent ductus arteriosus. Crit Care Med. 2002;30:343–8.
Jensen EA, Foglia EE, Schmidt B. Association between prophylactic indomethacin and death or bronchopulmonary dysplasia: a systematic review and meta-analysis of observational studies. Semin Perinatol. 2018;42:228–34.
Author information
Authors and Affiliations
Contributions
CJM and PP designed the study, collected, analyzed, interpreted the data, and drafted the manuscript. JM, MAR, and LDN designed the study, interpreted the data, and critically revised the manuscript for important intellectual content. KE, HS, and SS collected patient data and revised the manuscript for important intellectual content. All authors approved the final version of the manuscript to be published.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Miller, C.J., Prusakov, P., Magers, J. et al. Effects of prophylactic indomethacin on intraventricular hemorrhage and adverse outcomes in neonatal intensive care unit. J Perinatol 42, 1644–1648 (2022). https://doi.org/10.1038/s41372-022-01441-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-022-01441-2
This article is cited by
-
Prophylactic indomethacin and the risk of serious pulmonary hemorrhages in preterm infants less than 28 weeks’ gestation
Journal of Perinatology (2024)