Abstract
Background
There is limited information on pulseless electrical activity (PEA)/asystolic cardiac arrest (CA) in the infant population. The aim is to describe the incidence and factors associated with outcomes in infants with PEA/asystolic CA.
Methods
Single-center retrospective chart review study of infants less than one year of age who suffer in-hospital PEA/asystolic CA from January 1 2011 to June 30 2019. The primary outcome was the return of spontaneous circulation. The secondary outcome was survival to discharge.
Results
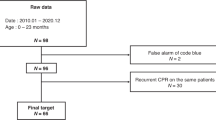
CA occurred in 148 infants and PEA/asystolic was found in 38 (26%). Of those 29 (76%) achieved ROSC, and 12 (32%) survived to discharge. Infants on inotrope support or receiving longer duration of chest compressions and epinephrine had increase mortality. All infants with respiratory etiology of arrest survived to hospital discharge.
Conclusion
PEA/asystolic CAs are uncommon. Poor prognostic indicators include the need for pre-arrest inotrope support and increased duration of chest compressions.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Berg RA, Nadkarni VM, Clark AE, Moler F, Meer K, Harrison RE, et al. Incidence and outcomes of cardiopulmonary resuscitation in PICUs. Crit Care Med. 2016;44:798–808.
Donoghue A, Berg RA, Hazinski MF, Praestgaard AH, Roberts K, Nadkarni VM. Cardiopulmonary resuscitation for bradycardia with poor perfusion versus pulseless cardiac arrest. Pediatrics. 2009;124:1541–8.
Holmberg MJ, Wiberg S, Ross CE, Kleinman M, Hoeyer-Nielsen AK, Donnino M, et al. Trends in survival after pediatric in-hospital cardiac arrest in the United States. Circulation. 2019;140:1398–408.
Ali N, Lam T, Gray MM, Clausen D, Riley M, Grover TR, et al. Cardiopulmonary resuscitation in quaternary neonatal intensive care units: a multicenter study. Resuscitation. 2021;159:77–84.
Foglia EE, Langeveld R, Heimall L, Heimall L, Deveney A, Ades A, et al. Incidence, characteristics, and survival following cardiopulmonary resuscitation in the quaternary neonatal intensive care unit. Resuscitation. 2017;110:32–6.
Ahmad KA, Velasquez SG, Kohlleppel KL, Henderson C, Stine C, LeVan J, et al. The characteristics and outcomes of cardiopulmonary resuscitation within the neonatal intensive care unit based on gestational age and unit level of care. Am J Perinatol. 2019;1. https://doi.org/10.1055/s-0039-1693990.
Topjian AA, Raymond TT, Atkins D, Chan M, Duff J, Joyner BL, et al. Part 4: pediatric basic and advanced life support: 2020 American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Circulation. 2020;142:s469–s523.
Weiner GM, Zaichkin J. Textbook of Neonatal Resuscitation (NRP). 8th ed. American Academy of Pediatrics and American Heart Association; 2021.
Sawyer T, Clark A, Ridout R. Infant resuscitation outside the delivery room in neonatal-perinatal and pediatric critical care fellowship programs: NRP or PALS? Results of a national survey. J Neonatal Perinat Med. 2009;2:95–102.
Ali N, Sawyer T, Barry J, Grover T, Ades A. Resuscitation practices for infants in the NICU, PICU and CICU: Results of a national survey. J Perinatol. 2017;37:172–6.
Morgan RW, Reeder RW, Meert KL, Telford R, Yates AR, Berger JT, et al. Survival and hemodynamics during pediatric cardiopulmonary resuscitation for bradycardia and poor perfusion versus pulseless cardiac arrest. Crit Care Med. 2020:1. https://doi.org/10.1097/ccm.0000000000004308.
Sillers L, Handley SC, James JR, Foglia EE. Pulseless electrical activity complicating neonatal resuscitation. Neonatology. 2019;115:95–98.
Luong D, Cheung PY, Barrington KJ, Davis P, Unrau J, Dakshinamurti S, et al. Cardiac arrest with pulseless electrical activity rhythm in newborn infants: a case series. Arch Dis Child Fetal Neonatal Ed. 2019;104:F572–F574.
Hyde P, Puddy V. Pulseless electrical activity after rapid administration of fresh frozen plasma. J Paediatr Child Health. 2008;44:464–6.
Polito A, Biasucci DG, Cogo P. Point-of-care pleural and lung ultrasound in a newborn suffering from cardiac arrest due to tension pneumothorax after cardiac surgery. Cardiol Young. 2015;26:400–2.
Raymond TT, Praestgaard A, Berg RA, Nadkarni VM, Parshuram CS. The association of hospital rate of delayed epinephrine administration with survival to discharge for pediatric nonshockable in-hospital cardiac arrest. Pediatr Crit Care Med. 2019;20:405–16.
Andersen LW, Berg KM, Saindon BZ, Massaro JM, Raymond TT, Berg RA, et al. Time to epinephrine and survival after pediatric in-hospital cardiac arrest. JAMA—J Am Med Assoc. 2015;314:802–10.
del Castillo J, López-Herce J, Canadas S, Matamoros M, Rodriguez-Nunez A, Rodriguez-Calvo A, et al. Cardiac arrest and resuscitation in the pediatric intensive care unit: a prospective multicenter multinational study. Resuscitation. 2014;85:1380–6.
Handley SC, Passarella M, Raymond TT, Lorch SA, Ades A, Foglia EE Epidemiology and outcomes of infants after cardiopulmonary resuscitation in the Neonatal and Pediatric Intensive Care Unit from a National Registry. Resuscitation. 2021. https://doi.org/10.1016/j.resusitation.2021.05.029.
Parish DC, Goyal H, Dane FC. Mechanism of dealth: there’s more to it than sudden cardiac arrest. J Thorac Dis. 2018;10:3081–7.
Gazmuri RJ, Radhakrishnan J Protecting mitochondrial bioenergetic function during resuscitation from cardiac arrest. Crit Care Clin. 2012. https://doi.org/10.1016/j.ccc.2021.02.001.
Vali P, Chandrasekharan P, Rawat M, Gugino S, Koeninsknecht C, Helman J, et al. Evaluation of timing and route of epinephrine in a neonatal model of asphyxial arrest. J Am Heart Assoc. 2017. https://doi.org/10.1161/JAHA.116.004402.
Raymond TT, Stromberg D, Stigall W, Burton G, Zaritsky A. Sodium bicarbonate use during in-hospital pediatric pulseless cardiac arrest—a report from the American Heart Association Get With The Guidelines—Resuscitation. Resuscitation. 2015;89:106–13.
Murthy K, Dykes FD, Padula MA, Pallotto EK, Reber KM, Durand DJ, et al. The Children’s Hospitals Neonatal Database: an overview of complexity, outcomes and variation in care. J Perinatol. 2014;34:582–6.
McCrory MC, Spaeder MC, Gower EW, Nakagawa TA, Simpson SL, Coleman MA, et al. Time of admission to the PICU and mortality. Pediatr Crit Care Med. 2017;18:915–23.
Authors contributors
KB and NA conceptualized and designed the study, drafted the initial manuscript and reviewed the manuscript. MHW helped with the study design and critically reviewed the manuscript. RH and ES analyzed the data and critically reviewed the manuscript. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Best, K., Wyckoff, M.H., Huang, R. et al. Pulseless electrical activity and asystolic cardiac arrest in infants: identifying factors that influence outcomes. J Perinatol 42, 574–579 (2022). https://doi.org/10.1038/s41372-022-01349-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-022-01349-x
This article is cited by
-
Unveiling pseudo-pulseless electrical activity (pseudo-PEA) in ultrasound-integrated infant resuscitation
European Journal of Pediatrics (2023)