Abstract
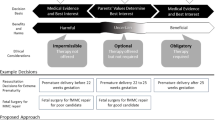
As the field of fetal intervention grows, novel ethical tensions will arise. We present a case of Fetal myelomeningocele repair involving a 25-week fetus where parents requested that if emergent delivery was necessary during the open uterine procedure, that the medical team did not perform resuscitation. This question brings forward an important discussion around the complicated space of maternal autonomy, child rights, and clinician obligations that exists in fetal intervention. In some regions, a mother in this situation may choose to terminate the pregnancy. Parents could also choose not to do the surgery. Parents in some regions could opt for no resuscitation of a child born at 25-weeks’ gestation. We offer an analysis of these relevant considerations, the different tensions, and the conflicting duties between the mother, fetus, and medical team. This analysis will provide ethical and clinical guidance for future questions that may arise in this burgeoning field.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Jatlaoui TC, Shah J, Mandel MG, Reeves JA, Oduyebo T, Petersen E, et al. Abortion surveillance—United States, 2014. MMWR Surveill Summ. 2018;66:1–29.
Guttmacher Institute. State bans on abortion throughout pregnancy. 2021. www.guttmacher.org. Accessed 1st, May 2021. https://www.guttmacher.org/state-policy/explore/state-policies-later-abortions
Adzick NS, Thom EA, Spong CY, Brock JW III, Burrows PK, Johnson MP, et al. A randomized trial of prenatal versus postnatal repair of myelomeningocele. N. Engl J Med. 2011;364:993–1004.
Heuer GG, Moldenhauer JS, Adzick NS. Prenatal surgery for myelomeningocele: review of the literature and future directions. Child Nerv Syst. 2017;33:1149–55.
Moron AF, Barbosa MM, Milani HJF, Sarmento SG, Santana EF, Suriano IC, et al. Perinatal outcomes after open fetal surgery for myelomeningocele repair: a retrospective cohort study. BJOG-Int J Obstet Gy. 2018;125:280–1286.
Farmer DL, Thom EA, Brock JW III, Burrows PK, Johnson MP, Howell LJ, et al. The management of myelomeningocele study: full cohort 30-month pediatric outcomes. Am J Obstet Gynecol. 2018;218:256.e1–256.e13.
Houtrow AJ, MacPherson C, Jackson-Coty J, Rivera M, Flynn L, Burrows PK, et al. Prenatal repair and physical functioning among children with myelomeningocele: a secondary analysis of a randomized clinical trial. JAMA Pediatr. 2021;175:e205674–e205674.
Kopelman LM. The best-interests standard as threshold, ideal, and standard of reasonableness. J Med Philos. 1997;22:271–89.
Diekema D. Parental refusals of medical treatment: the harm principle as threshold for state intervention. Theor Med Bioeth. 2004;25:243–64.
Gillam L. The zone of parental discretion: an ethical tool for dealing with disagreement between parents and doctors about medical treatment for a child. Clin Ethics. 2016;11:1–8.
Perinatal Palliative Care. ACOG committee opinion, Number 786. Obstet Gynecol. 2019;134:e84–e89.
Verhagen E, Sauer PJJ. The Groningen protocol — euthanasia in severely ill newborns. N. Engl J Med. 2005;352:959–62.
Hendriks MJ, Lantos JD. Fragile lives with fragile rights: Justice for babies born at the limit of viability. Bioethics 2018;32:205–14.
Rysavy MA, Mehler K, Oberthür A, Agren J, Kusuda S, McNamara PJ, et al. An immature science: intensive care for infants born at ≤23 weeks of gestation. J Pediatr. 2021;233:16–25.
Kono Y, Rysavy MA, Nakanishi H, Kusuda S. Outcomes of infants born at periviable gestations in Japan. Acta Paediatr. 2021;110:1694–1695.
Kaempf JW, Tomlinson M, Arduza C, Anderson S, Campbell B, Ferguson LA, et al. Medical staff guidelines for periviability pregnancy counseling and medical treatment of extremely premature infants. Pediatrics 2006;117:22–29.
Kaempf JW, Tomlinson MW, Tuohey J. Extremely premature birth and the choice of neonatal intensive care versus palliative comfort care: an 18-year single-center experience. J Perinatol. 2016;36:190–195.
Cummings J. Antenatal counseling regarding resuscitation and intensive care before 25 weeks of gestation. Pediatrics 2015;136:588–95.
Watkins PL, Dagle JM, Bell EF, Colaizy TT. 2020. Outcomes at 18 to 22 months of corrected age for infants born at 22 to 25 weeks of gestation in a center practicing active management. J Pediatr. 2020;217:52–58.
Berry MJ, Port LJ, Gately C, Stringer MD. Outcomes of infants born at 23 and 24 weeks’ gestation with gut perforation. J Pediatr Surg. 2019;54:2092–2098.
Mercurio MR, Carter BS. Resuscitation policies for extremely preterm newborns: finally moving beyond gestational age. J Perinatol. 2020;2020:1731–1733.
Krick JA, Hogue JS, Reese TR, Studer MA. Uncertainty: an uncomfortable companion to decision-making for infants. Pediatrics 2020;146:S13–7.
Hoagland MA, Chatterjee D. Anesthesia for fetal surgery. Pediatr Anesthesia. 2017;27:346–57. https://doi.org/10.1111/pan.13109.
Rychik J, Cohen D, Tran KM, Szwast A, Natarajan SS, Johnson MP, et al. The role of echocardiography in the intraoperative management of the fetus undergoing myelomeningocele repair. Fetal diagnosis Ther. 2015;37:172–178. pp
Handley SC, Sun Y, Wyckoff MH, Lee HC. Outcomes of extremely preterm infants after delivery room cardiopulmonary resuscitation in a population-based cohort. J Perinatol. 2015;35:379–83.
American Society of Anesthesiologists, Ethics Committee. “Ethical guidelines for the anesthesia care of patients with do-not-resuscitate orders or other directives that limit treatment.” Approved 17 October 2001. Last amended 16 October 2013, reaffirmed 17 October 2018. Accessed 2 June 2021. https://www.asahq.org/~/media/sites/asahq/files/public/resources/standards-guidelines/ethical-guidelines-for-the-anesthesia-care-of-patients.pdf
Fallat ME, Deshpande JK. Do-not-resuscitate orders for pediatric patients who require anesthesia and surgery. Pediatrics 2004;114:1686–92.
Jackson S. Perioperative do-not-resuscitate orders. AMA J Ethics. 2015;17:229–35.
Burkle CM, Swetz KM, Armstrong MH, Keegan MT. Patient and doctor attitudes and beliefs concerning perioperative do not resuscitate orders: anesthesiologists’ growing compliance with patient autonomy and self determination guidelines. BMC Anesthesiol. 2013;13:1–7.
Nurok M, Green DS, Chisholm MF, Fins JJ, Liguori GA. Anesthesiologists’ familiarity with the ASA and ACS guidelines on Advance Directives in the perioperative setting. J Clin Anesth. 2014;26:174–176.
Chervenak FA, McCullough LB. The fetus as a patient: an essential ethical concept for maternal-fetal medicine. J Matern Fetal Med. 1996;5:115–119.
Chervenak FA, McCullough LB. The fetus as a patient: an essential concept for the ethics of perinatal medicine. J Perinatol. 2003;20:399–404.
Chervenak FA, McCullough LB. Perinatal ethics: a practical method of analysis of obligations to mother and fetus. Obstet Gynecol. 1985;66:442–446.
Sacco A, Van der Veeken L, Bagshaw E, Ferguson C, Van Mieghem T, David AL, et al. Maternal complications following open and fetoscopic fetal surgery: a systematic review and meta‐analysis. Prenat Diagn. 2019;39:251–268.
Funding
No funding was received for this paper.
Author information
Authors and Affiliations
Contributions
IDW conceptualized and drafted the initial paper. JBL and BSC contributed to the drafting, design, and content of the paper. All authors contributed to review and revision of the paper and approve the final version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wolfe, I.D., Lillegard, J.B. & Carter, B.S. Parental request for non-resuscitation in fetal myelomeningocele repair: an analysis of the novel ethical tensions in fetal intervention. J Perinatol 42, 856–859 (2022). https://doi.org/10.1038/s41372-022-01317-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-022-01317-5
This article is cited by
-
Resuscitation decisions in fetal myelomeningocele repair should center on parents’ values: a counter analysis
Journal of Perinatology (2022)