Abstract
Introduction
No studies have determined if there is a threshold whereby use of mother’s own milk (MOM) during hospitalization predicts exclusive MOM feeding at discharge.
Methods
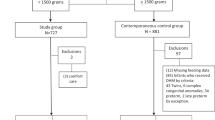
Among 113 very low birthweight neonates, the ratio of MOM to enteral feeds was measured in the first 14 days, 28 days, and overall hospital stay. The primary outcome was exclusive MOM feeding at discharge.
Results
For every 1% increase in MOM consumption in the first 14 and 28 days, the odds of being discharge home on an exclusive MOM diet increased nearly 7-fold (OR 7.01, 95% CI: 2.09–23.50) and 17-fold (OR 17.46, 95% CI 4.67–63.31), respectively. A threshold of >50%, >83%, and >85% MOM consumption compared to overall enteral feeds in the first 14 days, 28 days, and throughout hospitalization, respectively, is recommended.
Conclusions
Promotion of MOM consumption in the first 2–4 weeks is of paramount importance, with negligible impact of increasing MOM consumption after 28 days.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others

References
Section on Breastfeeding. Breastfeeding and the use of human milk. Pediatrics. 2012;129:e827–41. https://doi.org/10.1542/peds.2011-3552.
Gartner LM, Morton J, Lawrence RA, Naylor AJ, O’Hare D, Schanler RJ, et al. Breastfeeding and the use of human milk. Pediatrics. 2005;115:496–506. https://doi.org/10.1542/peds.2004-2491
Zutavern A, Brockow I, Schaaf B, Bolte G, von Berg A, Diez U, et al. Timing of solid food introduction in relation to atopic dermatitis and atopic sensitization: results from a prospective birth cohort study. Pediatrics. 2006;117:401–11. https://doi.org/10.1542/peds.2004-2521
Barclay AR, Russell RK, Wilson ML, Gilmour WH, Satsangi J, Wilson DC. Systematic review: the role of breastfeeding in the development of pediatric inflammatory bowel disease. J Pediatr. 2009;155:421–6. https://doi.org/10.1016/j.jpeds.2009.03.017.
Rosenbauer J, Herzig P, Giani G. Early infant feeding and risk of type 1 diabetes mellitus-a nationwide population-based case-control study in pre-school children. Diabetes Metab Res Rev. 2008;24:211–22. https://doi.org/10.1002/dmrr.791
Das UN. Breastfeeding prevents type 2 diabetes mellitus: but, how and why? Am J Clin Nutr. 2007;85:1436–7. https://doi.org/10.1093/ajcn/85.5.1436
Ip S, Chung M, Raman G, Chew P, Magula N, DeVine D, et al. Breastfeeding and maternal and infant health outcomes in developed countries. Evid Rep Technol Assess (Full Rep). 2007:1–186.
Ip S, Chung M, Raman G, Trikalinos TA, Lau J. A summary of the Agency for Healthcare Research and Quality’s evidence report on breastfeeding in developed countries. Breastfeed Med. 2009;4(Suppl 1):S17–30. https://doi.org/10.1089/bfm.2009.0050.
Committee on Nutrition; Section on Breastfeeding; Committee on Fetus and Newborn. Donor human milk for the high-risk infant: preparation, safety, and usage options in the United States. Pediatrics. 2017;139:e20163440 https://doi.org/10.1542/peds.2016-3440
Section on Breastfeeding. Breastfeeding and the use of human milk. Pediatrics. 2012;129:e827–41. https://doi.org/10.1542/peds.2011-3552.
Demers-Mathieu V, Huston RK, Markell AM, McCulley EA, Martin RL, Spooner M, et al. Differences in maternal immunoglobulins within mother’s own breast milk and donor breast milk and across digestion in preterm infants. Nutrients. 2019;11:920 https://doi.org/10.3390/nu11040920
García-Lara NR, Vieco DE, De la Cruz-Bértolo J, Lora-Pablos D, Velasco NU, Pallás-Alonso CR. Effect of Holder pasteurization and frozen storage on macronutrients and energy content of breast milk. J Pediatr Gastroenterol Nutr. 2013;57:377–82. https://doi.org/10.1097/MPG.0b013e31829d4f82
García-Lara NR, Escuder-Vieco D, García-Algar O, De la Cruz J, Lora D, Pallás-Alonso C. Effect of freezing time on macronutrients and energy content of breastmilk. Breastfeed Med. 2012;7:295–301. https://doi.org/10.1089/bfm.2011.0079.
Silvestre D, Miranda M, Muriach M, Almansa I, Jareño E, Romero FJ. Antioxidant capacity of human milk: effect of thermal conditions for the pasteurization. Acta Paediatr. 2008;97:1070–4. https://doi.org/10.1111/j.1651-2227.2008.00870.x.
Meier P, Patel A, Esquerra-Zwiers A. Donor human milk update: evidence, mechanisms, and priorities for research and practice. J Pediatr. 2017;180:15–21. https://doi.org/10.1016/j.jpeds.2016.09.027.
Hair AB, Rechtman DJ, Lee ML, Niklas V. Beyond necrotizing enterocolitis: other clinical advantages of an exclusive human milk diet. Breastfeed Med. 2018;13:408–11. https://doi.org/10.1089/bfm.2017.0192.
Hair AB, Peluso AM, Hawthorne KM, Perez J, Smith DP, Khan JY, et al. Beyond necrotizing enterocolitis prevention: improving outcomes with an exclusive human milk-based diet. Breastfeed Med. 2016;11:70–4. https://doi.org/10.1089/bfm.2015.0134. Erratum in: Breastfeed Med. 2017;12:663
Herrmann K, Carroll K. An exclusively human milk diet reduces necrotizing enterocolitis. Breastfeed Med. 2014;9:184–90. https://doi.org/10.1089/bfm.2013.0121.
Tyson JE, Parikh NA, Langer J, Green C, Higgins RD, National Institute of Child Health and Human Development Neonatal Research Network. Intensive care for extreme prematurity—moving beyond gestational age. N Engl J Med. 2008;358:1672–81. https://doi.org/10.1056/NEJMoa073059
Lee HC, Green C, Hintz SR, Tyson JE, Parikh NA, Langer J, et al. Prediction of death for extremely premature infants in a population-based cohort. Pediatrics. 2010;126:e644–50. https://doi.org/10.1542/peds.2010-0097.
Boland RA, Davis PG, Dawson JA, Doyle LW; Victorian Infant Collaborative Study Group. Predicting death or major neurodevelopmental disability in extremely preterm infants born in Australia. Arch Dis Child Fetal Neonatal Ed. 2013;98:F201–4. https://doi.org/10.1136/archdischild-2012-301628.
Ford SL, Lohmann P, Preidis GA, Gordon PS, O’Donnell A, Hagan J, et al. Improved feeding tolerance and growth are linked to increased gut microbial community diversity in very-low-birth-weight infants fed mother’s own milk compared with donor breast milk. Am J Clin Nutr. 2019;109:1088–97. https://doi.org/10.1093/ajcn/nqz006.
Whichelow MJ. Factors associated with the duration of breast feeding in a privileged society. Early Hum Dev. 1982;7:273–80. https://doi.org/10.1016/0378-3782(82)90090-1.
Chapman DJ, Pérez-Escamilla R. Identification of risk factors for delayed onset of lactation. J Am Diet Assoc. 1999;99:450–4. https://doi.org/10.1016/S0002-8223(99)00109-1. quiz455–6
Hurst NM. Recognizing and treating delayed or failed lactogenesis II. J Midwifery Womens Health. 2007;52:588–94. https://doi.org/10.1016/j.jmwh.2007.05.005
Hurst N, Engebretson J, Mahoney JS. Providing mother’s own milk in the context of the NICU: a paradoxical experience. J Hum Lact. 2013;29:366–73. https://doi.org/10.1177/0890334413485640.
Tshamala D, Pelecanos A, Davies MW. Factors associated with infants receiving their mother’s own breast milk on discharge from hospital in a unit where pasteurised donor human milk is available. J Paediatr Child Health. 2018;54:1016–22. https://doi.org/10.1111/jpc.14062.
Hill PD, Aldag JC. Milk volume on day 4 and income predictive of lactation adequacy at 6 weeks of mothers of nonnursing preterm infants. J Perinat Neonatal Nurs. 2005;19:273–82. https://doi.org/10.1097/00005237-200507000-00014
Parker LA, Sullivan S, Kruger C, Mueller M. Timing of milk expression following delivery in mothers delivering preterm very low birth weight infants: a randomized trial. J Perinatol. 2020;40:1236–45. https://doi.org/10.1038/s41372-020-0688-z.
Kent JC, Prime DK, Garbin CP. Principles for maintaining or increasing breast milk production. J Obstet Gynecol Neonatal Nurs. 2012;41:114–21. https://doi.org/10.1111/j.1552-6909.2011.01313.x.
Meier PP, Engstrom JL, Patel AL, Jegier BJ, Bruns NE. Improving the use of human milk during and after the NICU stay. Clin Perinatol. 2010;37:217–45. https://doi.org/10.1016/j.clp.2010.01.013
Meier PP, Engstrom JL. Evidence-based practices to promote exclusive feeding of human milk in very low-birthweight infants. NeoReviews. 2007;8:e467–77. https://doi.org/10.1542/neo.8-11-e467
Patel AL, Schoeny ME, Hoban R, Johnson TJ, Bigger H, Engstrom JL, et al. Mediators of racial and ethnic disparity in mother’s own milk feeding in very low birth weight infants. Pediatr Res. 2019;85:662–70. https://doi.org/10.1038/s41390-019-0290-2. Erratum in: Pediatr Res. 2019.
Funding
Evangelina “Evie” Whitlock Grant at Texas Children’s Hospital, Clinical Research Center, Texas Children’s Hospital.
Author information
Authors and Affiliations
Contributions
GV conceptualized the manuscript, performed the literature search, revised the drafted manuscript, and approved the final manuscript for submission. SF collected the data and reviewed and edited the final manuscript for submission. JH, NH, KA, and AH conceptualized the study and manuscript, revised the drafted manuscript, and approved the final manuscript for submission. JC and HY performed data extraction, revised the manuscript, and approved the final manuscript for submission. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Valentine, G., Ford, S., Hagan, J. et al. Percent mother’s own milk feedings for preterm neonates predicts discharge feeding outcomes. J Perinatol 41, 2766–2773 (2021). https://doi.org/10.1038/s41372-021-01205-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-021-01205-4