Abstract
Objectives
To identify the prevalence and risk factors for childhood overweight and obesity (OWO) at 3-year corrected age in children born <1500 g <29 weeks gestation.
Study design
A multicentre retrospective cohort study for preterm infants admitted to neonatal intensive care units between 2001 and 2014.
Results
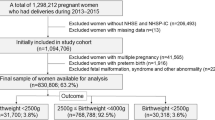
Data were available for 911 (89.4%) of the 1019 infants who met the inclusion criteria. Of them, 22 (2.4%) had OWO. There were no associations between OWO and being small for gestational age (RR = 1.3, 95% confidence interval (CI): 0.3–5.4) or weight <10th percentile at 36 weeks (RR = 1.1, 95% CI: 0.4–2.8). OWO was associated with low maternal education (RR = 7.4, 95% CI: 2.1–26), maternal diabetes (RR = 5.2, 95% CI: 1.9–15) and neonatal brain injury (RR = 4.9, 95% CI: 1.8–14). Adjusting for concurrent child weight at 3 years of age resulted in an overadjustment bias.
Conclusion
Small size at birth or at 36 weeks gestation in extremely preterm infants is not associated with increased risk of early childhood overgrowth or obesity.
Clinical trial registration
NCT03064022.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
GBD 2015 Obesity Collaborators, Afshin A, Forouzanfar MH, Reitsma MB, Sur P, Estep K, et al. Health effects of overweight and obesity in 195 countries over 25 years. N Engl J Med. 2017;377:13–27.
Jayedi A, Rashidy-Pour A, Khorshidi M, Shab-Bidar S. Body mass index, abdominal adiposity, weight gain and risk of developing hypertension: a systematic review and dose-response meta-analysis of more than 2.3 million participants. Obes Rev. 2018;19:654–67.
Cloostermans L, Wendel-Vos W, Doornbos G, Howard B, Craig CL, Kivimäki M, et al. Independent and combined effects of physical activity and body mass index on the development of Type 2 Diabetes—a meta-analysis of 9 prospective cohort studies. Int J Behav Nutr Phys Act. 2015;12:147.
Singhal A. Long-term adverse effects of early growth acceleration or catch-up growth. Ann Nutr Metab. 2017;70:236–40.
Singhal A. Early life origins of obesity and related complications. Indian J Pediatr. 2018;85:472–7.
Muelbert M, Harding JE, Bloomfield FH. Nutritional policies for late preterm and early term infants—can we do better? Semin Fetal Neonatal Med. 2019;24:43–7.
Strydom K, Van Niekerk E, Dhansay MA. Factors affecting body composition in preterm infants: assessment techniques and nutritional interventions. Pediatr Neonatol. 2019;60:121–8.
Gluckman PD, Hanson MA, Cooper C, Thornburg KL. Effect of in utero and early-life conditions on adult health and disease. N Engl J Med. 2008;359:61–73.
Hay WW. Strategies for feeding the preterm infant. Neonatology. 2008;94:245–54.
Fenton TR, Cormack B, Goldberg D, Nasser R, Alshaikh B, Eliasziw M, et al. “Extrauterine growth restriction” and “postnatal growth failure” are misnomers for preterm infants. J Perinatol. 2020;40:704–14.
Lin L, Crowther C, Gamble G, Bloomfield F, Harding JE, ESSENCE IPD-MA Group. Sex-specific effects of nutritional supplements in infants born early or small: protocol for an individual participant data meta-analysis (ESSENCE IPD-MA). BMJ Open. 2020;10:e033438.
Sutherland M, Ryan D, Black MJ, Kent AL. Long-term renal consequences of preterm birth. Clin Perinatol. 2014;41:561–73.
Fenton TR, Nasser R, Eliasziw M, Kim JH, Bilan D, Sauve R. Validating the weight gain of preterm infants between the reference growth curve of the fetus and the term infant. BMC Pediatr. 2013;13:92.
Fenton TR, Kim JH. A systematic review and meta-analysis to revise the Fenton growth chart for preterm infants. BMC Pediatr. 2013;13:59.
Fenton TR, Chan HT, Madhu A, Griffin IJ, Hoyos A, Ziegler EE, et al. Preterm infant growth velocity calculations: a systematic review. Pediatrics. 2017;139:e20162045.
World Health Organization. Interpreting indicators. Training course on child growth assessment. Geneva: WHO; 2008. Available from: https://www.who.int/nutrition/publications/childgrowthstandards_trainingcourse/en/.
Benavente-Fernández I, Synnes A, Grunau RE, Chau V, Ramraj C, Glass T, et al. Association of socioeconomic status and brain injury with neurodevelopmental outcomes of very preterm children. JAMA Netw Open. 2019;2:e192914.
Yusuf ZI, Dongarwar D, Yusuf RA, Bell M, Harris T, Salihu HM. Social determinants of overweight and obesity among children in the United States. Int J MCH AIDS. 2020;9:22–33.
de Onis M, Onyango AW, Borghi E, Siyam A, Nishida C, Siekmann J. Development of a WHO growth reference for school-aged children and adolescents. Bull World Health Organ. 2007;85:660–7.
Olsen IE, Lawson ML, Ferguson AN, Cantrell R, Grabich SC, Zemel BS, et al. BMI curves for preterm infants. Pediatrics. 2015;135:e572–81.
Richardson DK, Corcoran JD, Escobar GJ, Lee SK. SNAP-II and SNAPPE-II: simplified newborn illness severity and mortality risk scores. J Pediatr. 2001;138:92–100.
Agostoni C, Buonocore G, Carnielli VP, De Curtis M, Darmaun D, Decsi T, et al. Enteral nutrient supply for preterm infants: commentary from the European Society of Paediatric Gastroenterology, Hepatology and Nutrition Committee on Nutrition. J Pediatr Gastroenterol Nutr. 2010;50:85–91.
American Academy Pediatrics Committee on Nutrition. Nutritional needs of preterm infants. In: Kleinman RE, Greer FR, editors. Pediatric nutrition handbook. 8th ed. Itasca, IL: American Academy of Pediatrics; 2020.
Gidrewicz DA, Fenton TR. A systematic review and meta-analysis of the nutrient content of preterm and term breast milk. BMC Pediatr. 2014;14:216.
Saarela T, Kokkonen J, Koivisto M. Macronutrient and energy contents of human milk fractions during the first six months of lactation. Acta Paediatr. 2005;94:1176–81.
Thomas MR, Chan GM, Book LS. Comparison of macronutrient concentration of preterm human milk between two milk expression techniques and two techniques for quantitation of energy. J Pediatr Gastroenterol Nutr. 1986;5:597–601.
Meredith-Dennis L, Xu G, Goonatilleke E, Lebrilla CB, Underwood MA, Smilowitz JT. Composition and variation of macronutrients, immune proteins, and human milk oligosaccharides in human milk from nonprofit and commercial milk banks. J Hum Lact. 2018;34:120–9.
Greenland S, Rothman KJ, Lash LT. Introduction to categorical statistics. In: Rothman KJ, Greenland S, Lash TL, editors. Epidemiology M. 3rd ed. Wolters Kluwer Philadelphia PA USA; 2008.
Kramer MS, Zhang X, Dahhou M, Yang S, Martin RM, Oken E, et al. Does fetal growth restriction cause later obesity? Pitfalls in analyzing causal mediators as confounders. Am J Epidemiol. 2017;185:585–90.
Vittinghoff E, McCulloch CE. Relaxing the rule of ten events per variable in logistic and Cox regression. Am J Epidemiol. 2007;165:710–8.
Wood CL, Tinnion RJ, Korada SM, Cheetham TD, Relton CL, Cooke RJ, et al. Growth and metabolic outcome in adolescents born preterm (GROWMORE): follow-up protocol for the Newcastle Preterm Birth GRowth study (PTBGS). BMC Pediatr. 2013;13:213.
Gaskins RB, LaGasse LL, Liu J, Shankaran S, Lester BM, Bada HS, et al. Small for gestational age and higher birth weight predict childhood obesity in preterm infants. Am J Perinatol. 2010;27:721–30.
Singhal A, Cole TJ, Fewtrell M, Deanfield J, Lucas A. Is slower early growth beneficial for long-term cardiovascular health? Circulation. 2004;109:1108–13.
Crume TL, Scherzinger A, Stamm E, McDuffie R, Bischoff KJ, Hamman RF, et al. The long-term impact of intrauterine growth restriction in a diverse U.S. cohort of children: the EPOCH study. Obesity. 2014;22:608–15.
Zozaya C, Díaz C, Saenz de Pipaón M. How should we define postnatal growth restriction in preterm infants? Neonatology. 2018;114:177–80.
Shah PS, Wong KY, Merko S, Bishara R, Dunn M, Asztalos E, et al. Postnatal growth failure in preterm infants: ascertainment and relation to long-term outcome. J Perinat Med. 2006;34:484–9.
Hack M, Merkatz IR, Gordon D, Jones PK, Fanaroff AA. The prognostic significance of postnatal growth in very low-birth weight infants. Am J Obstet Gynecol. 1982;143:693–9.
Rochow N, Raja P, Liu K, Fenton T, Landau-Crangle E, Göttler S, et al. Physiological adjustment to postnatal growth trajectories in healthy preterm infants. Pediatr Res. 2016;79:870–9.
Rahman A, Kase JS, Murray YL, Parvez B. Neurodevelopmental outcome of extremely low birth weight infants fed an exclusive human milk diet is not affected by growth velocity. Breastfeed Med. 2020;15:362–9.
Andrea SB, Hooker ER, Messer LC, Tandy T, Boone-Heinonen J. Does the association between early life growth and later obesity differ by race/ethnicity or socioeconomic status? A systematic review. Ann Epidemiol. 2017;27:583–92.
Hayes JF, Eichen DM, Barch DM, Wilfley DE. Executive function in childhood obesity: promising intervention strategies to optimize treatment outcomes. Appetite. 2018;124:10–23.
Pieper JR, Laugero KD. Preschool children with lower executive function may be more vulnerable to emotional-based eating in the absence of hunger. Appetite. 2013;62:103–9.
Kong L, Nilsson IAK, Gissler M, Lavebratt C. Associations of maternal diabetes and body mass index with offspring birth weight and prematurity. JAMA Pediatr. 2019;173:371–8.
Pai VV, Carmichael SL, Kan P, Leonard SA, Lee HC. Maternal body mass index and risk of intraventricular hemorrhage in preterm infants. Pediatr Res. 2018;83:1146–51.
Hadjiyannakis S, Buchholz A, Chanoine J-P, Jetha MM, Gaboury L, Hamilton J, et al. The Edmonton obesity staging system for pediatrics: a proposed clinical staging system for paediatric obesity. Paediatr Child Health. 2016;21:21–6.
Tu Y-K, West R, Ellison GTH, Gilthorpe MS. Why evidence for the fetal origins of adult disease might be a statistical artifact: the “reversal paradox” for the relation between birth weight and blood pressure in later life. Am J Epidemiol. 2005;161:27–32.
Breukhoven PE, Kerkhof GF, Willemsen RH, Hokken-Koelega ACS. Fat mass and lipid profile in young adults born preterm. J Clin Endocrinol Metab. 2012;97:1294–302.
Schisterman EF, Cole SR, Platt RW. Overadjustment bias and unnecessary adjustment in epidemiologic studies. Epidemiology. 2009;20:488–95.
Huxley R, Neil A, Collins R. Unravelling the fetal origins hypothesis: is there really an inverse association between birthweight and subsequent blood pressure? Lancet. 2002;360:659–65.
Fairchild AJ, McDaniel HL. Best (but oft-forgotten) practices: mediation analysis. Am J Clin Nutr. 2017;105:1259–71.
Ananth CV, Schisterman EF. Confounding, causality, and confusion: the role of intermediate variables in interpreting observational studies in obstetrics. Am J Obstet Gynecol. 2017;217:167–75.
Williams TC, Bach CC, Matthiesen NB, Henriksen TB, Gagliardi L. Directed acyclic graphs: a tool for causal studies in paediatrics. Pediatr Res. 2018;84:487–93.
Porta M. Dictionary of epidemiology. 6th ed. New York, NY: Oxford University Press; 2014.
Belfort MB, Kuban KCK, O’Shea TM, Allred EN, Ehrenkranz RA, Engelke SC, et al. Weight status in the first 2 years of life and neurodevelopmental impairment in extremely low gestational age newborns. J Pediatr. 2016;168:30–5.
Vohr BR, Heyne R, Bann CM, Das A, Higgins RD, Hintz SR, et al. Extreme preterm infant rates of overweight and obesity at school age in the SUPPORT neuroimaging and neurodevelopmental outcomes cohort. J Pediatr. 2018;200:132–9.
Huke V, Rudloff S, Brugger M, Strauch K, Berthold LD, Landmann E. Prematurity is not associated with intra-abdominal adiposity in 5- to 7-year-old children. J Pediatr. 2013;163:1301–6.
Giannì ML, Roggero P, Piemontese P, Morlacchi L, Bracco B, Taroni F, et al. Boys who are born preterm show a relative lack of fat-free mass at 5 years of age compared to their peers. Acta Paediatr. 2015;104:e119–23.
Wood CT, Linthavong O, Perrin EM, Leviton A, Allred EN, Kuban KCK, et al. Antecedents of obesity among children born extremely preterm. Pediatrics. 2018;142:e20180519.
Roberts G, Cheong J, Opie G, Carse E, Davis N, Duff J, et al. Growth of extremely preterm survivors from birth to 18 years of age compared with term controls. Pediatrics. 2013;131:e439–45.
Saigal S, Stoskopf B, Streiner D, Paneth N, Pinelli J, Boyle M. Growth trajectories of extremely low birth weight infants from birth to young adulthood: a longitudinal, population-based study. Pediatr Res. 2006;60:751–8.
Novotny R, Fialkowski MK, Li F, Paulino Y, Vargo D, Jim R, et al. Systematic review of prevalence of young child overweight and obesity in the United States-affiliated pacific region compared with the 48 contiguous states: the Children’s Healthy Living Program. Am J Public Health. 2015;105:e22–35.
Clayborne ZM, Giesbrecht GF, Bell RC, Tomfohr-Madsen LM. Relations between neighbourhood socioeconomic status and birth outcomes are mediated by maternal weight. Soc Sci Med. 2017;175:143–51.
Cameron AJ, Spence AC, Laws R, Hesketh KD, Lioret S, Campbell KJ. A review of the relationship between socioeconomic position and the early-life predictors of obesity. Curr Obes Rep. 2015;4:350–62.
Poulsen PH, Biering K, Winding TN, Nohr EA, Petersen LV, Ulijaszek SJ, et al. How does psychosocial stress affect the relationship between socioeconomic disadvantage and overweight and obesity? Examining Hemmingsson’s model with data from a Danish longitudinal study. BMC Public Health. 2019;19:1475.
Wechsler D. Wechsler preschool and primary scale of intelligence. 4th ed. San Antonio, TX: The Psychological Corporation; 2012.
Acknowledgements
We wish to thank the Neonatologists, Nurses, Dietitians, and other staff who cared for the infants in this study, and the parents who provided consent for their infants’ data to be used in research. We thank Megan Ramsay, Ninfa Garay, Michelle Matiation, Sara Leuenberger, Jasmine Shourounis, Tian Huang for their excellent data collection and Lynn Rotariu and Kim Fichter from Health Records.
Funding
This work was supported by the Diabetes, Obesity and Nutrition Strategic Clinical Network, Alberta Health Services, Canada, and the Canadian Foundation for Dietetic Research.
Author information
Authors and Affiliations
Contributions
TRF conceptualized and designed the study with assistance from all the other authors, performed the statistical analysis, drafted the initial manuscript, and reviewed and revised the manuscript. All the other authors made substantial contributions to the conception or design of the work or the acquisition, analysis, and/or interpretation of data. All authors revised it critically for important intellectual content and approved the final of the version to be published.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Fenton, T.R., Nasser, R., Creighton, D. et al. Critical examination of relationships between early growth and childhood overweight in extremely preterm infants. J Perinatol 41, 2774–2781 (2021). https://doi.org/10.1038/s41372-021-01182-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-021-01182-8
This article is cited by
-
Does the evidence support in utero influences on later health and disease? A systematic review of highly cited Barker studies on developmental origins
Journal of Perinatology (2024)
-
Complementary feeding in preterm infants: a position paper by Italian neonatal, paediatric and paediatric gastroenterology joint societies
Italian Journal of Pediatrics (2022)