Abstract
Objective
Our hypothesis was that among infants with hypoxic-ischemic encephalopathy (HIE), venoarterial (VA), compared to venovenous (VV), extracorporeal membrane oxygenation (ECMO) is associated with an increased risk of mortality or intracranial hemorrhage (ICH).
Design/methods
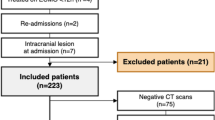
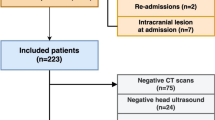
Retrospective cohort analysis of infants in the Children’s Hospitals Neonatal Database from 2010 to 2016 with moderate or severe HIE, gestational age ≥36 weeks, and ECMO initiation <7 days of age. The primary outcome was mortality or ICH.
Results
Severe HIE was more common in the VA ECMO group (n = 57), compared to the VV ECMO group (n = 53) (47.4% vs. 26.4%, P = 0.02). VA ECMO was associated with a significantly higher risk of death or ICH [57.9% vs. 34.0%, aOR 2.39 (1.08–5.28)] and mortality [31.6% vs. 11.3%, aOR 3.06 (1.08–8.68)], after adjusting for HIE severity.
Conclusions
In HIE, VA ECMO was associated with a higher incidence of mortality or ICH. VV ECMO may be beneficial in this population.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Shankaran S, Laptook AR, Pappas A, McDonald SA, Das A, Tyson JE, et al. Effect of depth and duration of cooling on death or disability at age 18 months among neonates with hypoxic-ischemic encephalopathy: a randomized clinical trial. JAMA. 2017;318:57–67.
Kurinczuk JJ, White-Koning M, Badawi N. Epidemiology of neonatal encephalopathy and hypoxic-ischaemic encephalopathy. Early Hum Dev. 2010;86:329–38.
Jacobs SE, Berg M, Hunt R, Tarnow-Mordi WO, Inder TE, Davis PG. Cooling for newborns with hypoxic ischaemic encephalopathy. Cochrane Database Syst Rev. 2013;1:CD003311.
Lakshminrusimha S, Saugstad OD. The fetal circulation, pathophysiology of hypoxemic respiratory failure and pulmonary hypertension in neonates, and the role of oxygen therapy. J Perinatol. 2016;36:S3–S11.
Lapointe A, Barrington KJ. Pulmonary hypertension and the asphyxiated newborn. J Pediatr. 2011;158:e19–24.
Benumof JL, Wahrenbrock EA. Dependency of hypoxic pulmonary vasoconstriction on temperature. J Appl Physiol Respir Environ Exerc Physiol. 1977;42:56–8.
Toubas PL, Hof RP, Heymann MA, Rudolph AM. Effects of hypothermia and rewarming on the neonatal circulation. Arch Fr Pediatr. 1978;35:84–92.
Bulas DI, Taylor GA, O’Donnell RM, Short BL, Fitz CR, Vezina G. Intracranial abnormalities in infants treated with extracorporeal membrane oxygenation: update on sonographic and CT findings. AJNR Am J Neuroradiol. 1996;17:287–94.
Shankaran S, Pappas A, Laptook AR, McDonald SA, Ehrenkranz RA, Tyson JE, et al. Outcomes of safety and effectiveness in a multicenter randomized, controlled trial of whole-body hypothermia for neonatal hypoxic-ischemic encephalopathy. Pediatrics. 2008;122:e791–8.
Shankaran S, Laptook AR, Pappas A, McDonald SA, Das A, Tyson JE, et al. Effect of depth and duration of cooling on deaths in the NICU among neonates with hypoxic ischemic encephalopathy: a randomized clinical trial. JAMA. 2014;312:2629–39.
Rutherford MA, Azzopardi D, Whitelaw A, Cowan F, Renowden S, Edwards AD. et al. Mild hypothermia and the distribution of cerebral lesions in neonates with hypoxic-ischemic encephalopathy. Pediatrics. 2005;116:1001–6.
Shankaran S, Barnes PD, Hintz SR, Laptook AR, Zaterka-Baxter KM, McDonald SA. et al. Brain injury following trial of hypothermia for neonatal hypoxic-ischaemic encephalopathy. Arch Dis Child Fetal Neonatal Ed. 2012;97:F398–404.
Cuevas Guaman M, Lucke AM, Hagan JL, Kaiser JR. Bleeding complications and mortality in neonates receiving therapeutic hypothermia and extracorporeal membrane oxygenation. Am J Perinatol. 2018;35:271–6.
Skinner SC, Iocono JA, Ballard HO, Turner MD, Ward AN, Davenport DL, et al. Improved survival in venovenous vs venoarterial extracorporeal membrane oxygenation for pediatric noncardiac sepsis patients: a study of the extracorporeal life support organization registry. J Pediatr Surg. 2012;47:63–7.
Cashen K, Reeder RW, Shanti C, Dalton HJ, Dean JM, Meert KL. et al. Is therapeutic hypothermia during neonatal extracorporeal membrane oxygenation associated with intracranial hemorrhage?. Perfusion. 2018;33:354–62.
Carpenter JL, Yu YR, Cass DL, Olutoye OO, Thomas JA, Burgman C, et al. Use of venovenous ECMO for neonatal and pediatric ECMO: a decade of experience at a tertiary children’s hospital. Pediatr Surg Int. 2018;34:263–8.
Murthy K, Dykes FD, Padula MA, Pallotto EK, Reber KM, Durand DJ, et al. The Children’s Hospitals neonatal database: an overview of patient complexity, outcomes and variation in care. J Perinatol. 2014;34:582–6.
Massaro AN, Murthy K, Zaniletti I, Cook N, DiGeronimo R, Dizon ML, et al. Intercenter cost variation for perinatal hypoxic-ischemic encephalopathy in the era of therapeutic hypothermia. J Pediatr. 2016;173:76–83. e1
Shankaran S, Laptook AR, Ehrenkranz RA, Tyson JE, McDonald SA, Donovan EF, et al. Whole-body hypothermia for neonates with hypoxic-ischemic encephalopathy. N Engl J Med. 2005;353:1574–84.
Pfister RH, Bingham P, Edwards EM, Horbar JD, Kenny MJ, Inder T, et al. The vermont oxford neonatal encephalopathy registry: rationale, methods, and initial results. BMC Pediatr. 2012;12:84.
Agarwal P, Altinok D, Desai J, Shanti C, Natarajan G. In-hospital outcomes of neonates with hypoxic-ischemic encephalopathy receiving extracorporeal membrane oxygenation. J Perinatol. 2019;39:661–5.
Polito A, Barrett CS, Wypij D, Rycus PT, Netto R, Cogo PE, et al. Neurologic complications in neonates supported with extracorporeal membrane oxygenation. An analysis of ELSO registry data. Intensive Care Med. 2013;39:1594–601.
Howard TS, Kalish BT, Rajagopal SK, Williams K, Zalieckas J, Thiagarajan RR, et al. Factors associated with mortality in children who successfully wean from extracorporeal membrane oxygenation. Pediatr Crit Care Med. 2018;19:875–83.
Melbourne L, Wien MA, Whitehead MT, Ridore M, Wang Y, Short BL, et al. Risk factors for brain injury in newborns treated with extracorporeal membrane oxygenation. Am J Perinatol. 2020. https://doi.org/10.1055/s-0040-1714208. [Epub ahead of print].
de Mol AC, Liem KD, van Heijst AF. Cerebral aspects of neonatal extracorporeal membrane oxygenation: a review. Neonatology. 2013;104:95–103.
Short BL, Bender K, Walker LK, Traystman RJ. The cerebrovascular response to prolonged hypoxia with carotid artery and jugular vein ligation in the newborn lamb. J Pediatr Surg. 1994;29:887–91.
Short BL, Walker LK, Traystman RJ. Impaired cerebral autoregulation in the newborn lamb during recovery from severe, prolonged hypoxia, combined with carotid artery and jugular vein ligation. Crit Care Med. 1994;22:1262–8.
Short BL. The effect of extracorporeal life support on the brain: a focus on ECMO. Semin Perinatol. 2005;29:45–50.
Guner YS, Harting MT, Fairbairn K, Delaplain PT, Zhang L, Chen Y, et al. Outcomes of infants with congenital diaphragmatic hernia treated with venovenous versus venoarterial extracorporeal membrane oxygenation: a propensity score approach. J Pediatr Surg. 2018;53:2092–9.
Puligandla PS, Grabowski J, Austin M, Hedrick H, Renaud E, Arnold M, et al. Management of congenital diaphragmatic hernia: a systematic review from the APSA outcomes and evidence based practice committee. J Pediatr Surg. 2015;50:1958–70.
Meek JH, Elwell CE, McCormick DC, Edwards AD, Townsend JP, Stewart AL, et al. Abnormal cerebral haemodynamics in perinatally asphyxiated neonates related to outcome. Arch Dis Child Fetal Neonatal Ed. 1999;81:F110–5.
Pryds O, Greisen G, Lou H, Friis-Hansen B. Vasoparalysis associated with brain damage in asphyxiated term infants. J Pediatr. 1990;117:119–25.
Sewell EK, Piazza AJ, Davis J, Heard ML, Figueroa J, Keene SD. Inotrope needs in neonates requiring extracorporeal membrane oxygenation for respiratory failure. J Pediatrics. 2019;214:128–33.
Origen: December 2019 statement from Richard Martin CoB, Origen Biomedical. https://www.origen.com/wp-content/uploads/Catheter.update.pdf.
Johnson SM, Itoga N, Garnett GM, Kilcommons M, Puapong DP, Woo RK. Increased risk of cardiovascular perforation during ECMO with a bicaval, wire-reinforced cannula. J Pediatr Surg. 2014;49:46–9. discussion 9-50
Speggiorin S, Robinson SG, Harvey C, Westrope C, Faulkner GM, Kirkland P, et al. Experience with the Avalon(R) bicaval double-lumen veno-venous cannula for neonatal respiratory ECMO. Perfusion. 2015;30:250–4.
Lillie J, Boot L, Speggiorin S, Nyman AG. Factors behind decline of venovenous extracorporeal membrane oxygenation to support neonatal respiratory failure. Pediatr Crit Care Med. 2020;21:e502–e4.
Extracorporeal Life Support Organisation: International Trend Report July Aahweo.
Roberts J, Keene S, Heard M, McCracken C, Gauthier TW. Successful primary use of VVDL+V ECMO with cephalic drain in neonatal respiratory failure. J Perinatol. 2016;36:126–31.
Griffin MP, Minifee PK, Landry SH, Allison PL, Swischuk LE, Zwischenberger JB. Neurodevelopmental outcome in neonates after extracorporeal membrane oxygenation: cranial magnetic resonance imaging and ultrasonography correlation. J Pediatr Surg. 1992;27:33–5.
Bulas D, Glass P. Neonatal ECMO: neuroimaging and neurodevelopmental outcome. Semin Perinatol. 2005;29:58–65.
Massaro AN, Murthy K, Zaniletti I, Cook N, DiGeronimo R, Dizon M, et al. Short-term outcomes after perinatal hypoxic ischemic encephalopathy: a report from the Children’s Hospitals Neonatal Consortium HIE focus group. J Perinatol. 2015;35:290–6.
Children’s Hospital Neonatal Consortium (CHNC) ECMO and HIE focus groups
Anthony Piazza14, Gregory Sysyn15, Carl Coghill16, Allison Black16, Ramasubbareddy Dhanireddy17, Anne Hansen18, Tanzeema Hossain18, Karna Murthy19, Gustave Falciglia19, Beth Haberman20, Amy Nathan20, Kristin Nelson20, Paul Kingma20, Stefanie Riddle20, Stephanie Merhar20, Heather Kaplan20, Kristina Reber21, Rashmin Savani22, Luc Brion22, Noorjahan Ali22, Theresa Grover23, Girija Natarajan24, Jonathan Nedrelow25, Annie Chi25, Yvette Johnson25, Gautham Suresh26, William Engle27, Lora Simpson27, Gregory Sokol27, Eugenia Pallotto28, Robert Lyle29, Becky Rogers29, Steven Chin30, Rachel Chapman30, Jamie Limjoco31, Lori Haack31, David Durand32, Jeanette Asselin32, Art D’Harlingue32, Priscilla Joe32, Jacquelyn Evans33, Michael Padula33, David Munson33, Suzanne Touch34, Toby Yanowitz35, Beverly Brozanski36, Rakesh Rao36, Victor McKay37, Mark Speziale38, Brian Lane38, Laural Moyer38, Billie Short39, Lamia Soghier39, Kevin Sullivan40, Con Yee Ling41, Shrena Patel41, Michael Uhing42, Ankur Datta42, Nicole Birge43, Rajan Wadhawan44, Elizabeth Jacobsen-Misbe45, Robert DiGeronimo45, Zeenia Billimoria45, Kyong-Soon Lee46, Michel Mikhael47, Irfan Ahmad47.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Members of the Children’s Hospital Neonatal Consortium (CHNC) ECMO and HIE focus groups are listed above Conflict of interest.
Rights and permissions
About this article
Cite this article
Agarwal, P., Natarajan, G., Sullivan, K. et al. Venovenous versus venoarterial extracorporeal membrane oxygenation among infants with hypoxic-ischemic encephalopathy: is there a difference in outcome?. J Perinatol 41, 1916–1923 (2021). https://doi.org/10.1038/s41372-021-01089-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-021-01089-4