Abstract
Objective
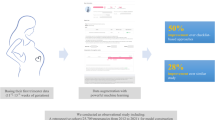
We sought to develop a prediction model using prenatal diagnosis codes that could help clinicians objectively stratify a women’s risk for delivery-related morbidity.
Study design
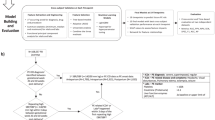
We performed a prospective cohort study of women delivering at a single academic medical center between 2016 and 2019. Diagnosis codes from outpatient encounters were extracted from the electronic health record. Standard and common machine-learning methods for variable selection were compared. The performance characteristics from the selected model in the training data set—a LASSO model with a lambda that minimized the Bayes information criteria—were compared in a testing and external validation set.
Results
The model identified a group of women, those in the highest decile of predicted risk, who were at a two to threefold increased risk of maternal morbidity.
Conclusion
As EHR data becomes more ubiquitous, other data types generated from the prenatal period may improve the model’s performance.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Creanga AA, Berg CJ, Syverson C, Seed K, Bruce FC, Callaghan WM. Pregnancy-related mortality in the United States, 2006–10. Obstet Gynecol. 2015;125:5–12.
Creanga AA, Syverson C, Seed K, Callaghan WM. Pregnancy-related mortality in the United States, 2011–3. Obstet Gynecol. 2017;130:366–73.
Creanga AA, Berg CJ, Ko JY, Farr SL, Tong VT, Bruce FC, et al. Maternal mortality and morbidity in the United States: where are we now? J Women’s Health. 2014;23:3–9.
Severe Maternal Morbidity in the United States Pregnancy Reproductive Health CDC. https://www.cdc.gov/reproductivehealth/maternalinfanthealth/severematernalmorbidity.html Accessed 4 Dec 2017.
Bateman BT, Bansil P, Hernandez-Diaz S, Mhyre JM, Callaghan WM, Kuklina EV. Prevalence, trends, and outcomes of chronic hypertension: a nationwide sample of delivery admissions. Am J Obstet Gynecol. 2012;206:134.e1–8.
DeSisto CL, Kim SY, Sharma AJ. Prevalence estimates of gestational diabetes mellitus in the United States, pregnancy risk assessment monitoring system (PRAMS), 2007–10. Prev Chronic Dis. 2014;11:E104.
Mogos MF, Salemi JL, Ashley M, Whiteman VE, Salihu HM. Recent trends in placenta accreta in the United States and its impact on maternal-fetal morbidity and healthcare-associated costs, 1998–2011. J Matern Fetal Neonatal Med. 2016;29:1077–82.
Bardenheier BH, Imperatore G, Gilboa SM, Geiss LS, Saydah SH, Devlin HM, et al. Trends in gestational diabetes among hospital deliveries in 19 U.S. States, 2000–10. Am J Prev Med. 2015;49:12–19.
Bauer ME, Bateman BT, Bauer ST, Shanks AM, Mhyre JM. Maternal sepsis mortality and morbidity during hospitalization for delivery: temporal trends and independent associations for severe sepsis. Anesth Analg. 2013;117:944–50.
American College of Obstetricians and Gynecologists and Society for Maternal–Fetal Medicine, Menard MK, Kilpatrick S, Saade G, Hollier LM, Joseph GF et al. Levels of maternal care. Am J Obstet Gynecol. 2015;212:259–71.
Easter SR, Robinson JN, Menard MK, Creanga AA, Xu X, Little SE, et al. Potential effects of regionalized maternity care on U.S. hospitals. Obstet Gynecol. 2019;134:545–52.
Bukowski R, Schulz K, Gaither K, Stephens KK, Semeraro D, Drake J, et al. Computational medicine, present and the future: obstetrics and gynecology perspective. Am J Obstet Gynecol. 2021;224:16–34.
Venkatesh KK, Strauss RA, Grotegut CA, Heine RP, Chescheir NC, Stringer JSA, et al. Machine learning and statistical models to predict postpartum hemorrhage. Obstet Gynecol. 2020;135:935–44.
Stamilio DM, Beckham AJ, Boggess KA, Jelovsek JE, Venkatesh KK. Risk factors for postpartum readmission for preeclampsia or hypertension before delivery discharge among low-risk women: a case-control study. Am J Obstet Gynecol MFM. 2021;3:100317.
Maric T, Singh N, Duncan K, Thorpe-Beeston GJ, Savvidou MD. First-trimester fetal growth discordance and development of preeclampsia in dichorionic twin pregnancies. J Perinat Med. 2015;43:755–9.
Bateman BT, Mhyre JM, Hernandez-Diaz S, Huybrechts KF, Fischer MA, Creanga AA, et al. Development of a comorbidity index for use in obstetric patients. Obstet Gynecol. 2013;122:957–65.
Easter SR, Bateman BT, Sweeney VH, Manganaro K, Lassey SC, Gagne JJ, et al. A comorbidity-based screening tool to predict severe maternal morbidity at the time of delivery. Am J Obstetr Gynecol. 2019. https://doi.org/10.1016/j.ajog.2019.06.025.
Hoffman MK, Ma N, Roberts A. A machine learning algorithm for predicting maternal readmission for hypertensive disorders of pregnancy. Am J Obstet Gynecol MFM. 2021;3:100250.
Rosenbloom JI, Tuuli MG, Stout MJ, Young OM, Woolfolk CL, López JD et al. A Prediction Model for Severe Maternal Morbidity in Laboring Patients at Term. Am J Perinatol. 2018. https://doi.org/10.1055/s-0038-1626716.
ICD—ICD-10-CM—International Classification of Diseases, ICD-10-CM/PCS Transition. 2019.https://www.cdc.gov/nchs/icd/icd10cm_pcs_background.htm Accessed 20 Jul 2020.
How Does CDC Identify Severe Maternal Morbidity? CDC. 2019.https://www.cdc.gov/reproductivehealth/maternalinfanthealth/smm/severe-morbidity-ICD.htm Accessed 21 Apr 2020.
HCUP-US NIS Overview. https://www.hcup-us.ahrq.gov/nisoverview.jsp Accessed 18 Jan 2017.
Steyerberg EW. Clinical prediction models. Second Edition. Switzerland: Springer Nature. 2019.
Vickers AJ, Elkin EB. Decision curve analysis: a novel method for evaluating prediction models. Med Decis Mak. 2006;26:565–74.
Collins GS, Reitsma JB, Altman DG, Moons KGM. Transparent reporting of a multivariable prediction model for individual prognosis or diagnosis (TRIPOD): the TRIPOD statement. BMJ. 2015;350:g7594.
Metcalfe A, Lix LM, Johnson J-A, Currie G, Lyon AW, Bernier F, et al. Validation of an obstetric comorbidity index in an external population. BJOG. 2015;122:1748–55.
Funding
Dr. Clapp’s work on this project was funded by a grant from the American Association of Obstetricians and Gynecologists Foundation and the American Board of Obstetricians and Gynecologists.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Perlis has received fees for consulting or service on scientific advisory boards for Genomind, Psy Therapeutics, Outermost Therapeutics, RID Ventures, and Takeda. He has received patent royalties from Massachusetts General Hospital. He holds equity in Psy Therapeutics and Outermost Therapeutics.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Clapp, M.A., McCoy Jr, T.H., James, K.E. et al. Derivation and external validation of risk stratification models for severe maternal morbidity using prenatal encounter diagnosis codes. J Perinatol 41, 2590–2596 (2021). https://doi.org/10.1038/s41372-021-01072-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-021-01072-z