Abstract
Objective
To assess the feasibility of real-time monitoring of work of breathing (WOB) indices and the impact of adjusting HFNC flow on breathing synchrony and oxygen stability in premature infants.
Study design
A prospective, observational study of infants stable on HFNC. The flow adjusted per predetermined algorithm. Respiratory inductive plethysmography (RIP) noninvasively measured WOB. A high-resolution pulse oximeter collected oxygen saturation and heart rate data. Summary statistics and mixed linear models were used.
Results
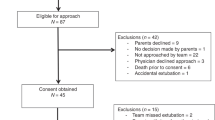
Baseline data for 32 infants, final analysis of 21 infants. Eighty-one percent with abnormal WOB. Sixty-two percent demonstrated 20% improvement in WOB. For infants with gestational age <28 weeks, an incremental increase in HFNC flow rate decreased WOB (p < 0.001) and improved oxygen saturation and stability (p < 0.01).
Conclusions
Premature infants do not receive optimal support on HFNC. The use of a real-time feedback system to adjust HFNC is feasible and improves WOB, oxygen saturation, and oxygen stability. This technology may improve the utility of HFNC in premature infants.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Fanaroff AA, Stoll BJ, Wright LL, Carlo WA, Ehrenkranz RA, Stark AR, et al. Trends in neonatal morbidity and mortality for very low birthweight infants. Am J Obstet Gynecol. 2007;196(2):147.e1–8.
Morley CJ, Davis PG, Doyle LW, Brion LP, Hascoet JM, Carlin JB. Nasal CPAP or intubation at birth for very preterm infants. N Engl J Med. 2008;358(7):700–8.
Finer NN, Carlo WA, Walsh MC, Rich W, Gantz MG, Laptook AR, et al. Early CPAP versus surfactant in extremely preterm infants. N Engl J Med. 2010;362(21):1970–9.
Dunn MS, Kaempf J, de Klerk A, de Klerk R, Reilly M, Howard D, et al. Randomized trial comparing 3 approaches to the initial respiratory management of preterm neonates. Pediatrics. 2011;128(5):e1069–76.
Schmölzer GM, Kumar M, Pichler G, Aziz K, O’Reilly M, Cheung PY. Non-invasive versus invasive respiratory support in preterm infants at birth: systematic review and meta-analysis. BMJ. 2013;347:f5980.
Hussain WA, Marks JD. Approaches to noninvasive respiratory support in preterm infants: from CPAP to NAVA. Neoreviews. 2019;20(4):e213–e21.
Manley BJ, Owen LS, Davis PG. High-flow nasal cannulae in very preterm infants after extubation. N Engl J Med. 2014;370(4):385–6.
Wilkinson D, Andersen C, O’Donnell CP, De Paoli AG, Manley BJ. High flow nasal cannula for respiratory support in preterm infants. Cochrane Database Syst Rev. 2016;2:Cd006405.
Roberts CT, Owen LS, Manley BJ, Frøisland DH, Donath SM, Dalziel KM, et al. Nasal high-flow therapy for primary respiratory support in preterm infants. N Engl J Med. 2016;375(12):1142–51.
Allen JL, Greenspan JS, Deoras KS, Keklikian E, Wolfson MR, Shaffer TH. Interaction between chest wall motion and lung mechanics in normal infants and infants with bronchopulmonary dysplasia. Pediatr Pulmonol. 1991;11(1):37–43.
de Jongh BE, Locke R, Mackley A, Emberger J, Bostick D, Stefano J, et al. Work of breathing indices in infants with respiratory insufficiency receiving high-flow nasal cannula and nasal continuous positive airway pressure. J Perinatol. 2014;34(1):27–32.
Perez A, Mulot R, Vardon G, Barois A, Gallego J. Thoracoabdominal pattern of breathing in neuromuscular disorders. Chest. 1996;110(2):454–61.
Ryan L, Rahman T, Strang A, Heinle R, Shaffer TH. Diagnostic differences in respiratory breathing patterns and work of breathing indices in children with duchenne muscular dystrophy. PLoS ONE. 2020;15(1):e0226980.
Wolfson MR, Greenspan JS, Deoras KS, Allen JL, Shaffer TH. Effect of position on the mechanical interaction between the rib cage and abdomen in preterm infants. J Appl Physiol. 1992;72(3):1032–8.
Ratnagiri MV, Ryan L, Strang A, Heinle R, Rahman T, Shaffer TH. Machine learning for automatic identification of thoracoabdominal asynchrony in children. Pediatr Res. 2020. https://doi.org/10.1038/s41390-020-1032-1. Jul 3[Online ahead of print]. PMID: 32620007
Rahman T, Page R, Page C, Bonnefoy JR, Cox T, Shaffer TH. pneuRIP(TM): a novel respiratory inductance plethysmography monitor. J Med Device. 2017;11(1):0110101–110106.
Strang A, Ryan L, Rahman T, Balasubramanian S, Hossain J, Heinle R, et al. Measures of respiratory inductance plethysmography (RIP) in children with neuromuscular disease. Pediatr Pulmonol. 2018;53(9):1260–8.
Balasubramaniam SL, Wang Y, Ryan L, Hossain J, Rahman T, Shaffer TH. Age-related ranges of respiratory inductance plethysmography (RIP) reference values for infants and children. Paediatr Respir Rev. 2019;29:60–7.
Ambalavanan N, Van Meurs KP, Perritt R, Carlo WA, Ehrenkranz RA, Stevenson DK, et al. Predictors of death or bronchopulmonary dysplasia in preterm infants with respiratory failure. J Perinatol. 2008;28(6):420–6.
Kanbar J, Shalish W, Laremouille S, Rao S, Brown K, Kearney R, et al. Cardiorespiratory behavior of preterm infants receiving continuous postiive airway pressure and high flow nasal cannula post extubation: randomzied crossover study. Pediatr Res. 2020;87(1):62–8.
Brooks L, DiFiore JM, Martin R. Assessment of tidal volume preterm infants using respiratory inductance plethysmography. Pediatr Pulmonol. 1997;23(6):429–33.
Stick S, Ellis E, Leouef P, Sly P. Validation of respiratory inductance plethysmography for the measurement of tidal breathing parameters in newborns. Pediatr Pulmonol. 1992;14(3):187–91.
Springer C, Godfrey S, Vilozni D, Bar-Yishay E, Noviski N, Avital A. Comparison of respiratory inductance thoracoabdominal compression in bronchial challenges in infants and young children. Am J Respir Crit Care Med. 1996;154(3):665–9.
Martin R, DiFiore JM, Korenke CB, Randal H, Miller MJ, Brooks LJ. Vulternability of respiratory control in healthy preterm infants placed supine. J Pediatr. 1995;127(4):609–14.
Robles-Rubio CA, Kearney R, Bertolizio G, Brown K. Automatic unnsupervised respiratory analysis of infant respiratory inductance plethymography signals. PLoS ONE. 2020;15(9):e0238402.
Kotecha SJ, Adappa R, Gupta N, Watkins WJ, Kotecha S, Chakraborty M. Safety and efficacy of high-flow nasal cannula therapy in preterm infants: a meta-analysis. Pediatrics. 2015;136(3):542–53.
Frizzola M, Miller TL, Rodriguez ME, Zhu Y, Rojas J, Hesek A, et al. High-flow nasal cannula: impact on oxygenation and ventilation in an acute lung injury model. Pediatr Pulmonol. 2011;46(1):67–74.
Saslow JG, Aghai ZH, Nakhla TA, Hart JJ, Lawrysh R, Stahl GE, et al. Work of breathing using high-flow nasal cannula in preterm infants. J Perinatol. 2006;26(8):476–80.
Chidekel A, Zhu Y, Wang J, Mosko JJ, Rodriguez E, Shaffer TH. The effects of gas humidification with high-flow nasal cannula on cultured human airway epithelial cells. Pulm Med. 2012;2012:380686.
Greenspan JS, Wolfson MR, Shaffer TH. Airway responsiveness to low inspired gas temperature in preterm neonates. J Pediatr. 1991;118(3):443–5.
Woodhead DD, Lambert DK, Clark JM, Christensen RD. Comparing two methods of delivering high-flow gas therapy by nasal cannula following endotracheal extubation: a prospective, randomized, masked, crossover trial. J Perinatol. 2006;26(8):481–5.
Dysart K, Miller TL, Wolfson MR, Shaffer TH. Research in high flow therapy: mechanisms of action. Respir Med. 2009;103(10):1400–5.
McQueen M, Rojas J, Sun SC, Tero R, Ives K, Bednarek F, et al. Safety and long-term outcomes with high flow nasal cannula therapy in neonatology: a large retrospective cohort study. J Pulm Respir Med. 2014;4(6):216.
Acknowledgements
THS receives funding from NIH COBRE grant P30GM114736. KS is supported by an Institutional Development Aware (IDeA) from the National Institute of General Medical Sciences of the NIH grant U54-GM104941 (PI Binder-Macleod).
Author information
Authors and Affiliations
Contributions
KZK provided a substantial contribution to the conception, design, acquisition of data, analysis, and interpretation of the data. She was primarily responsible for the drafting of the article and has approved the submitted manuscript. RGL provided a substantial contribution to the conception, design, analysis, and interpretation of the data. He contributed significantly to the revision of the manuscript and has approved the submitted manuscript. ABM provided a substantial contribution to the design and acquisition of data. She contributed significantly to the revision of the manuscript and has approved the submitted manuscript. KS contributed significantly to the analysis and interpretation of the data and the drafting of the manuscript. He has approved the submitted manuscript. THS served as a mentor to the first author and provided a substantial contribution to the conception, design, and interpretation of the data. He played a significant role in the revision of the manuscript and has approved the submitted manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kovatis, K.Z., Locke, R.G., Mackley, A.B. et al. Adjustment of high flow nasal cannula rates using real-time work of breathing indices in premature infants with respiratory insufficiency. J Perinatol 41, 1711–1717 (2021). https://doi.org/10.1038/s41372-021-00977-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-021-00977-z