Abstract
Objective
Investigate predictors of postoperative morbidity and mortality in surgical NEC.
Study design
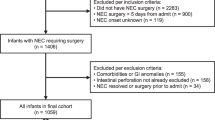
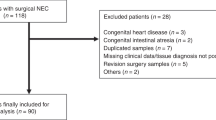
We analyzed the clinical outcomes of infants with surgical NEC from the years 2000–2015.
Results
Ninety infants born at gestation (mean ± standard deviation, SD; standard error of mean, SEM) 27.3 ± 6.6 weeks (SEM ± 0.07 weeks) and weighing 1008 ± 456 g (SEM ± 48 g) developed NEC on 25.2 ± 22.4 days (SEM ± 2.4 days). Average bowel resection was 29.2 ± 30.5 cm (SEM ± 3.2 cm). Postoperative Ileus lasted 16.5 ± 12.2 days (SEM ± 1.3 days), and was significantly longer in infants with higher gestation and birth weight, age at onset of NEC, length of intestinal resection, maternal chorioamnionitis, and need for pressors. Thirty-eight (42.2%) infants died. Mortality was higher at gestation <31 weeks.
Conclusion
Gestational age, birth weight, age at NEC onset, and length of resected bowel determined postoperative morbidity and mortality in NEC. Length of hospital stay was affected by above factors, and also the duration of postoperative ileus and parenteral nutrition.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Neu J, Modi N, Caplan M. Necrotizing enterocolitis comes in different forms: historical perspectives and defining the disease. Semin Fetal Neonatal Med. 2018;23:370–3.
Jones IH, Hall NJ. Contemporary outcomes for infants with necrotizing enterocolitis—a systematic review. J Pediatr. 2020;220:86–90.e3.
Han SM, Hong CR, Knell J, Edwards EM, Morrow KA, Soll RF, et al. Trends in incidence and outcomes of necrotizing enterocolitis over the last 12 years: a multicenter cohort analysis. J Pediatr Surg. 2020;55:998–1001.
Sjoberg Bexelius T, Ahle M, Elfvin A, Bjorling O, Ludvigsson JF, Andersson RE. Intestinal failure after necrotising enterocolitis: incidence and risk factors in a Swedish population-based longitudinal study. BMJ Paediatr Open. 2018;2:e000316.
Allin BSR, Long AM, Gupta A, Lakhoo K, Knight M. One-year outcomes following surgery for necrotising enterocolitis: a UK-wide cohort study. Arch Dis Child Fetal Neonatal Ed. 2018;103:F461–6.
Knell J, Han SM, Jaksic T, Modi BP. Current status of necrotizing enterocolitis. Curr Probl Surg. 2019;56:11–38.
Stoll BJ, Hansen NI, Bell EF, Walsh MC, Carlo WA, Shankaran S, et al. Trends in care practices, morbidity, and mortality of extremely preterm neonates, 1993–2012. JAMA 2015;314:1039–51.
Nair R, Kahlenberg CA, Patel RM, Knesek M, Terry MA. All-arthroscopic suprapectoral biceps tenodesis. Arthrosc Technol. 2015;4:e855–61.
Santulli TV, Schullinger JN, Heird WC, Gongaware RD, Wigger J, Barlow B, et al. Acute necrotizing enterocolitis in infancy: a review of 64 cases. Pediatrics. 1975;55:376–87.
Mowitz ME, Dukhovny D, Zupancic JAF. The cost of necrotizing enterocolitis in premature infants. Semin Fetal Neonatal Med. 2018;23:416–9.
Ganapathy V, Hay JW, Kim JH, Lee ML, Rechtman DJ. Long term healthcare costs of infants who survived neonatal necrotizing enterocolitis: a retrospective longitudinal study among infants enrolled in Texas Medicaid. BMC Pediatr. 2013;13:127.
Kurscheid T, Holschneider AM. Necrotizing enterocolitis (NEC)-mortality and long-term results. Eur J Pediatr Surg. 1993;3:139–43.
Thakkar HS, Lakhoo K. The surgical management of necrotising enterocolitis (NEC). Early Hum Dev. 2016;97:25–8.
Raval MV, Moss RL. Current concepts in the surgical approach to necrotizing enterocolitis. Pathophysiology. 2014;21:105–10.
Rees CM, Hall NJ, Eaton S, Pierro A. Surgical strategies for necrotising enterocolitis: a survey of practice in the United Kingdom. Arch Dis Child Fetal Neonatal Ed. 2005;90:F152–5.
Robinson JR, Rellinger EJ, Hatch LD, Weitkamp JH, Speck KE, Danko M, et al. Surgical necrotizing enterocolitis. Semin Perinatol. 2017;41:70–9.
Fenton TR, Kim JH. A systematic review and meta-analysis to revise the Fenton growth chart for preterm infants. BMC Pediatr. 2013;13:59.
Davies HT. Describing and estimating: use and abuse of standard deviations and standard errors. Hosp Med. 1998;59:327–8.
Manuck TA, Rice MM, Bailit JL, Grobman WA, Reddy UM, Wapner RJ, et al. Preterm neonatal morbidity and mortality by gestational age: a contemporary cohort. Am J Obstet Gynecol. 2016;215:103 e1–14.
Sheng Q, Lv Z, Xu W, Liu J, Wu Y, Shi J, et al. Short-term surgical outcomes of preterm infants with necrotizing enterocolitis: a single-center experience. Medicine. 2016;95:e4379.
Wright NJ, Thyoka M, Kiely EM, Pierro A, De Coppi P, Cross KM, et al. The outcome of critically ill neonates undergoing laparotomy for necrotising enterocolitis in the neonatal intensive care unit: a 10-year review. J Pediatr Surg. 2014;49:1210–4.
Li X, Li L, Wang Y, Deng C, Guo C. Postoperative characteristics of infants who developed necrotizing enterocolitis with different postnatal ages. Medicine. 2017;96:e7774.
Hau EM, Meyer SC, Berger S, Goutaki M, Kordasz M, Kessler U. Gastrointestinal sequelae after surgery for necrotising enterocolitis: a systematic review and meta-analysis. Arch Dis Child Fetal Neonatal Ed. 2019;104:F265–73.
Geng Q, Wang Y, Li L, Guo C. Early postoperative outcomes of surgery for intestinal perforation in NEC based on intestinal location of disease. Medicine. 2018;97:e12234.
Cole CR, Hansen NI, Higgins RD, Ziegler TR, Stoll BJ. Eunice Kennedy Shriver NNRN. Very low birth weight preterm infants with surgical short bowel syndrome: incidence, morbidity and mortality, and growth outcomes at 18 to 22 months. Pediatrics. 2008;122:e573–82.
Blakely ML, Lally KP, McDonald S, Brown RL, Barnhart DC, Ricketts RR, et al. Postoperative outcomes of extremely low birth-weight infants with necrotizing enterocolitis or isolated intestinal perforation: a prospective cohort study by the NICHD Neonatal Research Network. Ann Surg. 2005;241:984–9; discussion 9–94.
Bhatt D, Travers C, Patel RM, Shinnick J, Arps K, Keene S, et al. Predicting mortality or intestinal failure in infants with surgical necrotizing enterocolitis. J Pediatr. 2017;191:22–7 e3.
Jammeh ML, Adibe OO, Tracy ET, Rice HE, Clark RH, Smith PB, et al. Racial/ethnic differences in necrotizing enterocolitis incidence and outcomes in premature very low birth weight infants. J Perinatol. 2018;38:1386–90.
Horbar JD, Badger GJ, Carpenter JH, Fanaroff AA, Kilpatrick S, LaCorte M, et al. Trends in mortality and morbidity for very low birth weight infants, 1991-1999. Pediatrics. 2002;110(1 Pt 1):143–51.
Janevic T, Zeitlin J, Auger N, Egorova NN, Hebert P, Balbierz A, et al. Association of race/ethnicity with very preterm neonatal morbidities. JAMA Pediatr. 2018;172:1061–9.
Cuna A, George L, Sampath V. Genetic predisposition to necrotizing enterocolitis in premature infants: current knowledge, challenges, and future directions. Semin Fetal Neonatal Med. 2018;23:387–93.
Cuna A, Yu W, Menden HL, Feng L, Srinivasan P, Chavez-Bueno S, et al. NEC-like intestinal injury is ameliorated by Lactobacillus rhamnosus GG in parallel with SIGIRR and A20 induction in neonatal mice. Pediatr Res. 2020. https://doi.org/10.1038/s41390-020-0797-6. [Epub ahead of print]
Sampath V, Helbling D, Menden H, Dimmock D, Mulrooney NP, Murray JC, et al. Necrotizing enterocolitis is not associated with sequence variants in antioxidant response genes in premature infants. J Pediatr Gastroenterol Nutr. 2016;62:420–3.
Sampath V, Le M, Lane L, Patel AL, Cohen JD, Simpson PM, et al. The NFKB1 (g.-24519delATTG) variant is associated with necrotizing enterocolitis (NEC) in premature infants. J Surg Res. 2011;169:e51–7.
Sampath V, Menden H, Helbling D, Li K, Gastonguay A, Ramchandran R, et al. SIGIRR genetic variants in premature infants with necrotizing enterocolitis. Pediatrics. 2015;135:e1530–4.
Necrotizing enterocolitis in the premature infant. Br Med J. 1966;2:1089–90.
Remon JI, Amin SC, Mehendale SR, Rao R, Luciano AA, Garzon SA, et al. Depth of bacterial invasion in resected intestinal tissue predicts mortality in surgical necrotizing enterocolitis. J Perinatol. 2015;35:755–62.
Bell MJ, Feigin RD, Ternberg JL, Brotherton T. Evaluation of gastrointestinal microflora in necrotizing enterocolitis. J Pediatr. 1978;92:589–92.
Gewolb IH, Schwalbe RS, Taciak VL, Harrison TS, Panigrahi P. Stool microflora in extremely low birthweight infants. Arch Dis Child Fetal Neonatal Ed. 1999;80:F167–73.
Smith B, Bode S, Skov TH, Mirsepasi H, Greisen G, Krogfelt KA. Investigation of the early intestinal microflora in premature infants with/without necrotizing enterocolitis using two different methods. Pediatr Res. 2012;71:115–20.
Andrews WW, Goldenberg RL, Faye-Petersen O, Cliver S, Goepfert AR, Hauth JC. The Alabama Preterm Birth study: polymorphonuclear and mononuclear cell placental infiltrations, other markers of inflammation, and outcomes in 23- to 32-week preterm newborn infants. Am J Obstet Gynecol. 2006;195:803–8.
Dorling J, Kempley S, Leaf A. Feeding growth restricted preterm infants with abnormal antenatal Doppler results. Arch Dis Child Fetal Neonatal Ed. 2005;90:F359–63.
Venkatesh KK, Jackson W, Hughes BL, Laughon MM, Thorp JM, Stamilio DM. Association of chorioamnionitis and its duration with neonatal morbidity and mortality. J Perinatol. 2019.
Peterslund P, Rasmussen L, Qvist N, Hansen TP, Husby S, Detlefsen S. Frequencies of immune cells in the human small bowel during normal gestation and in necrotizing enterocolitis. Fetal Pediatr Pathol. 2019:1–14.
Funding
National Institutes of Health awards HL124078 and HL133022 to AM Category of study: Clinical science.
Author information
Authors and Affiliations
Contributions
PMG and AM designed the study and wrote the manuscript, MH and CB collected data and did data analysis. All the authors contributed to and approved the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Garg, P.M., Hitt, M.M., Blackshear, C. et al. Clinical determinants of postoperative outcomes in surgical necrotizing enterocolitis. J Perinatol 40, 1671–1678 (2020). https://doi.org/10.1038/s41372-020-0728-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-020-0728-8
This article is cited by
-
Outcomes by disease onset, sex, and intervention in neonates with SIP and surgical NEC
Pediatric Research (2023)
-
Postoperative Outcomes, and Growth and Brain Injury Outcomes in Spontaneous Intestinal Perforation vs Surgical Necrotizing Enterocolitis in Preterm Infants
Indian Pediatrics (2023)
-
Brain injury in preterm infants with surgical necrotizing enterocolitis: clinical and bowel pathological correlates
Pediatric Research (2022)
-
Serum HMGB1 level is correlated with serum I-FABP level in neonatal patients with necrotizing enterocolitis
BMC Pediatrics (2021)
-
Early Career Investigator: Biocommentary
Pediatric Research (2021)