Abstract
Objective
To assess the rate, location, risk factors, management, and outcomes of neonatal thrombosis (NT).
Design
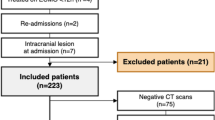
A retrospective study investigating infants admitted to NICUs in Canadian Neonatal Network between January 2014 and December 2016 and diagnosed with NT. Each infant with NT was matched with an infant without NT.
Results
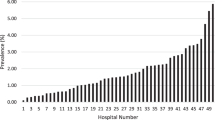
Of 39,971 infants, 587 (1.5%) were diagnosed with NT: 440 (75%) venous, 112 (19%) arterial, 29 (5%) both. NT rate was 1.4% in full-term and 1.7% in preterm infants. Venous thrombi occurred most commonly in the portal vein and arterial thrombi in the cerebral artery. Conservative management and low molecular weight heparin were the most common treatment modalities. Hospital stay was longer (p < 0.001) in the NT patients, but mortality was similar.
Conclusions
NT was diagnosed in ~15/1000 NICU admissions and most commonly in the portal vein and cerebral arteries. Management varied based on the type and location of thrombi. Large multicenter trials are needed to address the best management strategies.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Greenway A, Massicotte MP, Monagle P. Neonatal thrombosis and its treatment. Blood Rev. 2004;18:75–84.
Schmidt B, Andrew M. Neonatal thrombosis: report of a prospective Canadian and international registry. Pediatrics. 1995;96(5 Pt 1):939–43.
Seibert JJ, Taylor BJ, Williamson SL, Williams BJ, Szabo JS, Corbitt SL. Sonographic detection of neonatal umbilical-artery thrombosis: clinical correlation. Am J Roentgenol. 1987;148:965–8.
Andrew M. Developmental hemostasis: relevance to newborns and infants. In: Nathan DG, Orkin SH, Oski FA (eds). Nathan and Oski’s hematology of infancy and childhood. 5th ed. Philadelphia: WB Saunders; 1998. p. 114–58.
Albisetti M, Andrew M, Monagle P. Hemostatic abnormalities. In: De Alarcón P, Werner E, editors. Neonatal hematology. New York: Cambridge University Press; 2005. p. 310–48.
Monagle P, Chan A, Massicotte P, Chalmers E, Michelson AD. Antithrombotic therapy in children: the seventh ACCP conference on antithrombotic and thrombolytic therapy. Chest. 2004;126(3 Supp l):645S–87S.
Cabannes M, Bouissou A, Favrais G, Sembély-Taveau C, Morales L, Favreau A, et al. Systematic ultrasound examinations in neonates admitted to NICU: evolution of portal vein thrombosis. J Perinatol. 2018;38:1359–64.
Bryant BG. Drug, fluid, and blood products administered through the umbilical artery catheter: complication experiences from one NICU. Neonatal Netw. 1990;9:27–32.
Glickstein JS, Rutkowski M, Schacht R, Friedman D. Renal blood flow velocity in neonates with and without umbilical artery catheters. J Clin Ultrasound. 1994;22:543–50.
Bacciedoni V, Attie M, Donato H. Thrombosis in newborn infants. Arch Argent Pediatr. 2016;114:159–66.
Saxonhouse MA, Manco-Johnson MJ. The evaluation and management of neonatal coagulation disorders. Semin Perinatol. 2009;33:56.
Monagle P, Chan AK, Goldenberg NA, Ichord RN, Journeycake JM, Nowak-Göttl U, et al. Antithrombotic therapy in neonates and children: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed. American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest 2012;141(2 Supp l):e737S–801S.
Canadian Neonatal Network. Canadian Neonatal Network abstractor’s manual. v 2.1.2, 1–94. 2014. www.canadianneonatalnetwork.org. Accessed 7 Aug 2017.
Shah PS, Seidlitz W, Chan P, Yeh S, Musrap N, Lee SK.data abstractors of the Canadian Neonatal Network Internal audit of the Canadian Neonatal Network Data Collection System. Am J Perinatol. 2017;34:1241–9.
Nowak-Gottl U, von Kries R, Gobel U. Neonatal symptomatic thromboembolism in Germany: two year survey. Arch Dis Child Fetal Neonatal Ed. 1997;76:F163–7.
van Elteren HA, Veldt HS, Te Pas AB, Roest AA, Smiers FJ, Kollen WJ, et al. Management and outcome in 32 neonates with thrombotic events. Int J Pediatr. 2011;2011:217564.
Bhat R, Kumar R, Kwon S, Murthy K, Liem R. Risk factors for neonatal venous and arterial thromboembolism in the Neonatal Intensive Care Unit—a case control study. J Pediatr. 2018;195:28–32.
Patel R. Short and long-term outcomes for extremely preterm infants. Am J Perinatol. 2016;33:318–28.
Demirel N, Aydin M, Zenciroglu A, Bas AY, Yarali N, Okumus N, et al. Neonatal thrombo-embolism: risk factors, clinical features and outcome. Ann Trop Paediatr. 2009;29:271–9.
Rehan V, Seshia MM. Complications of umbilical vein catheter. Eur J Pediatr. 1994;153:141.
Schwartz DS, Gettner PA, Konstantino MM, Bartley CL, Keller MS, Ehrenkranz RA, et al. Umbilical venous catheterization and the risk of portal vein thrombosis. J Pediatr. 1997;131:760e2.
Kim JH, Lee YS, Kim SH, Lee SK, Lim MK, Kim HS. Does umbilical vein catheterization lead to portal venous thrombosis? Prospective US evaluation in 100 neonates. Radiology. 2001;219:645–50.
Andrew M, Monagle P, Brooker L. Thromboembolic complications in specific organ sites and pediatric diseases. In: Thromboembolic complications during infancy and childhood. Hamilton, BC: Decker Inc; 2000. p. 231–76.
Lee J, Croen LA, Lindan C, Nash KB, Yoshida CK, Ferriero DM, et al. Predictors of outcome in perinatal arterial stroke: a population-based study. Ann Neurol. 2005;58:303–8.
Grunt S, Mazenauer L, Buerki SE, Boltshauser E, Mori AC, Datta AN, et al. Incidence and outcomes of symptomatic neonatal arterial ischemic stroke. Pediatrics. 2015;135:e1220–8.
Raju TN, Nelson KB, Ferriero D, Lynch JK. NICHD-NINDS Perinatal Stroke Workshop Participants Ischemic perinatal stroke: summary of a workshop sponsored by the National Institute of Child Health and Human Development and the National Institute of Neurological Disorders and Stroke. Pediatrics. 2007;120:609–16.
Lau KK, Stoffman JM, Williams S, McCusker P, Brandao L, Patel S, et al. Neonatal renal vein thrombosis: review of the English-language literature between 1992 and 2006. Pediatrics. 2007;120:e1278–84.
Thornburg CD, Smith PB, Smithwick ML, Cotten CM, Benjamin DK Jr. Association between thrombosis and bloodstream infection in neonates with peripherally inserted catheters. Thromb Res. 2008;122:782–5.
Timsit JF, Farkas JC, Boyer JM, Martin JB, Misset B, Renaud B, et al. Central vein catheter-related thrombosis in intensive care patients: incidence, risks factors, and relationship with catheter-related sepsis. Chest. 1998;114:207–13.
Schroeder AR, Axelrod DM, Silverman NH, Rubesova E, Merkel E, Roth SJ. A continuous heparin infusion does not prevent catheterrelated thrombosis in infants after cardiac surgery. Pediatr Crit Care Med. 2010;11:489–95.
Lee J, Croen LA, Backstrand KH, Yoshida CK, Henning LH, Lindan C, et al. Maternal and infant characteristics associated with perinatal arterial stroke in the infant. JAMA. 2005;293:723–9.
Acknowledgements
The authors gratefully acknowledge all site investigators and abstractors of the Canadian Neonatal Network (CNN). We also thank the staff at the Maternal-Infant Care (MiCare) Research Centre at Mount Sinai Hospital, Toronto, ON for organizational support of CNN. In addition, we thank Sarah Hutchinson, PhD, and Heather McDonald Kinkaid, PhD, from MiCare for editorial assistance in the preparation of this manuscript. MiCare is supported by a team grant from the Canadian Institutes of Health Research (CTP 87518), the Ontario Ministry of Health, and support from participating hospitals.
Funding
Although no specific funding has been received for this study, organizational support for the Canadian Neonatal Network was provided by the Maternal-Infant Care Research Centre (MiCare) at Mount Sinai Hospital in Toronto, Ontario, Canada. MiCare is supported by a Canadian Institutes of Health Research (CIHR) Team Grant (CTP 87518), the Ontario Ministry of Health and individual participating centers. PSS holds an Applied Research Chair in Reproductive and Child Health Services and Policy Research awarded by the CIHR (APR-126340). The funding agencies had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; and decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Consortia
Contributions
WE-N and PSS conceptualized and designed the study, analyzed and interpreted the data, drafted the initial manuscript, and reviewed and revised the manuscript. EWY collected data, carried out the initial analyses, and reviewed and revised the manuscript. DM, JA, SM, BS, OdS, and SKL contributed to the analysis and interpretation of the data and critically reviewed the manuscript for intellectual content. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
El-Naggar, W., Yoon, E.W., McMillan, D. et al. Epidemiology of thrombosis in Canadian neonatal intensive care units. J Perinatol 40, 1083–1090 (2020). https://doi.org/10.1038/s41372-020-0678-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-020-0678-1
This article is cited by
-
Risk factors for venous thromboembolism in a single pediatric intensive care unit in China
Thrombosis Journal (2024)
-
Epidemiology and risk factors for thrombosis in children and newborns: systematic evaluation and meta-analysis
BMC Pediatrics (2023)
-
Predictors of venous thromboembolism among infants in children’s hospitals in the United States: a retrospective Pediatric Health Information Study
Journal of Perinatology (2022)