Abstract
Objective
To measure the macronutrient content (MNC) of donor human milk labelled as 24 kcal/oz (“high-calorie DHM,” hcDHM), compare to bank-labelled MNC, and examine variability of hcDHM MNC among milk banks.
Study design
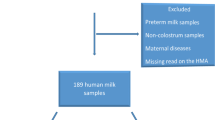
MNC was measured with near-infrared spectroscopy for 75 convenience samples from five milk banks collected during September 2016–July 2017. Concordance of measured MNC with labelled values was evaluated using three different thresholds: within ±20%, similar to FDA labelling standards for class II nutrients in foods; ±10%; and ±5%.
Results
Protein and caloric content differed significantly between measured and labelled values and varied significantly among milk banks. Measured caloric content ranged from 16.50 to 30.27 kcal/oz, with 89.3% of hcDHM samples within ±20%, 58.7% within ±10%, and 18.7% within ±5% of labelled content.
Conclusions
MNC of hcDHM used in clinical practice shows variation that may result in differences from desired diet. The clinical implications of such differences are unexplored.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Cregan MD, De Mello TR, Kershaw D, McDougall K, Hartmann PE. Initiation of lactation in women after preterm delivery. Acta Obstet Gynecol Scand. 2002;81:870–7.
Meier PP. Supporting lactation in mothers with very low birth weight infants. Pediatr Ann. 2003;32:317–25.
Jones E, Spencer SA. Optimising the provision of human milk for preterm infants. Arch Dis Child - Fetal Neonatal Ed. 2007;92:F236–8.
American Academy of Pediatrics. Breastfeeding and the use of human milk. Pediatrics. 2012;129:e827–41.
World Health Organization. Guidelines on optimal feeding of low birth-weight infants in low- and middle-income countries. World Health Organization. 2011. https://www.who.int/maternal_child_adolescent/documents/9789241548366.pdf. Accessed 18 Jul 2017.
Quigley M, Embleton ND, McGuire W. Formula versus donor breast milk for feeding preterm or low birth weight infants. Cochrane Database Syst Rev. 2018;7:CD002971.
John A, Sun R, Maillart L, Schaefer A, Spence EH, Perrin MT. Macronutrient variability in human milk from donors to a milk bank: implications for feeding preterm infants. PLoS ONE. 2019;14:e0210610.
Wu X, Jackson RT, Khan SA, Ahuja J, Pehrsson PR. Human milk nutrient composition in the United States: current knowledge, challenges, and research needs. Curr Dev Nutr. 2018;2:nzy025. https://doi.org/10.1093/cdn/nzy025.
Peila C, Moro G, Bertino E, Cavallarin L, Giribaldi M, Giuliani F, et al. The effect of holder pasteurization on nutrients and biologically-active components in donor human milk: a review. Nutrients. 2016;8:477.
Ahrabi AF, Schanler RJ. Human milk is the only milk for premies in the NICU! Early Hum Dev. 2013;89:S51–3.
Boyd CA, Quigley MA, Brocklehurst P. Donor breast milk versus infant formula for preterm infants: systematic review and meta-analysis. Arch Dis Child - Fetal Neonatal Ed. 2007;92:F169–75.
Human Milk Banking Association of North America. Find a milk bank. Human Milk Banking Association of North America. 2019. https://www.hmbana.org/find-a-milk-bank/. Accessed 4 Oct 2019.
Human Milk Banking Association of North America. Guidelines for the establishment and operation of a donor human milk bank. Fort Worth: HMBANA; 2015, p. 78.
Hagadorn JI, Brownell EA, Lussier MM, Parker MGK, Herson VC. Variability of criteria for pasteurized donor human milk use: a survey of U.S. neonatal intensive care unit medical directors. J Parenter Enter Nutr. 2016;40:326–33.
Vieira AA, Soares FVM, Pimenta HP, Abranches AD, Moreira MEL. Analysis of the influence of pasteurization, freezing/thawing, and offer processes on human milk’s macronutrient concentrations. Early Hum Dev. 2011;87:577–80.
Cooper AR, Barnett D, Gentles E, Cairns L, Simpson JH. Macronutrient content of donor human breast milk. Arch Dis Child - Fetal Neonatal Ed. 2013;98:F539–41.
Centers for Disease Control and Prevention. Proper storage and preparation of breast milk. Centers for Disease Control and Prevention. 2019. https://www.cdc.gov/breastfeeding/recommendations/handling_breastmilk.htm. Accessed 22 Sep 2019.
Food and Drug Administration. Compliance program guidance manual. Food and Drug Administration. 2008. https://www.fda.gov/media/71685/download. Accessed 18 Dec 2018.
Koo W, Tice H. Human milk fortifiers do not meet the current recommendation for nutrients in very low birth weight infants. J Parenter Enter Nutr. 2017. https://doi.org/10.1177/0148607117713202.
Sauer CW, Kim JH. Human milk macronutrient analysis using point-of-care near-infrared spectrophotometry. J Perinatol. 2011;31:339–43.
Morlacchi L, Mallardi D, Giannì ML, Roggero P, Amato O, Piemontese P, et al. Is targeted fortification of human breast milk an optimal nutrition strategy for preterm infants? An interventional study. J Transl Med. 2016;14:195. https://doi.org/10.1186/s12967-016-0957-y.
Choi A, Fusch G, Rochow N, Fusch C. Target fortification of breast milk: predicting the final osmolality of the feeds. PloS ONE. 2016;11:e0148941.
Griffin IJ, Tancredi DJ, Bertino E, Lee HC, Profit J. Postnatal growth failure in very low birthweight infants born between 2005 and 2012. Arch Dis Child - Fetal Neonatal Ed. 2016;101:50–5.
Horbar JD, Ehrenkranz RA, Badger GJ, Edwards EM, Morrow KA, Soll RF, et al. Weight growth velocity and postnatal growth failure in infants 501 to 1500 grams: 2000-2013. Pediatrics. 2015;136:e84–92.
Ofek Shlomai N, Reichman B, Lerner-Geva L, Boyko V, Bar-Oz B. Collaboration with the Israel Neonatal Network. Population-based study shows improved postnatal growth in preterm very-low-birthweight infants between 1995 and 2010. Acta Paediatr. 2014;103:498–503.
Ehrenkranz RA, Younes N, Lemons JA, Fanaroff AA, Donovan EF, Wright LL, et al. Longitudinal growth of hospitalized very low birth weight infants. Pediatrics. 1999;104:280–9.
Sammallahti S, Pyhälä R, Lahti M, Lahti J, Pesonen A-K, Heinonen K, et al. Infant growth after preterm birth and neurocognitive abilities in young adulthood. J Pediatr. 2014;165:1109–15.e3.
Embleton NE, Pang N, Cooke RJ. Postnatal malnutrition and growth retardation: an inevitable consequence of current recommendations in preterm infants? Pediatrics. 2001;107:270–3.
Cohen M. Should human milk be regulated. UC Irvine Law Rev. 2018;2019:557–634.
Food and Drug Administration. Pediatric advisory committee flash minutes. Food and Drug Administration. https://wayback.archive-it.org/7993/20170404142951/https://www.fda.gov/downloads/AdvisoryCommittees/CommitteesMeetingMaterials/PediatricAdvisoryCommittee/UCM238627.pdf. Accessed on: 18 Dec 2018.
Food and Drug Administration. Use of donor human milk. Food and Drug Administration. 2018. https://www.fda.gov/science-research/pediatrics/use-donor-human-milk. Accessed 23 Sep 2019.
García-Lara NR, Escuder-Vieco D, García-Algar O, De la Cruz J, Lora D, Pallás-Alonso C. Effect of freezing time on macronutrients and energy content of breastmilk. Breastfeed Med. 2012;7:295–301.
García-Lara NR, Vieco DE, De la Cruz-Bértolo J, Lora-Pablos D, Velasco NU, Pallás-Alonso CR. Effect of holder pasteurization and frozen storage on macronutrients and energy content of breast milk. J Pediatr Gastroenterol Nutr. 2013;57:377–82.
Chang Y-C, Chen C-H, Lin M-C. The macronutrients in human milk change after storage in various containers. Pediatr Neonatol. 2012;53:205–9.
Martinez FE, Desai ID, Davidson AG, Nakai S, Radcliffe A. Ultrasonic homogenization of expressed human milk to prevent fat loss during tube feeding. J Pediatr Gastroenterol Nutr. 1987;6:593–7.
Meng T, Perrin MT, Allen JC, Osborne J, Jones F, Fogleman AD. Storage of unfed and leftover pasteurized human milk. Breastfeed Med. 2016;11:538–43.
Rochow N, Fusch G, Zapanta B, Ali A, Barui S, Fusch C. Target fortification of breast milk: how often should milk analysis be done? Nutrients. 2015;7:2297–310.
Author information
Authors and Affiliations
Contributions
DBJ drafted the manuscript, interpreted the data, critically revised the manuscript for important intellectual content, and approved and takes responsibility for the final content of the manuscript. JIH conceived and designed the study, interpreted the data, critically revised the manuscript for important intellectual content, and approved and takes responsibility for the final content of the manuscript. KCS acquired, analyzed, and interpreted the data, and approved and takes responsibility for the final content of the manuscript. PAE critically revised the manuscript for important intellectual content, and approved and takes responsibility for the final content of the manuscript. EAB conceived and designed the study, analyzed and interpreted the data, critically revised the manuscript for important intellectual content, and approved and takes responsibility for the final content of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
EAB serves in a volunteer capacity on the Research Advisory Board of the Mother’s Milk Bank Northeast. The other authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jo, D.B., Hagadorn, J.I., Smith, K.C. et al. Macronutrient analysis of donor human milk labelled as 24 kcal/oz. J Perinatol 40, 666–671 (2020). https://doi.org/10.1038/s41372-020-0624-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-020-0624-2
This article is cited by
-
A comparison of macronutrient-based methods for deriving energy values in human milk
Journal of Perinatology (2020)