Abstract
Objective
To compare the effect of umbilical cord milking (UCM) vs. early cord clamping (ECC) on cerebral blood flow (CBF).
Method
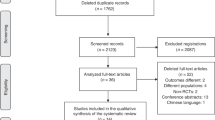
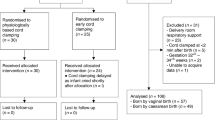
Preterm infants <31 weeks’ gestation were randomized to receive UCM or ECC at birth. Blood flow velocities and resistive & pulsatility indices of middle and anterior cerebral arteries were measured at 4–6 and 10–12 h after birth as an estimate of CBF.
Results
Randomization allocated 37 infants to UCM and 36 to ECC. Maternal and antenatal variables were similar. There were no significant differences between groups in middle or anterior CBF velocities and resistive indices at either study time point. CBF variables were not correlated with mean blood pressure, systemic blood flow, or intraventricular hemorrhage.
Conclusions
In very preterm infants, UCM compared with ECC was not shown to change CBF indices during the first 12 h of age or correlate with other hemodynamic measures or with intraventricular hemorrhage.
Trial registration
ClinicalTrials.gov: NCT01487187.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Katheria AC, Lakshminrusimha S, Rabe H, McAdams R, Mercer JS. Placental transfusion: a review. J Perinatol. 2017;37:105–11.
Katheria AC, Truong G, Cousins L, Oshiro B, Finer NN. Umbilical cord milking versus delayed cord clamping in preterm infants. Pediatrics. 2015;136:61–69.
Al-Wassia H, Shah PS. Efficacy and safety of umbilical cord milking at birth: a systematic review and meta-analysis. JAMA Pediatr. 2015;169:18–25.
Sweet DG, Carnielli V, Greisen G, Hallman M, Ozek E, Plavka R, et al. European Consensus Guidelines on the Management of Respiratory Distress Syndrome—2016 Update. Neonatology. 2017;111:107–25.
Hosono S, Mugishima H, Fujita H, Hosono A, Minato M, Okada T, et al. Umbilical cord milking reduces the need for red cell transfusions and improves neonatal adaptation in infants born less than 29 weeks’ gestation: a randomized controlled trial. Arch Dis Child Neonatal Fetal ed. 2008;93:F14–9.
Hosono S, Mugishima H, Fujita H, Hosono A, Okada T, Takahashi S, et al. Blood pressure and urine output during the first 120 h of life in infants born at less than 29 weeks’ gestation related to umbilical cord milking. Arch Dis Child Fetal Neonatal Ed. 2009;94:F328–31.
Katheria AC, Leone TA, Woelkers D, Garey DM, Rich W, Finer NN. The effects of umbilical cord milking on hemodynamics and neonatal outcomes in premature neonates. J Pediatr. 2014;164:1045–50.
Backes CH, Rivera BK, Haque U, Bridge JA, Smith CV, Hutchon DJ, et al. Placental transfusion strategies in very preterm neonates: a systematic review and meta-analysis. Obstet Gynecol 2014;124:47–56.
Katheria A, Blank D, Rich W, Finer N. Umbilical cord milking improves transition in premature infants at birth. PloS ONE. 2014; 9:e94085.
Blank DA, Polglase GR, Kluckow M, Gill AW, Crossley KJ, Moxham A, et al. Haemodynamic effects of umbilical cord milking in premature sheep during the neonatal transition. Arch Dis Child Fetal Neonatal Ed. 2018;103:F539–F546.
Takami T, Suganami Y, Sunohara D, Kondo A, Mizukaki N, Fujioka T, et al. Umbilical cord milking stabilizes cerebral oxygenation and perfusion in infants born before 29 weeks of gestation. J Pediatr. 2012;161:742–7.
El-Naggar W, Simpson D, Hussain A, Armson A, Dodds L, Warren A, et al. Cord milking versus immediate clamping in preterm infants: a randomised controlled trial. Arch Dis Child Fetal Neonatal Ed. 2019;104:F145–F150.
Popat H, Robledo KP, Sebastian L, Evans N, Gill A, Kluckow M, et al. Effect of delayed cord clamping on systemic blood flow: a randomized controlled trial. J Pediatr. 2016;178:81–86.
Nagano N, Saito M, Sugiura T, Miyahara F, Namba F, Ota E. Benefits of umbilical cord milking versus delayed cord clamping on neonatal outcomes in preterm infants: a systematic review and meta-analysis. PLoS ONE. 2018;13:e0201528.
Katheria AC, Reister F, Essers J, Mendler M, Hummler H, Subramaniam A, et al. Association of umbilical cord milking vs delayed umbilical cord clamping with death or severe intraventricular hemorrhage among preterm infants. JAMA. 2019;322:1877–86.
Banerjee J, Leung TS, Aladangady N. Cerebral blood flow and oximetry response to blood transfusion in relation to chronological age in preterm infants. Early Hum Dev. 2016;97:1–8.
Noori S, Anderson M, Soleymani S, Seri I. Effect of carbon dioxide on cerebral blood flow velocity in preterm infants during postnatal transition. Acta Paediatr. 2014;103:e334–9.
Bhatt S, Alison BJ, Wallace EM, Crossley KJ, Gill AW, Kluckow M, et al. Delaying cord clamping until ventilation onset improves cardiovascular function at birth in preterm lambs. J Physiol. 2013;591:2113–26.
Hooper SB, Te Pas AB, Lang J, van Vonderen JJ, Roehr CC, Kluckow M, et al. Cardiovascular transition at birth: a physiological sequence. Pediatr Res. 2015;77:608–14.
Niermeyer S, Velaphi S. Promoting physiologic transition at birth: re-examining resuscitation and the timing of cord clamping. Semin Fetal Neonatal Med. 2013;18:385–92.
Bhatt S, Polglase GR, Wallace EM, Te Pas AB, Hooper SB. Ventilation before umbilical cord clamping improves the physiological transition at birth. Front Pediatr. 2014;2:113.
Hansen NB, Stonestreet BS, Rosenkrantz TS, Oh W. Validity of Doppler measurements of anterior cerebral artery blood flow velocity: correlation with brain blood flow in piglets. Pediatrics. 1983;72:526–31.
Greisen G, Johansen K, Ellison PH, Fredriksen PS, Mali J, Friis-Hansen B. Cerebral blood flow in the newborn infant: comparison of Doppler ultrasound and 133xenon clearance. J Pediatr. 1984;104:411–8.
Benders MJ, Hendrikse J, de Vries L, Groenendaal F, van Bel F. Doppler- assessed cerebral blood flow velocity in the neonate as estimator of global cerebral blood volume flow measured using phase-contrast magnetic resonance angiography. Neonatology. 2013;103:21–6.
Pezzati M, Dani C, Biadaioli R, Filippi L, Biagiotti R, Giani T, et al. Early postnatal Doppler assessment of cerebral blood flow velocity in healthy preterm and term infants. Dev Med Child Neurol. 2002;44:745–52.
Gill AW. Postnatal cardiovascular adaptation. Arch Dis Child Fetal Neonatal Ed. 2019;104:F220–F224.
Baenziger O, Stolkin F, Keel M, von Siebenthal K, Fauchere JC, Das Kundu S, et al. The influence of the timing of cord clamping on postnatal cerebral oxygenation in preterm neonates: a randomized, controlled trial. Pediatrics. 2007;119:455–9.
Jaiswal P, Upadhyay A, Gothwal S, Chaudhary H, Tandon A. Comparison of umbilical cord milking and delayed cord clamping on cerebral blood flow in term neonates. Indian J Pediatr. 2015;82:890–5.
Shortland DB, Levene M, Archer N, Shaw D, Evans D. Cerebral blood flow velocity recordings and the prediction of intracranial haemorrhage and ischaemia. J Perinat Med. 1990;18:411–7.
Evans N, Kluckow M, Simmons M, Osborn D. Which to measure, systemic or organ blood flow? Middle cerebral artery and superior vena cava flow in very preterm infants. Arch Dis Child Fetal Neonatal Ed. 2002;87:F181–4.
Vesoulis ZA, Mathur AM. Cerebral autoregulation, brain injury, and the transitioning premature infant. Front Pediatr. 2017;5:64.
Rhee CJ, da Costa CS, Austin T, Brady KM, Czosnyka M, Lee JK. Neonatal cerebrovascular autoregulation. Pediatr Res. 2018;84:602–10.
Vutskits L. Cerebral blood flow in the neonate. Paediatr Anaesth. 2014;24:22–9.
Funding
This project was supported by grants from both Nova Scotia Health Research Foundation (PSO-EST-2013-9023 EGMS 1813) and IWK Research Foundation (1008052). No honorarium or other form of payment was given to anyone to produce this manuscript.
Author contributions
WE-N was involved in study design, Research Ethics Board (REB) approval, performing echocardiography studies, data review and manuscript preparation. DS was involved in conducting echocardiography studies, data review and manuscript reviewing. AH was involved in reading and interpreting echocardiography studies, data review and manuscript reviewing. AA was involved in study design, REB approval and manuscript reviewing. AW was involved in study design, REB approval and manuscript reviewing. RW was involved in study design, REB approval and manuscript reviewing. DM was involved in study design, REB approval, and manuscript reviewing. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
El-Naggar, W., McMillan, D., Hussain, A. et al. The effect of umbilical cord milking on cerebral blood flow in very preterm infants: a randomized controlled study. J Perinatol 41, 263–268 (2021). https://doi.org/10.1038/s41372-020-00780-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-020-00780-2