Abstract
Objective(s)
Quantify antimicrobial therapy (AMT) use in newborns with hypoxic-ischemic encephalopathy treated with therapeutic hypothermia (HIE/TH).
Study design
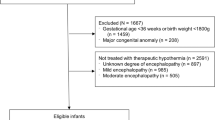
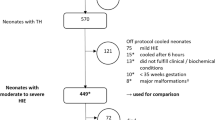
Newborns with HIE/TH were identified from the Children’s Hospital Neonatal Database (CHND). Early infection (onset ≤7 days of life) was defined as “confirmed” (culture proven) or “suspected infection” (culture negative but treated) and compared with a “no infection” group.
Results
1501/1534 (97.8%) neonates received AMT. 36 (2.3%) had confirmed, 255 (16.6%) suspected, and 1243 (81.0%) had no infection. The median (IQR) AMT duration was 13 (8–21), 8 (7–10), and 3 (3–7) days for the three groups, respectively (p < 0.001). AMT duration of use varied significantly across centers, adjusted for covariates (OR 1.88, 95% CI: 1.43–2.46).
Conclusion(s)
Incidence of early confirmed infection in neonates with HIE/TH (23/1000) is significantly higher than reported rates of early onset sepsis in term and near term infants (0.5–1.0/1000 live births). Antimicrobial-stewardship opportunities exist in infants with negative cultures.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Kurinczuk JJ, White-Koning M, Badawi N. Epidemiology of neonatal encephalopathy and hypoxic–ischaemic encephalopathy. Early Hum Dev 2010;86:329–38.
Gluckman PD, Gunn AJ, Wyatt JS. Hypothermia for neonates with hypoxic-ischemic encephalopathy. N Engl J Med. 2006;354:1643–5.
Shankaran S, Pappas A, McDonald SA, Vohr BR, Hintz SR, Yolton K, et al. Childhood outcomes after hypothermia for neonatal encephalopathy. N Engl J Med. 2012;366:2085–92.
Jacobs SE, Berg M, Hunt R, Tarnow-Mordi WO, Inder TE, Davis PG. Cooling for newborns with hypoxic ischaemic encephalopathy. Cochrane Database Syst Rev. 2013. https://doi.org/10.1002/14651858.CD003311.pub3.
Badawi N, Kurinczuk JJ, Keogh JM, Alessandri LM, O’Sullivan F, Burton PR, et al. Antepartum risk factors for newborn encephalopathy: the Western Australian case-control study. Br Med J. 1998;317:1549–53.
Martinez-Biarge M, Diez-Sebastian J, Wusthoff CJ, Mercuri E, Cowan FM. Antepartum and intrapartum factors preceding neonatal hypoxic-ischemic encephalopathy. Pediatrics. 2013;132:e952–9.
Zhao J, Chen Y, Xu Y, Pi G. Effect of intrauterine infection on brain development and injury. Int J Dev Neurosci. 2013;31:543–9.
Yuan T-M, Sun Y, Zhan C-Y, Yu H-M. Intrauterine infection/inflammation and perinatal brain damage: role of glial cells and Toll-like receptor signaling. J Neuroimmunol. 2010;229:16–25.
Lindberg TP, Caimano MJ, Hagadorn JI, Bennett EM, Maas K, Brownell EA, et al. Preterm infant gut microbial patterns related to the development of necrotizing enterocolitis. J Matern Fetal Neonatal Med. 2018:1–231. https://doi.org/10.1080/14767058.2018.1490719.
Gibson MK, Crofts TS, Dantas G. Antibiotics and the developing infant gut microbiota and resistome. Curr Opin Microbiol. 2015;27:51–6.
Lu J, Lu L, Yu Y, Cluette-Brown J, Martin CR, Claud EC. Effects of intestinal microbiota on brain development in humanized gnotobiotic mice. Sci Rep. 2018;8:5443.
Murthy K, Dykes FD, Padula MA, Pallotto EK, Reber KM, Durand DJ, et al. The Children’s Hospitals Neonatal Database: an overview of patient complexity, outcomes and variation in care. J Perinatol. 2014;34:582–6.
Massaro AN, Murthy K, Zaniletti I, Cook N, DiGeronimo R, Dizon ML, et al. Intercenter cost variation for perinatal hypoxic-ischemic encephalopathy in the era of therapeutic hypothermia. J Pediatr. 2016;173:76–83. e1.
Murthy K, Yanowitz TD, DiGeronimo R, Dykes FD, Zaniletti I, Sharma J, et al. Short-term outcomes for preterm infants with surgical necrotizing enterocolitis. J Perinatol. 2014;34:736–40.
Pasquali SK, Jacobs JP, Shook GJ, O’Brien SM, Hall M, Jacobs ML, et al. Linking clinical registry data with administrative data using indirect identifiers: implementation and validation in the congenital heart surgery population. Am Heart J. 2010;160:1099–104.
Mongelluzzo J, Mohamad Z, Ten Have TR, Shah SS. Corticosteroids and mortality in children with bacterial meningitis. JAMA. 2008;299:2048–55.
Massaro AN, Murthy K, Zaniletti I, Cook N, DiGeronimo R, Dizon M, et al. Short-term outcomes after perinatal hypoxic ischemic encephalopathy: a report from the Children’s Hospitals Neonatal Consortium HIE focus group. J Perinatol. 2015;35:290–6.
Shane AL, Sanchez PJ, Stoll BJ. Neonatal sepsis. Lancet. 2017;390:1770–80.
Simonsen KA, Anderson-Berry AL, Delair SF, Davies HD. Early-onset neonatal sepsis. Clin Microbiol Rev. 2014;27:21–47.
Keren R, Luan X, Localio R, Hall M, McLeod L, Dai D, et al. Prioritization of comparative effectiveness research topics in hospital pediatrics. Arch Pediatr Adolesc Med. 2012;166:1155–64.
Puopolo KM, Benitz WE, Zaoutis TE, Committee on Fetus and Newborn, Committee on Infectious Diseases. Management of neonates born at ≥35 0/7 weeks’ gestation with suspected or proven early-onset bacterial sepsis. Pediatrics. 2018;142:e20182894. https://doi.org/10.1542/peds.2018-2894.
Shankaran S, Laptook AR, Ehrenkranz RA, Tyson JE, McDonald SA, Donovan EF, et al. Whole-body hypothermia for neonates with hypoxic-ischemic encephalopathy. N Engl J Med. 2005;353:1574–84.
Hakobyan M, Dijkman KP, Laroche S, Naulaers G, Rijken M, Steiner K, et al. Outcome of infants with therapeutic hypothermia after perinatal asphyxia and early-onset sepsis. Neonatology. 2018;115:127–33.
Tann CJ, Nkurunziza P, Nakakeeto M, Oweka J, Kurinczuk JJ, Were J, et al. Prevalence of bloodstream pathogens is higher in neonatal encephalopathy cases vs. controls using a novel panel of real-time PCR assays. PLoS ONE. 2014;9:e97259.
Wu YW, Escobar GJ, Grether JK, Croen LA, Greene JD, Newman TB. Chorioamnionitis and cerebral palsy in term and near-term infants. JAMA. 2003;290:2677–84.
Falck M, Osredkar D, Maes E, Flatebo T, Wood TR, Sabir H, et al. Hypothermic neuronal rescue from infection-sensitised hypoxic-ischaemic brain injury is pathogen dependent. Dev Neurosci. 2017;39:238–47.
Osredkar D, Sabir H, Falck M, Wood T, Maes E, Flatebo T, et al. hypothermia does not reverse cellular responses caused by lipopolysaccharide in neonatal hypoxic-ischaemic brain injury. Dev Neurosci. 2015;37:390–7.
Osredkar D, Thoresen M, Maes E, Flatebo T, Elstad M, Sabir H. Hypothermia is not neuroprotective after infection-sensitized neonatal hypoxic-ischemic brain injury. Resuscitation. 2014;85:567–72.
Schrag SJ, Farley MM, Petit S, Reingold A, Weston EJ, Pondo T, et al. Epidemiology of invasive early-onset neonatal sepsis, 2005 to 2014. Pediatrics. 2016;138:e20162013. https://doi.org/10.1542/peds.2016-2013.
Nanduri SA, Petit S, Smelser C, Apostol M, Alden NB, Harrison LH, et al. Epidemiology of invasive early-onset and late-onset group B streptococcal disease in the United States, 2006 to 2015: multistate laboratory and population-based surveillance. JAMA Pediatr. 2019;173:224–33. https://doi.org/10.1001/jamapediatrics.2018.4826
Tann CJ, Martinello KA, Sadoo S, Lawn JE, Seale AC, Vega-Poblete M, et al. Neonatal encephalopathy with group B streptococcal disease worldwide: systematic review, investigator group datasets, and meta-analysis. Clin Infect Dis. 2017;65(suppl_2):S173–89.
Lakshminrusimha S, Shankaran S, Laptook A, McDonald S, Keszler M, Van Meurs K, et al. Pulmonary hypertension associated with hypoxic-ischemic encephalopathy-antecedent characteristics and comorbidities. J Pediatr. 2018;196:45–51. e3.
Tann CJ, Nakakeeto M, Willey BA, Sewegaba M, Webb EL, Oke I, et al. Perinatal risk factors for neonatal encephalopathy: an unmatched case-control study. Arch Dis Child Fetal Neonatal Ed. 2018;103:F250–6.
Schulman J, Dimand RJ, Lee HC, Duenas GV, Bennett MV, Gould JB. Neonatal intensive care unit antibiotic use. Pediatrics. 2015;135:826–33.
Soll RF, Edwards WH. Antibiotic use in neonatal intensive care. Pediatrics. 2015;135:928–9.
Kuzniewicz MW, Puopolo KM, Fischer A, Walsh EM, Li S, Newman TB, et al. A quantitative, risk-based approach to the management of neonatal early-onset sepsis. JAMA Pediatr. 2017;171:365–71.
Escobar GJ, Puopolo KM, Wi S, Turk BJ, Kuzniewicz MW, Walsh EM, et al. Stratification of risk of early-onset sepsis in newborns ≥34 weeks’ gestation. Pediatrics. 2014;133:30–6.
Polin RA, Committee on Fetus and Newborn. Management of neonates with suspected or proven early-onset bacterial sepsis. Pediatrics. 2012;129:1006–15.
Carola D, Vasconcellos M, Sloane A, McElwee D, Edwards C, Greenspan J, et al. Utility of early-onset sepsis risk calculator for neonates born to mothers with chorioamnionitis. J Pediatr. 2018;195:48–52. e1.
Jenster M, Bonifacio SL, Ruel T, Rogers EE, Tam EW, Partridge JC, et al. Maternal or neonatal infection: association with neonatal encephalopathy outcomes. Pediatr Res. 2014;76:93–9.
Saito J, Shibasaki J, Shimokaze T, Kishigami M, Ohyama M, Hoshino R, et al. Temporal relationship between serum levels of interleukin-6 and C-reactive protein in therapeutic hypothermia for neonatal hypoxic-ischemic encephalopathy. Am J Perinatol. 2016;33:1401–6.
Chiesa C, Signore F, Assumma M, Buffone E, Tramontozzi P, Osborn JF, et al. Serial measurements of C-reactive protein and interleukin-6 in the immediate postnatal period: reference intervals and analysis of maternal and perinatal confounders. Clin Chem. 2001;47:1016–22.
Laxminarayan R, Matsoso P, Pant S, Brower C, Rottingen JA, Klugman K, et al. Access to effective antimicrobials: a worldwide challenge. Lancet. 2016;387:168–75.
Hamer DH, Darmstadt GL, Carlin JB, Zaidi AK, Yeboah-Antwi K, Saha SK, et al. Etiology of bacteremia in young infants in six countries. Pediatr Infect Dis J. 2015;34:e1–8.
Panigrahi P, Chandel DS, Hansen NI, Sharma N, Kandefer S, Parida S, et al. Neonatal sepsis in rural India: timing, microbiology and antibiotic resistance in a population-based prospective study in the community setting. J Perinatol. 2017;37:911–21.
Cilla A, Arnaez J, Suarez J, Megias G, Cabrerizo M, Garcia-Alix A. Perinatal infection and hypoxic-ischemic encephalopathy: a pilot study. J Matern Fetal Neonatal Med. 2016;29:140–2.
Jenster M, Bonifacio SL, Ruel T, Rogers EE, Tam EW, Partridge JC, et al. Maternal or neonatal infection: association with neonatal encephalopathy outcomes. Pediatr Res. 2014;76:93.
Acknowledgements
We are indebted to the following institutions that serve the infants and their families; these institutions have also invested in, and continue to participate in the CHND. The site sponsors/contributors for the CHND are also included:
1. Children’s Healthcare of Atlanta, Atlanta, GA (Francine Dykes, Anthony Piazza)
2. Children’s Healthcare of Atlanta at Scottish Rite (Gregory Sysyn)
3. Children’s Hospital of Alabama, Birmingham, AL (Carl Coghill, Allison Black)
4. Le Bonheur Children’s Hospital, Memphis, TN (Ramasubbareddy Dhanireddy)
5. Children’s Hospital Boston, Boston, MA (Anne Hansen, Tanzeema Houssain)
6. Ann & Robert H. Lurie Children’s Hospital of Chicago, Chicago, IL (Karna Murthy, Gustave Falciglia)
7. Cincinnati Children’s Hospital, Cincinnati, OH (Beth Haberman, Breda Poindexter, Amy Nathan, Kristin Nelson, Paul Kingma, Stefanie Riddle, Stephanie Merhar, Heather Kaplan)
8. Nationwide Children’s Hospital, Columbus, OH (Kristina Reber)
9. Children’s Medical Center, Dallas, TX (Rashmin Savani, Luc Brion, Noorjahan Ali)
10. Children’s Hospital Colorado, Aurora, CO (Theresa Grover)
11. Children’s Hospital of Michigan, Detroit, MI (Girija Natarajan)
12. Cook Children’s Health Care System, Fort Worth, TX (Jonathan Nedrelow, Annie Chi, Yvette Johnson)
13. Texas Children’s Hospital, Houston, TX (Gautham Suresh)
14. Riley Children’s Hospital, Indianapolis, IN (William Engle, Lora Simpson, Gregory Sokol)
15. Children’s Mercy Hospitals & Clinics, Kansas City, MO (Eugenia Pallotto)
16. Arkansas Children’s Hospital, Little Rock, AR (Robert Lyle, Becky Rogers)
17. Children’s Hospital Los Angeles, Los Angeles, CA (Lisa Kelly [deceased], Steven Chin, Rachel Chapman)
18. American Family Children’s Hospital, Madison, WI (Jamie Limjoco, Lori Haack)
19. Children’s Hospital & Research Center Oakland, Oakland, CA (David Durand, Jeanette Asselin, Art D’Harlingue, Priscilla Joe)
20. The Children’s Hospital of Philadelphia, Philadelphia, PA (Jacquelyn Evans, Michael Padula, David Munson)
21. St. Christopher’s Hospital for Children, Philadelphia, PA (Suzanne Touch)
22. Children’s Hospital of Pittsburgh of UPMC, Pittsburgh, PA (Beverly Brozanski)
23. St. Louis Children’s Hospital, St Louis, MO (Tasnim Najaf, Rakesh Rao, Amit Mathur)
24. All Children’s Hospital, St. Petersburg, FL (Victor McKay)
25. Rady Children’s Hospital, San Diego, CA (Mark Speziale, Brian Lane, Laural Moyer)
26. Children’s National Medical Center, Washington, DC (Billie Short)
27. AI DuPont Hospital for Children, Wilmington, DE (Kevin Sullivan)
28. Primary Children’s Medical Center, Salt Lake City, UT (Con Yee Ling)
29. Children’s Hospital of Wisconsin, Milwaukee, WI (Michael Uhing, Ankur Datta)
30. Children’s Hospital of Omaha (Lynne Willett, Nicole Birge)
31. Florida Hospital for Children (Rajan Wadhawan)
32. Seattle Children’s Hospital, Seattle, WA (Elizabeth Jacobsen-Misbe, Robert DiGeronimo, Zeenia Billimoria)
33. Hospital for Sick Children, Toronto, ON (Kyong-Soon Lee)
34. Children’s Hospital Orange County, Los Angeles, CA (Michel Mikhael, Irfan Ahmad)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
IZ is an employee of Children’s Hospitals Association, Inc, (Overland Park, KS). KM is a Board member of the Children’s Hospital National Consortium (CHNC, Kansas City, MO). All other authors have no financial disclosures relevant to this article to disclose. KM is a Board member of the Children’s Hospital National Consortium (CHNC, Kansas City, MO). All other authors have no conflicts of interest relevant to this article to disclose.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Data presented in the manuscript were presented partially (abstract) at the Pediatric Academic Societies meeting in Toronto, Canada, in May 2018.
Rights and permissions
About this article
Cite this article
Rao, R., Lee, KS., Zaniletti, I. et al. Antimicrobial therapy utilization in neonates with hypoxic-ischemic encephalopathy (HIE): a report from the Children’s Hospital Neonatal Database (CHND). J Perinatol 40, 70–78 (2020). https://doi.org/10.1038/s41372-019-0527-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-019-0527-2
This article is cited by
-
The importance of not increasing confusion around neonatal encephalopathy and hypoxic-ischemic encephalopathy
Pediatric Research (2023)
-
Azithromycin reduces inflammation-amplified hypoxic–ischemic brain injury in neonatal rats
Pediatric Research (2022)
-
Noninfectious influencers of early-onset sepsis biomarkers
Pediatric Research (2022)