Abstract
Objective
To compare the differential effects of the retinopathy of prematurity (ROP) examination on the physiology of premature infants with and without oxygen support.
Study Design
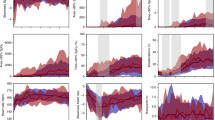
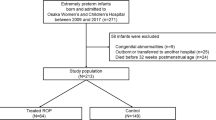
We collected data from 42 premature infants (room air = 19, oxygen support = 23) and compared physiological metrics including heart rate (HR), systemic peripheral saturation (SpO2), mesenteric tissue oxygen saturation (StO2) and clinical events (oxygen desaturation episodes, bradycardia events, and gastric residuals).
Results
We found significant differences between groups in HR during and briefly after the exam, and in mesenteric StO2, during eye drop administration, eye exam, and up to 8 min after the exam. SpO2 was significantly different between the groups at all time points. Gastric residuals were higher after the exam in infants on oxygen support, compared to baseline.
Conclusion
Premature infants on oxygen support may be at a higher risk of adverse physiologic effects in response to the ROP exam.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Hellström A, Smith LEH, Dammann O. Retinopathy of prematurity. Lancet. 2013;382:1445–57.
Grabska J, Walden P, Lerer T, Kelly C, Hussain N, Donovan T, et al. Can oral sucrose reduce the pain and distress associated with screening for retinopathy of prematurity? J Perinatol. 2005;25:33–5.
Belda S, Pallás CR, De la Cruz J, Tejada P. Screening for retinopathy of prematurity: is it painful? Biol Neonate. 2004;86:195–200.
Şener Taplak A, Erdem E. A Comparison of breast milk and sucrose in reducing neonatal pain during eye exam for retinopathy of prematurity. Breastfeed Med. 2017;12:305–10.
Mitchell A, Hall RW, Erickson SW, Yates C, Hendrickson H. Systemic absorption of cyclopentolate and adverse events after retinopathy of prematurity exams. Curr Eye Res. 2016;41:1601–7.
Reid B, Wang H, Guillet R. Apnea after routine eye examinations in premature infants. Am J Perinatol. 2017;34:199–203.
Bonthala S, Sparks JW, Musgrove KH, Berseth CL. Mydriatics slow gastric emptying in preterm infants. J Pediatr. 2000;137:327–30.
Cohen AM, Cook N, Harris MC, Ying G-S, Binenbaum G. The pain response to mydriatic eyedrops in preterm infants. J Perinatol. 2013;33:462–5.
Degirmencioglu H, Oncel MY, Calisici E, Say B, Uras N, Dilmen U. Transient ileus associated with the use of mydriatics after screening for retinopathy of prematurity in a very low birth weight infant. J Pediatr Ophthalmol Strabismus. 2014;51:e44–47.
Ozgun U, Demet T, Ozge KA, Zafer D, Murat S, Mehmet Y, et al. Fatal necrotising enterocolitis due to mydriatic eye drops. J Coll Physicians Surg--Pak Jcpsp. 2014;24(Suppl 2):S147–9.
Cortez J, Gupta M, Amaram A, Pizzino J, Sawhney M, Sood BG. Noninvasive evaluation of splanchnic tissue oxygenation using near-infrared spectroscopy in preterm neonates. J Matern-Fetal Neonatal Med. 2011;24:574–82.
Ophthalmology AAOPS on, Ophthalmology AAO, Strabismus AA for POA, Orthoptists AA of C. Screening examination of premature infants for retinopathy of prematurity. Pediatrics. 2013;131:189–95.
Papile L-A, Burstein J, Burstein R, Koffler H. Incidence and evolution of subependymal and intraventricular hemorrhage: A study of infants with birth weights less than 1,500 gm. J Pediatr. 1978;92:529–34.
Naulaers G, Meyns B, Miserez M, Leunens V, Van Huffel S, Casaer P, et al. Use of tissue oxygenation index and fractional tissue oxygen extraction as non-invasive parameters for cerebral oxygenation. A validation study in piglets. Neonatology. 2007;92:120–6.
Thoyre SM, Carlson J. Occurrence of oxygen desaturation events during preterm infant bottle feeding near discharge. Early Hum Dev. 2003;72:25–36.
Harsha SS, Archana BR. SNAPPE-II (Score for Neonatal Acute Physiology with Perinatal Extension-II) in Predicting Mortality and Morbidity in NICU. J Clin Diagn Res Jcdr. 2015;9:SC10–2.
Marsh VA, Young WO, Dunaway KK, Kissling GE, Carlos RQ, Jones SM, et al. Efficacy of topical anesthetics to reduce pain in premature infants during eye examinations for retinopathy of prematurity. Ann Pharmacother. 2005;39:829–33.
Yang AY, Chow J, Liu J. Corneal innervation and sensation: the eye and beyond. Yale J Biol Med. 2018;91:13–21.
Boron WF, Boulpaep EL, editors. Medical physiology. Third edition. Philadelphia, PA: Elsevier; 2017. p. 1297.
Tan JBC, Boskovic DS, Angeles DM. The energy costs of prematurity and the neonatal intensive care unit (NICU) Experience. Antioxidants. 2018;7:37.
McEwen BS. Stress, adaptation, and disease. Allostasis and allostatic load. Ann N Y Acad Sci. 1998;840:33–44.
Akotia DH, Durham JT, Arnell KM, Petruzzelli DL, Katheria AC. Relationship between near-infrared spectroscopy and transabdominal ultrasonography: noninvasive monitoring of intestinal function in neonates. Med Sci Monit Int Med J Exp Clin Res. 2016;22:61–8.
Sun X, Lemyre B, Barrowman N, O’Connor M. Pain management during eye examinations for retinopathy of prematurity in preterm infants: a systematic review. Acta Paediatr Oslo Nor 1992. 2010;99:329–34.
Kandasamy Y, Smith R, Wright IMR, Hartley L. Pain relief for premature infants during ophthalmology assessment. J AAPOS Publ Am Assoc Pediatr Ophthalmol Strabismus. 2011;15:276–80.
Samra HA, McGrath JM. Pain management during retinopathy of prematurity eye examinations: a systematic review. Adv Neonatal Care. 2009;9:99–110.
Belmonte C, Acosta MC, Merayo-Lloves J, Gallar J. What causes eye pain? Curr Ophthalmol Rep. 2015;3:111–21.
Trevino R, Stewart B. Change in intraocular pressure during scleral depression. J Optom. 2015;8:244–51.
Estévez-Herrera J, González-Santana A, Baz-Dávila R, Machado JD, Borges R. The intravesicular cocktail and its role in the regulation of exocytosis. J Neurochem. 2016;137:897–903.
Zhao J, Gonzalez F, Mu D. Apnea of prematurity: from cause to treatment. Eur J Pediatr. 2011;170:1097–105.
Ludington-Hoe SM, Anderson GC, Swinth JY, Thompson C, Hadeed AJ. Randomized controlled trial of kangaroo care: cardiorespiratory and thermal effects on healthy preterm infants. Neonatal Netw Nn. 2004;23:39–48.
Hunt F. The importance of kangaroo care on infant oxygen saturation levels and bonding. J Neonatal Nurs. 2008;14:47–51.
Bloch-Salisbury E, Zuzarte I, Indic P, Bednarek F, Paydarfar D. Kangaroo care: cardio-respiratory relationships between the infant and caregiver. Early Hum Dev. 2014;90:843–50.
Acknowledgements
We thank Dorothy Forde RN, Erin Hoch RN, Elena Kim-Saesim RN, and Sharon Lee RN for identifying and consenting subjects. We thank the LLU NICU physicians and nurses for their support. We thank the parents for allowing their babies to be part of this study.
Author Contribution
AH and DMA conceived the original idea and planned the experiments. JBCT and JD performed the experiments. JBCT worked out the technical details and calculations. JCBT and DMA wrote the manuscript. CGW and all co-authors contributed, revised and provided critical feedback and helped shape the research, analysis and manuscript.
Funding
This work was supported in part by NIH grant R01 NR011209 (DMA).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tan, J.B.C., Dunbar, J., Hopper, A. et al. Differential effects of the retinopathy of prematurity exam on the physiology of premature infants. J Perinatol 39, 708–716 (2019). https://doi.org/10.1038/s41372-019-0331-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-019-0331-z