Abstract
Objective
To investigate whether maternal overweight and obesity increased the risk of fetal acidosis measured in umbilical cord arterial blood after delivery.
Study design
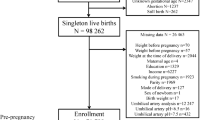
Population-based cohort study of 84,785 term (≥37 weeks) infants. Logistic regression was used to estimate risks of fetal acidosis in umbilical cord arterial blood. Fetal acidosis was defined as pH <7.10 or as pH <1st percentile on a normal reference curve.
Result
Risks of fetal acidosis increased, regardless of definition, with maternal overweight and obesity severity. Compared to normal weight (BMI 18.5–<25), the odds ratios (95% confidence interval) for pH <7.10 were 1.35 (1.23–1.47) for overweight (BMI 25–<30), 1.46 (1.27–1.69) for mild obesity (BMI 30–<35), and 1.75 (1.42–2.15) for severe obesity (BMI ≥35). The association for obesity was attenuated in analyses restricted to non-instrumental vaginal deliveries.
Conclusion
Maternal overweight and obesity increased the risk of fetal acidosis. More complicated deliveries in obese women may partially explain this association.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Owe KM. Weight in early pregnancy and outcomes in early infancy. BMJ. 2014;349:g6850.
Villamor E, Cnattingius S. Interpregnancy weight change and risk of adverse pregnancy outcomes: a population-based study. Lancet. 2006;368:1164–70.
Cnattingius S, Villamor E, Johansson S, Edstedt Bonamy AK, Persson M, Wikstrom AK, et al. Maternal obesity and risk of preterm delivery. JAMA. 2013;309:2362–70.
Persson M, Johansson S, Villamor E, Cnattingius S. Maternal overweight and obesity and risks of severe birth-asphyxia-related complications in term infants: a population-based cohort study in Sweden. PLoS Med. 2014;11:e1001648.
Johansson S, Villamor E, Altman M, Bonamy AK, Granath F, Cnattingius S. Maternal overweight and obesity in early pregnancy and risk of infant mortality: a population based cohort study in Sweden. BMJ. 2014;349:g6572.
Villamor E, Tedroff K, Peterson M, Johansson S, Neovius M, Petersson G, et al. Association between maternal body mass index in early pregnancy and incidence of cerebral palsy. JAMA. 2017;317:925–36.
Persson M, Johansson S, Cnattingius S. Inter-pregnancy weight change and risks of severe birth-asphyxia-related outcomes in singleton infants born at term: a nationwide Swedish cohort study. PLoS Med. 2016;13:e1002033.
Malin GL, Morris RK, Khan KS. Strength of association between umbilical cord pH and perinatal and long term outcomes: systematic review and meta-analysis. BMJ. 2010;340:c1471.
Yeh P, Emary K, Impey L. The relationship between umbilical cord arterial pH and serious adverse neonatal outcome: analysis of 51,519 consecutive validated samples. BJOG. 2012;119:824–31.
Sebastian Manzanares G, Angel Santalla H, Irene Vico Z, Lopez Criado MS, Alicia Pineda L, Jose Luis Gallo V. Abnormal maternal body mass index and obstetric and neonatal outcome. J Matern Fetal Neonatal Med. 2012;25:308–12.
Raja UA, McAree T, Bassett P, Sharma S. The implications of a raised maternal BMI: a DGH experience. J Obstet Gynaecol. 2012;32:247–51.
Maisonneuve E, Audibert F, Guilbaud L, Lathelize J, Jousse M, Pierre F, et al. Risk factors for severe neonatal acidosis. Obstet Gynecol. 2011;118:818–23.
Magann EF, Doherty DA, Sandlin AT, Chauhan SP, Morrison JC. The effects of an increasing gradient of maternal obesity on pregnancy outcomes. Aust N Z J Obstet Gynaecol. 2013;53:250–7.
Madi SRC, Garcia RMR, Souza VC, Rombaldi RL, Araujo BF, Madi JM. Effect of obesity on gestational and perinatal outcomes. Rev Bras Ginecol Obstet. 2017;39:330–6.
Conner SN, Tuuli MG, Longman RE, Odibo AO, Macones GA, Cahill AG. Impact of obesity on incision-to-delivery interval and neonatal outcomes at cesarean delivery. Am J Obstet Gynecol. 2013;209:386. e1-6
EpC. The Swedish Medical Birth Register: a summary of content and quality. 2003. Available at http://www.socialstyrelsen.se/Lists/Artikelkatalog/Attachments/10655/2003-112-3_20031123.pdf.
Brooke HL, Talback M, Hornblad J, Johansson LA, Ludvigsson JF, Druid H, et al. The Swedish cause of death register. Eur J Epidemiol. 2017;32:765–773.
Ludvigsson JF, Andersson E, Ekbom A, Feychting M, Kim JL, Reuterwall C, et al. External review and validation of the Swedish national inpatient register. BMC Public Health. 2011;11:450.
Hogberg U, Larsson N. Early dating by ultrasound and perinatal outcome. A cohort study. Acta Obstet Gynecol Scand. 1997;76:907–12.
Marsal K, Persson PH, Larsen T, Lilja H, Selbing A, Sultan B. Intrauterine growth curves based on ultrasonically estimated foetal weights. Acta Paediatr. 1996;85:843–8.
Diagnose codes in the Swedish version of iCD10 (Q00-Q99) not reported to the Surveillance Register of Birth Defects 2010 [2017-10-25]. Available at http://www.socialstyrelsen.se/register/halsodataregister/medicinskafodelseregistret/Documents/diagnoser-som-inte-ska-rapporteras.pdf.
Skiold B, Petersson G, Ahlberg M, Stephansson O, Johansson S. Population-based reference curve for umbilical cord arterial pH in infants born at 28 to 42 weeks. J Perinatol. 2017;37:254–9.
Sandstrom A, Altman M, Cnattingius S, Johansson S, Ahlberg M, Stephansson O. Durations of second stage of labor and pushing, and adverse neonatal outcomes: a population-based cohort study. J Perinatol. 2017;37:236–42.
Kominiarek MA, Zhang J, Vanveldhuisen P, Troendle J, Beaver J, Hibbard JU. Contemporary labor patterns: the impact of maternal body mass index. Am J Obstet Gynecol. 2011;205:244.e1-8
Carlhall S, Kallen K, Blomberg M. Maternal body mass index and duration of labor. Eur J Obstet Gynecol Reprod Biol. 2013;171:49–53.
Morken NH, Klungsoyr K, Magnus P, Skjaerven R. Pre-pregnant body mass index, gestational weight gain and the risk of operative delivery. Acta Obstet Gynecol Scand. 2013;92:809–15.
Hermann M, Le Ray C, Blondel B, Goffinet F, Zeitlin J. The risk of prelabor and intrapartum cesarean delivery among overweight and obese women: possible preventive actions. Am J Obstet Gynecol. 2015;212:241. e1-9
Edwards RK, Cantu J, Cliver S, Biggio JR Jr, Owen J, Tita AT. The association of maternal obesity with fetal pH and base deficit at cesarean delivery. Obstet Gynecol. 2013;122(2 Pt 1):262–7.
Funding
Supported by the Stockholm County Council (ALF No. 20150118) and the Swedish Research Council for Health, Working Life and Welfare (No. 2014-0073). The funders had no involvement in study design, collection, analysis, and/or interpretation of data, writing of the report, or the decision to submit the paper for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Johansson, S., Sandström, A. & Cnattingius, S. Maternal overweight and obesity increase the risk of fetal acidosis during labor. J Perinatol 38, 1144–1150 (2018). https://doi.org/10.1038/s41372-018-0144-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-018-0144-5
This article is cited by
-
Trends in Apgar scores and umbilical artery pH: a population-based cohort study on 10,696,831 live births in Germany, 2008–2022
European Journal of Pediatrics (2024)
-
Maternal pre-pregnancy body mass index and foetal acidosis in vaginal and caesarean deliveries: The Japan Environment and Children’s Study
Scientific Reports (2021)
-
Gestational weight gain and foetal acidosis in vaginal and caesarean deliveries: The Japan Environment and Children’s Study
Scientific Reports (2020)