Abstract
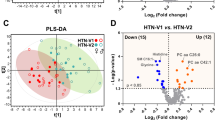
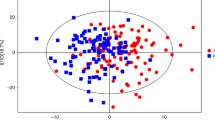
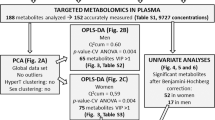
The regulatory mechanisms of hypertension in youth are incompletely understood. We aimed to identify potential serum metabolic alterations associated with hypertension in adolescents. A 1:1 age- and sex-matched case-control study including 30 hypertensive adolescents aged 12–17 years and 30 normotensive adolescents for the training set and 14 hypertensive adolescents and 14 normotensive adolescents for the test set was performed, which came from one cross-sectional study in Ningxia, China. Hypertension was defined based on blood pressure (BP) values measured on three different occasions according to the BP reference of Chinese children and adolescents. Untargeted ultra-high-performance liquid tandem chromatography quadrupole time of flight mass spectrometry was used to identify differential metabolites between hypertensive and normotensive adolescents. A total of 77 metabolites in positive mode and 101 in negative mode were identified (VIP > 1.0 and P < 0.05). After adjustment for the false discovery rate, 4 differential metabolites in positive mode and 10 in negative mode were found (Q value < 0.05). The logistic regression model adjusted for body mass index and lipid profile selected four significant metabolites (4-hydroxybutanoic acid, L-serine, acetone, and pterostilbene). The main metabolic pathways of amino acid metabolism, pantothenate and CoA biosynthesis, glyoxylate and dicarboxylate metabolism, fructose and mannose metabolism, and linoleic acid metabolism may contribute to the development of hypertension in Chinese adolescents. Based on the receiver operating characteristic plot, 4-hydroxybutanoic acid, L-serine, acetone, and pterostilbene may preliminarily help distinguish hypertension from normal BP in adolescents, with AUC values of 0.857 in the training set and 0.934 in the test set. The identified metabolites and pathways may foster a better understanding of hypertension pathogenesis in Chinese adolescents.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
Data is available from the corresponding author BX (Email: xibo2007@126.com).
References
Zhou M, Wang H, Zeng X, Yin P, Zhu J, Chen W, et al. Mortality, morbidity, and risk factors in china and its provinces, 1990–2017: a systematic analysis for the global burden of disease study 2017. Lancet.2019;394:1145–58.
Song P, Zhang Y, Yu J, Zha M, Zhu Y, Rahimi K, et al. Global prevalence of hypertension in children: a systematic review and meta-analysis. JAMA Pediatr. 2019:1–10.
Yang L, Magnussen CG, Yang L, Bovet P, Xi B. Elevated blood pressure in childhood or adolescence and cardiovascular outcomes in adulthood: a systematic review. Hypertension.2020;75:948–55.
Wurtz P, Raiko JR, Magnussen CG, Soininen P, Kangas AJ, Tynkkynen T, et al. High-throughput quantification of circulating metabolites improves prediction of subclinical atherosclerosis. Eur Heart J. 2012;33:2307–16.
Surendran P, Drenos F, Young R, Warren H, Cook JP, Manning AK, et al. Trans-ancestry meta-analyses identify rare and common variants associated with blood pressure and hypertension. Nat Genet. 2016;48:1151–61.
Evangelou E, Warren HR, Mosen-Ansorena D, Mifsud B, Pazoki R, Gao H, et al. Genetic analysis of over 1 million people identifies 535 new loci associated with blood pressure traits. Nat Genet. 2018;50:1412–25.
Warembourg C, Maitre L, Tamayo-Uria I, Fossati S, Roumeliotaki T, Aasvang GM, et al. Early-life environmental exposures and blood pressure in children. J Am Coll Cardiol. 2019;74:1317–28.
Carey RM, Muntner P, Bosworth HB, Whelton PK. Prevention and control of hypertension: Jacc health promotion series. J Am Coll Cardiol. 2018;72:1278–93.
Holmes E, Loo RL, Stamler J, Bictash M, Yap IK, Chan Q, et al. Human metabolic phenotype diversity and its association with diet and blood pressure. Nature.2008;453:396–400.
Zheng Y, Yu B, Alexander D, Mosley TH, Heiss G, Nettleton JA, et al. Metabolomics and incident hypertension among blacks: the atherosclerosis risk in communities study. Hypertension.2013;62:398–403.
Menni C, Graham D, Kastenmuller G, Alharbi NH, Alsanosi SM, McBride M, et al. Metabolomic identification of a novel pathway of blood pressure regulation involving hexadecanedioate. Hypertension.2015;66:422–9.
Hao Y, Wang Y, Xi L, Li G, Zhao F, Qi Y, et al. A nested case-control study of association between metabolome and hypertension risk. Biomed Res Int. 2016;2016:7646979.
Walejko JM, Kim S, Goel R, Handberg EM, Richards EM, Pepine CJ, et al. Gut microbiota and serum metabolite differences in african americans and white americans with high blood pressure. Int J Cardiol. 2018;271:336–9.
He WJ, Li C, Mi X, Shi M, Gu X, Bazzano LA, et al. An untargeted metabolomics study of blood pressure: findings from the bogalusa heart study. J Hypertens. 2020;38:1302–11.
Vignoli A, Tenori L, Luchinat C, Saccenti E. Age and sex effects on plasma metabolite association networks in healthy subjects. J Proteome Res. 2018;17:97–107.
Dunn WB, Broadhurst D, Begley P, Zelena E, Francis-McIntyre S, Anderson N, et al. Procedures for large-scale metabolic profiling of serum and plasma using gas chromatography and liquid chromatography coupled to mass spectrometry. Nat Protoc. 2011;6:1060–83.
Meng L, Hou D, Shan X, Mi J. Accuracy evaluation of omron hem-7012 electronic sphygmomanometers in measuring blood pressure of children and adolescents. Chin J Hypertension. 2013;21:158–62.
Mi J, Wang TY, Meng LH, G.J. Z, Han SM, Zhong Y, et al. Development of blood pressure reference standards for chinese children and adolescents. Chin J Evid Based Pediatr. 2010;5:4–14.
Storey JD, Tibshirani R. Statistical significance for genomewide studies. Proc Natl Acad Sci USA. 2003;100:9440–5.
Zhang ZY, Marrachelli VG, Yang WY, Trenson S, Huang QF, Wei FF, et al. Diastolic left ventricular function in relation to circulating metabolic biomarkers in a population study. Eur J Prev Cardiol. 2019;26:22–32.
Wang L, Hou E, Wang L, Wang Y, Yang L, Zheng X, et al. Reconstruction and analysis of correlation networks based on gc-ms metabolomics data for young hypertensive men. Anal Chim Acta. 2015;854:95–105.
Contaifer D Jr, Buckley LF, Wohlford G, Kumar NG, Morriss JM, Ranasinghe AD, et al. Metabolic modulation predicts heart failure tests performance. PLoS ONE. 2019;14:e0218153.
Poggiogalle E, Fontana M, Giusti AM, Pinto A, Iannucci G, Lenzi A, et al. Amino acids and hypertension in adults. Nutrients. 2019;11.
Aggoun Y, Farpour-Lambert NJ, Marchand LM, Golay E, Maggio AB, Beghetti M. Impaired endothelial and smooth muscle functions and arterial stiffness appear before puberty in obese children and are associated with elevated ambulatory blood pressure. Eur Heart J. 2008;29:792–9.
Li X, Kumar A, Carmeliet P. Metabolic pathways fueling the endothelial cell drive. Annu Rev Physiol. 2019;81:483–503.
Rochette L, Lorin J, Zeller M, Guilland JC, Lorgis L, Cottin Y, et al. Nitric oxide synthase inhibition and oxidative stress in cardiovascular diseases: possible therapeutic targets? Pharm Ther. 2013;140:239–57.
Wang TJ, Larson MG, Vasan RS, Cheng S, Rhee EP, McCabe E, et al. Metabolite profiles and the risk of developing diabetes. Nat Med. 2011;17:448–53.
Tibbetts AS, Appling DR. Compartmentalization of mammalian folate-mediated one-carbon metabolism. Annu Rev Nutr. 2010;30:57–81.
Mels CM, Delles C, Louw R, Schutte AE. Central systolic pressure and a nonessential amino acid metabolomics profile: the african prospective study on the early detection and identification of cardiovascular disease and hypertension. J Hypertens. 2019;37:1157–66.
Dumas SJ, Bru-Mercier G, Courboulin A, Quatredeniers M, Rucker-Martin C, Antigny F, et al. Nmda-type glutamate receptor activation promotes vascular remodeling and pulmonary arterial hypertension. Circulation.2018;137:2371–89.
Mangge H, Stelzer I, Reininghaus EZ, Weghuber D, Postolache TT, Fuchs D. Disturbed tryptophan metabolism in cardiovascular disease. Curr Med Chem. 2014;21:1931–7.
Siomkajlo M, Rybka J, Mierzchala-Pasierb M, Gamian A, Stankiewicz-Olczyk J, Bolanowski M, et al. Specific plasma amino acid disturbances associated with metabolic syndrome. Endocrine.2017;58:553–62.
Yamaguchi N, Mahbub MH, Takahashi H, Hase R, Ishimaru Y, Sunagawa H, et al. Plasma free amino acid profiles evaluate risk of metabolic syndrome, diabetes, dyslipidemia, and hypertension in a large asian population. Environ Health Prev Med. 2017;22:35.
Yang R, Dong J, Zhao H, Li H, Guo H, Wang S, et al. Association of branched-chain amino acids with carotid intima-media thickness and coronary artery disease risk factors. PLoS ONE. 2014;9:e99598.
Zhenyukh O, Gonzalez-Amor M, Rodrigues-Diez RR, Esteban V, Ruiz-Ortega M, Salaices M, et al. Branched-chain amino acids promote endothelial dysfunction through increased reactive oxygen species generation and inflammation. J Cell Mol Med. 2018;22:4948–62.
Mirmiran P, Teymoori F, Asghari G, Azizi F. Dietary intakes of branched chain amino acids and the incidence of hypertension: a population-based prospective cohort study. Arch Iran Med. 2019;22:182–8.
Lee S, Zhang C, Kilicarslan M, Piening BD, Bjornson E, Hallstrom BM, et al. Integrated network analysis reveals an association between plasma mannose levels and insulin resistance. Cell Metab. 2016;24:172–84.
Wang F, Han L, Hu D. Fasting insulin, insulin resistance and risk of hypertension in the general population: a meta-analysis. Clin Chim Acta. 2017;464:57–63.
Zhao H, Zhang Y, Liu B, Zhang L, Bao M, Li L, et al. A pilot study to identify the longitudinal serum metabolite profiles to predict the development of hyperuricemia in essential hypertension. Clin Chim Acta. 2020;510:466–74.
Rotroff DM, Shahin MH, Gurley SB, Zhu H, Motsinger-Reif A, Meisner M, et al. Pharmacometabolomic assessments of atenolol and hydrochlorothiazide treatment reveal novel drug response phenotypes. CPT Pharmacomet Syst Pharmacol. 2015;4:669–79.
Riche DM, Riche KD, Blackshear CT, McEwen CL, Sherman JJ, Wofford MR, et al. Pterostilbene on metabolic parameters: a randomized, double-blind, and placebo-controlled trial. Evid Based Complement Altern Med. 2014;2014:459165.
Hicks AR, Varner KJ. Cardiovascular responses elicited by intragastric administration of bdl and ghb. J Recept Signal Transduct Res. 2008;28:429–36.
Zhong L, Zhang JP, Nuermaimaiti AG, Yunusi KX. Study on plasmatic metabolomics of uygur patients with essential hypertension based on nuclear magnetic resonance technique. Eur Rev Med Pharm Sci. 2014;18:3673–80.
Acknowledgements
We are thankful to the National Natural Science Foundation of China for the funding support.
Funding
This work was supported by the National Natural Science Foundation of China (81722039, 81673195).
Author information
Authors and Affiliations
Contributions
Study design: BX. Data collection: WD, MZ. Analysis and interpretation of data: JS, XL. Drafting of the paper: JS, WD. Approval of the final version for publication: all the authors.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
The study protocol was approved by the Institutional Ethics Review Board of the School of Public Health, Shandong University.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Sun, J., Ding, W., Liu, X. et al. Serum metabolites of hypertension among Chinese adolescents aged 12–17 years. J Hum Hypertens 36, 925–932 (2022). https://doi.org/10.1038/s41371-021-00602-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41371-021-00602-8