Abstract
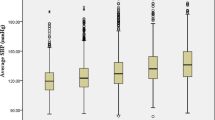
Often a single blood pressure (BP) measurement is used to diagnose and manage hypertension in busy clinics. However, repeated BP measurements have been shown to be more representative of the true BP status of the individual. Improper measurement of office BP can lead to inaccurate classification, overestimation of a patient’s true BP, unnecessary treatment, and misinterpretation of the true prevalence of hypertension. There is no consensus among major guidelines on the number of recommended measurements at a single visit or the method of arriving at final clinic BP reading. The participants of the National Family Health Survey (NFHS-4), a nationwide survey conducted in India from 2015 to 2016, were used for the analysis. The prevalence and median difference in systolic blood pressure (SBP) and diastolic blood pressure (DBP) for single as well as combinations of two or more readings were calculated. Cross-tabulation was used to assess classification of individuals based on first BP reading compared with the mean of two or more BP measurements. There was a 63% higher prevalence of hypertension when only the first reading was considered for diagnosis in comparison to the mean of the second and third readings. A decrease of 3.6 mmHg and 2.4 mm Hg in mean SBP and DBP, respectively, was observed when the mean of the second and third readings was compared to the first reading. In those who are identified to have grade 1 or higher categories of hypertension, we recommend three BP measurements, with the mean of the second and third measurements being the clinic BP.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Beevers G, Lip GY, O’Brien E. ABC of hypertension: blood pressure measurement. Part II-conventional sphygmomanometry: technique of auscultatory blood pressure measurement. BMJ . 2001;322:1043–7.
Handler J. The importance of accurate blood pressure measurement. Perm J. 2009;13:51–54.
Williams B, Mancia G, Spiering W, Agabiti Rosei E, Azizi M, Burnier M, et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension. Eur Heart J. 2018;39:3021–104.
Whelton PK, Carey RM, Aronow WS, Casey DE Jr, Collins KJ, Dennison Himmelfarb C, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: a report of the American College of Cardiology/American Heart Association Task Force on clinical practice guidelines. J Am Coll Cardiol 2018;71:e127–e248.
Michael WA, Ernesto SL, William WB, Samueld M, Lars LH, John KG, et al. Clinical practice guidelines for the management of hypertension in the community: a statement by the American Society of Hypertension and the International Society of Hypertension. J Hypertens. 2014;32:3–15. https://doi.org/10.1097/HJH.0000000000000065
IIPS. National Family Health Survey (NFHS-4) 2015–16. Mumbai, India: International Institute for Population Sciences, Mumbai, India and Macro International; 2017;1–637.
Einstadter D, Bolen SD, Misak JE, Bar-Shain DS, Cebul RD. Association of repeated measurements with blood pressure control in primary care. JAMA Intern Med. 2018;178:858–60. https://doi.org/10.1001/jamainternmed.2018.0315
Handler J, Zhao Y, Egan BM. Impact of the number of blood pressure measurements on blood pressure classification in US adults: NHANES 1999–2008. J Clin Hypertens. 2012;14:751–9. https://doi.org/10.1111/jch.12009. Epub 2012 Oct 22.
Centre for Chronic Disease Control. NCD Initiative Tripura. https://tripurancd.org/graph.html. Accessed February 11, 2019.
Geldsetzer P, Manne-Goehler J, Theilmann M, Davies JI, Awasthi A, Vollmer S, et al. Diabetes and hypertension in India: a nationally representative study of 1.3 million adults. JAMA Intern Med. 2018;178:363–72. https://doi.org/10.1001/jamainternmed.2017.8094
Funding
AA is supported by Department of Science and Technology, Government of India, New Delhi through INSPIRE Faculty program for some other work. No financial assistance was received in support of the study.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
AP, DP, and AR are associated with the Certificate Course in Management of Hypertension (CCMH) in various capacities. The CCMH program is implemented by the Public Health Foundation of India in collaboration with the Centre for Chronic Disease Control, International Society of Hypertension, and British Irish Hypertension Society, and is supported in part by Sun Pharmaceuticals Private Ltd. The authors declare no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Jose, A.P., Awasthi, A., Kondal, D. et al. Impact of repeated blood pressure measurement on blood pressure categorization in a population-based study from India. J Hum Hypertens 33, 594–601 (2019). https://doi.org/10.1038/s41371-019-0200-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41371-019-0200-4
This article is cited by
-
Mixed effects logistic regression analysis of blood pressure among Ghanaians and associated risk factors
Scientific Reports (2023)
-
Prevalence and subtypes of hypertension in normal-weight and obese Indian adolescents: a cross-sectional study
Journal of Human Hypertension (2022)
-
Spotlight on hypertension in the Indian subcontinent
Journal of Human Hypertension (2019)