Abstract
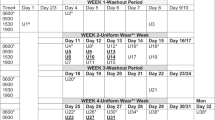
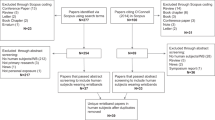
This study examined the effect of high-temperature conditions and uniform wear time durations (expeditionary, 33 h continuous wear; garrison, 3 days, 8 h/day wear) on permethrin exposure, assessed by urinary permethrin biomarkers, from wearing post-tailored, factory-treated military uniforms. Four group study sessions took place over separate 11-day periods, involving 33 male Soldiers. Group 1 (n = 10) and Group 2 (n = 8) participants wore a study-issued permethrin-treated Army uniform under high heat environment (35 °C, 40% relative humidity (rh)) and expeditionary and garrison wear-time conditions, respectively. For comparison, Group 3 (n = 7) and Group 4 (n = 8) participants wore study-issued permethrin-treated uniforms in cooler ambient conditions under operational and garrison wear-time conditions, respectively. Urinary biomarkers of permethrin (3-phenoxybenzoic acid, and the sum of cis- and trans-3-(2,2-dichlorovinyl)-2,2-dimethylcyclopropane-1-carboxylic acid) were significantly higher under high temperature compared to ambient conditions, regardless of wear-time situations (Group 1 vs. Group 3; Group 2 vs. Group 4; p < 0.001, for both). Under high-temperature conditions, expeditionary (continuous) compared to garrison wear-time resulted in significantly (p < 0.001) higher urinary biomarker concentrations (Group 1 vs. Group 2). Differences related to wear-time under the ambient conditions (Group 3 vs. Group 4) were not statistically significant. Findings suggest that wearing permethrin-treated clothing in heat conditions results in higher internal dose of permethrin above that observed under ambient conditions.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Armed Forces Pest Management Board (AFPMB). Technical guide no. 36. Personal protective measures against insects and other arthropods of military significance. 2015. https://www.acq.osd.mil/eie/afpmb/docs/techguides/tg36.pdf. Accessed 14 May 2018.
United States Army Public Health Center (USAPHC). DoD insect repellant system. 2018. https://phc.amedd.army.mil/topics/envirohealth/epm/Pages/DoD-Insect-Repellent-System.aspx. Accessed 14 May 2018.
United States Army Public Health Center (USAPHC). 2017 Health of the force report. 2018. https://phc.amedd.army.mil/Periodical%20Library/2017HealthoftheForceweb.pdf. Accessed 27 Mar 2018.
United States Environmental Protection Agency (EPA). Repellant-treated clothing. https://www.epa.gov/insect-repellents/repellent-treated-clothing. Accessed 14 May 2018.
Riederer AM, Bartell SM, Barr DB, Ryan PB. Diet and nondiet predictors of urinary 3-phenoxybenzoic acid in NHANES 1999–2002. Environ Health Perspect. 2008;116:1015–22.
Center for Disease Control and Prevention (CDC). Fourth national report on human exposure to environmental chemicals, updated tables, January 2017: vol. 1. 2017. https://www.cdc.gov/exposurereport/pdf/FourthReport_UpdatedTables_Volume1_Jan2017. pdf. Accessed 16 Feb 2018.
Barr DB, Olsson AO, Wong L, Udunka S, Baker SE, Whitehead RD, et al. Urinary concentrations of metabolites of pyrethroid insecticides in the general U.S. population: National Health and Nutrition Examination Survey 1999–2002. Environ Health Perspect. 2010;118:742–8.
Health Canada. Second report on human biomonitoring of environmental chemicals in Canada: Results of the Canadian Health Measures Survey Cycle 2 (2009–2011). 2013. https://www.canada.ca/content/dam/hc-sc/migration/hc-sc/ewh-semt/alt_formats/pdf/pubs/contaminants/chms-ecms-cycle2/chms-ecms-cycle2-eng.pdf. Accessed 16 Feb 2018.
Heudorf U, Angerer J. Metabolites of pyrethroid insecticides in urine specimens: current exposure in an urban population in Germany. Environ Health Perspect. 2001;109:213–7.
Trunnelle KJ, Bennett DH, Tulve NS, Clifton MS, Davis MD, Calafat AM, et al. Urinary pyrethroid and chlorpyrifos metabolite concentrations in Northern California families and their relationship to indoor residential insecticide levels, part of the Study of Use of Products and Exposure Related Behavior (SUPERB). Environ Sci Technol. 2014;48:1931–9.
Appel KE, Gundert-Remy U, Fischer H, Faulde M, Mross KG, Letzel S, et al. Risk assessment of Bundeswehr (German Federal Armed Forces) permethrin-impregnated battle dress uniforms (BDU). Int J Hyg Environ Health. 2008;211:88–104.
Kegel P, Letzel S, Rossbach B. Biomonitoring in wearers of permethrin impregnated battle dress uniforms in Afghanistan and Germany. Occup Environ Med. 2014;71:112–7.
Proctor SP, Maule AL, Heaton KJ, Adam GE. Permethrin exposure from fabric-treated military uniforms under difference wear-time scenarios. J Exp Sci Environ Epidemiol. 2014;24:572–8.
Proctor SP, Scarpaci MM, Maule AL, Heaton KJ, Taylor K, Dillon C, et al. Role of body composition and physical activity on permethrin urinary biomarker levels while wearing treated military uniforms. Toxicol Lett. 2018;299:210–7.
Rossbach B, Appel KE, Mross KG, Letzel S. Uptake of permethrin from impregnated clothing. Toxicol Lett. 2010;192:50–55.
Maule AL, Scarpaci MM, Proctor SP. Urinary concentrations of metabolites of permethrin in US Army personnel and US adult population: a review of occupational and population cohorts. Unpublished results; manuscript currently under review at journal.
Rossbach B, Niemietz A, Kegel P, Letzel S. Uptake and elimination of permethrin related to the use of permethrin treated clothing for forestry workers. Toxicol Lett. 2014;231:147–53.
FAO/WHO. Pesticide residues in food—1999. Report of the Joint Meeting of the FAO Panel of Experts on Pesticide Residues in Food and the Environment and the WHO Core Assessment Group. Geneva: World Health Organization; 1999.
Macedo PA, Peterson RKD, Davis RS. Risk assessments for exposure of deployed military personnel to insecticides and personal protective measures used for disease-vector management. J Toxicol Environ Health Part A. 2007;70:1758–71.
National Research Council. Health effects from permethrin-impregnated army battle dress uniforms. Washington, DC: National Academy Press; 1994.
United States Environmental Protection Agency (EPA). Permethrin. Reprot of the Cancer Assessment Review Committee (Third Evaluation). 2002. https://www3.epa.gov/pesticides/chem_search/cleared_reviews/csr_PC-109701_23-Oct-02_a.pdf. Accessed 15 May 2018.
United States Environmental Protection Agency (EPA). Reregistration Eligibility Decision (RED) for Permethrin. 2009. https://archive.epa.gov/pesticides/reregistration/web/pdf/permethrin-red-revised-may2009.pdf. Accessed 16 Feb 2018.
Vijverberg HP, van den Bercken J. Neurotoxicological effects and the mode of action of pyrethroid insecticides. Crit Rev Toxicol. 1990;21:105–26.
TBMED 507. Heat stress control and heat casualty management. In: Technical Bulletin Medical 507/air force pamphlet. Washington, DC: Department of the Army and Air Force; 2003. p. 5–10.
Gordon CJ. Role of environmental stress in the physiological response to chemical toxicants. Environ Res. 2003;92:1–7.
Doriot Climatic Chambers. 2009. http://doriot.natick.army.mil/. Accessed 30 Apr 2018.
Center for Disease Control and Prevention (CDC) Division of Nutrition, Physical Activity, and Obesity, National Center for Chronic Disease Prevention and Health Promotion. About BMI for Adults. 2017. http://www.cdc.gov/healthyweight/assessing/bmi/adult_bmi/index.html#Interpreted. Accessed 29 Apr 2018.
Baty International. The harpenden skinfold caliper HSB-BI. West Sussex, UK: Baty International Ltd.; 2010.
Heil DP. Predicting activity energy expenditure using the actical activity monitor. Res Q Exerc Sport. 2006;77:64–80.
Kazis LE, Wilson N, Skinner K, Lee A, Rogers W, Ren XS, et al. Health status and outcomes of veterans: physical and mental component summary scores (Veterans SF-12). 1998 National Survey of Hospitalized Patients. Executive Report. Washington, DC; Bedford, MA: Office of Performance and Quality, Health Assessment Project, Health Service Research and Development Service Field Program; 1999.
Proctor SP, Heeren T, White RF, Wolfe J, Borgos MS, Davis JD. Health status of Persian Gulf War veterans: self-reported symptoms, environmental exposures and the effect of stress. Int J Epidemiol. 1998;27:1000–10.
Proctor SP, Heaton KJ, Smith KW, Rodrigues ER, Widing DE, Herrick R, et al. The occupational JP8 exposure neruoepidemiology study (OJENES): repeated workday exposure and central nervous system functioning among US Air Force personnel. Neurotoxicology. 2011;32:799–808.
Stewart AL, Ware JE. Measuring functioning and well-being: the Medical Outcomes Study approach. Durham, NC: Duke University Press; 1992.
Matthews C, Klove K. Instruction manual for the adult neuropsychological test battery. Madison, WI: University of Wisconsin Medical Center; 1964.
Strauss E, Sherman EMS, Spreen O. A compendium of neuropyschological tests. 3rd ed. New York City, NY: Oxford University Press; 2006.
Kaminski TW, Groff RM, Glutting JJ. Examining the stability of Automated Neuropsychological Assessment Metric (ANAM) baseline test scores. J Clin Exp Neuropsychol. 2009;31:689–97.
Roebuck-Spencer TM, Reeves DL, Bleiberg J, Cernich AN, Schwab K, Ivins B, et al. Influence of demographics on computerized cognitive testing in a military sample. Mil Psychol. 2008;20:187–203.
Center for the Study of Human Operator Performance (C-SHOP). ANAM4: software user manual. Norman, OK: University of Oklahoma; 2007.
Vincent A, Bleiberg J, Yan S, Ivins B, Reeves DL, Schwab K, et al. Reference data from the Automated Neuropsychological Assessment Metrics for use in traumatic brain injury in an active duty military sample. Mil Med. 2008;173:836–52.
Vincent AS, Roebuck-Spencer T, Gilliland K, Schlegel R. Automated Neuropsychological Assessment Metrics (v4) Traumatic Brain Injury Battery: military normative data. Mil Med. 2012;177:256–69.
Davis MD, Wade EL, Restrepo PR, Roman-Esteva W, Bravo R, Kuklenyik P, et al. Semi-automated solid phase extraction method for the mass spectrometric quantification of 12 specific metabolites of organophosphorus pesticides, synthetic pyrethroids, and select herbicides in human urine. J Chromatogr B. 2013;929:18–26.
Hornung RW, Reed LD. Estimation of average concentration in the presence of nondetectable values. Appl Occup Environ Hyg. 1990;5:46–51.
Ix JH, Wassel CL, Stevens LA, Beck GJ, Froissart M, Navis G, et al. Equations to estimate creatinine excretion rate: the CKD Epidemiology Collaboration. Clin J Am Soc Nephrol. 2011;6:184–91.
Abou-Donia MB, Dechkovskaia AM, Goldstein LB, Abdel-Rahman A, Bullman SL, Khan WA. Co-exposure to pyridostygmine bromide, DEET, and/or permethrin causes sensorimotor deficit and alterations in brain acetylcholinesterase activity. Pharmacol Biochem Behav. 2004;77:253–62.
Riviere JE, Monteiro-Riviere NA, Baynes RE. Gulf War related exposure factors influencing topical absorption of 14C-permethrin. Toxicol Lett. 2002;135:61–71.
Acknowledgements
We acknowledge the contribution of additional USARIEM study team members who assisted in the data collection for this project and the laboratory technicians at the USARIEM Central Laboratory who performed sample analyses of creatinine. We also greatly appreciate the experience and input from Melynda Perry and Amy Johnson (Natick Textile Materials Evaluation Team, Natick Soldier Research, Development and Engineering Center, Natick, MA) who consulted on the project and conducted the permethrin analyses of the uniforms, respectively. We thank Mark Davis and Isuru Vidanage at the Centers for Disease Control and Prevention for technical assistance in the quantification of the pyrethroid metabolites in urine.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Proctor, S.P., Maule, A.L., Heaton, K.J. et al. Permethrin exposure from wearing fabric-treated military uniforms in high heat conditions under varying wear-time scenarios. J Expo Sci Environ Epidemiol 30, 525–536 (2020). https://doi.org/10.1038/s41370-019-0120-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41370-019-0120-y
Keywords
This article is cited by
-
Individual-level permethrin exposure biomarkers in U.S. army soldiers: comparison of two treatment formulations for military uniforms
Journal of Exposure Science & Environmental Epidemiology (2023)