Abstract
Introduction
Obesity is a growing public health problem leading to substantial economic impact. This study aimed to summarize the economic impact of obesity and to critically analyze the methods used in the cost-of-illness (COI) studies on obesity.
Methods
We conducted systematic search in PubMed and Scopus from September 1, 2016, to July 22, 2022. Original COI studies estimating the economic cost of obesity and/or overweight in at least one country, published in English were included. To facilitate the comparison of estimates across countries, we converted the cost estimates of different years to 2022 purchasing power parity (PPP) values using each country’s consumer price index (CPI) and PPP conversion rate.
Results
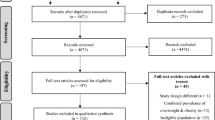
Nineteen studies were included. All studies employed a prevalence-based approach using Population Attributable Fraction (PAF) methodology. About half of the included studies (53%) were conducted in high-income countries while the others (47%) were conducted in middle-income countries. The economic burden of obesity ranged between PPP 15 million in Brazil to PPP 126 billion in the USA, in the year 2022. Direct medical costs accounted for 0.7% to 17.8% of the health system expenditure. Furthermore, the total costs of obesity ranged from 0.05% to 2.42% of the country’s gross domestic product (GDP). Of the seven studies that estimated both direct and indirect costs, indirect costs accounted for the largest portion of five studies. Nevertheless, a variety in methodology across studies was identified. The number of co-morbidities included in the analysis varied across studies.
Conclusions
Although there was a variety of methodologies across studies, consistent evidence indicated that the economic burden of obesity was substantial. Obesity prevention and control should be a public health priority, especially among countries with high prevalence of obesity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
The datasets generated and/or analyzed during the current study are available from the corresponding author upon reasonable request.
References
WHO. Obesity and overweight. Key facts. In, 2021.
Chu D-T, Minh Nguyet NT, Dinh TC, Thai Lien NV, Nguyen K-H, Nhu Ngoc VT, et al. An update on physical health and economic consequences of overweight and obesity. Diab Metab Syndr: Clin Res Rev. 2018;12:1095–1100.
Park A. Pathophysiology and aetiology and medical consequences of obesity. Medicine. 2019;47:169–74.
Bray GA, Kim KK, Wilding JPH. On behalf of the World Obesity F. Obesity: a chronic relapsing progressive disease process. A position statement of the World Obesity Federation. Obes Rev. 2017;18:715–23.
OECD. The heavy burden of obesity: the economics of prevention, OECD Health Policy Studies, OECD Publishing, Paris, OECD, 2019.
Jo C. Cost-of-illness studies: concepts, scopes, and methods. Clin Mol Hepatol. 2014;20:327–37.
Dobbs R, Sawers C, Thompson F, Manyika J, Woetzel JR, Child P, et al. Overcoming obesity: an initial economic analysis, McKinsey global institute, 2014.
Greenberg D, Mohamed Ibrahim MI, Boncz I. What Are the Challenges in Conducting Cost-of-Illness Studies? Value Health Reg Issues. 2014;4:115–6.
Onukwugha E, McRae J, Kravetz A, Varga S, Khairnar R, Mullins CD. Cost-of-Illness Studies: An Updated Review of Current Methods. Pharmaco Econ. 2016;34:43–58.
Dee A, Kearns K, O’Neill C, Sharp L, Staines A, O’Dwyer V, et al. The direct and indirect costs of both overweight and obesity: a systematic review. BMC Res Notes. 2014;7:242.
Goettler A, Grosse A, Sonntag D. Productivity loss due to overweight and obesity: a systematic review of indirect costs. BMJ Open. 2017;7:e014632.
Kent S, Fusco F, Gray A, Jebb SA, Cairns BJ, Mihaylova B. Body mass index and healthcare costs: a systematic literature review of individual participant data studies. Obes Rev: Official J Int Assoc Study Obes. 2017;18:869–79.
Specchia M, Veneziano M, Cadeddu C, Ferriero A, Mancuso A, Ianuale C, et al. Economic impact of adult obesity on health systems: A systematic review. Eur J Public Health. 2014;25:255–62.
Tremmel M, Gerdtham UG, Nilsson PM, Saha S. Economic Burden of Obesity: A Systematic Literature Review. Int J Environ Res Public Health. 2017;14:435.
Withrow D, Alter DA. The economic burden of obesity worldwide: a systematic review of the direct costs of obesity. Obes Rev: Official J Int Assoc Study Obes. 2011;12:131–41.
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71.
Ding D, Kolbe-Alexander T, Nguyen B, Katzmarzyk PT, Pratt M, Lawson KD. The economic burden of physical inactivity: a systematic review and critical appraisal. Br J Sports Med. 2017;51:1392–409.
Husereau D, Drummond M, Petrou S, Carswell C, Moher D, Greenberg D, et al. Consolidated Health Economic Evaluation Reporting Standards (CHEERS) statement. Value Health. 2013;16:e1–5.
International Monetary Fund (IMF). World Economic Outlook Database. In, 2022.
Oanda Corporation. Forex data services. Currency Converter. Foreign echange rates. In, 2023.
Aboulghate M, Elaghoury A, Elebrashy I, Elkafrawy N, Elshishiney G, Abul-Magd E, et al. The Burden of Obesity in Egypt. Front Public Health. 2021;9:718978.
Andersson E, Eliasson B, Steen, Carlsson K. Current and future costs of obesity in Sweden. Health policy (Amsterdam, Netherlands). 2022;126:558–64.
Boachie MK, Thsehla E, Immurana M, Kohli-Lynch C, Hofman KJ. Estimating the healthcare cost of overweight and obesity in South Africa. Global Health Action. 2022;15:2045092.
Coker T, Saxton J, Retat L, Alswat K, Alghnam S, Al-Raddadi RM, et al. The future health and economic burden of obesity-attributable type 2 diabetes and liver disease among the working-age population in Saudi Arabia. PloS one. 2022;17:e0271108.
Corrêa Ferreira da Silva R, Bahia LR, Machado da Rosa MQ, Malhão TA, Mendonça EP, Rosa RDS, et al. Costs of cancer attributable to excess body weight in the Brazilian public health system in 2018. PloS one. 2021;16:e0247983.
d’Errico M, Pavlova M, Spandonaro F. The economic burden of obesity in Italy: a cost-of-illness study. Eur J Health Econ: HEPAC: Health Econ Prevention Care. 2022;23:177–92.
Destri K, Alves J, Gregório MJ, Dias SS, Henriques AR, Mendonça N, et al. Obesity- attributable costs of absenteeism among working adults in Portugal. BMC Public Health. 2022;22:978.
Ferrari G, Giannichi B, Resende B, Paiva L, Rocha R, Falbel F, et al. The economic burden of overweight and obesity in Brazil: perspectives for the Brazilian Unified Health System. Public Health. 2022;207:82–87.
Gearon E, Backholer K, Lal A, Nusselder W, Peeters A. The case for action on socioeconomic differences in overweight and obesity among Australian adults: modelling the disease burden and healthcare costs. Australian New Zealand J Public Health. 2020;44:121–8.
Gil-Rojas Y, Garzón A, Hernández F, Pacheco B, González D, Campos J, et al. Burden of Disease Attributable to Obesity and Overweight in Colombia. Value Health Reg Issues. 2019;20:66–72.
Hoque ME, Molla AA, Hoque DM, Long KZ, Mamun AA. Health care cost of overweight-related diseases in Bangladesh. Public Health Nutr. 2020;23:2395–401.
Krueger H, Andres EN, Koot JM, Reilly BD. The economic burden of cancers attributable to tobacco smoking, excess weight, alcohol use, and physical inactivity in Canada. Curr Oncol (Toronto, Ont.). 2016;23:241–9.
Lee JE, Nam CM, Lee SG, Park S, Kim TH, Park EC. The economic burden of cancer attributable to obesity in Korea: A population-based cohort study. Eur J Cancer Care. 2019;28:e13084.
Lee JW, Choi YE, Kim DW, Lee S, Cho KH. Trends in socioeconomic costs of morbid obesity among Korean adults, 2009-13: Data from National Health Insurance Service. Obes Res Clin Practice. 2018;12:389–93.
Malkin JD, Baid D, Alsukait RF, Alghaith T, Alluhidan M, Alabdulkarim H, et al. The economic burden of overweight and obesity in Saudi Arabia. PloS one. 2022;17:e0264993.
Okunogbe A, Nugent R, Spencer G, Ralston J, Wilding J. Economic impacts of overweight and obesity: current and future estimates for eight countries. BMJ Glob Health. 2021;6:e006351.
Rezende LFM, Malhão TA, da Silva Barbosa R, Schilithz AOC, da Silva RCF, Moreira LGM, et al. The future costs of cancer attributable to excess body weight in Brazil, 2030-40. BMC Public Health. 2022;22:1236.
Riantoro BD, Kristina SA, Endarti D. Estimating Premature Mortality Cost of Cancers Attributable to Obesity in Indonesia. Asian Pacific J Cancer Prev: APJCP. 2019;20:87–90.
van den Broek-Altenburg E, Atherly A, Holladay E. Changes in healthcare spending attributable to obesity and overweight: payer- and service-specific estimates. BMC Public Health. 2022;22:962.
World Obesity Federation, World Obesity Atlas. In, 2023.
Danaei G, Robins JM, Young JG, Hu FB, Manson JE, Hernán MA. Weight Loss and Coronary Heart Disease: Sensitivity Analysis for Unmeasured Confounding by Undiagnosed Disease. Epidemiology. 2016;27:302–10.
Haase CL, Lopes S, Olsen AH, Satylganova A, Schnecke V, McEwan P. Weight loss and risk reduction of obesity-related outcomes in 0.5 million people: evidence from a UK primary care database. Int J Obes. 2021;45:1249–58.
Bray GA, Kim KK, Wilding JPH. Obesity: a chronic relapsing progressive disease process. A position statement of the World Obesity Federation. Obes Rev: Official J Int Assoc Study Obes. 2017;18:715–23.
Jastreboff AM, Kotz CM, Kahan S, Kelly AS, Heymsfield SB. Obesity as a Disease: The Obesity Society 2018 Position Statement. Obesity (Silver Spring, Md.). 2019;27:7–9.
Ciciurkaite G, Moloney ME, Brown RL. The Incomplete Medicalization of Obesity: Physician Office Visits, Diagnoses, and Treatments, 1996-2014. Public health reports (Washington, D.C. : 1974). 2019;134:141–9.
de Heer H, Kinslow B, Lane T, Tuckman R, Warren M. Only 1 in 10 Patients Told to Lose Weight Seek Help From a Health Professional: A Nationally Representative Sample. American journal of health promotion: AJHP. 2019;33:1049–52.
Tucker S, Bramante C, Conroy M, Fitch A, Gilden A, Wittleder S, et al. The Most Undertreated Chronic Disease: Addressing Obesity in Primary Care Settings. Current obesity reports. 2021;10:396–408.
Camilleri M, Malhi H, Acosta A. Gastrointestinal Complications of Obesity. Gastroenterology. 2017;152:1656–70.
Pugliese G, Liccardi A, Graziadio C, Barrea L, Muscogiuri G, Colao A. Obesity and infectious diseases: pathophysiology and epidemiology of a double pandemic condition. Int J Obes. 2022;46:449–65.
Sarwer DB, Polonsky HM. The Psychosocial Burden of Obesity. Endocrinol Metaboli Clin North America. 2016;45:677–88.
Ewing E. Weight bias and stigmatisation: what is it and what can we do about it? Br J Gen Prac:J Royal College of General Practitioners. 2019;69:349.
Singh K, Russell-Mayhew S, von Ranson K, McLaren L. Is there more to the equation? Weight bias and the costs of obesity. Canadian J Public Health. 2019;110:17–20.
Lobstein T, Brinsden H, Neveux M World Obesity Atlas 2022. In, 2022.
Brooks-Pollock E, Danon L. Defining the population attributable fraction for infectious diseases. Int J Epidemiol. 2017;46:976–82.
Greenland S. Concepts and pitfalls in measuring and interpreting attributable fractions, prevented fractions, and causation probabilities. Ann Epidemiol. 2015;25:155–61.
Lee IM, Shiroma EJ, Lobelo F, Puska P, Blair SN, Katzmarzyk PT, et al. Effect of physical inactivity on major non-communicable diseases worldwide: an analysis of burden of disease and life expectancy. Lancet. 2012;380:219–29.
Khosravi A, Mansournia MA. Methodological issues estimating population attributable fraction related to ‘Health care cost of overweight-related diseases in Bangladesh’. Public Health Nutr. 2021;24:4195–4195.
Khosravi A, Nielsen RO, Mansournia MA. Methods matter: population attributable fraction (PAF) in sport and exercise medicine. Br J Sports Med. 2020;54:1049.
Lin C-K, Chen S-T. Estimation and application of population attributable fraction in ecological studies. Environmental Health. 2019;18:52.
Poole C. A History of the Population Attributable Fraction and Related Measures. Ann Epidemiol. 2014;25:147–54.
Rezende L, Eluf-Neto J. Population attributable fraction: planning of diseases prevention actions in Brazil. Revista de Saúde Pública 2016;50:30.
Berger NA. Young Adult Cancer: Influence of the Obesity Pandemic. Obesity. 2018;26:641–50.
Acknowledgements
The authors would like to gratefully acknowledge Health Technology Assessment international (HTAi), Alberta- Canada and Mahidol University, Bangkok- Thailand. The findings, interpretations and conclusions expressed in this article do not necessarily reflect the views of the aforementioned agencies.
Author information
Authors and Affiliations
Contributions
All authors attest they meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship. All authors contributed to the study conception and design. Searching were performed by MAN. Study selection, quality assessment, and data extraction were performed by MAN, HA, and MAAR. All authors contributed to the data analysis and interpretation. The first draft of the manuscript was written by MAN. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
MAN, HA, MAAR, SS, MT, UC, and ZA declare that they have no relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript. This includes employment, consultancies, honoraria, stock ownership or options, expert testimony, grants or patents received or pending, or royalties.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nagi, M.A., Ahmed, H., Rezq, M.A.A. et al. Economic costs of obesity: a systematic review. Int J Obes 48, 33–43 (2024). https://doi.org/10.1038/s41366-023-01398-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-023-01398-y