Abstract
Background
There is a widespread notion that tobacco smoking controls weight based on the appetite suppressive effect of nicotine. However, the causal relationship between smoking initiation and obesity-related traits in the general population are unclear.
Methods
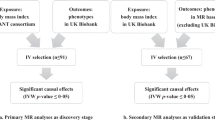
This Mendelian randomization analysis utilized 378 genetic variants associated with tobacco smoking initiation (usually in adolescence or young adulthood) identified in a genome-wide association study (meta-analysis) of 1.2 million individuals. Outcome data for body mass index, waist circumference, hip circumference, and waist-to-hip ratio were extracted from the 337,138 white British-ancestry UK Biobank participants aged 40–69 years. Replication analyses were performed for genome-wide association study meta-analysis for body mass index, including the GERA/GIANT data including 364,487 samples from mostly European individuals. In addition, summary-level Mendelian randomization by inverse variance weighted method and pleiotropy-robust Mendelian randomization methods, including median-based and MR–Egger regression, was performed.
Results
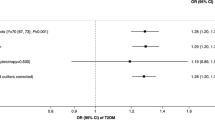
Summary-level Mendelian randomization analysis indicated that genetically predicted smoking initiation is causally linked to higher body mass index [+0.28 (0.18–0.38) kg/m2], waist circumference [+0.88 (0.66–1.10) cm], hip circumference [+0.40 (0.23–0.57) cm], and waist-to-hip ratio [+0.006 (0.005–0.007)]. These results were consistent with those of the pleiotropy-robust Mendelian randomization analysis. Additionally, in replication analysis, genetically predicted smoking initiation was significantly associated with a higher body mass index [+0.03 (0.01, 0.05] kg/m2).
Conclusion
Tobacco initiation may lead to worse obesity-related traits in the general 40- to 69-year-old individuals. Therefore, tobacco-use initiation as a long-term weight-control measure should be discouraged.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The data used for this study is available in the public database. The CKDGen data is openly available in the consortium website (URL: https://ckdgen.imbi.uni-freiburg.de/) and the UK Biobank data is accessible after acquiring approval from the organization (application No. 53799). The summary statistics for the GERA/GIANT meta-analysis is available in the GWAS catalog (https://www.ebi.ac.uk/gwas/studies/GCST006368). Dr. Dong Ki Kim and Dr. Sehoon Park had full access to all data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. The data for this study are available in the public domain, as described in the manuscript.
Code availability
The codes used for the statistical analyses in this study are available from each statistical package and the name of the packages are provided in the methods section.
References
Ghebreyesus TA. Progress in beating the tobacco epidemic. Lancet. 2019;394:548–9.
Chiolero A, Faeh D, Paccaud F, Cornuz J. Consequences of smoking for body weight, body fat distribution, and insulin resistance. Am J Clin Nutr. 2008;87:801–9.
Honjo K, Siegel M. Perceived importance of being thin and smoking initiation among young girls. Tob Control. 2003;12:289–95.
Amos A, Haglund M. From social taboo to “torch of freedom”: the marketing of cigarettes to women. Tob Control. 2000;9:3–8.
Chen H, Vlahos R, Bozinovski S, Jones J, Anderson GP, Morris MJ. Effect of short-term cigarette smoke exposure on body weight, appetite and brain neuropeptide Y in mice. Neuropsychopharmacology. 2005;30:713–9.
Bush T, Lovejoy JC, Deprey M, Carpenter KM. The effect of tobacco cessation on weight gain, obesity, and diabetes risk. Obesity (Silver Spring). 2016;24:1834–41.
Carreras-Torres R, Johansson M, Haycock PC, Relton CL, Davey Smith G, Brennan P, et al. Role of obesity in smoking behaviour: Mendelian randomisation study in UK Biobank. Bmj. 2018;361:k1767.
Davies NM, Holmes MV, Davey Smith G. Reading Mendelian randomisation studies: a guide, glossary, and checklist for clinicians. Bmj. 2018;362:k601.
Liu M, Jiang Y, Wedow R, Li Y, Brazel DM, Chen F, et al. Association studies of up to 1.2 million individuals yield new insights into the genetic etiology of tobacco and alcohol use. Nat Genet. 2019;51:237–44.
Bowden J, Davey Smith G, Burgess S. Mendelian randomization with invalid instruments: effect estimation and bias detection through Egger regression. Int J Epidemiol. 2015;44:512–25.
Buniello A, MacArthur JAL, Cerezo M, Harris LW, Hayhurst J, Malangone C, et al. The NHGRI-EBI GWAS Catalog of published genome-wide association studies, targeted arrays and summary statistics 2019. Nucleic Acids Res. 2019;47:D1005–d12.
Bowden J, Davey Smith G, Haycock PC, Burgess S. Consistent Estimation in Mendelian Randomization with Some Invalid Instruments Using a Weighted Median Estimator. Genet Epidemiol. 2016;40:304–14.
Hemani G, Tilling K, Davey Smith G. Orienting the causal relationship between imprecisely measured traits using GWAS summary data. PLoS Genet. 2017;13:e1007081.
Bycroft C, Freeman C, Petkova D, Band G, Elliott LT, Sharp K, et al. The UK Biobank resource with deep phenotyping and genomic data. Nature. 2018;562:203–9.
Sudlow C, Gallacher J, Allen N, Beral V, Burton P, Danesh J, et al. UK biobank: an open access resource for identifying the causes of a wide range of complex diseases of middle and old age. PLoS Med. 2015;12:e1001779.
Park S, Lee S, Kim Y, Lee Y, Kang MW, Kim K, et al. Atrial fibrillation and kidney function: a bidirectional Mendelian randomization study. Eur Heart J. 2021;42:2816–23.
Park S, Lee S, Kim Y, Cho S, Kim K, Kim YC, et al. Kidney function and obstructive lung disease: a bidirectional Mendelian randomisation study. Eur Respir J. 2021;58:2100848.
Chang CC, Chow CC, Tellier LC, Vattikuti S, Purcell SM, Lee JJ. Second-generation PLINK: rising to the challenge of larger and richer datasets. Gigascience. 2015;4:7.
Burgess S, Davies NM, Thompson SG. Bias due to participant overlap in two-sample Mendelian randomization. Genet Epidemiol. 2016;40:597–608.
Zhao W, Ware EB, He Z, Kardia SLR, Faul JD, Smith JA. Interaction between social/psychosocial factors and genetic variants on body mass index: a gene-environment interaction analysis in a longitudinal setting. Int J Environ Res Public Health. 2017;14:1153.
Kvale MN, Hesselson S, Hoffmann TJ, Cao Y, Chan D, Connell S, et al. Genotyping informatics and quality control for 100,000 subjects in the genetic epidemiology research on adult health and aging (GERA) cohort. Genetics. 2015;200:1051–60.
Locke AE, Kahali B, Berndt SI, Justice AE, Pers TH, Day FR, et al. Genetic studies of body mass index yield new insights for obesity biology. Nature. 2015;518:197–206.
Burgess S, Labrecque JA. Mendelian randomization with a binary exposure variable: interpretation and presentation of causal estimates. Eur J Epidemiol. 2018;33:947–52.
Hemani G, Zheng J, Elsworth B, Wade KH, Haberland V, Baird D, et al. The MR-Base platform supports systematic causal inference across the human phenome. Elife. 2018;7:e34408.
Dare S, Mackay DF, Pell JP. Relationship between smoking and obesity: a cross-sectional study of 499,504 middle-aged adults in the UK general population. PLoS One. 2015;10:e0123579.
Winsløw UC, Rode L, Nordestgaard BG. High tobacco consumption lowers body weight: a Mendelian randomization study of the Copenhagen General Population Study. Int J Epidemiol. 2015;44:540–50.
Dudbridge F. Commentary: Tobacco consumption and body weight: Mendelian randomization across a range of exposure. Int J Epidemiol. 2016;45:e1–e3.
Peacock A, Leung J, Larney S, Colledge S, Hickman M, Rehm J, et al. Global statistics on alcohol, tobacco and illicit drug use: 2017 status report. Addiction. 2018;113:1905–26.
Degens H, Gayan-Ramirez G, van Hees HW. Smoking-induced skeletal muscle dysfunction: from evidence to mechanisms. Am J Respir Crit Care Med. 2015;191:620–5.
Moslemi-Haghighi F, Rezaei I, Ghaffarinejad F, Lari R, Pouya F. Comparison of physical fitness among smoker and non-smoker men. Addict Health. 2011;3:15–9.
Wang J, Bai Y, Zeng Z, Wang J, Wang P, Zhao Y, et al. Association between life-course cigarette smoking and metabolic syndrome: a discovery-replication strategy. Diabetol Metab Syndr. 2022;14:11.
Yuan S, Larsson SC. A causal relationship between cigarette smoking and type 2 diabetes mellitus: A Mendelian randomization study. Sci Rep. 2019;9:19342.
Acknowledgements
The study was based on the data provided by the UK Biobank consortium (application No. 53799). We thank the investigators of the CKDGen, GERA, and GIANT consortium who provided the summary statistics for the outcome data of this study.
Funding
This research was supported by a grant of the Korea Health Technology R&D Project through the Korea Health Industry Development Institute (KHIDI), funded by the Ministry of Health & Welfare, Republic of Korea (grant number: HI23C1484). This work was supported by the National Research Foundation of Korea (NRF) grant funded by the Korea government (MSIT, Ministry of Science and ICT) (No. 2021R1A2C2094586). This research was supported by the research fund from Seoul National University (3020210020). The funder played no role in the performance of the study, and the study was performed independently by the authors.
Author information
Authors and Affiliations
Contributions
The corresponding author attests that all listed authors meet the authorship criteria and that no others meeting the criteria have been omitted. SP, HL, KSK, KWJ, and DKK contributed to the conception and design of the study. SL, SK, YK, YCK, SSH, JPL, KWJ, CSL, YSK, and DKK provided statistical advice and interpreted the data. SP and KSK performed the main statistical analysis, assisted by SK, SL, and YK. HL, JPL, KWJ, CSL, YSK, and DKK provided advice regarding the data interpretation. YCK, SSH, HL, JPL, KWJ, CSL, and YSK provided material support during the study. SP and DKK had full access to all data in the study and took responsibility for the integrity of the data and the accuracy of the data analysis. All authors participated in drafting the manuscript. All authors reviewed the manuscript and approved the final version to be published.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
This study was approved by the institutional review boards of Seoul National University Hospital (No. E-2203-053-1303) and the UK Biobank consortium (application No. 53799) [14, 15], and was performed in accordance with the Declaration of Helsinki. The requirement for informed consent was waived by the attending institutional review boards because anonymous public databases were used for collecting data for research purposes.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Park, S., Kim, S.G., Lee, S. et al. Causal effects from tobacco smoking initiation on obesity-related traits: a Mendelian randomization study. Int J Obes 47, 1232–1238 (2023). https://doi.org/10.1038/s41366-023-01371-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-023-01371-9