Abstract
Background/objectives
We aimed to evaluate the relationships between body fat percentage (BF%), fat mass (FM), fat mass index (FMI) and visceral (VAT) and subcutaneous adipose tissue (SAT) with risk of all-cause mortality.
Methods
We did a systematic search in PubMed, Scopus, and Web of Science to June 2021. We selected prospective cohorts of the relationship between body fat with risk of all-cause mortality in the general population. We applied random-effects models to calculate the relative risks (RRs) and 95%CIs.
Results
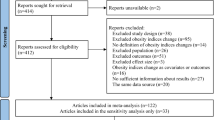
A total of 35 prospective cohort studies with 923,295 participants and 68,389 deaths were identified. The HRs of all-cause mortality for a 10% increment in BF were 1.11 (95%CI: 1.02, 1.20; I2 = 93%, n = 11) in the general adult populations, and 0.92 (95%CI: 0.79, 1.06; I2 = 76%, n = 7) in adults older than 60 years. The HRs were 1.06 (95%CI: 1.01, 1.12; I2 = 86%, n = 10) for a 5 kg increment in FM, 1.11 (95%CI: 1.06, 1.16; I2 = 79%, n = 7) for a 2 kg/m2 increment in FMI, and 1.17 (95%CI: 1.03, 1.33; I2 = 72%, n = 8) and 0.81 (0.66, 0.99; I2 = 59%, n = 6) for a 1-SD increment in VAT and SAT, respectively. There was a J shaped association between BF% and FM and all-cause mortality risk, with the lowest risk at BF% of 25% and FM of 20 kg. In subgroup analyses, although there was little evidence of between-subgroup heterogeneity, the observed positive associations were more pronounced in studies which had a longer duration, excluded participants with prevalent cardiovascular disease and cancer at baseline, with adjustment for smoking or restricted to never smokers, and less pronounced in studies which adjusted for potential intermediates, suggesting an impact of reverse causation, confounding and over-adjustment in some of the studies.
Conclusions
Higher body fat content was related to a higher risk of mortality in a J shaped manner. Any future studies should further assess the impact of reverse causation and residual confounding on these associations.
Registration
PROSPERO (CRD42021240743).
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The data and analytical codes used for the present review will be available upon request.
References
Aune D, Sen A, Prasad M, Norat T, Janszky I, Tonstad S et al. BMI and all cause mortality: systematic review and non-linear dose-response meta-analysis of 230 cohort studies with 3.74 million deaths among 30.3 million participants. BMJ. 2016;353.
Di Angelantonio E, Bhupathiraju SN, Wormser D, Gao P, Kaptoge S, De Gonzalez AB, et al. Body-mass index and all-cause mortality: individual-participant-data meta-analysis of 239 prospective studies in four continents. Lancet. 2016;388:776–86.
Jayedi A, Soltani S, Zargar MS, Khan TA, Shab-Bidar S. Central fatness and risk of all cause mortality: systematic review and dose-response meta-analysis of 72 prospective cohort studies. BMJ. 2020;370.
Després J-P. Body fat distribution and risk of cardiovascular disease: an update. Circulation. 2012;126:1301–13.
Nevill AM, Stewart AD, Olds T, Holder R. Relationship between adiposity and body size reveals limitations of BMI. Am J Phys Anthropol. 2006;129:151–6.
Shen W, Wang Z, Punyanita M, Lei J, Sinav A, Kral JG, et al. Adipose tissue quantification by imaging methods: a proposed classification. Obes Res. 2003;11:5–16.
Cheung A, De Rooy C, Hoermann R, Gianatti E, Hamilton E, Roff G, et al. Correlation of visceral adipose tissue measured by Lunar Prodigy dual X-ray absorptiometry with MRI and CT in older men. Int J Obes. 2016;40:1325–8.
Park Y, Heymsfield S, Gallagher D. Are dual-energy X-ray absorptiometry regional estimates associated with visceral adipose tissue mass? Int J Obes. 2002;26:978–83.
Schousboe JT, Langsetmo L, Schwartz AV, Taylor BC, Vo TN, Kats AM, et al. Comparison of associations of DXA and CT visceral adipose tissue measures with insulin resistance, lipid levels, and inflammatory markers. J Clin Densitom. 2017;20:256–64.
Houtkooper LB, Lohman TG, Going SB, Howell WH. Why bioelectrical impedance analysis should be used for estimating adiposity. Am J Clin Nutr. 1996;64:436S–48S.
Lee DH, Keum N, Hu FB, Orav EJ, Rimm EB, Sun Q, et al. Development and validation of anthropometric prediction equations for lean body mass, fat mass and percent fat in adults using the National Health and Nutrition Examination Survey (NHANES) 1999–2006. Br J Nutr. 2017;118:858–66.
Cornier M-A, Despres J-P, Davis N, Grossniklaus DA, Klein S, Lamarche B, et al. Assessing adiposity: a scientific statement from the American Heart Association. Circulation. 2011;124:1996–2019.
Matsuzawa Y, Shimomura I, Nakamura T, Keno Y, Kotani K, Tokunaga K. Pathophysiology and pathogenesis of visceral fat obesity. Obes Res. 1995;3:187s–94s.
Ibrahim MM. Subcutaneous and visceral adipose tissue: structural and functional differences. Obes Rev. 2010;11:11–18.
Hutley L, Prins JB. Fat as an endocrine organ: relationship to the metabolic syndrome. Am J Med Sci. 2005;330:280–9.
Chan DC, Barrett HP, Watts GF. Dyslipidemia in visceral obesity. Am J Cardiovasc Drugs. 2004;4:227–46.
Fontana L, Eagon JC, Trujillo ME, Scherer PE, Klein S. Visceral fat adipokine secretion is associated with systemic inflammation in obese humans. Diabetes. 2007;56:1010–3.
Frayn KN. Visceral fat and insulin resistance—causative or correlative? Br J Nutr. 2000;83:S71–7.
Rosenquist KJ, Massaro JM, Pedley A, Long MT, Kreger BE, Vasan RS, et al. Fat quality and incident cardiovascular disease, all-cause mortality, and cancer mortality. J Clin Endocrinol Metab. 2015;100:227–34.
Porter SA, Massaro JM, Hoffmann U, Vasan RS, O’Donnel CJ, Fox CS. Abdominal subcutaneous adipose tissue: a protective fat depot? Diabetes Care. 2009;32:1068–75.
McLaughlin T, Lamendola C, Liu A, Abbasi F. Preferential fat deposition in subcutaneous versus visceral depots is associated with insulin sensitivity. J Clin Endocrinol Metab. 2011;96:E1756–60.
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6:e1000097.
Britton KA, Massaro JM, Murabito JM, Kreger BE, Hoffmann U, Fox CS. Body fat distribution, incident cardiovascular disease, cancer, and all-cause mortality. J Am Coll Cardiol. 2013;62:921–5.
Chuang S-Y, Hsu Y-Y, Chen RC-Y, Liu W-L, Pan W-H. Abdominal obesity and low skeletal muscle mass jointly predict total mortality and cardiovascular mortality in an elderly Asian population. J Gerontol A Biomed Sci Med Sci. 2016;71:1049–55.
de Santana FM, Domiciano DS, Gonçalves MA, Machado LG, Figueiredo CP, Lopes JB, et al. Association of appendicular lean mass, and subcutaneous and visceral adipose tissue with mortality in older Brazilians: The São Paulo Ageing & Health Study. J Bone Miner Res. 2019;34:1264–74.
Han SS, Kim KW, Kim KI, Na KY, Chae DW, Kim S, et al. Lean mass index: a better predictor of mortality than body mass index in elderly Asians. J Am Geriatr Soc. 2010;58:312–7.
Padwal R, Majumdar SR, Leslie WD. Relationship among body fat percentage, body mass index, and all-cause mortality. Ann Intern Med. 2016;165:604.
Sanada K, Chen R, Willcox B, Ohara T, Wen A, Takenaka C, et al. Association of sarcopenic obesity predicted by anthropometric measurements and 24-y all-cause mortality in elderly men: The Kuakini Honolulu Heart Program. Nutrition. 2018;46:97–102.
Sedlmeier AM, Baumeister SE, Weber A, Fischer B, Thorand B, Ittermann T, et al. Relation of body fat mass and fat-free mass to total mortality: results from 7 prospective cohort studies. Am J Clin Nutr. 2021;113:639–46.
Spahillari A, Mukamal KJ, DeFilippi C, Kizer JR, Gottdiener JS, Djoussé L, et al. The association of lean and fat mass with all-cause mortality in older adults: The Cardiovascular Health Study. Nutr Metab Cardiovasc Dis. 2016;26:1039–47.
Wells GA, Shea B, O’Connell DA, Peterson J, Welch V, Losos M et al. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. In: Oxford, 2000.
Symons M, Moore D. Hazard rate ratio and prospective epidemiological studies. J Clin Epidemiol. 2002;55:893–9.
Jyväkorpi SK, Urtamo A, Kivimäki M, Salomaa V, Strandberg TE. Association of midlife body composition with old-age health-related quality of life, mortality, and reaching 90 years of age: a 32-year follow-up of a male cohort. Am J Clin Nutr. 2020;112:1287–94.
Kuk JL, Katzmarzyk PT, Nichaman MZ, Church TS, Blair SN, Ross R. Visceral fat is an independent predictor of all‐cause mortality in men. Obesity. 2006;14:336–41.
Zhang J, Kai FY. What’s the relative risk?: A method of correcting the odds ratio in cohort studies of common outcomes. Jama. 1998;280:1690–1.
Crippa A, Discacciati A, Bottai M, Spiegelman D, Orsini N. One-stage dose–response meta-analysis for aggregated data. Stat Methods Med Res. 2019;28:1579–96.
DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials. 1986;7:177–88.
Bigaard J, Frederiksen K, Tjønneland A, Thomsen BL, Overvad K, Heitmann BL, et al. Waist circumference and body composition in relation to all-cause mortality in middle-aged men and women. Int J Obes (Lond). 2005;29:778–84.
Howell CR, Mehta T, Ejima K. Body composition and mortality in Mexican American adults: results from the national health and nutrition examination survey. Obesity (Silver Spring). 2018;26:1372–80.
Lahmann PH, Lissner L, Gullberg B, Berglund G. A prospective study of adiposity and all‐cause mortality: the Malmö Diet and Cancer Study. Obes Res. 2002;10:361–9.
Myint PK, Kwok CS, Luben RN, Wareham NJ, Khaw K-T. Body fat percentage, body mass index and waist-to-hip ratio as predictors of mortality and cardiovascular disease. Heart. 2014;100:1613–9.
Romero-Corral A, Somers VK, Sierra-Johnson J, Korenfeld Y, Boarin S, Korinek J, et al. Normal weight obesity: a risk factor for cardiometabolic dysregulation and cardiovascular mortality. Eur Heart J. 2010;31:737–46.
Santanasto AJ, Goodpaster BH, Kritchevsky SB, Miljkovic I, Satterfield S, Schwartz AV, et al. Body composition remodeling and mortality: the health aging and body composition study. J Gerontol A Biol Sci Med Sci. 2017;72:513–9.
Simpson JA, MacInnis RJ, Peeters A, Hopper JL, Giles GG, English DR. A comparison of adiposity measures as predictors of all‐cause mortality: the Melbourne Collaborative Cohort Study. Obesity. 2007;15:994–1003.
Yu T, Bo Y, Chang L-Y, Liu X, Tam T, Lao XQ. Adiposity and risk of death: A prospective cohort study of 463,002 adults. Clin Nutr. 2020;40:1932–41.
Heitmann B, Erikson H, Ellsinger B, Mikkelsen K, Larsson B. Mortality associated with body fat, fat-free mass and body mass index among 60-year-old Swedish men—a 22-year follow-up. The study of men born in 1913. Int J Obes. 2000;24:33–7.
Shil Hong E, Khang AR, Roh E, Jeong Ku E, An Kim Y, Min Kim K, et al. Counterintuitive relationship between visceral fat and all‐cause mortality in an elderly A sian population. Obesity. 2015;23:220–7.
Sørensen TIA, Frederiksen P, Heitmann BL. Levels and changes in body mass index decomposed into fat and fat-free mass index: relation to long-term all-cause mortality in the general population. Int J Obes. 2020;44:2092–100.
Zong G, Zhang Z, Yang Q, Wu H, Hu FB, Sun Q. Total and regional adiposity measured by dual‐energy X‐ray absorptiometry and mortality in NHANES 1999‐2006. Obesity. 2016;24:2414–21.
Hamling J, Lee P, Weitkunat R, Ambühl M. Facilitating meta‐analyses by deriving relative effect and precision estimates for alternative comparisons from a set of estimates presented by exposure level or disease category. Stat Med. 2008;27:954–70.
Bagheri M, Speakman J, Shabbidar S, Kazemi F, Djafarian K. A dose‐response meta‐analysis of the impact of body mass index on stroke and all‐cause mortality in stroke patients: a paradox within a paradox. Obes Rev. 2015;16:416–23.
Jayedi A, Shab-Bidar S. Nonlinear dose–response association between body mass index and risk of all-cause and cardiovascular mortality in patients with hypertension: A meta-analysis. Obes Res Clin Pract. 2018;12:16–28.
Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ et al. Cochrane handbook for systematic reviews of interventions, John Wiley & Sons, 2019.
Egger M, Smith GD, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. BMJ. 1997;315:629–34.
Begg CB, Mazumdar M. Operating characteristics of a rank correlation test for publication bias. Biometrics. 1994;50:1088–101.
Bea JW, Thomson CA, Wertheim BC, Nicholas JS, Ernst KC, Hu C, et al. Risk of mortality according to body mass index and body composition among postmenopausal women. Am J Epidemiol. 2015;182:585–96.
Brown JC, Harhay MO, Harhay MN. Anthropometrically‐predicted visceral adipose tissue and mortality among men and women in the third national health and nutrition examination survey (NHANES III). Am J Human Biol. 2017;29:e22898.
Dolan CM, Kraemer H, Browner W, Ensrud K, Kelsey JL. Associations between body composition, anthropometry, and mortality in women aged 65 years and older. Am J Pub Health. 2007;97:913–8.
Gale CR, Martyn CN, Cooper C, Sayer AA. Grip strength, body composition, and mortality. Int J Epidemiol. 2007;36:228–35.
Genton L, Graf CE, Karsegard VL, Kyle UG, Pichard C. Low fat-free mass as a marker of mortality in community-dwelling healthy elderly subjects. Age Ageing. 2013;42:33–39.
Katzmarzyk P, Mire E, Bouchard C. Abdominal obesity and mortality: the Pennington Center longitudinal study. Nutr Diabetes. 2012;2:e42–e42.
Koster A, Murphy RA, Eiriksdottir G, Aspelund T, Sigurdsson S, Lang TF, et al. Fat distribution and mortality: the AGES‐Reykjavik Study. Obesity. 2015;23:893–7.
Lee CD, Blair SN, Jackson AS. Cardiorespiratory fitness, body composition, and all-cause and cardiovascular disease mortality in men. Am J Clin Nutr. 1999;69:373–80.
Lee DH, Keum N, Hu FB, Orav EJ, Rimm EB, Willett WC, et al. Predicted lean body mass, fat mass, and all cause and cause specific mortality in men: prospective US cohort study. BMJ. 2018;362:k2575.
McNeely MJ, Shofer JB, Leonetti DL, Fujimoto WY, Boyko EJ. Associations among visceral fat, all-cause mortality, and obesity-related mortality in Japanese Americans. Diabetes Care. 2012;35:296–8.
Oh H, Kwak S-Y, Jo G, Lee J, Park D, Lee DH, et al. Adiposity and mortality in Korean adults: a population-based prospective cohort study. Am J Clin Nutr. 2020;113:142–53.
Ortega FB, Sui X, Lavie CJ, Blair SN. Body Mass Index, the Most Widely Used But Also Widely Criticized Index: Would a Criterion Standard Measure of Total Body Fat Be a Better Predictor of Cardiovascular Disease Mortality? Mayo Clin Proc. 2016;91:443–55. https://doi.org/10.1016/j.mayocp.2016.01.008.
Wannamethee SG, Shaper AG, Lennon L, Whincup PH. Decreased muscle mass and increased central adiposity are independently related to mortality in older men. Am J Clin Nutr. 2007;86:1339–46.
Flegal KM, Ioannidis JP. The obesity paradox: a misleading term that should be abandoned. Obesity. 2018;26:629–30.
Bergman RN, Kim SP, Catalano KJ, Hsu IR, Chiu JD, Kabir M, et al. Why visceral fat is bad: mechanisms of the metabolic syndrome. Obesity. 2006;14:16S.
Pandžić Jakšić V, Grizelj D. Under the surface of subcutaneous adipose tissue biology. Acta Dermatovenerol Croat. 2016;24:250–250.
Bidulescu A, Liu J, Hickson DA, Hairston KG, Fox ER, Arnett DK, et al. Gender differences in the association of visceral and subcutaneous adiposity with adiponectin in African Americans: the Jackson Heart Study. BMC Cardiovasc Disord. 2013;13:1–10.
Fox C, Massaro J, Hoffmann U, Pou K, Maurovich-Horvat P, Liu C-Y. Abdominal visceral and subcutaneous adipose tissue compartments: association with metabolic risk factors in the Framingham Heart Study. Circulation. 2007;116:39–48.
Liu J, Fox CS, Hickson DA, May WD, Hairston KG, Carr JJ, et al. Impact of abdominal visceral and subcutaneous adipose tissue on cardiometabolic risk factors: the Jackson Heart Study. J Clin Endocrinol Metab. 2010;95:5419–26.
Oka R, Yagi K, Sakurai M, Nakamura K, Nagasawa S-y, Miyamoto S, et al. Impact of visceral adipose tissue and subcutaneous adipose tissue on insulin resistance in middle-aged Japanese. J Atheroscler Thromb. 2012;12294:814–22.
Böhm A, Heitmann B. The use of bioelectrical impedance analysis for body composition in epidemiological studies. Eur J Clin Nutr. 2013;67:S79–S85.
Jaffrin MY. Body composition determination by bioimpedance: an update. Curr Opin Clin Nutr Metab Care. 2009;12:482–6.
Ward LC. Bioelectrical impedance analysis for body composition assessment: reflections on accuracy, clinical utility, and standardisation. Eur J Clin Nutr. 2019;73:194–9.
Author information
Authors and Affiliations
Contributions
AJ contributed to the study conception, literature search, data extraction, data analysis, and manuscript drafting. AE contributed to the literature search, data extraction, and manuscript drafting. SSB contributed to study conception, data analysis, and manuscript drafting. TK contributed to the data analysis, provided STATA syntax for dose-response meta-analysis, and approving the final manuscript. DA critically revised the manuscript and contributed to the interpretation of the findings. All authors acknowledge full responsibility for the analyses and interpretation of the report. All authors have read and approved the final manuscript. SS-B is the guarantor. The corresponding author attests that all listed authors meet authorship criteria and that no others meeting the criteria have been omitted.
Corresponding author
Ethics declarations
Competing interests
AJ, DA, AE, and SSB: have no relevant financial or non-financial interests to disclose. Dr. Tauseef A Khan has received research support from the Canadian Institutes of Health Research (CIHR), the International Life Science Institute (ILSI), and National Honey Board, outside the submitted work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Jayedi, A., Khan, T.A., Aune, D. et al. Body fat and risk of all-cause mortality: a systematic review and dose-response meta-analysis of prospective cohort studies. Int J Obes 46, 1573–1581 (2022). https://doi.org/10.1038/s41366-022-01165-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-022-01165-5