Abstract
Background
Although sarcopenic obesity is associated with a higher risk of cardiovascular events compared with obesity without sarcopenia, it is difficult to diagnose sarcopenia in daily clinical settings. Recently, a simple scoring system has been developed to identify sarcopenia patients based on three variables (age, hand grip strength, and calf circumference). However, the utility of this score for cardiovascular risk stratification in patients with abdominal obesity is unknown.
Methods
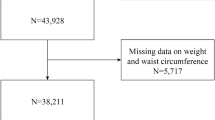
We calculated the sarcopenia score in 262 patients with abdominal obesity, defined as a waist circumference ≥90 cm in women or ≥85 cm in men. The composite endpoint of this study was cardiovascular mortality, nonfatal myocardial infarction, stroke, unstable angina, and heart failure hospitalization.
Results
Of the 262 patients, 108 had a high sarcopenia score based on previously established criteria (≥105 in men and ≥120 in women). The patients with a high sarcopenia score had a significantly higher plasma level of B-type natriuretic peptide compared with those with a low sarcopenia score (median 56.7, interquartile range [28.2–142.9] vs. 37.9 [13.8–76.1] pg/mL; p < 0.0001). Kaplan–Meier curves revealed a significantly lower event-free survival rate in those with a high compared with a low sarcopenia score (log-rank test p = 0.001), even after adjustment for confounding factors using propensity score matching (log-rank test p = 0.009). Multivariate Cox proportional hazard analysis identified a high sarcopenia score (hazard ratio: 2.46; 95% confidence interval: 1.31–4.64, p = 0.005) as an independent predictor of the primary endpoints. The combination of a high sarcopenia score and low body mass index (<25 kg/m2) predicted a significantly higher risk of future adverse events (p = 0.005). Furthermore, patients with a high sarcopenia score and high B-type natriuretic peptide level (≥200 pg/mL) had the poorest prognosis (p < 0.0001).
Conclusions
This simple screening test for sarcopenia can predict future adverse cardiovascular events in patients with abdominal obesity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Prospective Studies C, Whitlock G, Lewington S, Sherliker P, Clarke R, Emberson J. et al. Body-mass index and cause-specific mortality in 900 000 adults: collaborative analyses of 57 prospective studies. Lancet. 2009;373:1083–96.
Jensen MD, Ryan DH, Apovian CM, Ard JD, Comuzzie AG, Donato KA. et al. AHA/ACC/TOS guideline for the management of overweight and obesity in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. Circulation. 2014;129:S102–38.
Romero-Corral A, Montori VM, Somers VK, Korinek J, Thomas RJ, Allison TG, et al. Association of bodyweight with total mortality and with cardiovascular events in coronary artery disease: a systematic review of cohort studies. Lancet. 2006;368:666–78.
Curtis JP, Selter JG, Wang Y, Rathore SS, Jovin IS, Jadbabaie F, et al. The obesity paradox: body mass index and outcomes in patients with heart failure. Arch Intern Med. 2005;165:55–61.
Neeland IJ, Poirier P, Després JP. Cardiovascular and Metabolic Heterogeneity of Obesity: Clinical Challenges and Implications for Management. Circulation.2018;137:1391–406.
Boggs DA, Rosenberg L, Cozier YC, Wise LA, Coogan PF, Ruiz-Narvaez EA, et al. General and abdominal obesity and risk of death among black women. N Engl J Med. 2011;365:901–8.
Kanaya AM, Vittinghoff E, Shlipak MG, Resnick HE, Visser M, Grady D, et al. Association of total and central obesity with mortality in postmenopausal women with coronary heart disease. Am J Epidemiol. 2003;158:1161–70.
Delmonico MJ, Harris TB, Lee JS, Visser M, Nevitt M, Kritchevsky SB, et al. Alternative definitions of sarcopenia, lower extremity performance, and functional impairment with aging in older men and women. J Am Geriatr Soc. 2007;55:769–74.
Iannuzzi-Sucich M, Prestwood KM, Kenny AM. Prevalence of sarcopenia and predictors of skeletal muscle mass in healthy, older men and women. J Gerontol A Biol Sci Med Sci. 2002;57:M772–77.
Cruz-Jentoft AJ, Baeyens JP, Bauer JM, Boirie Y, Cederholm T, Landi F, et al. Sarcopenia: European consensus on definition and diagnosis: report of the European Working Group on Sarcopenia in Older People. Age Ageing. 2010;39:412–23.
Arango-Lopera VE, Arroyo P, Gutiérrez-Robledo LM, Pérez-Zepeda MU, Cesari M. Mortality as an adverse outcome of sarcopenia. J Nutr Health Aging. 2013;17:259–62.
Myint PK, Welch AA. Healthier ageing. BMJ. 2012;344:e1214.
Atkins JL, Whincup PH, Morris RW, Lennon LT, Papacosta O, Wannamethee SG. Sarcopenic obesity and risk of cardiovascular disease and mortality: a population-based cohort study of older men. J Am Geriatr Soc. 2014;62:253–60.
Chen LK, Liu LK, Woo J, Assantachai P, Auyeung TW, Bahyah KS, et al. Sarcopenia in Asia: consensus report of the Asian Working Group for Sarcopenia. J Am Med Dir Assoc. 2014;15:95–101.
Ishii S, Tanaka T, Shibasaki K, Ouchi Y, Kikutani T, Higashiguchi T, et al. Development of a simple screening test for sarcopenia in older adults. Geriatr Gerontol Int. 2014;14:93–101.
Onoue Y, Izumiya Y, Hanatani S, Tanaka T, Yamamura S, Kimura Y, et al. A simple sarcopenia screening test predicts future adverse events in patients with heart failure. Int J Cardiol. 2016;215:301–6.
Hanatani S, Izumiya Y, Onoue Y, Tanaka T, Yamamoto M, Ishida T, et al. Non-invasive testing for sarcopenia predicts future cardiovascular events in patients with chronic kidney disease. Int J Cardiol. 2018;268:216–21.
Nakao YM, Miyamoto Y, Ueshima K, Nakao K, Nakai M, Nishimura K, et al. Effectiveness of nationwide screening and lifestyle intervention for abdominal obesity and cardiometabolic risks in Japan: the metabolic syndrome and comprehensive lifestyle intervention study on nationwide database in Japan (MetS ACTION-J study). PLoS ONE. 2018;13:e0190862.
Matsuo S, Imai E, Horio M, Yasuda Y, Tomita K, Nitta K, et al. Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis. 2009;53:982–92.
Yu CM, Sanderson JE, Marwick TH, Oh JK. Tissue Doppler imaging a new prognosticator for cardiovascular diseases. J Am Coll Cardiol. 2007;49:1903–14.
Ouchi N, Oshima Y, Ohashi K, Higuchi A, Ikegami C, Izumiya Y, et al. Follistatin-like 1, a secreted muscle protein, promotes endothelial cell function and revascularization in ischemic tissue through a nitric-oxide synthase-dependent mechanism. J Biol Chem. 2008;283:32802–11.
Izumiya Y, Bina HA, Ouchi N, Akasaki Y, Kharitonenkov A, Walsh K. FGF21 is an Akt-regulated myokine. FEBS Lett. 2008;582:3805–10.
Walsh K. Adipokines, myokines and cardiovascular disease. Circ J. 2009;73:13–8.
Trayhurn P, Beattie JH. Physiological role of adipose tissue: white adipose tissue as an endocrine and secretory organ. Proc Nutr Soc. 2001;60:329–39.
Arita Y, Kihara S, Ouchi N, Takahashi M, Maeda K, Miyagawa J, et al. Paradoxical decrease of an adipose-specific protein, adiponectin, in obesity. Biochem Biophys Res Commun. 1999;257:79–83.
Araki S, Izumiya Y, Hanatani S, Rokutanda T, Usuku H, Akasaki Y, et al. Akt1-mediated skeletal muscle growth attenuates cardiac dysfunction and remodeling after experimental myocardial infarction. Circ Heart Fail. 2012;5:116–25.
Hanatani S, Izumiya Y, Araki S, Rokutanda T, Kimura Y, Walsh K, et al. Akt1-mediated fast/glycolytic skeletal muscle growth attenuates renal damage in experimental kidney disease. J Am Soc Nephrol. 2014;25:2800–11.
Kopelman PG. Obesity as a medical problem. Nature. 2000;404:635–43.
Bray GA, Heisel WE, Afshin A, Jensen MD, Dietz WH, Long M, et al. The science of obesity management: an Endocrine Society scientific statement. Endocr Rev. 2018;39:79–132.
Neeland IJ, Poirier P, Després JP. Cardiovascular and metabolic heterogeneity of obesity: clinical challenges and implications for management. Circulation. 2018;137:1391–406.
Fan H, Li X, Zheng L, Chen X, Lan Q, Wu H, et al. Abdominal obesity is strongly associated with cardiovascular disease and its risk factors in elderly and very elderly community-dwelling Chinese. Sci Rep. 2016;6:21521.
Sahakyan KR, Somers VK, Rodriguez-Escudero JP, Hodge DO, Carter RE, Sochor O, et al. Normal-weight central obesity: Implications for total and cardiovascular mortality. Ann Intern Med. 2015;163:827–35.
Acknowledgements
This study was supported in part by a Grant-in-Aid for Young Scientists B (16K19412) to SH and a Grant-in-Aid for Scientific Research C (18K08110) to KT from the Ministry of Education, Science, and Culture.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hanatani, S., Izumiya, Y., Yamamoto, M. et al. A simple method of sarcopenia detection can predict adverse cardiovascular events in patients with abdominal obesity. Int J Obes 45, 2214–2220 (2021). https://doi.org/10.1038/s41366-021-00895-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-021-00895-2
This article is cited by
-
Calf Circumference and All-Cause Mortality: A Systematic Review and Meta-Analysis Based on Trend Estimation Approaches
The Journal of nutrition, health and aging (2022)