Abstract
Background
Estimating energy requirements forms an integral part of developing diet and activity interventions. Current estimates often rely on a product of physical activity level (PAL) and a resting metabolic rate (RMR) prediction. PAL estimates, however, typically depend on subjective self-reported activity or a clinician’s best guess. Energy-requirement models that do not depend on an input of PAL may provide an attractive alternative.
Methods
Total daily energy expenditure (TEE) measured by doubly labeled water (DLW) and a metabolic chamber from 119 subjects obtained from a database of pre-intervention measurements measured at Pennington Biomedical Research Center were used to develop a metabolic ward and free-living models that predict energy requirements. Graded models, including different combinations of input variables consisting of age, height, weight, waist circumference, body composition, and the resting metabolic rate were developed. The newly developed models were validated and compared to three independent databases.
Results
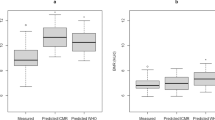
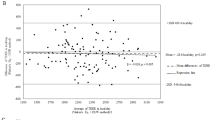
Sixty-four different linear and nonlinear regression models were developed. The adjusted R2 for models predicting free-living energy requirements ranged from 0.65 with covariates of age, height, and weight to 0.74 in models that included body composition and RMR. Independent validation R2 between actual and predicted TEE varied greatly across studies and between genders with higher coefficients of determination, lower bias, slopes closer to 1, and intercepts closer to zero, associated with inclusion of body composition and RMR covariates. The models were programmed into a user-friendly web-based app available at: http://www.pbrc.edu/research-and-faculty/calculators/energy-requirements/ (Video Demo for Reviewers at: https://www.youtube.com/watch?v=5UKjJeQdODQ)
Conclusions
Energy-requirement equations that do not require knowledge of activity levels and include all available input variables can provide more accurate baseline estimates. The models are clinically accessible through the web-based application.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Reeves MM, Capra S. Predicting energy requirements in the clinical setting: are current methods evidence based? Nutr Rev. 2003;61:143–51.
Tharion WJ, Lieberman HR, Montain SJ, et al. Energy requirements of military personnel. Appetite. 2005;44:47–65.
Schoeller DA, van Santen E. Measurement of energy expenditure in humans by doubly labeled water method. J Appl Physiol Respir Environ Exerc Physiol. 1982;53:955–9.
Green AJ, Smith P, Whelan K. Estimating resting energy expenditure in patients requiring nutritional support: a survey of dietetic practice. Eur J Clin Nutr. 2008;62:150–3.
Judges D, Knight A, Graham E, Goff LM. Estimating energy requirements in hospitalised underweight and obese patients requiring nutritional support: a survey of dietetic practice in the United Kingdom. Eur J Clin Nutr. 2012;66:394–8.
Harris JA, Benedict FG. A biometric study of human basal metabolism. Proc Natl Acad Sci USA. 1918;4:370–3.
Mifflin MD, St Jeor ST, Hill LA, Scott BJ, Daugherty SA, Koh YO. A new predictive equation for resting energy expenditure in healthy individuals. Am J Clin Nutr. 1990;51:241–7.
Westerterp KR. Doubly labelled water assessment of energy expenditure: principle, practice, and promise. Eur J Appl Physiol. 2017;117:1277–85.
FAO/ WHO/UNU Expert Consultation. Human energy requirements: report of a joint FAO/ WHO/UNU expert consultation. Food Nutr Bull. 2005;26:166
Troiano RP, Berrigan D, Dodd KW, Masse LC, Tilert T, McDowell M. Physical activity in the United States measured by accelerometer. Med Sci Sports Exerc. 2008;40:181–8.
Livingston EH, Kohlstadt I. Simplified resting metabolic rate-predicting formulas for normal-sized and obese individuals. Obes Res. 2005;13:1255–62.
Goran MI. Estimating energy requirements: regression based prediction equations or multiples of resting metabolic rate. Public Health Nutr. 2005;8:1184–6.
Vinken AG, Bathalon GP, Sawaya AL, Dallal GE, Tucker KL, Roberts SB. Equations for predicting the energy requirements of healthy adults aged 18-81y. Am J Clin Nutr. 1999;69:920–6.
Heo M, Faith MS, Pietrobelli A, Heymsfield SB. Percentage of body fat cutoffs by sex, age, and race-ethnicity in the US adult population from NHANES 1999-2004. Am J Clin Nutr. 2012;95:594–602.
Stevens J, Ou FS, Cai J, Heymsfield SB, Truesdale KP. Prediction of percent body fat measurements in Americans 8 years and older. Int J Obes (Lond). 2016;40:587–94.
Cunningham JJ. Body composition as a determinant of energy expenditure: a synthetic review and a proposed general prediction equation. Am J Clin Nutr. 1991;54:963–9.
Institute of Medicine (U.S.). Panel on Macronutrients., Institute of Medicine (U.S.). Standing Committee on the Scientific Evaluation of Dietary Reference Intakes. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty acids, Cholesterol, Protein, and Amino acids. Washington, DC: National Academies Press; 2005.
Levine JA, Eberhardt NL, Jensen MD. Role of nonexercise activity thermogenesis in resistance to fat gain in humans. Science. 1999;283:212–4.
Hand GA, Shook RP, Paluch AE, et al. The Energy Balance Study: the design and baseline results for a longitudinal study of energy balance. Res Q Exerc Sport. 2013;84:1–12.
Roberts SB, Dietz W, Sharp T, Dallal GE, Hill JO. Multiple laboratory comparison of the doubly labeled water technique. Obes Res. 1995;3(Suppl 1):3–13.
Van Der Ploeg GE, Withers RT, Laforgia J. Percent body fat via DEXA: comparison with a four-compartment model. J Appl Physiol (1985). 2003;94:499–506.
Trabulsi J, Troiano RP, Subar AF, et al. Precision of the doubly labeled water method in a large-scale application: evaluation of a streamlined-dosing protocol in the Observing Protein and Energy Nutrition (OPEN) study. Eur J Clin Nutr. 2003;57:1370–7.
DeGregory KW, Kuiper P, DeSilvio T, et al. A review of machine learning in obesity. Obes Rev. 2018;19:668–85.
Sabounchi NS, Rahmandad H, Ammerman A. Best-fitting prediction equations for basal metabolic rate: informing obesity interventions in diverse populations. Int J Obes (Lond). 2013;37:1364–70.
Murakami H, Kawakami R, Nakae S, et al. Accuracy of wearable devices for estimating total energy expenditure: comparison with metabolic chamber and doubly labeled water method. JAMA Intern Med. 2016;176:702–3.
Evenson KR, Goto MM, Furberg RD. Systematic review of the validity and reliability of consumer-wearable activity trackers. Int J Behav Nutr Phys Act. 2015;12:159.
Plasqui G, Westerterp KR. Physical activity assessment with accelerometers: an evaluation against doubly labeled water. Obes (Silver Spring). 2007;15:2371–9.
Plasqui G, Bonomi AG, Westerterp KR. Daily physical activity assessment with accelerometers: new insights and validation studies. Obes Rev. 2013;14:451–62.
Westreich D, Lessler J, Funk MJ. Propensity score estimation: neural networks, support vector machines, decision trees (CART), and meta-classifiers as alternatives to logistic regression. J Clin Epidemiol. 2010;63:826–33.
Heymsfield SB, Pietrobelli A. Body size and human energy requirements: reduced mass-specific total energy expenditure in tall adults. Am J Hum Biol. 2010;22:301–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Plucker, A., Thomas, D.M., Broskey, N. et al. Adult energy requirements predicted from doubly labeled water. Int J Obes 42, 1515–1523 (2018). https://doi.org/10.1038/s41366-018-0168-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-018-0168-0
This article is cited by
-
Predicting energy intake in adults who are dieting and exercising
International Journal of Obesity (2022)
-
Estimating total daily energy requirements in community-dwelling older adults: validity of previous predictive equations and modeling of a new approach
European Journal of Clinical Nutrition (2021)
-
A new doubly labelled water anthropometry-based equation for prediction of total daily energy expenditure in older people from low- and middle-income countries
European Journal of Clinical Nutrition (2021)