Abstract
Cytochrome c oxidase (COX) deficiency has been associated with a variety of clinical conditions and can be due to mutations in nuclear or mitochondrial genes. Despite recent progress in our understanding of the molecular bases of COX deficiency, the genetic defect remains elusive in many cases. We performed mutation screening in 30 patients with biochemical evidence of isolated COX deficiency and heterogeneous clinical phenotypes. Sixteen patients had various forms of encephalomyopathy, and six of these had the neuroradiological features of Leigh syndrome. Four patients had encephalohepatopathy, six had hypertrophic cardiomyopathy, and four had other phenotypes. We studied the three mtDNA genes encoding COX subunits, the 22 mtDNA tRNA genes, and seven COX assembly genes: SCO1, SCO2, SURF1, COX10, COX11, COX15, and COX17. We report two novel pathogenic SURF1 mutations in a patient with Leigh syndrome and one novel SCO2 mutation in a patient with hypertrophic cardiomyopathy. These data show that heterogeneous clinical phenotypes are associated with COX deficiency, that mutations in mtDNA COX genes are rare, and that mutations in additional genes remain to be identified.
Similar content being viewed by others
Main
Cytochrome c oxidase (COX), complex IV of the mitochondrial respiratory chain (EC 1.9.3.1), catalyzes the transfer of reducing equivalents from cytochrome c to molecular oxygen and utilizes the energy generated by this reaction to pump protons across the mitochondrial inner membrane. COX, active as a dimer, comprises 13 subunits, two heme groups (a and a3), three copper ions (two in the CuA site and one in CuB site), a zinc ion, and a magnesium ion (1). The biogenesis of COX requires the interplay of two genomes. Mitochondrial DNA (mtDNA) encodes the three larger subunits (COX I, COX II, and COX III) that compose the catalytic core of the enzyme and contain the prosthetic groups. Nuclear DNA (nDNA) encodes the 10 smaller COX subunits, which have regulatory and structural functions, and several accessory proteins, which control the folding and maturation of the different polypeptides, and the delivery and insertion of the prosthetic groups into the holoenzyme. In theory, COX deficiency may result from mutations in structural subunits of the enzyme or in ancillary proteins required for its assembly (2).
To date, pathogenic mutations have been described in the three mtDNA genes and in four COX assembly genes, SCO1 (3), SCO2 (4), COX10 (5), and SURF1 (6, 7). These result in a variety of clinical phenotypes. However, in some patients with isolated COX deficiency, the molecular defects remain elusive.
In a series of 30 patients with COX deficiency and unknown molecular causes, we screened for mutations in the three mtDNA COX genes, the 22 mtDNA tRNA genes, the four nDNA COXassembly genes already associated with disease in humans (SURF1, SCO1, SCO2, and COX10), and three candidate COX-assembly genes (COX11, COX15, and COX17). The yield was meager: one patient had two novel mutations in SURF1, and one had a novel mutation in SCO2 associated with the common E140 K mutation.
METHODS
We studied 30 patients with isolated COX deficiency [COX activity in muscle (referred to citrate synthase) below 33% of the normal mean; other respiratory chain enzyme activities within normal ranges]. Table 1 lists clinical and biochemical features. It should be noted that four patients with typical Leigh syndrome (LS) had already been screened for SURF1 and SCO2 mutations and found negative by Sue et al. (8). They were included in this study to be screened for other gene defects. Biopsies were obtained with the informed consent of parents or guardians, and all studies were approved by the Institutional Review Board of Columbia University College of Physicians & Surgeons.
Biochemical analysis.
Measurements of respiratory chain enzymes activities were performed in skeletal muscle as described (9). COX activity was measured in liver in one patient and in heart in two patients.
Histochemical analysis.
Muscle biopsies were stained for COX and succinate dehydrogenase as described (10).
DNA analysis.
DNA was extracted from tissues according to standard protocols (11).
The entire coding region of SCO1, SCO2, COX10, COX11, COX15, and COX17 was amplified as summarized in Table 2. SURF1 (7); mtDNA tRNA genes (12); and COXI, COXII, and COX III were amplified as described (13).
Mutation screening was performed by direct sequencing of SURF1, SCO2, COX I, COX II, COX III, and mtDNA tRNA genes, using the ABI PRISM Dye Terminator Cycle Sequencing Ready Reaction Kit and 310 Automatic Sequencer (Applied Biosystem, Perkin Elmer, Foster City, CA, U.S.A.). The remaining genes were studied by single strand conformational polymorphism (SSCP) analysis.
SSCP analysis.
A total of 100 ng of genomic DNA was amplified as described in Table 2. Reactions were carried out in 25 μL of 10 mM Tris-HCl (pH 8.9); 1.5 mM MgCl2; 0.4 mM each forward and reverse oligonucleotides; 0.2 mM each dATP, dGTP, and dTTP; 0.02 mM dCTP and 1 μCi of α32P dCTP; and 1.25 units of TAQ DNA polymerase (Roche, Basel, Switzerland). Samples were denatured and separated on a 6% MDE polyacrylamide (BME, Rockland, ME, U.S.A.), with 5% glycerol, according to the manufacturer's protocol. Singlestranded conformers were visualized by autoradiography using BIOMAX film (Kodak, Rochester, NY, U.S.A.). Samples with abnormal patterns were sequenced as above.
Analysis of insertions/deletions.
Exons harboring heterozygous insertions or deletions were amplified, and PCR products were subcloned in a pCRIITOPO Vector using a Topo TA Cloning kit (Invitrogen, Carlsbad, CA, U.S.A.) according to the manufacturer's protocol. Plasmid DNA was extracted using a Plasmid Mini Kit (Qiagen Inc., Valencia, CA, U.S.A.) and sequenced using M13R and M13-40 primers. Hydropathy plots were calculated with the Kyte-Doolittle algorithm using DNA Strider 1.2 software (CEA, Gif-Sur-Yvette, Cedax, France).
RESULTS
We studied 30 unrelated patients with isolated COX deficiency. COX activity in affected tissues ranged from 3% to 30% of control samples. Other respiratory chain enzyme activities were normal. The biochemical finding of COX deficiency was confirmed by histochemical analysis. None of the patients had evidence of ragged-red fibers on muscle biopsy.
All of our patients had onset of disease in early childhood and clusters of clinical symptoms suggestive of mitochondrial disorder (Table 1). They can be divided into six groups on the basis of the clinical phenotype. Group 1 patients (1–6) had clinical and neuroradiological features of LS; group 2 patients (7–16) had encephalomyopathy but lacked the neuroradiological features of LS. Group 3 patients (17, 18) had encephalopathy, myoclonus, and optic atrophy. Group 4 patients (19–22) had hepatoencephalopathy as the main clinical feature. Group 5 patients (23–28) had hypertrophic cardiomyopathy. Group 6 patients (29 and 30) had clinical pictures not classifiable within any of the previous groups. We were able to detect pathogenic mutations in only two of these patients.
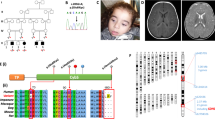
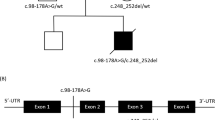
Patient 1, a child with LS, was a compound heterozygote for SURF1 mutations. The first mutation was a T→C transversion at nucleotide 608 (Fig. 1A) that changes a highly conserved leucine to a proline at position 203 (L203P). The second mutation was an 18-bp deletion 675_692del in exon 7 (Fig. 2A); the resulting protein lacked six highly conserved amino acids (aa 226-231), and leucine at position 232 was changed to isoleucine. This is the first in-frame deletion reported in SURF1. Subcloning and sequencing the PCR fragment containing exons 6 and 7 demonstrated that the two mutations were located in different alleles.
(A) Reverse-complemented sequence of the allele harboring the 608 T→C mutation (arrow). The black triangle indicates the 610 A→T polymorphism. (B) Alignments of Surf1 polypeptides in different species. Note in our patient the L203P mutation (arrow) and the adjacent I204F polymorphism (underlined). (C) Hydropathy plots of the Surf1 region with the L203P mutation (aa 150-250). The arrow indicates the altered peak in the patient's protein. Note that the I204F substitution does not alter the plot.
Patient 28 with hypertrophic cardiomyopathy and encephalomyopathy had two mutations in SCO2. He harbored the common E140 K mutation and a novel T→C transition at nt 1575 (Fig. 3A) that changed a conserved leucine at position 151 to a proline (L151P). We analyzed the DNA of his parents and older brother, who had died some years earlier of a similar disease. The brother harbored both mutations, whereas the father carried the E140 K and the mother carried the L151P mutation. These three novel mutations were absent in 100 controls. No pathogenic mutations were found in the three mtDNA-encoded COX subunits; in the 22 tRNA genes; or in SCO1, COX10, COX11, COX15, and COX17.
DISCUSSION
COX deficiency is a relatively common biochemical finding underlying a variety of clinical conditions. It can occur as an isolated defect, or it can accompany defects of other respiratory chain enzymes containing mtDNA-encoded subunits (14). The latter situation usually reflects mtDNA mutations, either largescale rearrangements of mtDNA or mutations in tRNA genes. The genetic causes for isolated COX deficiency can be divided into two main groups. The first includes mutations in structural components of the enzyme, which have been described only in the three mtDNA-encoded COX subunits but not yet in any of the 10 nuclear encoded polypeptides. These mutations are usually sporadic and are associated with variable clinical phenotypes, ranging from exercise intolerance and myoglobinuria to severe multisystemic disease. Ages at onset also vary from neonatal period to adulthood (2, 15).
The second group includes mutations in COX-assembly genes. The proteins encoded by these genes are not structural components of COX but are required for the correct folding and maturation of the various polypeptides and for the synthesis, delivery, and insertion of the prosthetic groups into the holoenzyme. They have been studied extensively in yeast, and some of their human homologues have been identified (Table 3) (16–22). Mutations in COX-assembly genes usually present in the neonatal period or in early childhood, have an autosomal recessive pattern of inheritance, and are associated with severe phenotypes (2).
SURF1 mutations have been reported in >40 patients (23). They are usually associated with classical LS, although they have also been reported in one patient with leukodystrophy (24) and in another with normal neuroimaging, which was limited, however, to computerized tomography (25).
SCO2 defects have been described in 10 patients (4, 26–28). All of them harbored one common mutation, E140 K. Patients with the severe form of the disease are compound heterozygotes, harboring the E140 K and one other mutation. They usually present soon after birth with hypertrophic cardiomyopathy, encephalopathy, and myopathy. One patient, however, presented at birth with a Werdnig-Hoffmann-like syndrome and developed cardiomyopathy later (28). The severe form is fatal within the first year of life. In contrast, patients homozygous for the E140 K mutation exhibit a milder phenotype, with later onset and slower progression of disease (27).
Clinical data for SCO1 and COX10 mutations are scarce. SCO1 defects have been described in two brothers with neonatalonset hepatic failure and encephalopathy (3), whereas COX10 mutations have been reported in a family with encephalopathy and renal tubulopathy (4). These findings suggest that COX assembly pathways are, to a certain extent, tissue-specific (2). In addition, four patients with myoclonic epilepsy, ataxia, hearing loss, and isolated COX deficiency in muscle were found to harbor mutations in mtDNA tRNASer(UCN) (29). The precise mechanism by which a mutation in a tRNA gene produces isolated COX deficiency is still unclear.
We surveyed all genes thus far associated with COX deficiency in a series of 30 patients with various clinical manifestations and biochemical evidence of isolated COX deficiency. We also studied three COX-assembly genes, COX11, COX15, and COX17, which are known to cause COX deficiency in yeast when mutated, but have not yet been associated with human disease. We decided not to screen the 10 nDNAencoded COX genes because previous studies (29, 30), including one by our group (M. Hirano unpublished results), failed to show any mutation.
We identified pathogenic mutations in only two patients. One patient had hypertrophic cardiomyopathy and mutations in SCO2. He had the classical phenotype seen in SCO2 defects: hypertrophic cardiomyopathy in the first days of life, encephalomyopathy, and rapid progression, with death in the second month of life. He harbored the common E140 K mutation and a novel L151P mutation. This leucine is conserved throughout evolution (Fig. 3B). We aligned >80 SCO proteins from different eukaryotic and prokaryotic species. In some species, leucine is substituted either by valine or by isoleucine, both hydrophobic amino acids; no other amino acid was found in the reported sequences. We believe that proline disrupts the secondary structure of the SCO2 protein in a region close to the putative copper binding site. Only one of the six patients with hypertrophic cardiomyopathy had mutations in SCO2, confirming the notion that this clinical phenotype is genotypically heterogeneous (31).
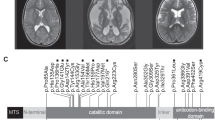
The second patient, with typical features of LS, had mutations in SURF1. He had an 18-bp deletion in exon 7 and a missense mutation 608T→C changing leucine 203 to proline (L203P). Interestingly, this mutation is associated with another nucleotide change, a 610 A→T transversion that changes a nonconserved isoleucine to a phenylalanine (I204F), probably a neutral polymorphism. Leucine at position 203 is conserved throughout evolution (Fig. 1B), and the substitution with a proline clearly alters the hydropathy plot of the protein, whereas the I204P change affecting the adjacent amino acid residue does not alter it (Fig. 1C). The resulting protein is probably incorrectly folded. The 675_692del ablates six conserved amino acids, including tryptophan at position 227 and aspartate at position 231, which are conserved even in prokaryotic homologues of SURF1 (Fig. 2B).
This patient was the only one of six with the classical features of LS in which we could find SURF1 mutations. However, four of the six patients with typical LS had been part of a cohort previously screened by Sue et al. (8) for SURF1 mutations (and found negative). Thus, our LS group was biased against SURF1 mutants. Of the two unbiased LS patients, one (50%) harbored SURF1 mutations, a frequency close to the 41% found by Sue et al. (8), although lower than that found in a large series of European patients (10, 32, 33). Complementation studies in European patients also showed that the majority of COX-deficient LS patients belong to a single complementation group (34, 35). Ethnic factors could account for the lower frequency of SURF1 mutations in our American population, which includes patients of Hispanic, Arabic, Asian, and African origin.
Mutations in the promoter region or in intronic regions not amplified by our primer set might have been overlooked, although our protocols (7) allow us to sequence all SURF1 exons and all those intronic regions where mutations have been reported thus far (16, 36, 37). It is noteworthy, however, that in six of the 40 patients reviewed by Pequignot et al. (16), a mutation was found in only one SURF1 allele, indicating that some mutations must affect regions of the SURF1 gene that are not studied by standard protocols (6, 7) Unfortunately, we could not test this hypothesis because biologic samples from patients 2-6 were not available for immunoblot analysis of Surf1p or complementation studies.
We did not find mutations in COXI, COXII, COXIII, COX10, COX11, COX15 COX17, SCO1, or in the tRNA genes. Mutations in the mtDNA-encoded COX subunits are known to be rare (2), and our study confirms this. Remarkably, none of the patients with liver involvement had mutations in SCO1, indicating that mutations in this gene are probably uncommon and that this phenotype is genetically heterogeneous. None of our patients with encephalopathy had evidence of renal tubulopathy, and this may explain why we did not find mutations in COX10, which have been associated with renal disease in the two reported patients (5).
We also failed to find pathogenic mutations in COX11, COX15, and COX17. Mutation screening of COX15 and COX17 in a patient with LS was negative (18), and another study failed to find mutations in COX17 in patients with myopathy and hypertrophic cardiomyopathy (31). Even when we extended our screening to patients with different phenotypes, we came up empty-handed. Mutations in these genes may be embryonically lethal, very rare, or associated with phenotypes other than isolated infantile COX deficiency.
Because we studied genomic DNA, we may have overlooked some intronic mutations affecting splicing sites or mutations in the promoter region. In addition, the sensitivity of SSCP protocols is ˜90%. Even with these caveats, however, our data underscore the genetic heterogeneity of COX deficiency and indicate that a number of genes remain to be identified. For example, the Saguenay-Lac-St-Jean form of COX deficiency maps to chromosome 2p16 (38), a region with no obvious candidate genes.
The problem of establishing a molecular diagnosis in patients with COX deficiency persists. Most of our cases are sporadic, and even in the presence of a positive family history, the number of affected individuals is too small to perform linkage analysis. Comprehensive genetic screenings like the present one are not practical for routine diagnosis. Immunoblot techniques using anti-Surf1 antibodies have been useful in detecting SURF1 defects because Surf1 levels are markedly reduced in patients (39, 40), including those harboring missense mutation (17). A similar approach could be used for other COX-assembly genes.
Further research will be designed to identify new genes responsible for COX deficiency. We believe that functional complementation studies are the most promising approach to the problem (2). We are currently performing such experiments in fibroblasts from some of the patients in this series.
Abbreviations
- COX:
-
cytochrome c oxidase (EC 1.9.3.1)
- mtDNA:
-
mitochondrial DNA
- nDNA:
-
nuclear DNA
- SSCP:
-
single strand conformational polymorphism
- LS:
-
Leigh syndrome
REFERENCES
Michel H, Behr J, Harrenga A, Kannt A 1998 Cytochrome c oxidase: structure and spectroscopy. Ann Rev Biophys Biomol Struct 27: 329–356.
Shoubridge EA 2001 Cytochrome c oxidase deficiency. Am J Med Genet 106: 46–52.
Valnot I, Osmond S, Gigarel N, Mehaye B, Amiel J, Cormier-Daire V, Munnich A, Bonnefont JP, Rustin P, Rotig A 2000 Mutations of the SCO1 gene in mitochondrial cytochrome c oxidase deficiency with neonatal-onset hepatic failure and encephalopathy. Am J Hum Genet 67: 1104–1109.
Papadopoulou LC, Sue CM, Davidson M, Tanji K, Nishino I, Sadlock J, Selby J, Glerum DM, Van Coster R, Lyon G, Scalais E, Lebel R, Kaplan P, Shanske S, De Vivo DC, Bonilla E, Hirano M, DiMauro S, Schon EA 1999 Fatal infantile cardioencephalomyopathy with COX deficiency and mutations in SCO2, a human COX assembly gene. Nat Genet 23: 333–337.
Valnot I, von Kleist-Retzow JC, Barrientos A, Gorbatyuk M, Taanman JW, Mehaye B, Rustin P, Tzagoloff A, Munnich A, Rotig A 2000 A mutation in the human heme A:farnesyltransferase gene (COX10) causes cytochrome c oxidase deficiency. Hum Mol Genet 9: 1245–1249.
Zhu Z, Yao J, Johns T, Fu K, De Bie I, Macmillan C, Cuthbert AP, Newbold RF, Wang J, Chevrette M, Brown GK, Brown RM, Shoubridge EA 1998 SURF1, encoding a factor involved in the biogenesis of cytochrome c oxidase, is mutated in Leigh syndrome. Nat Genet 20: 337–343.
Tiranti V, Hoertnagel K, Carrozzo R, Galimberti C, Munaro M, Granatiero M, Zelante L, Gasparini P, Marzella R, Rocchi M, Bayona-Bafaluy MP, Enriquez JA, Uziel G, Bertini E, Dionisi-Vici C, Franco B, Meitinger T, Zeviani M 1998 Mutations of SURF-1 in Leigh disease associated with cytochrome c oxidase deficiency. Am J Hum Genet 63: 1609–1621.
Sue CM, Karadimas C, Checcarelli N, Tanji K, Papadopoulou LC, Pallotti F, Guo FL, Shanske S, Hirano M, De Vivo DC, Van Coster R, Kaplan P, Bonilla E, DiMauro S 2000 Differential features of patients with mutations in two COX assembly genes, SURF-1 and SCO2. Ann Neurol 47: 589–595.
DiMauro S, Servidei S, Zeviani M, DiRocco M, De Vivo DC, DiDonato S, Uziel G, Berry K, Hoganson G, Johnsen SD, Johnson PC 1987 Cytochrome c oxidase deficiency in Leigh syndrome. Ann Neurol 22: 498–506.
Sciacco M, Bonilla E 1996 Cytochemistry and immunocytochemistry of mitochondria in tissue sections. Methods Enzymol 264: 509–521.
Sambrook J, Russel DW 2001 Molecular Cloning: A Laboratory Manual. Cold Spring Harbor Laboratory Press, Cold Spring Harbor, NY, pp. 6.4–6.11
Rieder MJ, Taylor SL, Tobe V, Nickerson DA 1998 Automatic identification of DNA variations using quality-based fluorescence re-sequencing: analysis of the human mitochondrial genome. Nucleic Acids Res 26: 967–973.
Karadimas CL, Greenstein P, Sue CM, Joseph JT, Tanji K, Haller RG, Taivassalo T, Davidson MM, Shanske S, Bonilla E, DiMauro S 2000 Recurrent myoglobinuria due to a nonsense mutation in the COX I gene of mitochondrial DNA. Neurology 55: 644–649.
DiMauro S, Bonilla E, Davidson M, Hirano M, Schon EA 1998 Mitochondria in neuromuscular disorders. Biochim Biophys Acta 1366: 199–210.
Campos Y, Garcia-Redondo A, Fernandez-Moreno MA, Martinez-Pardo M, Goda G, Rubio JC, Martin MA, del Hoyo P, Cabello A, Bornstein B, Garesse R, Arenas J 2001 Early-onset multisystem mitochondrial disorder caused by a nonsense mutation in the mitochondrial DNA cytochrome c oxidase II gene. Ann Neurol 50: 409–413.
Glerum DM, Tzagoloff A 1994 Isolation of a human cDNA for heme A:farnesyltransferase by functional complementation of a yeast cox10 mutant. Proc Natl Acad Sci U S A 91: 8452–8456.
Amaravadi R, Glerum DM, Tzagoloff A 1997 Isolation of a cDNA encoding the human homolog of COX17, a yeast gene essential for mitochondrial copper recruitment. Hum Genet 99: 329–333.
Petruzzella V, Tiranti V, Fernandez P, Ianna P, Carrozzo R, Zeviani M 1998 Identification and characterization of human cDNAs specific to BCS1, PET112, SCO1, COX15, and COX11, five genes involved in the formation and function of the mitochondrial respiratory chain. Genomics 54: 494–504.
Dickinson EK, Adams DL, Schon EA, Glerum DM 2000 A human SCO2 mutation helps define the role of Sco1p in the cytochrome oxidase assembly pathway. J Biol Chem 275: 26780–26785.
Hiser L, Di Valentin M, Hamer AG, Hosler JP 2000 Cox11p is required for stable formation of the Cu(B) and magnesium centers of cytochrome c. J Biol Chem 275: 619–623.
Barros MH, Carlson CG, Glerum DM, Tzagoloff A 2001 Involvement of mitochondrial ferredoxin and Cox15p in hydroxylation of heme O. FEBS Lett 492: 133–138.
Nijtmans LG, Artal Sanz M, Bucko M, Farhoud MH, Feenstra M, Hakkaart GA, Zeviani M, Grivell LA 2001 Shy1p occurs in a high molecular weight complex and is required for efficient assembly of cytochrome c oxidase in yeast. FEBS Lett 498: 46–51.
Pequignot MO, Dey R, Zeviani M, Tiranti V, Godinot C, Poyau A, Sue C, Di Mauro S, Abitbol M, Marsac C 2001 Mutations in the SURF1 gene associated with Leigh syndrome and cytochrome c oxidase deficiency. Hum Mutat 17: 374–381.
Rahman S, Brown RM, Chong WK, Wilson CJ, Brown GK 2001 A SURF1 gene mutation presenting as isolated leukodystrophy. Ann Neurol 49: 797–800.
Von Kleist-Retzow JC, Yao J, Taanman JW, Chantrel K, Chretien D, Cormier-Daire V, Rötig A, Munnich A, Rustin P, Shoubridge EA 2001 Mutations in SURF1 are not specifically associated with Leigh syndrome. J Med Genet 38: 109–113.
Jaksch M, Ogilvie I, Yao J, Kortenhaus G, Bresser HG, Gerbitz KD, Shoubridge EA 2000 Mutations in SCO2 are associated with a distinct form of hypertrophic cardiomyopathy and cytochrome c oxidase deficiency. Hum Mol Genet 9: 795–801.
Jaksch M, Horvath R, Horn N, Muller-Hocker J, Horvath R, Trepesch N, Stecker G, Freisinger P, Thirion C, Muller J, Lunkwitz R, Rodel G, Shoubridge EA, Lochmuller H 2001 Homozygosity (E140K) in SCO2 causes delayed infantile onset of cardiomyopathy and neuropathy. Neurology 57: 1440–1446.
Salviati L, Sacconi S, Rasalam M, Kron DF, Braun A, Davidson M, Bonilla E, Shanske S, Canoll P, Hays AP, Schon EA, DiMauro S 2002 Cytochrome oxidase deficiency due to a novel SCO2 mutation mimics Werdnig-Hoffmann disease. Arch Neurol 59: 862–865.
Jaksch M, Hofmann S, Kleinle S, Liechti-Gallati S, Pongratz DE, Muller-Hocker J, Jedele KB, Meitinger T, Gerbitz KD 1998 A systematic mutation screen of 10 nuclear and 25 mitochondrial candidate genes in 21 patients with cytochrome c oxidase (COX) deficiency shows tRNA(Ser)(UCN) mutations in a subgroup with syndromal encephalopathy. J Med Genet 35: 895–900.
Adams PL, Lightowlers RN, Turnbull DM 1997 Molecular analysis of cytochrome c oxidase deficiency in Leigh's syndrome. Ann Neurol 41: 268–270.
Horvath R, Lochmuller H, Stucka R, Yao J, Shoubridge EA, Kim SH, Gerbitz KD, Jaksch M 2000 Characterization of human SCO1 and COX17 genes in mitochondrial cytochrome-c-oxidase deficiency. Biochem Biophys Res Commun 276: 530–533.
Tiranti V, Jaksch M, Hofmann S, Galimberti C, Hoertnagel K, Lulli L, Freisinger P, Bindoff L, Gerbitz KD, Comi GP, Uziel G, Zeviani M, Meitinger T 1999 Loss-offunction mutations of SURF-1 are specifically associated with Leigh syndrome with cytochrome c oxidase deficiency. Ann Neurol 46: 161–166.
Coenen MJ, van den Heuvel LP, Nijtmans LG, Morava E, Marquardt I, Girschick HJ, Trijbels FJ, Grivell LA, Smeitink JA 1999 SURFEIT-1 gene analysis and twodimensional blue native gel electrophoresis in cytochrome c oxidase deficiency. Biochem Biophys Res Commun 265: 339–344.
Brown RM, Brown GK 1996 Complementation analysis of systemic cytochrome oxidase deficiency presenting as Leigh syndrome. J Inherit Metab Dis 19: 752–760.
Munaro M, Tiranti V, Sandona D, Lamantea E, Uziel G, Bisson R, Zeviani M 1997 A single cell complementation class is common to several cases of cytochrome c oxidase-defective Leigh's syndrome. Hum Mol Genet 6: 221–228.
Williams SL, Taanman JW, Hansikova H, Houst'kova H, Chowdhury S, Zeman J, Houstek J 2001 A novel mutation in SURF1 causes skipping of exon 8 in a patient with cytochrome c oxidase-deficient Leigh syndrome and hypertrichosis. Mol Genet Metab 73: 340–343.
Pequignot MO, Desguerre I, Dey R, Tartari M, Zeviani M, Agostino A, Benelli C, Fouque F, Prip-Buus C, Marchant D, Abitbol M, Marsac C 2001 New splicing-site mutations in the SURF1 gene in Leigh syndrome patients. J Biol Chem 276: 15326–15329.
Lee N, Daly MJ, Delmonte T, Lander ES, Xu F, Hudson TJ, Mitchell GA, Morin CC, Robinson BH, Rioux JD 2001 A genomewide linkage-disequilibrium scan localizes the Saguenay-Lac-Saint-Jean cytochrome oxidase deficiency to 2p16. Am J Hum Genet 68: 397–409.
Tiranti V, Galimberti C, Nijtmans L, Bovolenta S, Perini MP, Zeviani M 1999 Characterization of SURF-1 expression and Surf-1p function in normal and disease conditions. Hum Mol Genet 8: 2533–2540.
Yao J, Shoubridge EA 1999 Expression and functional analysis of SURF1 in Leigh syndrome patients with cytochrome c oxidase deficiency. Hum Mol Genet 8: 2541–2549.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was supported by National Institutes of Health Grants PO1HD32062 and NS11766 and by a grant from the Muscular Dystrophy Association. L.S. is supported by grant 439b from Telethon Italia and by a scholarship from the University of Padova.
Rights and permissions
About this article
Cite this article
Sacconi, S., Salviati, L., Sue, C. et al. Mutation Screening in Patients With Isolated Cytochrome c Oxidase Deficiency. Pediatr Res 53, 224–230 (2003). https://doi.org/10.1203/01.PDR.0000048100.91730.6A
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/01.PDR.0000048100.91730.6A