Abstract
We studied gastric volume, wall compliance, sensory perception, and receptive relaxation during the first postnatal 80 h in 17 healthy term infants, using a computer-driven air pump and simultaneously measuring pressure and volume within a latex balloon placed through the oropharynx into the stomach. To evaluate gastric compliance, we measured pressures while we infused air into the intragastric balloon at different rates (10, 20, and 60 mL/min) in random sequence. In all infants, there was a linear relationship between intragastric pressure and volume to the maximum pressure tested, 30 mm Hg. Gastric compliance ranged from 0.2 mL/mm Hg to 3.8 mL/mm Hg. Different infusion rates had no effect on compliance. We calculated gastric receptive relaxation by measuring the volume needed to maintain a constant pressure of 10 mm Hg within the balloon for 5 min. Gastric receptive relaxation ranged from 0.5 mL/min to 54 mL/min. Gastric compliance and receptive relaxation increased with postnatal age (r = 0.70, p < 0.005;r = 0.79, p < 0.001, respectively) and with number of feedings (r = 0.80, r = 0.88, respectively, both p < 0.001). There was no correlation between weight or type of feeding (breast versus formula) and either gastric compliance or relaxation. In conclusion, these results may explain the small feedings that neonates ingest in the first days of life. During the first 3 postnatal d, the newborn stomach becomes more compliant and develops more receptive relaxation, associated with a larger volume capacity.
Similar content being viewed by others
Main
In healthy neonates, the volume of feedings in the first days of life is 60–100 mL/kg per day or about 20–40 mL per feeding. After a few days, the healthy neonate ingests approximately 150 mL/kg per day, or about 75 mL per feeding. The relatively low feeding volume during the first hours of life, coinciding with the physiologic diuresis of excess extracellular fluid that accompanies the transition from prenatal to postnatal life, may be caused by one or more factors, including a lack of hunger or thirst because of CNS depression or arousal, changing hormone concentrations associated with parturition, or immaturity of gastric function. Despite the appearance of anatomic features of the digestive tract early in fetal life (1, 2), many aspects of gastrointestinal motility are immature in the neonate (3–6). In vitro studies demonstrated rapid postnatal changes in the receptors (7, 8) and responses to agonists in rabbit gastric muscle (9, 10). One potential explanation for the small voluntary feeding volumes in the hours immediately after birth is an immaturity of gastric relaxation to accommodate the entry of a meal.
In healthy children and adults, the gastric fundus and body relax as a meal enters, so that there is little increase in intragastric pressures over a wide range of volumes (11–13). Azpiroz and Malagelada (12, 13) used a computer-driven air pump to infuse air into a noncompliant balloon placed in the stomach. Pressures increased initially as the stomach started to fill. As the stomach continued to fill, there was a pressure plateau at which continued increases in intragastric volume caused no increase in intragastric pressure over a wide range of volumes. Finally, the pressures begin to rise again, with the subject experiencing a sense of fullness and then pain. The pressure plateau is caused by gastric accommodation to filling, also known as receptive relaxation. Receptive relaxation requires sensory and motor coordination through vagovagal reflexes, with relaxation likely to be mediated by nitric oxide (14) and dopamine (15).
The purposes of this study were to obtain data about the response of the stomach to distention and to identify factors involved in the maturation of gastric relaxation in healthy term newborn infants.
METHODS
The study group included 17 healthy term breast- or bottle-fed (every 4 h) neonates (eight boys), all within the first week of life. Subjects were approved for testing by the attending neonatologist. The protocol was approved by the Harbor-UCLA Medical Center Human Subjects Committee in May 1993, and written informed consent was obtained from the parents. The assessment was timed to begin 3 h after the previous feeding, or 1 h before the next scheduled feeding.
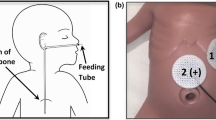
We placed a latex balloon attached to the end of an 8F infant feeding tube through the oropharynx into the stomach. We monitored the heart rate in all patients during the test session. We began testing when heart rate returned to baseline and the infant was comfortable, several minutes after passage of the balloon. Infants were swaddled and held by a nurse during the test session. A computer-driven air pump simultaneously recorded pressure and volume within the balloon to evaluate variables of gastric volume, compliance, and relaxation. To assure subject safety, we set the maximum intragastric pressure at 30 mm Hg. Any increase in intragastric or intraabdominal pressure >30 mm Hg, such as that caused by a retch or a cry, triggered an instantaneous balloon deflation. For comparison, vomiting is associated with intragastric pressures of approximately 300 mm Hg, and normal gastric antral contractions are 80 mm Hg in healthy term infants, and twice that value in adults. Adult volunteers noted an initial perception from the stomach with balloon distending pressures averaging 23 mm Hg, and pain with pressures averaging 26 mm Hg (16). We used computer software to determine intragastric pressure by subtracting the average pressure generated for each volume during three balloon inflations outside the body from pressures obtained at each balloon volume inside the body. For one part of the testing, we infused air into the balloon at different rates (10, 30, and 60 mL/min) in random sequence. During a second phase of the testing, using the same balloon, we set the intragastric pressure at 10 mm Hg, and assessed balloon volume for 5 min. It was our plan to stop the air infusion when the gastric pressure caused a sign of discomfort indicated by a facial grimace and retch, or when we reached the maximal programed intragastric pressure of 30 mm Hg. Each test session lasted approximately 40 min, after which the balloon was deflated and removed with the tube.
We noted sex, age (in hours), number of meals, and the type of feeding (bottle-versus breast-feeding) for each participant. An actual compliance curve was calculated for each neonate. We defined gastric compliance as the ratio of the difference between two volume measurements and the corresponding pressure values. After reviewing the volume-pressure plots for each child, we decided to calculate compliance from volumes obtained when intragastric pressures were 10 and 28 mm Hg. Thus, gastric compliance was defined by the slope of the volume-pressure curve in units of milliliters per millimeter of mercury. In healthy adults, the initial compliance was 55 ± 6 mL/mm Hg (16). Based on adult data (13, 16–18), we defined gastric receptive relaxation by the volume needed to maintain a constant pressure of 10 mm Hg within the balloon for 5 min (in milliliters per minute). We used the Mann-Whitney U test with a level of significance of 0.05 to test for sex differences in birth weight, number of meals, type of feeding (breast versus bottle), gastric compliance, and gastric relaxation. To test age and number of meals as predictors of gastric compliance and receptive relaxation, we used correlation analysis and multiple regression analysis. Age was entered first into the equation as a stable characteristic followed by number of meals.
RESULTS
Gastric volumes at the maximal pressure tested, 30 mm Hg, ranged from 38 to 76 mL. In all neonates, there was a linear relationship between intragastric pressure and volume to 30 mm Hg (Fig. 1). Different infusion rates had no effect on the pressure-volume relationship or on discomfort. There were no complications associated with testing, and there were no heart rate increases to the maximal pressure tested, suggesting an absence of discomfort. Gastric compliance ranged from 0.2 to 3.8 mL/mm Hg. When normalized for body surface area, compliance was 32 ± 10 mL·mm Hg−1·m−2 for adults versus 1–17 mL·mm Hg−1·m−2 in the infants. Gastric receptive relaxation ranged from 0.5 to 54 mL/min in the infants. There were no differences at p < 0.05 between boys and girls in age (in hours), weight at birth, number of meals, type of feeding (breast milk versus bottle), gastric compliance, and gastric relaxation. There was a positive correlation between age and gastric compliance (r = 0.70, p < 0.01) and gastric receptive relaxation (r = 0.79, p < 0.001). There was a positive correlation between number of feedings and gastric compliance (r = 0.80, p < 0.001; Fig. 2), and number of feedings and gastric receptive relaxation (r = 0.88, p < 0.001; Fig. 3).
An intragastric pressure-volume plot from a single distention in one newborn. The flat portion of the curve between 0 and 15 mL is an artifact caused by the volume required to open the balloon. Note the linear pressure-volume relationship from 5 mm Hg to the maximal pressure tested, 30 mm Hg. There is no plateau with a 0 slope, as expected in adults.
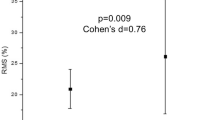
Relationship between gastric compliance and the number of feedings in neonates. Each neonate had a fixed compliance value (the slope of the volume-pressure relationship was linear) up to 30 mm Hg. There was a positive correlation between number of feedings and gastric compliance (r = 0.80;p < 0.001).
Relationship etween gastric receptive relaxation and the number of feedings in neonates. Gastric receptive relaxation was evaluated by measuring the volume needed to maintain a constant pressure of 10 mm Hg within the balloon for 5 min. There was a positive correlation between number of feedings and receptive relaxation (r = 0.88;p < 0.001).
Age accounted for 48.5% of the variance in gastric compliance (p < 0.05). Above and beyond age, the number of meals accounted for an additional 14.2% of compliance (p < 0.05). Both factors taken together explain 63% of the increase in compliance in these neonates (p < 0.001). A second multiple regression equation was calculated to predict gastric receptive relaxation with age first and number of meals second as independent variables. Age explained 63.1% (p < 0.0001) and number of meals, 15.4% of the variance in gastric receptive relaxation (p < 0.01). Age and number of meals explained a total of 79% of the variance of receptive relaxation for these neonates. The high correlation between compliance and receptive relaxation of 0.87 (p < 0.001) indicates that they mature at a similar rate.
DISCUSSION
Our current data demonstrated that in contrast to adults, the plateau in intragastric pressure as the gastric lumen distends until full is absent in the newborn. In the newborn intragastric pressures increased for every increase in gastric volume. However, even within the first days of life and the first few feedings, there was a change toward developing greater receptive relaxation and compliance in response to distention. Calculated values for both receptive relaxation and compliance increased during the first 3 d of life. Moreover, the volumes required to fill the stomach to the maximal pressure that we allowed more than doubled during this same period.
The clinical consequences of a noncompliant, nonrelaxing stomach are apparent from the natural history of the newborn infant. The first feedings are small in volume. Regurgitation is common. Both of these observations may be related to a noncompliant stomach. Slow gastric emptying because of postprandial duodenal hypomotility might also contribute to small feeding volumes and regurgitation in the first hours after birth in healthy term infants, as it does in preterm infants (19, 20). Both infant age and the number of feedings increased gastric compliance and receptive relaxation, resulting in larger balloon infusion volumes. Statistics demonstrated that increasing age and number of feedings accounted for more than half the measured changes.
There are so many rapid physiologic changes within the first hours of extrauterine life that explaining how a few hours and a few meals alter gastric neuromuscular function can only be speculative at this time. One possible factor is the surge and ebb of stress hormones during and after delivery (21, 22). Accommodation to luminal distention may be diminished in the first hours of life because of the dominance of sympathetic tone over parasympathetic tone (21, 22).
The rapidly changing newborn gut peptide profile, including increases from adult values in gastrin, enteroglucagon, and neurotensin serum concentrations are another potential influence on gastric adaptation (23). From in vitro studies we learned that gastric smooth muscle undergoes rapid time-dependent changes in the maturation of actomyosin (24), calcium channels (25), neurotransmitter receptors (7, 8), and responses to a variety of ligands (9, 10). It is possible that the matrix of connective tissue supporting gastric smooth muscle requires an initial series of stretches before becoming relaxed.
The most likely explanation for rapid postnatal increase in gastric compliance may be the maturation of vagovagal reflexes (26, 27). Gastric receptive relaxation is regulated mainly by inhibitory vagal neurons and nitrergic neurons (14). Dopamine also inhibits gastric tone (15). Perinatal changes in these signals have not yet been explored, but may be a fertile area for investigation.
In adults, early satiety may occur in the absence of disease as a symptom of functional dyspepsia (28). Early satiety caused by functional dyspepsia may be a consequence of one or more of three mechanisms:1) delayed gastric emptying, 2) visceral hyperalgesia, an increased sensitivity of afferent sensory nerves from the stomach to the CNS, and 3) impaired accommodation to distention (18). From our results, impaired accommodation seems a likely explanation for early satiety in neonates. From results of motility testing, delayed gastric emptying also seems a plausible explanation (19, 20). On the basis of our studies, in which 30 mm Hg did not provoke evidence for discomfort, visceral hyperalgesia seems an unlikely cause of early satiety in the neonate.
A group of thought leaders in gastrointestinal sensory testing recently recommended an infinitely compliant balloon for barostat studies (29). We used a latex balloon because it was more compact, easier, and safer to pass through the newborn's oropharynx than the recommended polyethylene balloon. To compensate for the compliance of the latex, we measured the balloon's filling pressures for each volume when outside the body, and subtracted those values from the pressures obtained at corresponding volumes in the stomach to record the intragastric pressure. We used a random sequence of three different distention rates to assess whether rapid or slow distention altered the results. At the infusion rates tested there were no differences, although in adults there are receptors that respond to either slow or fast stretch (30).
These data add to our knowledge of neonatal physiology and provide insight into the mechanisms for early satiety in the first days of life. Further research will be necessary to determine how rapidly adult patterns are attained, and whether there are clinical implications to these findings.
References
Grand RJ, Watkins JB, Torti FM 1976 Development of the human gastrointestinal tract: a review. Gastroenterology 70: 790–810
Gershon MD, Chalazonitis A, Rothman TP 1993 From neural crest or bowel: development of enteric nervous system. J Neurobiol 24: 199–214
Amaranath RP, Berseth CL, Malagelada JR, Perrault J, Abell TL, Hoffman AD 1989 Postnatal maturation of small intestinal motility in preterm infants. J Gastro Motil 1: 138–143
Bisset WM, Watt JB, Rivers RPA, Milla PJ 1988 Ontogeny of fasting small intestinal motor activity in human infant. Gut 29: 483–488
Berseth CL 1989 Gestational evolution of small intestinal motility in preterm and term infants. J Pediatr 115: 646–651
Tomomasa T, Itoh Z, Koizumi T, Kuroume T 1985 Nonmigrating rhythmic activity in the stomach and duodenum of neonates. Biol Neonate 48: 1–9
Tomomasa T, Hyman PE, Hsu CT, Jing J, Snape WJ 1988 Development of the muscarinic receptor in rabbit gastric smooth muscle. Am J Physiol 254: G680–G686
Hyman PE, Kimura S, Tomomasa T, Yuan QX, Snape WJ, McRoberts JA 1988 Postnatal changes in the substance P receptor on rabbit gastric smooth muscle. Am J Physiol 262: G291–G297
Tomomasa T, Yagi H, Kimura S, Snape WJ, Hyman PE 1989 Developmental changes in agonist-mediated gastric smooth muscle contraction in the rabbit. Pediatr Res 26: 458–461
Hyman PE, Hou HX, Willenbucher R, Snape WJ, Tomomasa T 1993 Postnatal changes in receptor-mediated rabbit gastric smooth muscle relaxation. Biol Neonate 64: 310–317
Cannon WB, Lieb CW 1911 The receptive relaxation of the stomach. Am J Physiol 29: 267–273
Azpiroz F, Malagelada J-R 1985 Physiologic variations in canine gastric tone measured by an electronic barostat. Am J Physiol 248: G229–G237
Azpiroz F, Malagelada J-R 1987 Gastric tone measured by an electronic barostat in health and postsurgical gastroparesis. Gastroenterology 192: 934–943
Desai KM, Cessa WC, Vane JR 1991 Involvement of nitric oxide in the reflex relaxation of the stomach to accommodate food or fluid. Nature 351: 477–479
Valenzuela JE 1976 Dopamine as a possible neurotransmitter in gastric relaxation. Gastroenterology 71: 1019–1021
Tack J, Piessevaux H, Coulie B, Caenepeel P, Janssens J 1998 Role of impaired gastric accommodation to a meal in functional dyspepsia. Gastroenterology 115: 1346–1352
Tack J, Coulie B, Wilmer A, Andrioli A, Janssens J 2000 Influence of sumatriptan on gastric fundus tone and on the perception of gastric distension in man. Gut 46: 468–473
Holtman G, Gschossmann J, Neufang-Huber J, Gerken G, Talley NJ 2000 Differences in gastric mechanosensory function after repeated ramp distensions in non-consulters with dyspepsia and healthy controls. Gut 47: 332–336
DeVille K, Knapp E, Al-Tawil Y, Berseth CL 1998 Slow infusion feedings enhance duodenal motor responses and gastric emptying in preterm infants. Am J Clin Nutr 68: 103–108
Al-Tawil Y, Berseth CL 1996 Gestational and postnatal maturation of duodenal motor responses to intragastric feeding. J Pediatr 129: 374–381
Lagercrantz H, Slotkin TA 1986 The “stress” of being born. Sci Am 254: 100–107
Padbury J, Martinez M 1988 Sympathoadrenal system activity at birth: integration of postnatal adaptation. Semin Perinatol 12: 163–172
Lucas A 1989 Ontogeny of gut hormones and hormone related substances. Acta Pediatr Scand (suppl): 80–87
Tomomasa T, Xie YN, Morikawa A, Kurome T, Hyman PE 1995 Postnatal changes in size and actomyosin content of rabbit gastric myocytes. Reprod Fertil Dev 7: 1305–1310
Hyman PE, Martin MG, Tomomasa T, Jing J, Snape WJ 1989 Development of calcium channels in gastric smooth muscle. Pediatr Res 25: 600–604
Andrews PLR, Scratcherd T 1980 The gastric motility patterns induced by direct and reflex excitation of the vagus nerves in the anesthetized ferret. J Physiol Lond 302: 363–378
Wilbur BG, Kelly KA, Code CF 1973 Effect of proximal gastric, complete gastric and truncal vagotomy on canine gastric electric activity, motility and emptying. Ann Surg 178: 295–302
Talley NJ, Stanghellini V, Heading RC, Koch KL, Malagelada J-R, Tytgat GNJ 2000 The Functional Gastrointestinal Disorders, 2nd ed. Degnon Associates, McLean, VA
Whitehead WE, Delvaux M 1997 Standardization of barostat procedures for testing smooth muscle tone and sensory thresholds in the gastrointestinal tract. Dig Dis Sci 42: 223–241
Mayer EA, Gebhart GF 1994 Basic and clinical aspects of visceral hyperalgesia. Gastroenterology 107: 271–293
Acknowledgements
The authors thank Dr. Emeran Mayer for advice on methodology and data analysis. Also, we are indebted to UCLA biomedical engineer John Parker for creating the hardware and software for our computer-driven air pump.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported in part by Janssen Research Foundation.
Rights and permissions
About this article
Cite this article
Zangen, S., Di Lorenzo, C., Zangen, T. et al. Rapid Maturation of Gastric Relaxation in Newborn Infants. Pediatr Res 50, 629–632 (2001). https://doi.org/10.1203/00006450-200111000-00016
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-200111000-00016