Abstract
Although evidence shows that victims of sudden infant death syndrome (SIDS) suffer repetitive episodes of hypoxemia, only subtle abnormalities have been found in their brains by light microscopy. The aim of the present study was to determine whether apoptosis, a form of cell death that can be triggered by hypoxemia and that leaves no scarring detectable by light microscopy, would be present in hypoxia-sensitive brain regions of SIDS victims. We looked for the presence of apoptosis with an in situ end-labeling method that detects DNA fragmentation. We studied 29 SIDS victims who were age-matched to nine control cases. We found significant neuronal apoptosis in 79% of the SIDS cases: 55% of the cases positive in the hippocampus and 96% positive in the brainstem. Whereas the distribution of apoptosis in the hippocampus was in hypoxia-sensitive subregions, the distribution in the brainstem was mostly in dorsal nuclei, including those involved with sensation in the face and position of the head (nucleus of the spinal trigeminal tract and vestibular nuclei). The control cases showed no significant apoptosis in the hippocampus and a mild degree in the brainstem in three cases. Our results indicate the occurrence of an acute insult at least several hours before death, an insult from which the infants had apparently recuperated. This suggests that SIDS victims suffered repeated apoptosis resulting in significant neuronal damage and, thus, functional loss in key brain regions. The involvement of specific nuclei in the brainstem may be linked to the fact that prone sleeping is a significant risk factor for SIDS. Enhanced neuronal death by apoptosis may thus have major implications for understanding the sequence of events leading to SIDS.
Similar content being viewed by others
Main
SIDS is defined as the sudden death of an infant under 1 y of age that remains unexplained after performance of a complete autopsy, examination of the death scene, and review of the clinical history (1). It is hypothesized that infants who die of SIDS have a brain abnormality (possibly at the brainstem level) or a maturational delay related to neuroregulation of cardiorespiratory control leading to repeated episodes of hypoxemia (2). SIDS victims present histologic and biochemical findings consistent with prior repeated episodes of hypoxemia in several organs (3–8). However, examination of the brains of SIDS victims by light microscopy has revealed only subtle abnormalities (9) that, in themselves, are insufficient to explain the death.
Programmed cell death (apoptosis) can be triggered acutely in the brain by a hypoxic insult (10–12) and, typically, leaves no scarring. A cell that dies by apoptosis retains an intact membrane and is engulfed and digested by neighboring cells without any inflammatory reaction (unlike the process of necrosis) (13). Thus, an attractive hypothesis for the cause of death in SIDS is that repeated episodes of hypoxemia first lead neuronal apoptosis in select vulnerable brain regions, then to the disappearance of a significant number of cells, and eventually to impaired function. Apoptosis involves a distinctive multistage process of DNA fragmentation by endonucleolytic degradation (14,15). A relatively new technique to identify such fragmentation allows quantification of this process in various tissues, including the brain (16,17).
The aim of the present study was to determine whether apoptosis is found in the brainstem and hippocampus of SIDS victims. We chose to include the hippocampus because we had found evidence of recent hypoxemic-ischemic insult predominant in this brain region in a group of SIDS victims (18). The hippocampus is composed of subregions that are either sensitive or resistant to hypoxic-ischemic insult (19–21), thus permitting us to determine whether enhanced apoptosis (if present) is predominantly located in hypoxia-sensitive subregions or is more generalized. Moreover, in the neonatal period, the brainstem and hippocampus display a distinct pattern of reaction to hypoxic-ischemic insults (22–24); also, the hippocampus is the region in which the histologic findings in SIDS victims (8) resemble those found in animals exposed to hypoxic-ischemic insults (25–27).
METHODS
We studied 29 SIDS (19 males) and nine control cases (six males). Four additional cases of SIDS who survived temporarily after resuscitation were also included. The control group consisted of infants who had died in circumstances similar to those of the SIDS victims: death occurred suddenly in asymptomatic infants with no prior evidence of either neurologic disorder or any disease characterized by chronic hypoxia. The diagnoses were as follows: bronchopneumonia, three cases; pyelonephritis with early septicemia, two cases; septicemia, one case; endocardial fibroelastosis, one case. Although the remaining two control cases had no definitive diagnosis after a full autopsy, the infants died suddenly in the awake state during a crying spell (possible arrhythmia). Inasmuch as true control cases are rare, these were identified first and age-matched SIDS cases were then found (age range 35 to 127 d). All infants had had a thorough autopsy at a pediatric center, and an expert panel reviewed all cases to ensure conformity to the accepted definition of SIDS (11).
We used two techniques to identify apoptotic cells. First, we used the in situ end-labeling of DNA, a method now well established for paraffin-embedded tissue that enables the quantification of the apoptotic process in subregions of the brain (16,17). Second, we confirmed the nuclear changes typical of apoptosis by morphologic criteria. Those were the following: a well-defined nucleus; condensed chromatin within the nucleus or at the periphery of the nuclear membrane; and, at later stages, condensation of the cytoplasm and the appearance of apoptotic bodies (28). To this end, we examined slides stained for apoptosis and slides from adjacent sections stained with HPS.
We used a commercial kit (Apoptag, ONCOR, Gaithersburg, MD) for the in situ labeling. We performed the test on 5-µm paraffin sections. The apoptotic cells were identified by direct immunoperoxidase detection of digoxigenin-labeled genomic DNA in situ. The Apoptag kit targets (for labeling) the 3′-OH ends generated by DNA fragmentation. The paraffin sections were mounted on poly-L-lysine-coated slides. They were then deparaffinized in xylene, dehydrated in ethanol, and treated with proteinase K (10 µg/mL in PBS) for 10 min to digest protein before being treated with 50% methanol for inactivation of endogenous peroxidase (30 min in 2% hydrogen peroxide). All sections then underwent treatment to add digoxigenin-dUTP to the 3′-OH ends of the DNA fragments by terminal deoxynucleotidyl transferase (Tdt). Next, an antidigoxigenin antibody carrying a conjugated peroxidase was added. The peroxidase enzyme catalytically generates an intense signal from chromogenic substrates in nuclei that have high concentrations of cleaved DNA 3′-OH ends. Apoptotic nuclei will then appear dark brown, whereas normal nuclei will have blue background coloration (Mayer's hematoxylin). All sections were processed in triplicate, with each run including a positive (adrenal tissue) and a negative control (Tdt omitted).
We also examined the HPS slides for features of neuronal necrosis, features comprising an increased cytoplasmic density (eosinophilic cytoplasm), indistinct nuclear-cytoplasmic boundaries, hyperchromatic pyknotic nuclei, and retracted cells (29–31). The presence of such damaged neurons attests to the occurrence of a recent neuronal insult; their regional distribution within the hippocampus helps to determine the time of such an insult (32–34).
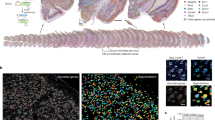
One section containing the hippocampus (Fig. 1) and usually two to three sections of the right brainstem were available to us in paraffin blocks. The brainstem blocks had been taken from two places: one usually at the obex and the other at the open medulla near the level of the cranial nuclei X and XII. The nuclei studied at each level are shown in a diagrammatic representation of the brainstem in Figure 2.
Overview of the hippocampus showing the location of the analyzed regions. The surface of the counted area represents about one half of the CA4 and subiculum (SUB) region. Except for the boundary regions (the transition is not always clearly evident), the entire area of the CA3, CA2, and CA1 subregions were included in the counts. The average number of neurons counted per region were as follows: CA4 = 245, CA3 = 191, CA2 = 96, CA1 = 79, and SUB = 277.
Computer-generated diagram of the brainstem sections. Left panel, level of the obex; right panel, level of the open medulla. Abbreviations and average number of neurons counted per nuclei: Acc Oliv, accessory olive; Cun, cuneate (163); Grac, gracilis (93); Hypo, hypoglossal (29); Inf Oliv, inferior olive (63, obex; 104, open medulla); Inf Vest, inferior vestibular (98); Lat Cun, lateral cuneate (89); Lat Ret, lateral reticular formation (115, obex; 50, open medulla); NA, nucleus ambigus; NTS, nucleus of the tractus solitarius (107, obex; 89, open medulla); Sp Trig, spinal trigeminal (158, obex; 80, open medulla); Sp trig T, spinal trigeminal tract; Vag, vagus (36, obex; 42, open medulla).
For neuronal counts, each slide stained for DNA end-labeling was reviewed by two investigators, both ignorant of the diagnosis (SIDS or control brains). We studied all hippocampal subregions and the whole hemibrainstem on each slide. We examined the cells under a ×40 objective to ensure the presence of adequate staining, to permit differentiation between neuronal and nonneuronal cells, and to ascertain the morphologic characteristics of apoptosis and/or necrosis.
For the hippocampus, all neurons were counted in an area of each subregion at magnification ×10. We counted normal neurons (negative staining), positively stained neurons having the features of apoptosis, and positively stained neurons that could not be identified as apoptotic (damaged neurons, possibly by necrosis). The number of apoptotic neurons was expressed as a percentage of the total number of neurons. The cases were considered negative (physiologic apoptosis) if only rare neurons were positive (<1% positive cells). Normal and necrotic neurons on the HPS sections were counted and the number of necrotic neurons expressed as a percentage of the total number of neurons.
For the brainstem, we counted apoptotic neurons in the same way as for the hippocampus. For small, well-defined nuclei (nucleus tractus solitarius, nucleus of the spinal trigeminal tract, for instance), the whole nucleus was counted. For large nuclei (gracile and cuneate, for example), a region was chosen within each nucleus and at least 100 cells were counted.
We used the Mann-Whitney test for comparison between SIDS and control groups and for comparison between subgroups of SIDS victims. The Fisher exact test was used to compare proportions between different groups. p < 0.05 was considered significant.
The present study received approval from our Institutional Review Board. Permission to obtain information from all cases of sudden death was obtained from the Office of the Chief Coroner of the province and the Bureau d'Accès à l'information du Québec.
RESULTS
Neuronal apoptosis was found in 23 of the 29 SIDS victims (79%). Comparing SIDS cases that exhibited apoptosis with those that did not, we discerned no effects of age, sex, postmortem interval, or formalin-fixation duration. All cases were consistently identified as positive or negative by both observers. For positive cases, we elected to group the data in the following three categories: a) mild apoptosis, 1 to 9%; b) moderate apoptosis, 10 to 19%; and c) marked apoptosis, >20% of positive neurons. This was done because, when the data were examined, there was an apparent grouping into these three categories. Although some variability occurred in the results of percent positive neurons between observers, all cases ended up in the same categories when we grouped them as above.
No control cases were positive in the hippocampus (0/9 versus 15/27, p < 0.005, control versus SIDS), whereas three control cases were positive in the brainstem (3/7 versus 22/23, p = 0.006).
Hippocampus. Neuronal apoptosis in the hippocampus was found in 15 (55%) of the 27 SIDS victims for which a good section was available. The presence of apoptosis in the hippocampus correlated very well with the presence of necrosis (p < 0.001). In the SIDS cases, 13 of the 15 cases positive for apoptosis were also positive for necrosis. Two control cases displayed necrotic neurons but no apoptosis.
A clear regional distribution of apoptosis and necrosis was noted within the hippocampus (Table 1). The CA4 and subiculum subregions were most often involved in the apoptotic process and, in two cases, these subregions alone displayed positive findings. CA2 was least often involved (four cases) and, when involved, all other regions of the hippocampus were involved as well. This finding may suggest a somewhat more severe insult in these cases. As for necrosis, the subiculum, CA4, and CA1 were involved in the 13 positive SIDS cases, whereas other subregions were negative. In all cases, the number of neurons that had undergone apoptosis much exceeded the number that had undergone necrosis. Representative examples of apoptosis and necrosis are shown in Figures 3 and 4.
Hippocampus: (a) Normal neuron in CA1. (b) Necrotic neuron in CA1; compared with the normal neuron, the necrotic neuron is dense and retracted, its cytoplasm is eosinophilic, and the boundary between the nucleus and the cytoplasm is indistinct. (c) Cells with the morphologic features of apoptosis (arrow).
Brainstem. Neuronal apoptosis was present in 22 of the 23 SIDS cases (96%) for which a good section was available and in three of the control cases (all having died of bronchopneumonia or septicemia). Also, the brainstem showed a regional distribution of neuronal apoptosis, with the greatest number of positive nuclei in the dorsal (sensory) region. A representative example of apoptosis in the spinal trigeminal nucleus is shown in Figure 5. The data for each of the positive nuclei are presented in Table 2. Although three cases were positive for apoptosis in the control group, the distribution and degree of apoptosis differed from that of the SIDS victims (Table 2).
Neuronal apoptosis in temporary survivors. We studied the brainstem and hippocampus of four infants who were successfully resuscitated and survived temporarily for 6, 13, 24, and 96 h (organ donor), respectively. Neuronal apoptosis was present in both the brainstem and the hippocampus of two of these four infants (survival of 13 and 24 h) and in the hippocampus only in one infant (survival of 6 h). The infant who survived 96 h showed no apoptosis but rather a marked diffuse loss of neurons throughout both the brainstem and the hippocampus. The highest degree of apoptosis (>50% of neurons in each subregion of the hippocampus and in nuclei of the brainstem) was noted in the infants who survived 13 and 24 h. The pattern distribution of apoptosis in both the brainstem and hippocampus of the temporary survivors was similar to that of the other SIDS victims.
DISCUSSION
The degree of apoptosis found in the present study is very significant. Apoptosis in 2 to 3% of neurons can signify a cell regression rate of 25%/d (35). Therefore, the extent of apoptosis described in this study (often >20%) implies a high rate of cell death, with potential significant dysfunction in the affected brain regions of these infants.
The presence of both apoptotic and necrotic neurons in the hippocampus of our SIDS victims provides evidence of a serious insult at some time, probably within 24 to 48 h before death. The exact time of the insult is impossible to determine accurately. It could not have occurred less than 4 to 6 h before death because this is the earliest period during which necrosis-induced changes are observable by light microscopy (32,33). Yet, the interval between the insult and the nuclear changes characteristic of apoptosis could not have been much more than 24 h, because the initiation of apoptosis-induced changes must be underway by that point (16,28,34). In addition, the predominant involvement of specific hippocampal subregions also provides information on the time of the triggering event for both types of neuronal injury. After a hypoxemic-ischemic insult, the necrotic process in CA4 occurs within hours of the insult, but the involvement of CA1 is typically delayed, for up to 3 d in adults and less in immature subjects (19–21,36). Our finding in the infants who were resuscitated and survived temporarily seems to confirm the time of 24 to 48 h. Indeed, there was almost no apoptosis in the survivor of 6 h, a marked degree in the survivors of 13 and 24 h, and nothing but extensive cell loss in the survivor of 4 d.
It is impossible for us to assess the presence of previous apoptosis or enhanced apoptosis as a continuous slow process secondary to repeated insults in our group of SIDS victims. Once triggered, the apoptosis process is fast and cells can disappear in 24 h. Our technique identifies only recent apoptosis. Previous apoptosis can be evaluated solely by identifying significant neuronal loss in the regions of interest. In fact, neuronal loss evaluation in various brain regions requires volumetric counting of serial sections. One cannot evaluate the number of neurons properly in a single section because neuronal populations (especially in brainstem nuclei) are not always uniformly distributed throughout the brain and brainstem nuclei.
How does the present finding of neuronal apoptosis in the hippocampus and brainstem fit into the current hypotheses regarding the cause of SIDS? It is now clear that repeated, at times severe, hypoxemic and/or asphyxial episodes occur in infants who are at increased risk for SIDS (37). In accordance with the most widely accepted hypothesis on the pathology underlying SIDS, the repeated events are secondary to a brainstem dysfunction possibly resulting from an adverse intrauterine milieu or to events occurring postnatally (9,38–40). The brainstem is more sensitive to hypoxemic-ischemic injury in fetal and early postnatal life than later on (22,23), and the immature, in contrast with the adult, brain appears to respond to injury with apoptosis rather than with necrosis (24,41–43). Future SIDS victims may well have experienced repeated triggering for apoptosis and, eventually, significant dysfunction because of neuronal loss in the brainstem. For instance, neuronal loss has been reported in the arcuate nucleus in brainstems of SIDS victims (44), a region thought to be involved in control of respiration. Perhaps, then, damage occurred at critical stages of the development of cardiorespiratory control. Such damage will predispose to cardiorespiratory pattern abnormalities that, in turn, could cause the hypoxic-ischemic insult leading to apoptosis in other brain and brainstem areas, as found in the present study. We did find significant neuronal apoptosis in the nucleus of the tractus solitarius, a region involved in autonomic and respiratory control. However, it was impossible for us to assess precisely the degree of apoptosis in the arcuate nucleus. The arcuate nucleus is a thin band of cells located at the periphery of the brainstem, and peripheral regions are often positive with the method we used even though the nuclei of the neurons lack the features of apoptosis (possible nonspecific staining because of drying).
Our findings of predominant apoptosis in the vestibular and trigeminal nucleus in the brainstem could have important implications. The vestibular system mediates postural reflexes and information concerning the orientation of the head; the trigeminal system mediates cutaneous and proprioceptive sensations from skin, muscles, and joints in the face and mouth. Perhaps, then, a dysfunction at the level of the vestibular and trigeminal nuclei (because of repeated events that triggered apoptosis in those regions) is linked to the fact that prone sleeping is a major risk factor for SIDS (45–47). The prone sleeping position (especially when the face is turned into the mattress) has been shown to lead to hypoxemic and hypercapnic episodes (48,49). It is generally thought that normal infants should be able to turn or lift their heads to avoid asphyxia. However, we speculate that if infants have repeated damage to the system that controls sensation of the face and orientation of the head, suffocation may occur.
Another possibility is that SIDS victims, compared with normal infants, are vulnerable to apoptosis because of a relative deficiency of protective factors. The bcl family of protooncogenes, for instance, encodes, proteins that protect cells from apoptosis. Their expression changes during development in the newborn rat (50), and their expression also changes during fetal life in humans (51). We do not know the time course or mode of expression of bcl-xL (expressed in human brain) in postnatal life in humans, nor whether the exposure to repeated hypoxia could modify it. Interestingly, whereas hypoxemia-ischemia leads to substantial apoptosis in the hippocampus of neonatal mice (wild-type), the overexpression of bcl-xL (transgenic mice) is neuroprotective (52). The absence of apoptosis in the hippocampus of our control infants and in those who have died of cardiac disease (53) favors the hypothesis that SIDS victims are more vulnerable to apoptosis than are other infants. However, several brain regions should be examined before such a conclusion is definitively drawn; a study of the expression of promotors and/or suppressors of apoptosis should then be undertaken.
In summary, we report, in 79% of a group of SIDS victims, significant neuronal apoptosis in the brainstem and in subregions of the hippocampus known to be vulnerable to hypoxemic-ischemic insults. The event that triggered the apoptosis seems to have occurred several hours before death. This finding, coupled with the reported repeated hypoxemic episodes in SIDS victims before their death, suggests that those infants may have suffered repeated apoptosis resulting in significant neuronal damage and, thus, functional loss in key brain regions. Our findings may well constitute an important first step in understanding the pathogenesis of SIDS and the cause of death in such victims.
Abbreviations
- SIDS:
-
sudden infant death syndrome
- HPS:
-
hematoxylin-phloxine-saffron
References
Willinger M, James LS, Catz C 1991 Defining the sudden infant death syndrome (SIDS): deliberations of an expert panel convened by the National Institute of Child Health and Human Development. Pediatr Pathol 11: 677–681
Hunt CE 1992 The cardiorespiratory control hypothesis for sudden infant death syndrome. In: Hunt CE (ed) Apnea and SIDS. Clinics in Perinatology series. WB Saunders, Philadelphia, 757–771.
Gillan JE, Curran C, O'Reilly E, Seamus FC, Unwin AR 1989 Abnormal patterns of pulmonary neuroendocrine cells in victims of sudden infant death syndrome. Pediatrics 84: 828–834
Naeye RL 1974 Hypoxia and the sudden infant death syndrome. Science 186: 837–838
Rognum TO, Saugstad OD, Θyasæter S, Olaisen B 1988 Elevated levels of hypoxanthine in vitreous humor indicate prolonged cerebral hypoxia in victims of sudden infant death syndrome. Pediatrics 82: 615–618
Valdes-Dapena M, Gillane MM, Catherman R 1976 Brown fat retention in sudden infant death syndrome. Arch Pathol Lab Med 100: 547–549
Williams A, Vawter G, Reid L 1979 Increased muscularity of the pulmonary circulation in victims of sudden infant death syndrome. Pediatrics 63: 18–24
Del Bigio MR, Becker LE 1994 Microglial aggregation in the dentate gyrus: a marker of mild hypoxic-ischemic brain insult in human infants. Neuropathol Appl Neurobiol 20: 144–151
Kinney HC, Filiano JJ, Harper RM 1992 The neuropathology of the sudden infant death syndrome. J Neuropathol Exp Neurol 51: 115–126
Ferrer I, Tortosa A, Macaya A, Sierra A, Moreno D, Munell F, Blanco R, Squier W 1994 Evidence of nuclear DNA fragmentation following hypoxia-ischemia in the infant rat brain, and transient forebrain ischemia in the adult gerbil. Brain Pathol 4: 115–122
Mehmet H, Yue X, Squier MV, Lorek A, Cady E, Penrice J, Sarraf C, Wylezinska M, Kirkbride V, Cooper C 1994 Increased apoptosis in the cingulate sulcus of newborn piglets following transient hypoxia-ischemia is related to the degree of high energy phosphate depletion during the insult. Neurosci Lett 181: 121–125
Rosenbaum DM, Michaelson M, Batter DK, Doshi P, Kessler JA 1994 Evidence for hypoxia-induced, programmed cell death of cultured neurons. Ann Neurol 36: 864–870
Clarke PGH 1990 Developmental cell death: morphological diversity and multiple mechanism. Anat Embryol 181: 195–213
Wyllie AH 1980 Glucocorticoid-induced thymocyte apoptosis is associated with endogenous endonuclease activation. Nature 284: 555–556
Wyllie AH, Morris GG, Smith AL, Dunlop D 1984 Chromatin cleavage in apoptosis: association with condensed chromatin morphology and dependence on macromolecular synthesis. J Pathol 142: 67–77
Gavrieli Y, Sherman Y, Ben-Sasson SA 1992 Identification of programmed cell death in situ via specific labeling of nuclear DNA fragmentation. J Cell Biol 119: 493–501
Wijsman JH, Jonker YY, Keijzer R, Van de Velde CJH, Cornelisse CJ, Van Dierendonck JH 1993 A new method to detect apoptosis in paraffin sections: in situ end-labeling of fragmented DNA. J Histochem Cytochem 41: 7–12
Waters KA, Côté A 1996 Evidence for previous hypoxia in a population of infants dying from SIDS. Pediatr Res 39: 392A ( abstr)
Kirino T 1982 Delayed neuronal death in the gerbil hippocampus following ischemia. Brain Res 239: 57–69
Schmidt-Kastner R, Freund FF 1991 Selective vulnerability of the hippocampus in brain ischemia. Neuroscience 40: 599–616
Pulsinelli WA 1985 Selective neuronal vulnerability: morphological and molecular characteristics. Progr Brain Res 63: 29–37
Friede RL 1972 Ponto-subicular lesions in perinatal anoxia. Arch Pathol 94: 343–354
Mito T, Kamei A, Takashima S, Becker LE 1993 Clinicopathological study of pontosubicular necrosis. Neuropediatrics 24: 204–207
Yue X, Mehmet H, Penrice J, Cooper C, Cady E, Wyatt JS, Reynolds EO, Edwards AD, Squier MV 1997 Apoptosis and necrosis in the newborn piglet brain following transient cerebral hypoxia-ischemia. Neuropathol Appl Neurobiol 23: 16–25
Morioka T, Kalehua AN, Streit WJ 1991 The microglial reaction of the rat dorsal hippocampus following transient forebrain ischemia. J Cereb Blood Flow Metab 11: 966–973
Jorgensen MB, Finsen BR, Castellano B, Biemer NH, Zimmer J 1993 Microglial and astroglial reactions to ischemic and kainic acid-induced lesions of the adult rat hippocampus. Exp Neurol 120: 70–88
Gerhnann J, Bonnekoh P, Miyazawa T, Hossmann KA, Kreutzberg GW 1992 Immunocytochemical study of an early microglial activation in ischemia. J Cereb Blood Flow Metab 12: 257–269
Bursch W, Kleine L, Tenniswood M 1990 Biochemistry of cell death by apoptosis. Biochem Cell Biol 68: 1071–1074
Brown AW, Brierly JB 1968 The nature, distribution, and earliest stages of anoxic-ischaemic nerve cell damage in the rat brain as defined by the optical microscope. Br J Exp Pathol 49: 87–106
Auer RN, Benveniste H 1997 Hypoxia and related conditions. In: Graham DI, Lantos PL (eds) Greenfield's Neuropathology. Arnold, London, 263–314.
Eke A, Conger KA, Anderson M, Garcia JH 1990 Histologic assessment of neurons in rat models of cerebral ischemia. Stroke 21: 299–304
Kirino T, Sano K 1984 Fine structural nature of delayed neuronal death following ischemia in the gerbil hippocampus. Acta Neuropath 62: 209–216
Pulsinelli WA, Brierly JB, Plum F 1982 Temporal profile of neuronal damage in a model of transient forebrain ischemia. Ann Neurol 11: 491–498
Li Y, Chopp M, Jiang N, Yao F, Zaloga C 1995 Temporal profile of in situ DNA fragmentation after transient middle cerebral artery occlusion in the rat. J Cereb Blood Flow Metab 15: 389–397
Meyn RE 1994 Programmed cell death in normal development and disease. Cancer Bull 46: 120–124
Rice JE, Vannucci RC, Brierley JB 1981 The influence of immaturity on hypoxic-ischemic brain damage in the rat. Ann Neurol 9: 131–141
Poets CF, Samuels MP, Noyes JP, Hewertson J, Hartman H, Holder A, Southall DP 1993 Home event recordings of oxygenation, breathing movements, and heart rate and rhythm in infants with recurrent life-threatening events. J Pediatr 123: 693–701
Kinney HC, Burger PC, Harrell FE, Hudson RP 1983 'Reactive gliosis' in the medulla oblongata of victims of the sudden infant death syndrome. Pediatrics 72: 181–187
Summers GC, Parker VC 1981 The brainstem in the sudden infant death syndrome: a postmortem survey. Am J Forensic Med Pathol 2: 23–30
Takashima S, Armstrong D, Becker LE, Bryan C 1978 Cerebral hypoperfusion in the sudden infant death syndrome? Brainstem gliosis and vasculature. Ann Neurol 4: 257–262
Ferrer I, Tortosa A, Macaya A, Sierra A, Moreno D, Munell F, Blanco R, Squier W 1994 Evidence of nuclear DNA fragmentation following hypoxia-ischemia in the infant rat brain, and transient forebrain ischemia in the adult gerbil. Brain Pathol 4: 115–122
Scott RJ, Hegyi L 1997 Cell death in perinatal hypoxic-ischaemic brain injury. Neuropathol Appl Neurobiol 23: 307–314
Edwards AD, Yue X, Hope PL, Azzopardi DV, Squier MV, Mehmet H 1997 Apoptosis in the brains of infants suffering intrauterine cerebral injury. Pediatr Res 42: 684–689
Filiano JJ, Kinney HC 1992 . Arcuate nucleus hypoplasia in the sudden infant death syndrome. J Neuropathol Exp Neurol 51: 394–403
de Jonge GA, Burgmeijer RJF, Engelberts AC, Hoogenboezen J, Kortense PJ, Sprij AJ 1993 Sleeping position for infants and cot death in the Netherlands 1985-1991. Arch Dis Child 69: 660–663
Fleming PJ, Gilbert R, Azaz Y, Berry PJ, Rudd PT, Stewart A, Hall E 1990 Interaction between bedding and sleeping position in the sudden infant death syndrome: a population based case-control study. Br Med J 301: 85–89
Mitchel EA, Taylor BJ, Ford RPK, Stewart AW, Becroff DM, Thompson JM, Scragg R, Hassal IB, Barry DM, Allen EM, Roberts AP 1992 Four modifiable and major other risk factors for cot death: the New Zealand study. J Pediatr Child Health 28( suppl): S3–S8
Chiodini B, Thach BT 1993 Impaired ventilation in infants sleeping facedown: potential significance for sudden infant death syndrome. J Pediatr 123: 686–692
Waters KA, Gonzalez A, Jean C, Morielli A, Brouillette RT 1996 Face-straight-down and face-near-straight-down positions in healthy prone-sleeping infants. J Pediatr 128: 616–625
Ferrer I, Tortosa A, Condom E, Blanco R, Macaya A, Planas A 1994 Increased expression of bcl-2 immunoreactivity in the developing cerebral cortex of the rat. Neurosci Lett 179: 13–16
Yachnis AT, Powell SZ, Olmsted JJ, Eskin TA 1997 Distinct neurodevelopmental patterns of bcl-2 and bcl-x expression are altered in glioneuronal hamartias of the human temporal lobe. J Neuropathol Exp Neurol 56: 186–198
Parsadanian AS, Cheng Y, Keller-Peck CR, Holtzman DM, Snider WD 1998 Bcl-xL is an antiapoptotic regulator for postnatal CNS neurons. J Neurosci 18: 1009–1019
Gelbard HA, James HJ, Sharer LR, Perry SW 1995 Apoptotic neurons in brains from paediatric patients with HIV-1 encephalitis and progressive encephalopathy. Neuropathol Appl Neurobiol 21: 208–217
Acknowledgements
The authors thank Karim Ouallouche and Nancy Vézina for technical help, and Robert T. Brouillette and Immanuela R. Moss for their critical review of the manuscript.
Author information
Authors and Affiliations
Additional information
Supported in part by the Medical Research Council of Canada, The Montreal Children's Hospital Research Institute, and the local SIDS Foundation. K.A.W. was a research fellow at the Montreal Children's Hospital Research Institute. A.C. is a Research Scholar (Chercheur-Boursier) of the Fonds de la recherche en santé du Québec.
Rights and permissions
About this article
Cite this article
Waters, K., Meehan, B., Huang, J. et al. Neuronal Apoptosis in Sudden Infant Death Syndrome. Pediatr Res 45, 166–172 (1999). https://doi.org/10.1203/00006450-199902000-00002
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199902000-00002
This article is cited by
-
Cell death in the lateral geniculate nucleus, and its possible relationship with nicotinic receptors and sudden infant death syndrome (SIDS)
Molecular Neurobiology (2023)
-
The Unfolded Protein Response in the Human Infant Brain and Dysregulation Seen in Sudden Infant Death Syndrome (SIDS)
Molecular Neurobiology (2021)
-
The α7 and β2 nicotinic acetylcholine receptor subunits regulate apoptosis in the infant hippocampus, and in sudden infant death syndrome (SIDS)
Apoptosis (2020)
-
Cell death in the human infant central nervous system and in sudden infant death syndrome (SIDS)
Apoptosis (2019)
-
Neuronal apoptosis in the brainstem medulla of sudden unexpected death in infancy (SUDI), and the importance of standardized SUDI classification
Forensic Science, Medicine and Pathology (2018)