Abstract
Acid α-glucosidase (GAA) deficiency causes Pompe disease, a lethal lysosomal glycogen storage disease for which no effective treatment currently exists. We investigated the endocytic process in deficient cells of human recombinant GAA produced in Chinese hamster ovary cells, and the potential of GAA-deficient Japanese acid maltase-deficient quail as a model for evaluating the enzyme replacement therapy for Pompe disease. After 24-h incubation with a single dose of recombinant enzyme, intracellular GAA and glycogen levels in deficient human fibroblasts were normalized, and this correction lasted for 7 d. The 110-kD precursor recombinant enzyme was processed to the 76-kD mature form within 24 h after uptake. Intracellular GAA levels in deficient quail fibroblasts and myoblasts were similarly corrected to their average normal levels within 24 h. Differences existed in the efficiency of endocytosis among subfractions of the enzyme, and among different cell types. Fractions with a larger proportion of precursor GAA were endocytosed more efficiently. Quail fibroblasts required a higher dose, 4200 nmol·h-1·mL-1 to normalize intracellular GAA levels than human fibroblasts, 1290 nmol·h-1·mL-1, whereas primary quail myoblasts required 2800 nmol·h-1·mL-1. In all three cell lines, the endocytosed enzyme localized to the lysosomes on immunofluorescence staining, and the endocytosis was inhibited by mannose 6-phosphate (Man-6-P) added to the culture medium. Despite structural differences in Man-6-P receptors between birds and mammals, these studies illustrate that Man-6-P receptor mediated endocytosis is present in quail muscle cells, and demonstrate the potential of acid maltase-deficient quail to test receptor mediated enzyme replacement therapy for Pompe disease.
Similar content being viewed by others
Main
GAA (EC 3.2.1.20) is synthesized as a 110-kD precursor enzyme that matures through a 95-kD endosomal intermediate into 76- and 67-kD mature lysosomal enzymes(1–4). This enzyme catalyzes the hydrolysis of both the α-1,4- and the α-1,6-glycosidic bonds of glycogen(5). In Pompe disease (glycogen storage disease type II), deficiency of GAA activity causes lysosomal glycogen accumulation, leading to disruption of cellular functions(5). Patients with the most common infantile form of Pompe disease have extremely low (<1%) GAA activity, and present with a progressive myopathy and hypertrophic cardiomyopathy leading to death before age 2 y(5). Patients with juvenile and adult forms present with progressive skeletal muscle weakness and are characterized biochemically by residual GAA activity.
Currently, there is no effective treatment for Pompe disease. Initial attempts of enzyme replacement therapy using purified GAA from human placenta or Aspergillus niger normalized the GAA and glycogen levels in liver, but not in muscle and heart of patients with Pompe disease, presumably due to the absence of Man-6-P groups in those enzyme preparations(6–9). To achieve therapeutic success, exogenous GAA must target the affected organs. Endocytosis of exogenous GAA mediated by Man-6-P present on the precursor enzyme, and by Man-6-P receptors on the cell membrane of muscle cells resulted in greatly improved uptake into the lysosomes by the deficient cells(10). After i.v. injection in mice of such Man-6-P-rich GAA isolated from bovine testis, there was noticeable uptake of the enzyme in heart and muscle due to the abundance of Man-6-P receptors in these organs(11).
Recently production of large quantities of recombinant human GAA produced by transfected Chinese hamster ovary cells, and purification of this enzyme from culture medium has become available(12, 13). Endocytosis of this precursor enzyme by cultured fibroblasts from patients with infantile Pompe disease was blocked by Man-6-P, indicating that Man-6-P receptor mediated uptake of the enzyme. After i.v. injection in a guinea pig of the precursor recombinant human GAA, increased enzyme levels were observed in liver and heart(12).
To study the efficacy of this new enzyme replacement therapy by Man-6-P receptor-targeted enzyme uptake, an appropriate animal model is needed. The only reported living animals with GAA deficiency are Shorthorn cattle(14, 15), Brahman cattle(16), and a strain of Japanese quails(17, 18). Because cattle are too large for therapeutic experimentation with limited recombinant enzyme, Japanese AMD quail is at present the only practical animal model. Generalized glycogen accumulation becomes evident on histology at 4 wk after hatching, and precedes the progressive muscle weakness that presents at 6 wk after hatching(19–21). The disease in AMD quails resembles the adult form of Pompe disease in humans in its late onset, the presence of residual GAA activity, and the histologic changes in affected muscles(19–21). The cation-independent Man-6-P receptor, which is primarily responsible for receptor-mediated endocytosis of exogenous GAA, also has IGF II binding activity in mammals, but not in birds(22, 23). This difference in Man-6-P receptors raised questions on the suitability of the AMD quail is as a model for studying Man-6-P receptor mediated enzyme replacement therapy.
In this study, we investigated the kinetics of Man-6-P receptor-mediated endocytosis of precursor GAA in cultured fibroblasts from patients with infantile Pompe disease, and the fate of this enzyme after endocytosis. Furthermore, by comparative study of endocytosis of the recombinant GAA and its fate in both cultured fibroblasts and myoblasts from AMD quails, we investigated the potential of the AMD quail as an animal model for evaluating enzyme replacement therapy of Pompe disease through Man-6-P receptor-mediated endocytosis.
METHODS
Materials. DMEM, minimum essential medium, FCS, chicken serum, and chick embryo extract were purchased from Life Technologies (Gaithersburg, MD). Conalbumin (chicken transferrin), horse serum, Cy3-conjugated sheep anti-rabbit IgG, FITC-conjugated goat anti-guinea pig IgG, DAPI, amyloglucosidase, Man-6-P, and 4-methylumbelliferone and its derivatives were obtained from Sigma Chemical Co. (St. Louis, MO). Tissue culture plates and dishes precoated with rat tail collagen type I were purchased from Collaborative Biomedical Products (Bedford, MA). The reagent for glucose was from Roche Diagnostic System (Nutley, NJ). Enhanced chemiluminescence detection reagents for Western blot were from Amersham Life Science(Cleveland, OH). Antiserum was raised in guinea pigs against purified recombinant human GAA and in rabbits against purified human placental GAA.
Enzyme assays. Enzyme activities of acid and neutralα-glucosidase were assayed in a 96-well microtiter plate using 4-methylumbelliferone-α-D-glucoside at pH 4.3 and 6.7, respectively(24). Acid β-galactosidase was similarly assayed using respective 4-methylumbelliferyl β-galactosidase(25). The glycogen content of fibroblasts was assayed by the release of glucose after digestion of boiled cell lysate with Aspergillus niger amyloglucosidase. The released glucose was measured using a COBAS FaraII centrifugal analyzer from Roche Diagnostic System (Nutley, NJ) to follow the absorbance or the fluorescence of NADH generated by a linked enzymatic assay with glucokinase and glucose-6-phosphate dehydrogenase(12). Total protein concentration was determined according to the Bradford(26) method.
Production and evaluation of recombinant human GAA. Recombinant human GAA was produced by transformed Chinese hamster ovary cells and purified from the culture medium using a concanavalin-Sepharose 4B column, followed by affinity chromatography on a Sephadex G-200 column(12). Early eluting fractions from the Sephadex column contained more precursor recombinant human GAA, late eluting fractions had an increasing contribution of mature enzyme(12). Each batch of purified enzyme was analyzed for specific enzyme activity and by Coomassie staining after SDS-PAGE gel electrophoresis for purity. The recombinant human GAA used for time and dose response curves of uptake in the GAA-deficient cells was of >90% purity of the precursor enzyme and contained at least 250μmol·h-1·mg-1 of protein specific GAA activity.
Tissue culture. Human diploid fibroblasts were established from skin biopsies from patients with infantile Pompe disease and from normal controls, and maintained in minimum essential medium with 10% FCS. Quail fibroblasts and myoblasts were established from skin and pectoral muscles of 9-d embryos of AMD quails and unaffected controls, respectively. At this age pathologic glycogen accumulation is present in all quail tissues(19). Quail fibroblasts were maintained in DMEM with 4.5 g/L glucose supplemented by 10% FCS, 2% chicken serum, and 30 μg/mL conalbumin. Primary quail myoblasts were preplated for 30 min to select against the outgrowth of fibroblasts, then explanted into 35-mm collagen-coated tissue culture plates, and grown in growth medium containing DMEM with 20% FCS and 0.5% chick embryo extract. One day later, the medium was changed to fusion medium that contained DMEM with 0.5% chick embryo extract, 2% horse serum, and 30 μg/mL conalbumin(27, 28). To eliminate interference of endogenous GAA present in the serum, all sera were incubated at 56 °C and pH 10 for 1 h before use(2).
Uptake experiments. Both deficient cells and normal controls were subcultured onto 35-mm well plates at a similar cell density of 105 cells/mL. Uptake experiments were started in deficient human and quail fibroblasts 1 d after attaining confluence, and in deficient quail myoblasts 1 d after the majority of cells differentiated into multinuclear myotubes. Immediately before each uptake experiment, an aliquot of recombinant human GAA was added into fresh culture medium, the medium was filter-sterilized, and assayed for final GAA activity. Deficient cells were incubated with this medium for 24 h, or a specified period of time. Normal control cells and sham-treated deficient cells were maintained in parallel in medium without added recombinant human GAA. All experiments were done in triplicates with differences less than 20%. After the uptake, fibroblasts from both human and quail were harvested by scraping after washing with PBS, whereas quail myoblasts were harvested by a brief trypsinization, followed by washing with PBS. After centrifugation, cell pellets were resuspended in cold deionized water, sonicated, and the supernatant was used for assay of GAA enzyme activity, glycogen content, and protein concentration. The processing of the recombinant precursor enzyme after uptake was analyzed by SDS-PAGE, Western blotting, incubation with 1:5000 rabbit anti-human GAA antiserum, followed by incubation with 1:10 000 horse radish peroxidase-coupled goat anti-rabbit IgG, and detection by chemoluminescence.
Immunofluorescence staining. The intracellular localization of recombinant GAA in deficient fibroblasts and myoblasts after endocytosis was analyzed by immunofluorescence staining. Fibroblasts of human and AMD quail were grown on sterilized glass slides, and uptake of recombinant GAA for 24 h was started in the deficient cells when they reached 70% confluence, allowing observation in individual cells. Unlike the fibroblasts, primary myoblasts from AMD and normal control quails were maintained in growth medium on collagen-coated plates for 1 d, then subcultured to grow on sterilized noncollagen-coated glass slides the next day. In the following 3 d, cells were maintained in fusion medium to induce differentiation of myoblasts into myotubes. When the majority of cells had a multinucleated myotubular morphology indicating complete differentiation, a 24-h uptake experiment was started by adding recombinant human GAA to DMEM medium with 10% chicken serum and 30 μg/mL conalbumin.
After uptake, cells on each glass slide were washed with PBS buffer and fixed by incubating with 2% formaldehyde in PBS at room temperature for 45 min. Before each incubation with antibodies, cells were incubated with 0.1% Saponin, 1% goat serum in PBS for 4 min at room temperature, and washed with PBS. Double stained cells were incubated first for 3 h at room temperature with the first primary antibody, and then incubated overnight at 4 °C with the second primary antibody. The next day, cells were separately incubated for 3 h each with both secondary antibodies conjugated with FITC and CY3, respectively, then counterstained with DAPI, and mounted with 0.5%n- propyl gallate in glycerol for detection by fluorescence microscopy and photography. Primary antibodies used were antiserum raised in rabbits to Purified human placental GAA, antiserum raised in guinea pigs to purified recombinant human GAA, and antiserum raised in rabbits against recombinant human α-L-iduronidase (EC 3.2.1.76). Myocytes and myotubes were identified with antibodies raised in mouse against chicken myoblast plasma membrane glycoprotein (Hybridoma Bank, Iowa city, IA).
RESULTS
Uptake Experiment in Deficient Human Fibroblasts
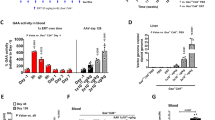
Kinetics of the uptake. Intracellular GAA activity in cultured normal human fibroblasts averaged 255 nmol·h-1·mg-1 of protein (66-489 nmol·h-1·mg-1; n = 22), whereas the levels in cultured fibroblasts from two patients with infantile Pompe disease were undetectable. When deficient human fibroblasts were incubated with 1000 nmol·h-1·mL-1 precursor recombinant human GAA, a time response curve showed normalization of the intracellular GAA level in less than 24 h (Fig. 1A). The increase in intracellular GAA levels in the deficient fibroblasts over time was paralleled by a decrease of enzyme levels in the culture medium. The dose response of 24-h uptake of recombinant human GAA in these deficient cells was saturable suggesting receptor mediated uptake. Within 24 h, correction of intracellular GAA level in deficient human fibroblasts to the average of normal control cells was attained using a single dose of 1290 nmol·h-1·mL-1(Fig. 1B). The endocytosis of recombinant GAA and correction of deficient human fibroblasts were inhibited >99% by addition of 1 mM Man-6-P to the recombinant human GAA-containing medium.
Uptake efficiency of subfractions of purified recombinant GAA. After each purification through Sephadex G-200 column, the recombinant human GAA was divided into four fractions as previously described(12). The early eluting fractions contained higher proportions of a 110-kD precursor enzyme, and the later eluting fractions contained more 95- and 76-kD mature enzymes. When deficient human fibroblasts were incubated for 24 h with 1000 nmol·h-1·mL-1 of recombinant human GAA from each fraction of purified enzyme, the early eluting fraction were endocytosed more efficiently than the later eluting fractions. The median of increased intracellular enzyme levels after uptake were 454(n = 3), 349 (n = 5), 290 (n = 5), and 247(n = 4) nmol·h-1·mg-1 of protein for fractions 1 to 4, respectively (p = 0.02, Kruskal-Wallis). To achieve comparative analysis of the uptake kinetics in different deficient cell lines, fractions 1 and 2 from successive purification batches were pooled together and used for all subsequent uptake experiments.
Evolution of GAA and glycogen levels after uptake endocytosis of recombinant GAA. To study therapeutic efficacy of a single dose of recombinant GAA in cultured deficient human cells, patient fibroblasts were incubated with medium containing 2000 nmol·h-1·mL-1 of recombinant human GAA for 24 h, and intracellular GAA and glycogen levels were followed thereafter for 10 d. Intracellular GAA activity in the deficient cells increased to above the average level of normal human fibroblasts at the end of the uptake, then the level fell rapidly in 1 d to equivalent of the average level of normal human fibroblasts, where it remained until the 7th d after uptake. Finally it declined to 90 nmol·h-1·mg-1 of protein on the 10th d (Fig. 2A). Glycogen levels in patient fibroblasts were normalized 2 d after the uptake and this correction was maintained until the 7th d after the uptake (Fig. 2B). Thereafter, the intracellular glycogen level increased concomitantly with the decline of intracellular GAA activity.
Evolution of intracellular enzyme and glycogen levels after incubation of human fibroblasts with recombinant GAA. After 24-h incubation with 2000 nmol·h-1·mL-1 of recombinant GAA, deficient cells were maintained in medium without added recombinant GAA, and intracellular GAA and glycogen levels followed for 10 d. Results from two deficient human fibroblast cell lines are shown as ▪ and ⋄, respectively.
Fate of recombinant enzyme after endocytosis. Because glycogen accumulates primarily in the lysosomes in Pompe disease, the administered recombinant human GAA should localize to the lysosomes to achieve therapeutic efficacy. Immunofluorescent staining was performed to study the intracellular localization of human GAA in normal cells and recombinant GAA after it was endocytosed by deficient cells. In normal human fibroblasts, staining with antiserum against human GAA showed a perinuclear punctate pattern typical of a lysosomal distribution (Fig. 3A), colocalizing with that of α-L-iduronidase (Fig. 3B). This finding was absent in deficient human fibroblasts (not shown). After these deficient cells were incubated for 24 h with 1000 nmol·h-1·mL-1 of recombinant human GAA, immunofluorescent staining showed a perinuclear punctate pattern similar to that seen in normal control human fibroblasts (Fig. 3C). This lysosomal localization was further confirmed by colocalization upon dual staining with antiserum against human lysosomal α-L-iduronidase (Fig. 3D).
Immunofluorescent staining of recombinant GAA in human fibroblasts. Normal control human fibroblasts were dual stained with antiserum raised in guinea pigs against human recombinant GAA detected with FITC-conjugated goat anti-guinea pig antibodies (A) and antiserum raised in rabbit against recombinant human lysosomal α-L-iduronidase detected with Cy3 conjugated sheep anti-rabbit IgG (B), demonstrating intracellular colocalization in a perinuclear punctate pattern typical of a lysosomal distribution. The nuclei are visible by counterstaining with DAPI. After 24-h incubation of deficient human fibroblasts with recombinant GAA, lysosomal distribution of endocytosed GAA is demonstrated by similar staining of human GAA (FITC, in C) and colocalization with human lysosomal α-L-iduronidase (Cy3, in D).
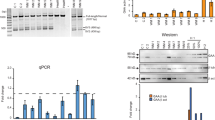
The molecular processing of the 110-kD precursor recombinant human GAA after endocytosis by deficient fibroblasts was studied by Western blot analysis (Fig. 4). Normal human fibroblasts showed a prominent band at 76 kD, and minor bands at 95 and 67 kD. Patient fibroblasts did not show any enzyme band. After 24-h incubation with exclusively 110-kD precursor recombinant human GAA, patient fibroblasts showed a major band at 76 kD similar to the mature enzyme, and minor bands at 95 and 67 kD, indicating normal maturation of the precursor recombinant enzyme after endocytosis.
Molecular processing of GAA in human fibroblasts. Western blot analysis of molecular processing of 110-kD precursor GAA after 24-h incubation of this enzyme with deficient human fibroblasts. Ur, GAA purified from human urine; E1 and E2, purified recombinant GAA;P, deficient human fibroblasts only; P+E2, deficient human fibroblasts treated with recombinant human GAA; C, normal control human fibroblasts; C+E2, normal control fibroblasts treated with recombinant human GAA.
Uptake Experiments in AMD Quail Fibroblast and Myoblasts
Kinetics of the uptake. Intracellular GAA level in the cultured AMD quail fibroblasts averaged 9.3 nmol·h-1·mg-1 of protein, which was 25% of the average level in normal control quail fibroblasts of 36.8 nmol·h-1·mg-1 of protein. In the cultured AMD quail myoblasts, intracellular GAA levels were lower than in fibroblasts and averaged 6.3 nmol·h-1·mg-1 of protein, 38% of the average level of normal control quail myoblasts 16.4 nmol·h-1·mg-1 of protein. The dose-response curves of uptake of the recombinant enzyme in both AMD fibroblasts and AMD myoblasts showed a similar saturating pattern (Fig. 5). After an incubation with medium containing recombinant human GAA for 24 h, intracellular GAA levels in AMD quail fibroblasts and myoblasts were corrected to their average normal control levels with 4200 and 2800 nmol·h-1·mL-1 of recombinant enzyme, respectively. This uptake of recombinant enzyme by both AMD fibroblasts and myoblasts was inhibited by the presence of 5 mM Man-6-P during the incubation for uptake.
Immunofluorescence staining. With antiserum raised in rabbits against human placental GAA, neither Western blot nor immunofluorescence staining of AMD and normal quail fibroblasts and myoblasts showed a detectable signal, indicating that this antiserum against human GAA does not cross-react with quail GAA. After the AMD quail fibroblasts were incubated for 24 h with 2000 nmol·h-1·mL-1 of recombinant human GAA, staining with the same antiserum showed a typical lysosomal perinuclear punctate pattern (Fig. 6B). A similar pattern, but of less intensity, was observed in the myoblasts and myotubes after endocytosis, presumably due to lower levels of GAA activity in muscle cells than in fibroblasts (Fig. 6C). Myotubes were identified from contaminating fibroblasts by the multinucleated pattern shown by counterstaining with DAPI. Myotubes and myoblasts were further identified by immunostaining with antibodies against chicken myoblast plasma membrane glycoprotein (Fig. 6D).
Immunofluorescence staining of AMD fibroblasts and myotubes after uptake of recombinant human GAA. AMD fibroblast, without enzyme treatment (A). After 24-h incubation with 2000 nmol·h-1·mL-1 of recombinant human GAA, endocytosed human GAA was detected by antiserum raised in rabbit against human placental GAA and detected by FITC-conjugated anti-rabbit IgG in a lysosomal perinuclear punctate pattern in the AMD quail fibroblasts (B), and, of less intensity, in the myoblasts and myotubes (C). Myoblasts and myotubes were recognized by immunostaining with mouse anti-chicken myoblast plasma membrane glycoprotein antibodies detected with Cy3 conjugated anti-mouse IgG (D), and by the multinucleated pattern shown by counterstaining of the nuclei with DAPI.
DISCUSSION
For enzyme replacement therapy in Pompe disease to be successful, the enzyme must be taken up in the lysosomes of cells of affected organs, particularly in muscle and heart. The recombinant enzyme produced by the Chinese hamster ovary cells is endocytosed through the Man-6-P receptor, as indicated by the near complete inhibition with addition of Man-6-P to the medium. The endocytosis process is complete in 24 h. After endocytosis, the enzyme localized to the lysosomes, as demonstrated by immunofluorescence. The precursor recombinant enzyme is less active toward the natural substrate and has a lower Vmax than the natural mature enzyme(3, 12). Yet, this precursor enzyme was a similarly therapeutically effective enzyme, because complete processing from 110 kD to mature 76 kD occurred after endocytosis, and the enzyme normalized glycogen levels. This maturation subsequent to endocytosis also indicates that proteolytic processing occurs in the endosome or lysosome, and is not limited to the Golgi apparatus(3).
Dose-response studies can provide initial dosing guidelines for in vivo studies. The dose required for the correction of deficient cells is dependent on the efficiency of receptor-mediated endocytosis. The efficiency of receptor-mediated endocytosis depends on the ligand structure, and on the receptor density and affinity, both characteristics of the cell type. Structural heterogeneity was previously described in recombinant GAA, with early eluting fractions of the Sephadex column containing more precursor enzyme. These early eluting fractions were endocytosed more efficiently, indicating that these precursor-rich fractions contain more Man-6-P rich enzyme. It illustrates the biologic relevance of the microheterogeneity of purified recombinant enzyme. Sephadex chromatography does not allow complete separation of fractions characterized by these differences in endocytosis efficiency. A more robust separation procedure will be advantageous to achieve reproducible biologic strength. Dose response studies indicate that a single dose of 1290 nmol·h-1·mL-1 of recombinant GAA provides full correction of deficient human fibroblasts. Because in vivo the recombinant enzyme must distribute in the extracellular fluid, and given the assumption that all cells would behave similar to fibroblasts, a dose of 320 μmol·h-1·kg-1 should be sufficient for full correction. In the whole animal, however, cells with receptors other than Man-6-P, in particular mannose receptors in macrophages of liver, lung, and spleen, will compete for the enzyme. Therefore, the required dose can be expected to be substantially higher. After in vitro endocytosis, normal enzyme and glycogen levels were maintained for one week. This suggests that weekly dosing will be sufficient to maintain correction, similar to findings in enzyme replacement therapy of other lysosomal storage conditions(29–32).
To evaluate therapeutic biologic efficacy, the therapy has to be studied in an animal model. The AMD Japanese quail provides such a model, with late onset symptoms allowing sufficient survival for the recognition of biologic response. The efficient in vitro endocytosis of human recombinant GAA, which is blocked by Man-6-P, indicates that Man-6-P receptor mediated enzyme replacement is possible despite structural differences of the Man-6-P receptor between birds and mammals(22, 23). Dosage studies indicate that the dose required for complete normalization of cultured deficient fibroblasts in the quail (4250 nmol·h-1·mL-1) is 3.3 times higher than in human fibroblasts. Even though fibroblasts from human and quail were maintained in different media, using identical media during the uptake experiment provided similar results as described.
Correction of myoblast culture was more efficient than fibroblasts. Immunofluorescence study confirmed uptake of the enzyme not only in myoblasts but also in fully differentiated myotubes. Increased expression of the combined IGF-II cation-independent Man-6-P receptor with differentiation of myoblasts into myotubes had been noted previously in mouse C2 cells, but has not been confirmed in birds(33). Because the distribution of the cation-independent Man-6-P receptor in birds is not well characterized, the finding of efficient uptake in myotubes indicates the potential for localization of the recombinant enzyme after i.v. injection to muscle in this species. The absence of cross-reactivity of the antiserum against the human recombinant enzyme with the residual natural enzyme in the quail will allow unambiguous detection of the administered human enzyme in the quail organs. These data demonstrate the potential of the Japanese AMD quail for the study on the efficacy of recombinant enzyme replacement therapy in Pompe disease.
Abbreviations
- GAA:
-
acid α-glucosidase
- Man-6-P:
-
mannose 6-phosphate
- AMD:
-
acid maltase deficient
- DMEM:
-
Dulbecco's modified Eagle medium with high glucose
- DAPI:
-
4,6-diamidino-2-phenylindole
References
Hoefsloot LH, Hoogeveen-Westerveld M, Kroos MA, van Beeumen J, Reuser AJJ, Oostra BA 1988 Primary structure and processing of lysosomal -glucosidase; homology with the intestinal sucrase-isomaltase complex. EMBO J 7: 1697–1704
Hoefsloot LH, Willemsen R, Kroos MA, Hoogeveen-Westerveld M, Hermans MMP, Van der Ploeg AT, Oostra BA, Reuser AJJ 1990 Expression and routing of human lysosomal -glucosidase in transiently transfected mammalian cells. Biochem J 272: 485–492
Wisselaar HA, Kroos MA, Hermans MMP, van Beeumen J, Reuser AJJ 1993 Structural and functional changes of lysosomal acid-glucosidase during intracellular transport and maturation. J Biol Chem 268: 2223–2231
Hermans MMP, Wisselaar HA, Kroos MA, Oostra BA, Reuser AJJ 1993 Human lysosomal I-glucosidase: functional characterization of the glycosylation sites. Biochem J 289: 681–686
Hirschhorn R 1995 Glycogen storage disease type II: acidα-glucosidase (acid maltase) deficiency In: Scriver CR, Beaudet AL, Sly WS, Valle D (eds) The Metabolic and Molecular Basis of Inherited Disease, 7th Ed. McGraw-Hill, New York, pp 2443–2464
de Barsy T, Van Hoof F 1974 Enzyme replacement therapy with purified human acid I-glucosidase in type II glycogenosis In: Tager JM, Hooghwinkel GJM, Daems WT (eds) Enzyme Replacement Therapy in Lysosomal Storage Diseases. North-Holland, Amsterdam, pp 277–279
Hug G, Schubert WK 1967 Lysosomes in type II glycogenosis. J Cell Biol 35:C1–C6
de Barsy T, Jacquemin P, Van Hoof F, Hers Henri-G 1973 Enzyme replacement in Pompe disease: an attempt with purified human acid I-glucosidase. Birth Defects Orig Art Ser 9: 184–190
Hug G, Schubert WK 1967 Hepatic lysosomes in Pompe's disease: disappearance during glucosidase administration. J Clin Invest 46: 1073–1073
Van der Ploeg AT, Loonen MCB, Bolhuis PA, Busch HMF, Reuser AJJ, Galjaad H 1988 Receptor-mediated uptake of acidα-glucosidase corrects lysosomal glycogen storage in cultured skeletal muscle. Pediatr Res 24: 90–94
Van der Ploeg AT, Kroos MA, Willemsen R, Brons NHC, Reuser AJJ 1991 Intravenous administration of phosphorylated acid-glucosidase leads to uptake of enzyme in heart and skeletal muscle of mice. J Clin Invest 87: 513–518
Van Hove JLK, Yang HW, Wu Jer-Y, Brady RO, Chen Yuan-T 1996 High level production of recombinant human lysosomal acid α-glucosidase in Chinese hamster ovary cells which targets to heart muscle and corrects glycogen accumulation in fibroblasts from patients with Pompe disease. Proc Natl Acad Sci USA 93: 65–70
Fullar M, Van Der Ploeg A, Reuser AJJ, Anson DS, Hopwood JJ 1996 Isolation and characterization of a recombinant precursor form of lysosomal acid α-glucosidase. Eur J Biochem
Richards RB, Edwards JR, Cook RD, White RR 1977 Bovine generalized glycogenosis. Neuropathol Appl Neurobiol 3: 45–56
Howell JMcC, Dorling PR, Cook RD, Robinson WF, Bradley S, Gawthorne JM 1981 Infantile and late onset form of generalised glycogenosis type II in cattle. J Pathol 134: 267–277
O'Sullivan BM, Healy PJ, Fraser RE, Nieper RE, Whittle RJ, Sewell CA 1981 Generalized glycogenosis in Brahman cattle. Aust Vet J 57: 227–229
Murakami H, Takagi A, Nonaka S, Ishiura S, Sugita H, Mizutani 1980 Glycogenosis II in a Japanese quail. Exp Anim 29: 475–485
Murakami H, Takagi A, Nonaka I, Ishiura S, Sugita H, Mizutani M 1982 Type 2 glycogen storage disease in Japanese quails. In: Ebashi S (ed) Muscular Dystrophy. University of Tokyo Press, Tokyo, pp 37–48
Miyagawa-Tomita S, Morishima M, Nakazawa M, Mizutami M, Kikuchi T 1996 Pathological study of Japanese quail embryo with acid α-glucosidase deficiency during early development. Acta Neuropathol 92: 249–254
Higuchi I, Nonaka I, Usuki F, Ishiura S, Sugita H 1987 Acid maltase deficiency in the Japanese quail; early morphological event in skeletal muscle. Acta Neuropathol 73: 32–37
Fujita T, Nonaka I, Sugita H 1991 Japanese quail and human acid maltase deficiency: a comparative study. Brain Dev 13: 247–255
Canfield WM, Kornfeld S 1989 The chicken liver cation-independent mannose 6-phosphate receptor lacks the high affinity binding site for insulin-like growth factor II. J Biol Chem 264: 7100–7103
Yang YW-H, Robbins AR, Nissley SP, Rechler M 1991 The chick embryo fibroblast cation-independent mannose 6-phosphate receptor is functional and immunologically related to the mammalian insulin-like growth factor-II (IGF-II)/Man 6-P receptor but does not bind IGF-II. Endocrinology 128: 1177–1189
Reuser AJJ, Koster JF, Hoogeveen A, Galjaard H 1978 Biochemical, immunological, and cell genetic studies in glycogenosis type II. Am J Hum Genet 30: 132–143
Wenger DA, Williams C 1991 Screening for lysosomal disorders In: Hommes FA (ed) Techniques in Diagnostic Human Biochemical Genetics. A Laboratory Manual. Wiley-Liss, New York, pp 587–617
Bradford MM 1976 A rapid and sensitive method for the quantitation of microgram quantities of protein using the principle of protein-dye binding. Anal Biochem 72: 248–254
Blau HM, Webster C 1981 Isolation and characterization of human muscle cells. Proc Natl Acad Sci USA 78: 5623–5627
Hagiwara Y, Saito K, Atsumi S, Ozawa E 1987 Iron supports myogenic cell differentiation to the same degree as does iron-bound transferrin. Dev Biol 120: 236–244
Barton NW, Furbish FS, Murray GJ, Garfield M, Brady RO 1990 Therapeutic response to intravenous infusions of glucocerebrosidase in a patient with Gaucher disease. Proc Natl Acad Sci USA 87: 1913–1916
Vogler C, Sands M, Higgins A, Levy B, Grubb J, Brikenmeier EH, Sly WS 1993 Enzyme replacement with recombinant β-glucuronidase in the newborn mucopolysaccharidosis type VII mouse. Pediatr Res 34: 837–840
Sands MS, Vogler C, Kyle JW, Grubb JH, Levy B, Galvin N, Sly WS, Birkenmeier EH 1994 Enzyme replacement therapy for murine mucopolysaccharidosis type VII. J Clin Invest 93: 2324–2331
Shull RM, Kakkis ED, McEntee MF, Kania SA, Jonas AJ, Neufeld EF 1994 Enzyme replacement in a canine model of Hurler syndrome. Proc Natl Acad Sci USA 91: 12937–12941
Tollefsen SE, Sadow JL, Rotwein P 1989 Coordinate expression of insulin-like growth factor II and its receptor during muscle differentiation. Proc Natl Acad Sci USA 86: 1543–1547
Acknowledgements
The authors thank Letealia Oliver, Alice Chen, and Xi Zhang for technical assistance. Antiserum against recombinant humanα-L-iduronidase was a gift of E. Kakkis, M.D., Ph.D. (Harbor University of California, Los Angeles Medical Center, Torrance, CA).
Author information
Authors and Affiliations
Additional information
Supported by a grant from the Muscular Dystrophy Association and a grant gift from Synpac Pharmaceuticals Ltd.
Rights and permissions
About this article
Cite this article
Yang, H., Kikuchi, T., Hagiwara, Y. et al. Recombinant Human Acid α-Glucosidase Corrects Acidα-Glucosidase-Deficient Human Fibroblasts, Quail Fibroblasts, and Quail Myoblasts. Pediatr Res 43, 374–380 (1998). https://doi.org/10.1203/00006450-199803000-00011
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199803000-00011