Abstract
Primary carnitine deficiency is associated with deficient blood and tissue carnitine concentrations. The clinical syndrome is dominated by heart and skeletal muscle symptoms, and the clinical response to oral carnitine supplementation is life-saving. Carnitine uptake has been shown to be defective in cultured skin fibroblasts and leukocytes obtained from patients with this condition. We report a new case of primary carnitine deficiency and offer direct evidence consistent with an impairment of carnitine uptake in differentiating muscle culture. The patient presented with severe and progressive cardiomyopathy and moderate proximal limb weakness. Plasma and muscle carnitine levels were very low, and the maximal rate of carnitine transport in cultured fibroblasts was deficient. An asymptomatic sister with intermediate levels of carnitine in plasma showed partially deficient carnitine uptake in fibroblasts, indicating heterozygosity. The patient's condition improved dramatically with oral carnitine therapy. Further studies were performed in cultured muscle cells at different stages of maturation, which demonstrated deficient maximal rates of carnitine uptake. Our findings are consistent with the concept that primary carnitine deficiency is the result of a generalized defect involving carnitine transport across tissue membranes.
Similar content being viewed by others
Main
PCD is defined as a decrease of intracellular carnitine content that impairs fatty acid oxidation and that is not associated with another identifiable systemic illness which might deplete tissue carnitine stores(1). The criteria for the diagnosis of PCD are: 1) severe reduction of plasma or tissue carnitine levels, 2) evidence that the low carnitine levels impair fatty acid oxidation, 3) correction of the disorder when carnitine levels are raised with L-carnitine replacement, and 4) absence of other primary defects in fatty acid oxidation(2).
PCD patients present with severe progressive cardiomyopathy and/or recurrent episodes of encephalopathy associated with hypoketotic hypoglycemia and liver dysfunction. Skeletal muscle involvement may manifest as motor delay, hypotonia, or proximal limb weakness. A dramatic clinical improvement occurs when plasma carnitine levels are raised by oral carnitine replacement(3).
Deficient transport of carnitine in cultured fibroblasts and leukocytes has been found in PCD patients(3). Parents show intermediate levels of uptake indicating an autosomal recessive pattern of inheritance(3, 4). Both renal reabsorption and intestinal uptake of carnitine are low in PCD patients, indicating that carnitine transport in kidney and gut are also affected(2, 5). The defective renal and intestinal carnitine handling causes carnitine levels to fall in blood, but it is still not clear whether the low carnitine content in other tissues is secondary to the low levels of serum carnitine, or whether it involves a more generalized defect of carnitine transport(6). In this report, we present a new patient with PCD, in whom deficient carnitine uptake is documented in fibroblast as well as in muscle cultures. This study provides direct evidence consistent with impairment of carnitine uptake in muscle in this condition.
METHODS
Case report. A 12-y-old Polish girl was the product of a full-term pregnancy and uncomplicated delivery. The parents and an older sister were healthy. An older brother died at age 9 y of a progressive cardiomyopathy.
At age 7 y, she began to complain of right-sided chest pain. Six months later congestive heart failure secondary to dilated cardiomyopathy was diagnosed. Digoxin and diuretics resulted in initial symptomatic improvement and decrease in heart size. Four years later, she was evaluated at our institution for possible cardiac transplantation. Cardiac failure was refractory to medical management. The physical examination was consistent with heart failure, with tachycardia, moderate mitral insufficiency, gallop rhythm, and left ventricular heave. She had mild diffuse hypotonia and mild weakness of the axial musculature. A two-dimensional echocardiogram showed the left ventricular end-diastolic dimension to be dilated at 7.46 cm with a fractional shortening of 15%. Laboratory data showed Hb of 11.8 g/dL, hematocrit 34.9%, and normal red blood cell indices. Aspartate aminotransferase was 55 IU/L (normal, 1-31), alanine aminotransferase 64 IU/L (normal, 1-31), and CK 366 IU/L (normal, 24-170), which was 100% CK-MM (isoenzyme of CK with muscle subunits). Serum total carnitine was 8.2 μmol/L (normal, 59 ± 12), and free carnitine was 7.6 μmol/L (normal, 47 ± 10). Oral L-carnitine therapy was started at 180 mg/kg/d. Ten days later, her gallop and heave disappeared, and on echocardiogram her fractional shortening had increased to 25%. Over the next month her digoxin and captopril were discontinued. On echocardiogram her left ventricular end-diastolic dimension decreased to 5.08 cm, and her mitral regurgitation disappeared. Serum total carnitine levels increased to 36 μmol/L and free carnitine to 27 μmol/L. Four months after starting L-carnitine, muscle total carnitine was 0.6% of control values. Skeletal muscle biopsy revealed mild atrophy of type II fibers and mild excess of sarcoplasmic lipid, mainly in type I fibers.
Her asymptomatic 19-y-old sister had a plasma total carnitine level of 24 μmol/L and a free carnitine of 12 μmol/L.
Culture conditions. Skin fibroblast cultures, first grown as 0.5-1 mm2 explants, were trypsinized and propagated further in monolayer, as previously described(7). The cells were grown in Eagle's minimal essential medium and 10% FBS, without antibiotics. Muscle cultures were grown in minimal essential medium and 15% FBS, supplemented with additional nonessential amino acids and vitamins, as described previously(8). Briefly, the muscle was cleaned of adhering connective tissue, trypsinized, and grown at low density in 10-cm2 Petri dishes (200-400 cells/dish). After 2-3 wk, the muscle cell colonies were trypsinized and pooled in 75-cm2 culture flasks. As the cultures approached confluency the cells were trypsinized again and transferred to appropriate dishes for further studies. After 6-7 d some of the cultures were induced to fuse in low mitogen medium, consisting of Ham's F14 nutrient mixture, supplemented with 0.01 μg/mL epidermal growth factor, 10 μg/mL insulin, and 0.5 μg/mL BSA(9). Cultures were routinely fed every 3rd d. (All media components were from Life Technologies Inc., Grand Island, NY). Control fibroblast and muscle cultures were prepared from diagnostic biopsies of patients considered free of muscle disease after all diagnostic studies were performed. The studies were done after approval by the institutional review board on human investigation of Columbia University.
Immunocytochemistry. An anti-myosin heavy chain MAb (MF20), kindly provided by Drs. D. Fischman and D. Bader (Cornell University, New York), recognizing sarcomeric myosin, was used as a marker of muscle differentiation. The cultures were grown in 35-mm2 six-well cluster dishes with coverslip inserts, rinsed in PBS (pH 7.3), fixed in acetone at -20 °C for 1 min, and air-dried. After exposure to the antibody (diluted 1:50) in PBS and 5% FBS for 1 h, the cultures were rinsed and incubated with rhodamine-conjugated anti-mouse antibody (diluted 1:100) for 1 h. Specificity was confirmed by incubating paired cultures with nonimmune serum. The preparations were studied in a Nikon microscope with epi illumination, using appropriate filters to detect rhodamine fluorescence.
CK isoenzymes. CK isoenzymes were studied after electrophoretic separation in cellulose acetate membranes, as described previously(8).
Carnitine uptake studies. The uptake of carnitine was investigated in fibroblasts and cultured muscle cells plated onto 9.5-cm2 six-well plates. Cells were fed 24 h before the study with RPMI 1640 medium (Life Technologies) supplemented with 10% FCS. The monolayer was washed with PBS, and the medium was replaced with RPMI 1640 without FCS, containing 0.05 μCi of L-methyl-[3H]carnitine (Amersham Corp., Arlington Heights, IL) per mL and unlabeled L-carnitine (gift from Sigma Chemical Co.-Tau Pharmaceutical Inc., Gaithersburg, MD) at concentrations ranging from 0.1 to 50 μmol/L. A carnitine concentration of 10 mmol/L was used to determine nonspecific uptake. Incubations were performed for 4 h at 37 °C in humidified 95% air and 5% CO2. The cell monolayer was washed four times with cold PBS and then hydrolyzed with 0.5 N sodium hydroxide. The cell-bound radioactivity was determined in 800 μL of the final cell hydrolysate using CytoScint (ICN Biomedicals Inc., Costa Mesa, CA). Cell protein was measured in the remaining 200 μL of the hydrolysate for each individual plate by the method of Lowry et al.(10). Experiments were performed in duplicate and were run in parallel with one or two control cultures. Specific uptake of radioactivity was used to calculate the rates -of total carnitine uptake. Apparent Michaelis-Menten constants (Km and Vmax values) were obtained by linear regression analysis of Lineweaver-Burk plots.
Radiolabeled fatty acid oxidation. [1-14C]Butyrate oxidation, [9,10(N)-3H]myristate oxidation, and [9,10(N)-3H]palmitate oxidation were performed in the patient and her sister's cultured skin fibroblasts as previously described(11). Cells were assayed in duplicate three times with [1-14C]butyrate, five times with [9,10(N)-3H]myristate, and twice with [9,10(N)-3H]palmitate. A second set of [9,10(N)-3H]palmitate oxidation experiments were performed preincubating 1 mM carnitine for 15 min before adding [9,10(N)-3H]palmitate.
RESULTS
Immunostaining and CK isoenzymes. We studied the uptake of carnitine in the patient's cultured skin fibroblasts, as well as cultured skeletal muscle cells at the myoblast stage, and after muscle differentiation in postmitotic muscle syncytia. To determine whether myogenesis was affected in PCD, and to ascertain that the patient's cultures and control muscle cultures were compared at similar stages of development, we estimated the degree of myogenesis in the cultures by two criteria: 1) the expression of sarcomeric myosin, which appears during myogenesis, at the time of myoblast fusion, and 2) the transition of CK isoenzymes from CK-BB (isoenzyme of CK with brain subunits) expressed in undifferentiated myoblasts, to CK-MM, which becomes detectable at the time of myoblast fusion and is further up-regulated during differentiation. Using these two criteria, we found no significant difference in myogenesis between the patient's muscle cultures, and those of the controls. In immunocytochemical studies, using a specific MAb, we found no sarcomeric myosin expression in the patient's cultures and in the control cultures that were studied at the myoblast stage. By electrophoresis, only CK-BB isozyme activity was demonstrable in the myoblasts from the patient and controls. In 18-d-old cultures, 8 d after myoblast fusion, there was also no difference between the patient's cultures and the controls: 74.4 ± 9.4% and 76.4 ± 12.5%, respectively, of the total number of muscle nuclei had been incorporated into multinucleate myotubes. At the myotube stage, the patient's and the controls' cultures expressed sarcomeric myosin. Specific muscle CK-MM isoenzyme was demonstrable, measuring approximately 25% of the total CK.
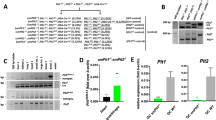
Carnitine uptake studies. Carnitine uptake in cultured skin fibroblasts from the patient was minimal at concentrations ranging from 0.1 to 5 μM, thereby precluding the calculation of Km and Vmax values. At a 5 μM carnitine concentration, the uptake was 0.032 pmol/min/mg of protein (normal, 1.230 ± 0.466) (mean ± SD). Fibroblasts from the patient's sister showed intermediate values of uptake: at a carnitine concentration of 5 μM, the uptake was 0.654 pmol/min/mg protein (Fig. 1A). The Km was 3.29 μM (normal, 4.94 ± 1.68 μM) and the maximum rate of uptake (Vmax) was 1.13 pmol/min/mg of protein (normal, 2.50 ± 0.85).
In control myoblasts, the Km was 2.38 ± 0.80 μM and the Vmax was 3.80 ± 1.51 pmol/min/mg of protein. In control myotubes, the Km was 1.31 ± 0.27 μM and the Vmax was 3.85 ± 0.67 pmol/min/mg of protein. Carnitine uptake in the cultured muscle cells of the patient was minimal at carnitine concentrations ranging from 0.1 to 5 μM: at 5 μM carnitine concentration, carnitine uptake in myoblasts was 0.038 pmol/min/mg of protein (normal, 1.629 ± 0.521) (Fig. 1B) and in myotubes was 0.044 pmol/min/mg of protein (normal, 0.844 ± 0.312) (Fig. 1C). Again, due to the markedly reduced uptake, it was not possible to calculate the Km and Vmax values.
Radiolabeled fatty acid oxidation. Oxidation studies were consistent with a defect in long chain fatty acid oxidation. When fibroblasts were incubated with 1 mM carnitine, [9,10(N)-3H]palmitate oxidation increased from 25 to 63% of normal control values (Table 1). This extracellular concentration of carnitine was likely high enough to facilitate its entrance into the cell by passive diffusion down a concentration gradient. Therefore, the restoration of [9,10(N)-3H]palmitate oxidation, when carnitine was available within the cell, demonstrated that both long chain fatty acid oxidation and carnitine metabolism were normal. [1-14C]Butyrate oxidation and [9,10(N)-3H]myristate oxidation in skin fibroblasts from the patient's sister were within normal limits (Table 1).
DISCUSSION
Different abnormalities in carnitine metabolism have been considered to explain the pathogenesis of PCD(13–15), but deficiency of carnitine transport is the only etiology demonstrated so far in this condition(3). Carnitine is transported from blood into tissues against a large concentration gradient driven by a putative sodium-dependent transporter(16). Differences in the kinetic properties of the transporter have been documented in several tissues. In skeletal muscle, heart cells, and cultured skin fibroblasts, a putative high affinity carnitine transporter functions at low carnitine concentrations (Km = 0.5-10 μmM)(3, 17–19). In fibroblast and muscle cultures, there also appears to be a second transporter with lower affinity (Km = 40-200 μM), which, in muscle cells, appears to develop during muscle maturation(19). A putative intermediate affinity transporter has been described in intestinal epithelial and renal tubular tissues (Km = 10-200 μM)(20–22), whereas a low affinity transporter functioning at high carnitine concentrations has been found in liver and brain (Km = 500-1000 μM)(16, 23).
Assay of the high affinity, low concentration carnitine uptake in cultured fibroblasts is used for the diagnosis of patients with PCD and for the screening of siblings and heterozygous parents(2–4, 24, 25).
We report a new patient with PCD, who fulfilled all diagnostic criteria: 1) severe reduction of carnitine in plasma and skeletal muscle; 2) impairment of fatty acid oxidation manifesting as severe progressive cardiomyopathy and lipid storage myopathy; 3) significant clinical improvement in cardiac and muscle function after carnitine treatment, with plasma carnitine concentration restored to half of normal; and 4) restoration of long chain fatty acid oxidation in fibroblasts with carnitine supplementation (Table 1).
In cultured skin fibroblasts from our patient, carnitine uptake was 2.6% of normal, precluding the calculation of Km and Vmax. These data are in agreement with previous reports in which residual carnitine uptake in fibroblasts varied between 2 and 10% of control values(2–4, 25). Because heterozygote patients may became symptomatic(24), we also investigated the proband's sister for possible heterozygosity. Carnitine uptake in cultured fibroblasts from the sister showed a normal Km, whereas the Vmax was approximately 45% of control subjects, supporting heterozygosity. These results are consistent with those reported in other affected families, where obligate heterozygote parents had normal Km and intermediate Vmax values (13-50%)(3–4, 24), suggesting a reduced number of normally functioning carnitine transporters(4).
We also studied carnitine uptake in cultured muscle from our patient. Two lines of evidence had suggested that muscle carnitine transport is also affected in PCD: 1) muscle carnitine concentrations increase only slightly after raising plasma carnitine concentrations(2–4) and 2) muscle cells share similar kinetic properties with fibroblasts when studied in culture under the same assay conditions(17, 19). However, direct evidence of deficient carnitine transport in skeletal muscle in PCD patients was lacking. We compared carnitine uptake in muscle cultures from our patient and from control subjects at the myoblast stage, and after myoblast fusion into multinucleated syncytia (myotubes). The Km and Vmax values in control myoblasts and myotubes confirmed previous studies(17, 19). A defect in the high affinity carnitine uptake was demonstrated in both myoblasts and myotubes from the patient (Fig. 1,B and C). The mean uptake rate at a carnitine concentration of 5 μM was 2.3% of control values in myoblasts, and 5.2% of control values in myotubes. Thus the severity of carnitine uptake impairment in cultured muscle cells was similar to that in cultured skin fibroblasts (Fig. 1).
Aneural muscle cultures fuse and differentiate but they may not reach sufficient maturity to achieve full phenotypic expression of some genetic diseases with muscle involvement(26). According to the degree of cellular fusion, the pattern of CK isoenzymes and the presence of sarcomeric myosin, our patient's muscle cells were brought to a high level of differentiation in culture(7). We analyzed the high affinity carnitine uptake at successive stages of differentiation, and in agreement with others(19), we did not find differences in the carnitine uptake between myoblasts and myotubes of control cells. Because myogenesis was not found to be affected in the PCD patient and in the control subjects and because the patient's muscle cultures were compared at the same stages of development (see “Results”), the finding of deficient carnitine uptake in our PCD patient suggests that this transporter is already expressed in cultured muscle cells at early stages of myogenesis.
In the past, similar studies failed to demonstrate deficient carnitine uptake in fibroblast and muscle cultures from patients with systemic carnitine deficiency(17). It was postulated that the lack of achieving a high degree of differentiation, as well as contamination by non-muscle cells, was the cause of the failure. Subsequently, it was reported that these particular patients were, in fact, affected with medium chain acyl-CoA dehydrogenase deficiency. Therefore the documented carnitine deficiency was secondary(27). Normal carnitine uptake in cultured fibroblasts has been documented in secondary carnitine deficiencies due to intramitochondrial fatty acid oxidation defects(12), thus explaining the failure to demonstrate abnormal uptake in these patients.
Our findings are consistent with a primary defect of carnitine uptake into muscle, which would explain the low tissue carnitine concentrations and the lipid storage myopathy in our patient. Furthermore, these results suggest that this patient has a genetic defect involving a common transporter shared both by fibroblasts and skeletal muscle, or at least, a common subunit shared by different isoforms of the transporter.
The results suggest that the lack of normalization of carnitine concentration in the muscle of patients with PCD during carnitine treatment is due to defective uptake. After 4 mo of oral carnitine treatment, our patient's muscle carnitine concentration was only 0.6% of the control value. These patients would, therefore, be at risk for increased muscle weakness when higher fatty acid oxidation rates are required (e.g. fasting, intercurrent infections, prolonged exercise), or when higher amounts of carnitine are needed (e.g. pregnancy, lactating women). It would therefore seem prudent to increase the L-carnitine supplementation during these periods of added stress.
The kinetics of carnitine uptake in myocardial cells are similar to those in muscle cells(18), and heart carnitine concentrations in PCD are very low(3). The dramatic improvement cardiac function 4 mo after carnitine supplementation in our patient suggests that a modest increase in tissue carnitine concentration is sufficient to restore efficient long chain fatty acid oxidation in the heart(28).
Carnitine uptake in liver does not seem to be affected in PCD, as suggested by the large increase in carnitine concentration with carnitine supplementation(2, 3). Moreover, different kinetic properties of carnitine uptake in liver compared with fibroblasts or muscle implies that the liver transporter is distinct(16). Carnitine uptake in brain also differs in its kinetic properties from fibroblasts and muscle(16, 23). The presence of CNS signs such as cognitive delay or pyramidal tract signs in some cases of PCD is considered to be secondary to associated complications such as hypoglycemic encephalopathy or cardiac failure(4).
In summary, we documented a defect of carnitine uptake in skin fibroblasts and in muscle cells cultured from a patient who fulfilled the criteria for PCD. These results suggest that both the putative muscle and fibroblast carnitine transporters share a single genetic defect in PCD. These results further support the hypothesis that PCD is due to a generalized defect in the uptake of carnitine in fibroblasts, kidney, gut, skeletal muscle, and heart. This defect does not involve the liver or brain. Further studies are needed to isolate and characterize the putative plasmalemmal carnitine transporter and to elucidate the molecular defect in this condition.
Abbreviations
- PCD:
-
primary carnitine deficiency
- CK:
-
creatine kinase
- FBS:
-
fetal bovine serum
References
Roe CR, Coates PM 1995 Mitochondrial fatty acid oxidation disorders. In: Scriver CR, Beaudet AL, Sly WS and Valle D (eds) The Metabolic and Molecular Basis of Inherited Diseases, Vol 1, 7th Ed. McGraw-Hill, New York, pp 1501–1533.
Treem WR, Stanley CA, Finegold DN, Hale DE, Coates PM 1988 Primary carnitine deficiency due to a failure of carnitine transport in kidney, muscle and fibroblasts. N Engl J Med 319: 1331–1336.
Stanley CA, DeLeeuw S, Coates PM, Vieney-Liaud C, Divry P, Bonnefont JP, Saudubray JM, Haymond M, Trefz FK, Breningstall GN, Wapper RS, Byrd DJ, Sansariq G, Tein I, Grover W, Valle D, Rutledge L, Treem WR 1991 Chronic cardiomyopathy and weakness or acute coma in children with a defect in carnitine uptake. Ann Neurol 30: 709–716.
Tein I, DeVivo DC, Bierman F, Pulver P, LJ DeMerleir, Cvitanovic-Sojat Pagon RA, Bertini E, Dionisi-Vici, Servidei S, DiMauro 1990 Impaired skin fibroblasts carnitine uptake in primary systemic carnitine deficiency manifested by childhood carnitine-responsive cardiomyopathy. Pediatr Res 28: 247–253
Waber LJ, Valle D, Neill C, DiMauro S, Shug A 1982 Carnitine deficiency presenting as familial cardiomyopathy: a treatable defect in carnitine transport. J Pediatr 101: 700–705.
Pons R, De Vivo DC 1995 Primary and secondary carnitine deficiency syndromes. J Child Neurol 10( supp): 2S8-2S24.
Miranda AF, Somer H, DiMauro S 1979 Isoenzymes as markers of differentiation. In: Mauro A (ed) Muscle Regeneration. Raven Press, New York, pp 453–473.
Miranda AF, Babiss LE, Fisher PB 1986 Measurement of the effect of interferons on cellular differentiation of human skeletal muscle cells. Methods Enzymol 119: 619–628.
ST Clair JA, Meyer-Demarest SD, Ham RG 1992 Improved medium with EGF and BSA for differentiated human skeletal muscle cells. Muscle Nerve 15: 774–779.
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ 1951 Protein measurement with folin phenol reagent. J Biol Chem 193: 265–275.
Rhead W, Roettger V, Marshall T, Amendt B 1993 Multiple acyl-CoA coenzyme A dehydrogenation disorder responsive to riboflavin: substrate oxidation, flavin metabolism, and flavoenzyme activities in fibroblasts. Pediatr Res 33: 129–135.
Tein I, De Vivo DC, Ranucci D, DiMauro S 1993 Skin fibroblasts carnitine uptake in secondary carnitine deficiency disorders. J Inherited Metab Dis 16: 135–146.
Rebouche CJ, Engel AG 1980 In vitro analysis of hepatic carnitine biosynthesis in systemic carnitine deficiency syndromes. Clin Chim Acta 106: 295–300.
Engel AG, Rebouche CJ, Wilson DM, Glasgow AM, Romshe CA, Cruse RP 1985 Primary systemic carnitine deficiency. II. Renal handling of carnitine. Neurology 31: 819–825.
Rebouche CJ, Engel AG 1984 Kinetic compartmental analysis of carnitine deficiency syndromes. Evidence of alterations in the tissues carnitine transport. J Clin Invest 73: 857–867.
Bremer J 1983 Carnitine-metabolism and functions. Physiol Rev 63: 1420–1480.
Rebouche CJ, Engel AG 1982 Carnitine transport in cultured muscle cells and skin fibroblasts from patients with primary systemic carnitine deficiency. In Vitro 18: 495–500.
Bohmer T, Eiklid K, Jonsen J 1977 Carnitine uptake into human heart cells in culture. Biochim Biophys Acta 465: 627–633.
Martinuzzi A, Vergani L, Rosa M, Angelini C 1991 L-Carnitine uptake in differentiating human cultured muscle. Biochim Biophys Acta 1095: 217–222.
Shaw RD, Li BUK, Hamilton JW, Shug AL, Olsen W 1983 Carnitine transport in rat small intestine. Am J Physiol 245:G376–G381.
Huth PJ, Shug AL 1980 Properties of carnitine transport in rat kidney cortex slices. Biochim Biophys Acta 602: 621–634.
Rebouche CJ, Mack DL 1984 Sodium gradient-stimulated transport of l-carnitine into renal brush border membrane vesicles: kinetics, specificity, and regulation by dietary carnitine. Arch Biochem Biophys 235: 393–402.
Bieber LL 1988 Carnitine. Annu Rev Biochem 57: 261–283.
Garavaglia B, Uziel G, Dworzak F, Carrara F, DiDonato S 1991 Primary carnitine deficiency: heterozygote and intrafamilial phenotypic variation. Neurology 41: 1691–1693.
Erikson BO, Gustafson B, Lindstedt S, Nordin I 1989 Transport of carnitine into cells in hereditary carnitine deficiency. J Inherited Metab Dis 12: 108–111.
Miranda AF 1994 Disease muscle in tissue culture. In: Engel AG and Franzini-Amstrong CL (eds) Myology: Basic and Clinical, Vol 1, 2nd Ed. MacGraw-Hill, New York, pp 1045–1071.
Stanley CA 1987 New genetic defects in mitochondrial fatty acid oxidation and carnitine deficiency. Adv Pediatr 34: 59–88.
Stanley CA 1991 Carnitine disorders. Adv Pediatr 42: 208–243.
Acknowledgements
The authors thank Pamela Kranz-Eble for the preparation of fibroblast cultures.
Author information
Authors and Affiliations
Additional information
Supported in part by the Colleen Giblin Foundation for Pediatric Neurology Research, by Sigma-Tau Pharmaceuticals (Pomezia, Italy, and Gaithersburg, MD), and by an Operating Grant from the Heart and Stroke Foundation of Ontario. R.P. is a recipient of the grant FIS 94/5825 (Ministerio de Sanidad y Consumo, Spain). R.C. is a recipient of the fellowship grant from Telethon, Italy, CPT/CL/5777. I.T. is a recipient of a Scholarship from the Medical Research Council of Canada.
Rights and permissions
About this article
Cite this article
Pons, R., Carrozzo, R., Tein, I. et al. Deficient Muscle Carnitine Transport in Primary Carnitine Deficiency. Pediatr Res 42, 583–587 (1997). https://doi.org/10.1203/00006450-199711000-00005
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199711000-00005
This article is cited by
-
Intracellular in vitro probe acylcarnitine assay for identifying deficiencies of carnitine transporter and carnitine palmitoyltransferase-1
Analytical and Bioanalytical Chemistry (2013)
-
Hyperammonemic Encephalopathy Caused by Carnitine Deficiency
Journal of General Internal Medicine (2008)