Abstract
Objectives:
Neuroendocrine prostate cancers (NEPCs) are rare. The current lack of consensus for clinical, biological and pathological characterization as well as therapeutic approach makes the management of those tumors a clinical challenge. This literature review aims to summarize available data on the characterization and management of patients with prostate cancer with a neuroendocrine element. We try to identify major controversies and uncertainties in order to understand all aspects of this particular entity.
Methods:
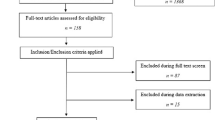
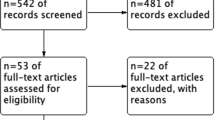
We searched for all articles published and registered in the MEDLINE database before 31 November 2013 with the following search terms: ((‘prostatic neoplasms’ (MeSH Terms)) AND (‘carcinoma, neuroendocrine’ (MeSH Terms)) OR (‘carcinoma, small cell’ (MeSH Terms))) AND (English (Language)).
Results:
Case reports, letters or comments were excluded. We then selected relevant articles from titles and abstracts. Overall, 278 articles published between 1976 and November 2013 were identified. No definition of NEPC seems to be clearly established. Natural history of the disease reveals poor prognosis with median survival of up to 10 to 13 months. Histological characterization appears difficult. Serum markers could be helpful with some controversies in terms of prognostic significance. Concerning management, the majority of patients received local treatment combined with chemotherapy in case of early and localized disease. Few clinical trials described strategy for metastatic disease.
Conclusions:
The exploration of the different pathways implicated in the neuroendocrine differentiation of prostate cancers is essential for the comprehension of castration-resistance mechanisms. It will enable the identification of optimal therapeutic strategies for which no recommendation is currently established. Inclusion in prospective clinical trials appears necessary to identify the adequate strategy.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
di Sant'Agnese PA, Cockett AT . Neuroendocrine differentiation in prostatic malignancy. Cancer 1996; 78: 357–361.
Helpap B, Kollermann J . Undifferentiated carcinoma of the prostate with small cell features: immunohistochemical subtyping and reflections on histogenesis. Virchows Arch 1999; 434: 385–391.
Abrahamsson PA . Neuroendocrine differentiation in prostatic carcinoma. Prostate 1999; 39: 135–148.
Berruti A, Dogliotti L, Mosca A, Bellina M, Mari M, Torta M et al. Circulating neuroendocrine markers in patients with prostate carcinoma. Cancer 2000; 88: 2590–2597.
Abbas F, Civantos F, Benedetto P, Soloway MS . Small cell carcinoma of the bladder and prostate. Urology 1995; 46: 617–630.
Grobholz R, Griebe M, Sauer CG, Michel MS, Trojan L, Bleyl U . Influence of neuroendocrine tumor cells on proliferation in prostatic carcinoma. Hum Pathol 2005; 36: 562–570.
Sciarra A, Innocenzi M, Ravaziol M, Minisola F, Alfarone A, Cattarino S et al. [Role of neuroendocrine cells in prostate cancer progression]. Urologia 2011; 78: 126–131.
Vashchenko N, Abrahamsson PA . Neuroendocrine differentiation in prostate cancer: implications for new treatment modalities. Eur Urol 2005; 47: 147–155.
Amato RJ, Logothetis CJ, Hallinan R, Ro JY, Sella A, Dexeus FH . Chemotherapy for small cell carcinoma of prostatic origin. J Urol 1992; 147: 935–937.
di Sant'Agnese PA . Neuroendocrine differentiation in prostatic carcinoma: an update on recent developments. Ann Oncol 2001; 12 (Suppl 2): S135–S140.
Spiess PE, Pettaway CA, Vakar-Lopez F, Kassouf W, Wang X, Busby JE et al. Treatment outcomes of small cell carcinoma of the prostate: a single-center study. Cancer 2007; 110: 1729–1737.
Leibovici D, Spiess PE, Agarwal PK, Tu SM, Pettaway CA, Hitzhusen K et al. Prostate cancer progression in the presence of undetectable or low serum prostate-specific antigen level. Cancer 2007; 109: 198–204.
Nishio R, Furuya Y, Nagakawa O, Fuse H . Metastatic prostate cancer with normal level of serum prostate-specific antigen. Int Urol Nephrol 2003; 35: 189–192.
Papandreou CN, Daliani DD, Thall PF, Tu SM, Wang X, Reyes A et al. Results of a phase II study with doxorubicin, etoposide, and cisplatin in patients with fully characterized small-cell carcinoma of the prostate. J Clin Oncol 2002; 20: 3072–3080.
Galanis E, Frytak S, Lloyd RV . Extrapulmonary small cell carcinoma. Cancer 1997; 79: 1729–1736.
Spieth ME, Lin YG, Nguyen TT . Diagnosing and treating small-cell carcinomas of prostatic origin. Clin Nucl Med 2002; 27: 11–17.
Kawai S, Hiroshima K, Tsukamoto Y, Tobe T, Suzuki H, Ito H et al. Small cell carcinoma of the prostate expressing prostate-specific antigen and showing syndrome of inappropriate secretion of antidiuretic hormone: an autopsy case report. Pathol Int 2003; 53: 892–896.
Palmgren JS, Karavadia SS, Wakefield MR . Unusual and underappreciated: small cell carcinoma of the prostate. Semin Oncol 2007; 34: 22–29.
Tu SM, Lin SH, Logothetis CJ . Stem-cell origin of metastasis and heterogeneity in solid tumours. Lancet Oncol 2002; 3: 508–513.
Ishida E, Nakamura M, Shimada K, Tasaki M, Konishi N . Immunohistochemical analysis of neuroendocrine differentiation in prostate cancer. Pathobiology 2009; 76: 30–38.
Lotan TL, Gupta NS, Wang W, Toubaji A, Haffner MC, Chaux A et al. ERG gene rearrangements are common in prostatic small cell carcinomas. Mod Pathol 2011; 24: 820–828.
Beltran H, Tagawa ST, Park K, MacDonald T, Milowsky MI, Mosquera JM et al. Challenges in recognizing treatment-related neuroendocrine prostate cancer. J Clin Oncol 2012; 30: e386–e389.
Furtado P, Lima MV, Nogueira C, Franco M, Tavora F . Review of small cell carcinomas of the prostate. Prostate Cancer 2011; 2011: 543272.
Nelson EC, Cambio AJ, Yang JC, Ok JH, Lara PN Jr., Evans CP . Clinical implications of neuroendocrine differentiation in prostate cancer. Prostate Cancer Prostatic Dis 2007; 10: 6–14.
Dunning NL, Laversin SA, Miles AK, Rees RC . Immunotherapy of prostate cancer: should we be targeting stem cells and EMT? Cancer Immunol Immunother 2011; 60: 1181–1193.
Smith BN, Odero-Marah VA . The role of Snail in prostate cancer. Cell Adh Migr 2012; 6: 433–441.
McKeithen D, Graham T, Chung LW, Odero-Marah V . Snail transcription factor regulates neuroendocrine differentiation in LNCaP prostate cancer cells. Prostate 2010; 70: 982–992.
Chu GC, Zhau HE, Wang R, Rogatko A, Feng X, Zayzafoon M et al. RANK- and c-Met-mediated signal network promotes prostate cancer metastatic colonization. Endocr Relat Cancer 2014; 21: 311–326.
Alberti C . Neuroendocrine differentiation in prostate carcinoma: focusing on its pathophysiologic mechanisms and pathological features. G Chir 2010; 31: 568–574.
Sagnak L, Topaloglu H, Ozok U, Ersoy H . Prognostic significance of neuroendocrine differentiation in prostate adenocarcinoma. Clin Genitourin Cancer 2011; 9: 73–80.
Evans AJ, Humphrey PA, Belani J, van der Kwast TH, Srigley JR . Large cell neuroendocrine carcinoma of prostate: a clinicopathologic summary of 7 cases of a rare manifestation of advanced prostate cancer. Am J Surg Pathol 2006; 30: 684–693.
Wang W, Epstein JI . Small cell carcinoma of the prostate. A morphologic and immunohistochemical study of 95 cases. Am J Surg Pathol 2008; 32: 65–71.
Mai KT, Roustan Delatour NL, Assiri A, Al-Maghrabi H . Secondary prostatic adenocarcinoma: a cytopathological study of 50 cases. Diagn Cytopathol 2007; 35: 91–95.
Jongsma J, Oomen MH, Noordzij MA, Romijn JC, van der Kwast TH, Schroder FH et al. Androgen-independent growth is induced by neuropeptides in human prostate cancer cell lines. Prostate 2000; 42: 34–44.
Stein ME, Bernstein Z, Abacioglu U, Sengoz M, Miller RC, Meirovitz A et al. Small cell (neuroendocrine) carcinoma of the prostate: etiology, diagnosis, prognosis, and therapeutic implications–a retrospective study of 30 patients from the rare cancer network. Am J Med Sci 2008; 336: 478–488.
Palapattu GS, Wu C, Silvers CR, Martin HB, Williams K, Salamone L et al. Selective expression of CD44, a putative prostate cancer stem cell marker, in neuroendocrine tumor cells of human prostate cancer. Prostate 2009; 69: 787–798.
Ather MH, Abbas F, Faruqui N, Israr M, Pervez S . Correlation of three immunohistochemically detected markers of neuroendocrine differentiation with clinical predictors of disease progression in prostate cancer. BMC Urol 2008; 8: 21.
Fernandes RC, Matsushita MM, Mauad T, Nascimento Saldiva PH . Prostate carcinoma with neuroendocrine differentiation: case report and literature review. Rev Hosp Clin Fac Med Sao Paulo 2001; 56: 153–158.
Tamas EF, Epstein JI . Prognostic significance of paneth cell-like neuroendocrine differentiation in adenocarcinoma of the prostate. Am J Surg Pathol 2006; 30: 980–985.
Jeetle SS, Fisher G, Yang ZH, Stankiewicz E, Moller H, Cooper CS et al. Neuroendocrine differentiation does not have independent prognostic value in conservatively treated prostate cancer. Virchows Arch 2012; 461: 103–107.
Kamiya N, Akakura K, Suzuki H, Isshiki S, Komiya A, Ueda T et al. Pretreatment serum level of neuron specific enolase (NSE) as a prognostic factor in metastatic prostate cancer patients treated with endocrine therapy. Eur Urol 2003; 44: 309–314.
Aoki H, Ishidoya S, Ito A, Endoh M, Shimazui T, Arai Y . Experience of the treatment with gemcitabine, docetaxel, and carboplatin (GDC) chemotherapy for patients with small-cell carcinoma of the prostate. Int J Urol 2006; 13: 1254–1258.
May M, Siegsmund M, Hammermann F, Loy V, Gunia S . Prognostic significance of proliferation activity and neuroendocrine differentiation to predict treatment failure after radical prostatectomy. Scand J Urol Nephrol 2007; 41: 375–381.
Gunia S, Albrecht K, Koch S, Herrmann T, Ecke T, Loy V et al. Ki67 staining index and neuroendocrine differentiation aggravate adverse prognostic parameters in prostate cancer and are characterized by negligible inter-observer variability. World J Urol 2008; 26: 243–250.
Autorino R, Lamendola MG, De LG, De SM, Giuliano F, D' Armiento M et al. Neuroendocrine immunophenotype as predictor of clinical recurrence in 110 patients with prostate cancer. Int J Immunopathol Pharmacol 2007; 20: 765–770.
Krauss DJ, Hayek S, Amin M, Ye H, Kestin LL, Zadora S et al. Prognostic significance of neuroendocrine differentiation in patients with Gleason score 8-10 prostate cancer treated with primary radiotherapy. Int J Radiat Oncol Biol Phys 2011; 81: e119–e125.
Lilleby W, Paus E, Skovlund E, Fossa SD . Prognostic value of neuroendocrine serum markers and PSA in irradiated patients with pN0 localized prostate cancer. Prostate 2001; 46: 126–133.
Mackey JR, Au HJ, Hugh J, Venner P . Genitourinary small cell carcinoma: determination of clinical and therapeutic factors associated with survival. J Urol 1998; 159: 1624–1629.
Asmis TR, Reaume MN, Dahrouge S, Malone S . Genitourinary small cell carcinoma: a retrospective review of treatment and survival patterns at The Ottawa Hospital Regional Cancer Center. BJU Int 2006; 97: 711–715.
Flechon A, Pouessel D, Ferlay C, Perol D, Beuzeboc P, Gravis G et al. Phase II study of carboplatin and etoposide in patients with anaplastic progressive metastatic castration-resistant prostate cancer (mCRPC) with or without neuroendocrine differentiation: results of the French Genito-Urinary Tumor Group (GETUG) P01 trial. Ann Oncol 2011; 22: 2476–2481.
Culine S, El DM, Lamy PJ, Iborra F, Avances C, Pinguet F . Docetaxel and cisplatin in patients with metastatic androgen independent prostate cancer and circulating neuroendocrine markers. J Urol 2007; 178: 844–848.
Loriot Y, Massard C, Gross-Goupil M, Di PM, Escudier B, Bossi A et al. Combining carboplatin and etoposide in docetaxel-pretreated patients with castration-resistant prostate cancer: a prospective study evaluating also neuroendocrine features. Ann Oncol 2009; 20: 703–708.
Aparicio AM, Harzstark AL, Corn PG, Wen S, Araujo JC, Tu SM et al. Platinum-based chemotherapy for variant castrate-resistant prostate cancer. Clin Cancer Res 2013; 19: 3621–3630.
Aparicio A, Tzelepi V, Araujo JC, Guo CC, Liang S, Troncoso P et al. Neuroendocrine prostate cancer xenografts with large-cell and small-cell features derived from a single patient’s tumor: morphological, immunohistochemical, and gene expression profiles. Prostate 2011; 71: 846–856.
Ueda T, Suzuki H, Akakura K, Ishihara M, Kamiya N, Komiya A et al. Bisphosphonate and low-dose dexamethasone treatment for patients with hormone-refractory prostate cancer. Hinyokika Kiyo 2006; 52: 515–521.
Hsieh TC, Lin CY, Lin HY, Wu JM . AKT/mTOR as novel targets of polyphenol piceatannol possibly contributing to inhibition of proliferation of cultured prostate cancer cells. ISRN Urol 2012; 2012: 272697.
Ciarlo M, Benelli R, Barbieri O, Minghelli S, Barboro P, Balbi C et al. Regulation of neuroendocrine differentiation by AKT/hnRNPK/AR/beta-catenin signaling in prostate cancer cells. Int J Cancer 2012; 131: 582–590.
Beltran H, Rickman DS, Park K, Chae SS, Sboner A, MacDonald TY et al. Molecular characterization of neuroendocrine prostate cancer and identification of new drug targets. Cancer Discov 2011; 1: 487–495.
Meulenbeld HJ, Bleuse JP, Vinci EM, Raymond E, Vitali G, Santoro A et al. Randomized phase II study of danusertib in patients with metastatic castration-resistant prostate cancer after docetaxel failure. BJU Int 2013; 111: 44–52.
Veltri RW, Isharwal S, Miller MC, Epstein JI, Mangold LA, Humphreys E et al. Long-term assessment of prostate cancer progression free survival: evaluation of pathological parameters, nuclear shape and molecular biomarkers of pathogenesis. Prostate 2008; 68: 1806–1815.
Gong J, Lee J, Akio H, Schlegel PN, Shen R . Attenuation of apoptosis by chromogranin A-induced Akt and survivin pathways in prostate cancer cells. Endocrinology 2007; 148: 4489–4499.
Feng S, Agoulnik IU, Truong A, Li Z, Creighton CJ, Kaftanovskaya EM et al. Suppression of relaxin receptor RXFP1 decreases prostate cancer growth and metastasis. Endocr Relat Cancer 2010; 17: 1021–1033.
Littlepage LE, Sternlicht MD, Rougier N, Phillips J, Gallo E, Yu Y et al. Matrix metalloproteinases contribute distinct roles in neuroendocrine prostate carcinogenesis, metastasis, and angiogenesis progression. Cancer Res 2010; 70: 2224–2234.
Hussain M, Vaishampayan U, Du W, Redman B, Smith DC . Combination paclitaxel, carboplatin, and gemcitabine is an active treatment for advanced urothelial cancer. J Clin Oncol 2001; 19: 2527–2533.
Acknowledgements
We thank Pippa McKelvie-Sebileau and Jone Iriondo-Alberdi of Institut Bergonié for medical editorial.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Sargos, P., Ferretti, L., Gross-Goupil, M. et al. Characterization of prostate neuroendocrine cancers and therapeutic management: a literature review. Prostate Cancer Prostatic Dis 17, 220–226 (2014). https://doi.org/10.1038/pcan.2014.17
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pcan.2014.17