Abstract
G-protein-coupled receptor 120 (GPR120) functions as a receptor for unsaturated long-chain free fatty acids and has an important role in regulating lipid and glucose metabolism. However, a role for GPR120 in the development of tumors has not yet been clarified. Here, we show that GPR120 signaling promotes angiogenic switching and motility of human colorectal carcinoma (CRC) cells. We show that the expression of GPR120 is significantly induced in CRC tissues and cell lines, which is associated with tumor progression. Activation of GPR120 signaling in human CRC promotes angiogenesis in vitro and in vivo, largely by inducing the expression and secretion of proangiogenic mediators such as vascular endothelial growth factor (VEGF), interleukin-8 and cyclooxygenase-2-derived prostaglandin E2. The PI3K/Akt–NF-κB pathway is activated by GPR120 signaling and is required for GPR120 signaling-induced angiogenic switching in CRC cells. And, GPR120 activation enhances the motility of CRC cells and induces epithelial–mesenchymal transition. Furthermore, in vivo study shows that activation of GPR120 promotes angiogenesis and tumor growth. Finally, we find that GPR120 expression is positively correlated with VEGF expression and inversely correlated with the epithelial marker E-cadherin in CRC tissues. Collectively, our results demonstrate that GPR120 functions as a tumor-promoting receptor in CRC and, therefore, shows promise as a new potential target for cancer therapeutics.
Similar content being viewed by others
Introduction
Colorectal carcinoma (CRC) is one of the most common malignancies and the major causes of cancer-related mortality worldwide.1 Although the molecular mechanism of CRC has become better understood in the past two decades, the prognosis of CRC, especially in advanced cancer, has not been significantly improved. Colorectal carcinogenesis is based on a sequence of molecular events in enterocytes, including gene mutations, epigenetic modifications and aberrant signaling in basic cellular pathways. Thus, it is of great clinical value to identify potential molecules for tumor-preventive strategies.
Dysregulated G-protein-coupled receptor (GPCR) expression and dysregulation of GPCR signaling has been recognized as a hallmark of cancer.2 Cancer cells may acquire the capacity for autonomous and unregulated growth through abnormal, enhanced expression of specific GPCRs on cell membranes. This process may trigger a series of intracellular signals that ultimately lead to the proliferation of cancer cells, induction of angiogenesis and metastasis. Recently, several GPCRs identified as free fatty acid receptors have emerged as key players in various physiological homeostasis mechanisms. In particular, G-protein-coupled receptor 120 (GPR120), which is the most enigmatic member of this large family, has generated attention because of its potential role in the regulation of metabolic and inflammatory diseases such as obesity and type 2 diabetes.
GPR120 was originally described as an orphan receptor before its endogenous ligands, poly-unsaturated long-chain free fatty acids (FFAs), were known.3, 4, 5 It has been proposed to have an important role in regulating lipid and glucose metabolism by stimulating the release of incretin peptide hormones such as cholecystokinin and glucagon-like-peptide-1.6, 7 More recently, GPR120 has been shown to exert effects in regulating inflammation, mediating insulin sensitization and reducing obesity.8, 9 However, there is no report about the expression of GPR120 in tumors, and the role of GPR120 in tumor development is unknown, even though GPR120 is abundantly expressed in intestine.
In the present study, we focused on the role of GPR120 signaling in the development of human CRC. We showed that the expression of GPR120 was significantly increased in CRC tissues and cell lines, which was associated with tumor progression. Activation of GPR120 signaling induced the expression and secretion of proangiogenic mediators of CRC cells to promote angiogenesis. The PI3K/Akt–NF-κB pathway was activated by GPR120 signaling and was required for GPR120 signaling-induced angiogenic switching in CRC cells. Furthermore, GPR120 activation enhanced motility of CRC cells and induced epithelial–mesenchymal transition (EMT) of CRC cells. Altogether, our results indicate that GPR120 functions as a tumor-promoting receptor in CRC and, therefore, represents a potential target for treatment of cancers.
Results
GPR120 is induced in human CRC tissues and its expression is correlated with clinicopathologic characteristics of patients
As GPR120 is abundantly expressed in the intestine, we sought to investigate the relationship between its expression and clinicopathologic characteristics of CRC. We examined GPR120 expression in paraffin-embedded, archived CRC tissues using immunohistochemistry (IHC) staining and real-time PCR. Clinical features of these patients and statistical analyses of the IHC staining are summarized in Table 1. As shown in Figures 1a and b, GPR120 exhibited cytoplasmic localization and its expression in cancerous tissues was significantly higher than that in adjacent noncancerous tissues (P<0.001). In addition, both IHC and real-time PCR analysis of GPR120 expression demonstrated that GPR120 expression increased in tumors with poor pathologic differentiation (Figure 1a) and with advanced clinical stage (Figure 1b), suggesting a clinical association between the expression of GPR120 and progression of CRC. Interestingly, we also found that there was a significant association between the expression of GPR120 in CRC tissues and the body mass index of both male (P=0.036) and female patients (P=0.048). This result was fully consistent with recent publication showing an association of an increase in GPR120 expression with human obesity.9
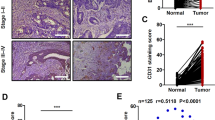
Increased GPR120 expression in human CRC tissues. (a, b) Representative examples of IHC staining analyses of GPR120 in human normal colorectal tissues and CRC tissues with different degrees of differentiation (a) or in different clinical stages (b), and comparison of GPR120 ratios in CRC tissues with different degrees of differentiation (a) or in different clinical stages (b). (c) Representative examples of IHC staining analyses of GPR40 in human normal colorectal tissues and CRC tissues, and RT–PCR analyses of GPR40 expression in CRC cell lines and samples. Pancreatic tissue was employed as IHC positive control. The black arrows indicated positive staining of pancreatic islets. Scale bar, 2 mm (top panel), 50 μm (bottom panel). MCF-7 was employed as RT–PCR positive control. P1–P2: representative of 20 patients.
G-protein-coupled 40 (GPR40), which is predominantly expressed in pancreatic β-cells10 shares the same ligands with GPR120. Thus, we also examined GPR40 expression in CRC tissues using IHC staining, and RT–PCR. There was no detectable GPR40 expression in either of the cancerous tissues (Figure 1c).
GPR120 is overexpressed in CRC cell lines
Based on its tissue expression pattern, it was of particular interest to pursue the biology of GPR120 in human CRC. We detected GRP120 expression in a panel of malignant and nonmalignant human colorectal cell lines. Higher GPR120 expression was detected in all the eight tested CRC cell lines, as compared with two normal colon cell lines (Figure 2a). Cells HCT 116 and SW480, which expressed a high level of GPR120, were used for further study.
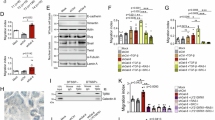
GPR120 is overexpressed and functional in human CRC cell lines. (a) Western blotting analyses of GPR120 expression in eight human CRC cell lines and two normal colon cell lines. β-actin was used as the loading control. (b) HCT 116 and SW480 cells were transfected with scramble shRNA (Src) or GPR120 shRNA-expressing constructs (GPR120 KD). GPR120 KD cell lines exhibited a marked reduction in GRP120 protein level compared with Src. (c) A [Ca2+]i response was induced by GW9508 in HCT116 Src/GPR120 KD cell lines and SW480 Src/GPR120 KD cell lines. HCT116 Src/GPR120 KD and SW480 Src/GPR120 KD cells were treated with GW9508 (10 μM). [Ca2+]i was stained with Flura-4 and changes in [Ca2+]i in cells with or without GW9508 stimulation were monitored by confocal laser scanning microscopy. Magnification, × 630.
To pursue the biology of GPR120 in further studies, the compound GW9508 was employed as a tool. GW9508, developed as a selective GPR40 agonist,11 also stimulates GPR120. As CRC cell lines do not express GPR40 (Figure 1c), GW9508 is a functional GPR120-specific compound in these cells. It was previously reported that GPR120 signals via a Gαq/11-coupled pathway.7 Thus, activation of GPR120 should result in an increase in the intracellular Ca2+ ([Ca2+]i) levels, an action mediated via Gαq/11.10, 12, 13 To determine whether GPR120 in CRC cells could respond to GW9508 stimulation, we examined the effects of GW9508 on the concentration of [Ca2+]i response by using [Ca2+]i staining. GW9508 stimulation induced a specific rise in [Ca2+]i, which was completely abrogated by shRNA-mediated knockdown of GPR120 (Figure 2c), suggesting that these effects were mediated through the activation of GPR120.
Activation of GPR120 promotes angiogenesis in vitro
Angiogenesis is essential for malignant tumor growth. Tumor cells induce angiogenesis by secreting a variety of angiogenic factors, which eventually promote tumor survival and metastasis. We evaluated the effects of GPR120 activation on regulating the expression of angiogenic factors in tumor cells. Among a panel of factors related to inflammation and angiogenesis, vascular endothelial growth factor (VEGF) and interlukin-8 (IL-8) increased significantly at both mRNA and protein levels in HCT 116 and SW480 cells upon GW9508 stimulation (Figures 3a and b).
Activation of GPR120 promotes angiogenesis of CRC cells. (a, b) HCT 116 Src/GPR120 KD and SW480 Src/GPR120 KD cells were seeded in 6-well plates and stimulated with GW9508 (10 μM) for the indicated times. (a) VEGF, IL-8 and COX-2 mRNA expression was measured by quantitative real-time PCR, and (b) VEGF, IL-8 and PGE2 secretion levels were measured by enzyme-linked immunosorbent assay. (c) Representative images of HUVEC tube formation. HUVECs were treated with 0.5% FBS (control), Src-CM, or GPR120 KD-CM. Tube formation was quantified in three randomly selected fields. Magnification, × 100. Bars represent mean number of branch points ±s.e.m. of three independent experiments. *P<0.05, **P<0.01.
Cyclooxygenase-2 (COX-2), an important factor related to inflammation, is critical for the development of colorectal neoplasia.14 Upon GW9508 stimulation, we found that COX-2 expression also was markedly increased in HCT 116 and SW480 cells (Figure 3a). Enzyme linked immunosorbent assay analysis showed that GW9508 induced an increase in prostaglandin E2 (PEG2) production in conditioned media (CM) of HCT 116 and SW480 cells (Figure 3b). Although COX-2 may modulate angiogenesis in several ways, increased production of PGE2 is thought to mediate the major role of COX-2 in angiogenesis.15 These data suggest that GPR120 signaling promotes angiogenesis, at least in part, by inducing COX-2-derived PGE2 production. However, enhanced VEGF, IL-8 and COX-2 expression by GW9508 treatment was completely abrogated by shRNA-mediated knockdown of GPR120 (Figures 3a and b). Furthermore, reintroduction of GPR120 in GPR120-knockdown cell lines was sufficient to restore proangiogenic gene expression (Supplementary Figure 1a), indicating that the inhibitory effects mediated by shRNA were specifically due to GPR120 depletion.
Additionally, we examined the effects of GPR120 signaling in tumor cells on tube formation in endothelial cells. In this regard, HCT 116 and SW480 cells were treated with or without GW9508, and CM was then collected for culture of human vein umbilical endothelial cells (HUVECs). As shown in Figure 3c, GW9508-pretreated CM efficiently promoted endothelial branching, as compared with those of controls, whereas knock down of GPR120 in HCT 116 and SW480 cells significantly impaired GW9508-induced effects on endothelial branching. Altogether, these data indicate that CRC may grow up and progress partly through activating GPR120 signaling to induce angiogenic switching.
GRP120 signaling induces angiogenesis in CRC cells through activation of the PI3K/Akt–NF-κB pathway
GPR120 triggers various cellular pathways to exert disparate functions.7, 8 As the above-identified induced proangiogenic genes are known downstream targets of NF-κB,16 we focused on the role of the NF-κB pathway in the production of proangiogenic mediators. First, we performed western blotting analysis to determine whether the NF-κB pathway was modulated by GPR120 signaling. Western blotting analysis revealed that phosphorylation of IκBα significantly increased in HCT 116 and SW480 cells after GW9508 stimulation. This stimulatory effect of GW9508 was blocked when GPR120 was depleted by knock down with shRNA (Figure 4a). Cells were then pretreated with the NF-κB inhibitor BAY 11-7082 (10 μM) before treatment with GW9508 to inhibit NF-κB activation. As shown in Figure 4b, NF-κB inhibition suppressed GW9508-induced proangiogenic gene expression in HCT 116 and SW480 cells. These data suggest that activation of NF-κB is indispensable for GW9508-induced release of angiogenic factors in CRC cells.
GPR120 signaling promotes angiogenesis through activation of the PI3K/Akt–NF-κB pathway. (a) Src or GPR120 KD cells were seeded in 6-well plates and were treated with GW9508 (10 μM) for the indicated period. P-Akt, T-Akt, P-IκBα and T-IκBα expression was measured by western blotting. β-actin was used as the loading control. The results shown are representative of three independent experiments. (b) Src or GPR120 KD cells were seeded in 6-well plates and were treated with PI3K inhibitor LY294002 (20 μM) or NF-κB inhibitor BAY 11-7082 (10 μM) for 30 min before GW9508 treatment (10 μM) for 8 h. VEGF, IL-8 and COX-2 mRNA abundance was measured by quantitative real-time PCR. Data were expressed as the mean±s.e.m. of three independent experiments. *P<0.05, **P<0.01. (c) Src or GPR120 KD cells were seeded in 6-well plates and were treated with PI3K inhibitor LY294002 (20 μM) for 30 min before GW9508 treatment (10 μM) for 30 min. P-Akt and P-IκBα levels were measured by western blotting. β-actin was used as the loading control. The results shown are representative of three independent experiments. (d) HCT 116 and SW480 cells (Src and GPR120 KD) were transfected with scramble siRNA (siRNA control), siRNA targeting Akt (Akt siRNA), or siRNA targeting IκBα (IκBα siRNA). siRNA cell lines exhibited a marked reduction in Akt or IκBα protein level compared with siRNA control. (e) Src or GPR120 KD cells were treated with siRNA to knock down Akt or IκBα, and then were seeded in 6-well plates and were stimulated with GW9508 (10 μM) for 8 h. VEGF, IL-8 and COX-2 mRNA abundance was measured by real-time PCR. Data were expressed as the mean±s.e.m. of three independent experiments. *P<0.05, **P<0.01. (f) HUVECs were treated with 0.5% FBS (control), or siRNA-CM. Tube formation was quantified in three randomly selected fields. Bars represent mean number of branch points ±s.e.m. of three independent experiments. *P<0.05, **P<0.01.
As the IκBα/NF-κB pathway can be activated by Akt,17, 18, 19 and GRP120 signaling can stimulate phosphorylation of Akt,8 our next step was to test whether PI3K/Akt signaling was involved in GW9508-induced activation of NF-κB. As shown in Figure 4a, the level of phosphorylated-Akt was indeed elevated in GW9508-stimulated HCT 116 and SW480 cells, whereas GPR120 depletion by shRNA blocked the activation of Akt. However, western blotting analysis showed that the observed increases in IκBα phosphorylation after GW9508 stimulation were reversed by pretreatment with the PI3K inhibitor LY294002 (20 μM). This indicated that GPR120 signaling mediated IκBα/NF-κB through the PI3K/Akt pathway (Figure 4c). Moreover, real-time PCR analysis showed thst LY294002 inhibited GW9508-induced induction of VEGF, IL-8 and COX-2 in HCT 116 and SW480 cells (Figure 4b). This suggested that activation of PI3K/Akt was essential for the GPR120 signaling-mediated induction of proangiogenic genes.
Next, we performed RNA interference of Akt and IκBα (to exclude the possible effects of inhibitors on HUVECs) to examine if angiogenesis mediated by GPR120 ligation was dependent on PI3K/Akt–NF-κB pathway. We found that knocking down these genes indeed eliminated the effect of GPR120-induced proangiogenic gene expression (Figure 4e). As shown in Figure 4f, knock down of PI3K/Akt–NF-κB pathway in HCT 116 and SW480 cells significantly impaired GW9508-induced effects on endothelial branching. Taken together, our results indicate that angiogenesis enhanced by GPR120 signaling is mediated by the PI3K/Akt–NF-κB pathway through regulating angiogenic factors.
Activation of GPR120 enhances migration and induces EMT of CRC cells
As recent evidence showed that ω-3 fatty acid (FA) treatment can inhibit migration of primary WT macrophages by signaling through GPR120,8 we sought to determine whether GPR120 signaling affects motility in CRC cells. We measured the migratory capability of HCT 116 and SW480 cells using an in vitro transwell chemotaxis assay. As shown in Figure 5a, pretreatment of cancer cells with GW9508 for 72 h before exposure to fetal bovine serum (FBS)-containing media led to a significant increase in chemotactic capacity of tumor cells, but had no evident effect on GPR120-knockdown cells. Overexpression of GPR120 in GPR120-knockdown cells was sufficient to restore the migratory capability in response to GW9508 stimulation (Supplementary Figure 1b).
Activation of GPR120 enhances migration of CRC cells. (a) Migratory capacity of Src or GPR120 KD cells was measured using a transwell migration assay. Src or GPR120 KD cells were stimulated with or without GW9508 (10 μM) for 72 h, and then transferred to the top chambers of 24-well transwell insert chambers. After 24 h, the cells that migrated into the lower chambers were stained with crystal violet and counted. Magnification, × 100. Bars represent fold-change of mean number of migrating cells ±s.e.m. of three independent experiments compared with src cells. *P<0.05, **P<0.01. (b) Src or GPR120 KD cells were seeded in 6-well plates and stimulated with GW9508 (10 μM) for the indicated times. Differentiated epithelial marker (E-cadherin) and mesenchymal marker (N-cadherin, vimentin) expression was measured by western blotting. The results shown were representative of three independent experiments.
The EMT process can promote motility of tumor cells by decreasing epithelial (E-cadherin) and increasing mesenchymal markers (N-cadherin, vimentin). To test whether GRP120 signaling can induce EMT, we performed western blotting to detect the expression of EMT markers in CRC cells after GPR120 activation. As shown in Figure 5b, GPR120 signaling reduced E-cadherin, and enhanced N-cadherin and vimentin expression in HCT 116 and SW480 cells. However, all these effects of GW9508 were abrogated by the depletion of GPR120 with shRNA. Reintroduction of GPR120 in GPR120-knockdown cell lines was sufficient to restore EMT in response to GW9508 stimulation (Supplementary Figure 1c). These data collectively suggest that GPR120 signaling may induce EMT to enhance motility of tumor cells.
Activation of GPR120 promotes angiogenesis and tumor growth in vivo
To investigate whether GPR120 signaling can accelerate malignant progression in vivo, we further examined the effects of GPR120 signaling on HCT 116 xenografts in nude mice. We generated subcutaneous xenograft tumors using two cell lines: HCT 116 transfected with negative control (HCT 116-Src) or GPR120 shRNA-expressing constructs (HCT 116-GPR120 KD). Mice were injected intraperitoneal daily with either 10 mg/kg of GW9508 or vehicle alone, from the first day of cell implantation. As shown in Figure 6a, from day 6, tumors derived from HCT 116-Src cells treated with GW9508 grew significantly faster than the control tumors treated with vehicle (P<0.001). Next, we analyzed tumors for proliferation index using Ki67 staining in tumor biopsies obtained from each group of mice (n=5). The proliferation rates (Ki67 Labeling Index) of tumors from mice treated with GW9508 were significantly higher, as compared with those from mice treated with vehicle (Figure 6b). The proliferation-promoting effect of GW9508 was abrogated by the deletion of GPR120.
GPR120 activation promotes tumor growth of HCT 116 cells in a xenograph mouse model. (a) Xenograft model in nude mice. Four different sets of nude mice (BALB/C nu/nu, n=5 for each group, Src+GW9508, GPR120 KD+GW9508, Src+Vehicle and GPR120 KD+Vehicle) were injected subcutaneously. Tumors were measured every 3 days. Data were expressed as the mean size ±s.e.m. (b) Ki67-positive cell numbers were determined in individual xenograft tumors. Representative IHC stains of tumors from each group of mice were shown. Magnification, × 400. Scale bar, 50 μm. Bars represent the mean percentage of Ki67-positive cells ±s.e.m. (c) Changes in VEGF, IL-8 and COX-2 mRNA expression and their products (VEGF, IL-8 and PGE2) in tumors of different groups were measured by real-time PCR and enzyme-linked immunosorbent assay, respectively. (d) Representative examples of immunofluorescence staining analyses of CD31 in tumor tissues from HCT116 xenografts. Magnification, × 400. Bars represent fold-change of the mean number of CD31-positive cells ±s.e.m. compared with the src+Vehicle group. (e) Representative examples of IHC staining analyses of EMT markers in tumors of each group of mice. Magnification, × 400. Scale bar, 50 μm.
To investigate whether GPR120 signaling can promote angiogenesis in vivo, we detected changes in proangiogenic gene expression and their products in tumors of the different groups. As shown in Figure 6c, proangiogenic genes and their products were markedly increased in tumors from mice treated with GW9508. Meanwhile, tumor samples were analyzed by immunofluorescent staining for CD31. Compared with tumors from mice treated with vehicle, the microvascular density (CD31-positivity) of tumors of mice treated with GW9508 was significantly higher (Figure 6d), indicating that GPR120 signaling promoted new blood vessel formation. These data suggest that GPR120 signaling promotes CRC tumor growth in vivo, probably through enhanced angiogenesis.
Furthermore, we analyzed EMT markers in tumor samples to test whether GRP120 signaling could induce EMT in vivo. We observed that epithelial marker E-cadherin expression was reduced, and mesenchymal marker vimentin expression was enhanced in tumors from GW9508-treated mice (Figure 6e). Altogether, all of these results fully supported our in vitro observations of proangiogenic and EMT inducing characteristics of GPR120 signaling.
GPR120 correlates with VEGF and E-cadherin expression in human CRC
Based on the above evidence, which provided a link between GPR120 signaling and angiogenesis/migration, we finally sought to determine whether GPR120 expression correlates with angiogenesis and migration capability of CRC cell lines. Indeed, cell lines with high GPR120 expression had greater proangiogenic capacity (Figure 7a). The chemotactic activity also correlates with GPR120 in seven out of eight CRC cell lines (Figure 7b). Furthermore, we detected angiogenic factor VEGF and EMT marker E-cadherin in human CRC according to the levels of expression of GPR120. Entire sections of each CRC case were analyzed to derive staining scores for GPR120, VEGF and E-cadherin expression, respectively, and used for statistical analyses. We found that high levels of GPR120 were associated with high VEGF and low E-cadherin (Figure 7c and Table 2). These results strongly suggested that GPR120 expression could increase tumor progression in vitro and in vivo.
GPR120 expression correlates with angiogenesis and migration capacity in CRC cells and human CRC. (a, b) Spearman rank correlation analysis of GPR120 mRNA and angiogenesis capacity in eight CRC cell lines (a), and migration capacity in seven out of eight CRC cell lines (b). (c) IHC staining of GPR120, VEGF and E-cadherin in serial sections of human CRC. Examples of patients with low and high levels of GPR120 expression are displayed. Magnification, × 200. Scale bar, 100 μm.
Discussion
GPR120 functions as a receptor/sensor for ω-3 FAs. As it is expressed in enteroendocrine L cells, proinflammatory M1-like macrophages and mature adipocytes, past interest in this receptor has focused on its potential ability to regulate metabolism, inflammation and adipogenesis. In the current study, we aimed to investigate whether GPR120 signaling could modify the development and progression of human CRC and explore the underlying mechanisms. Here, we identified GPR120 as a tumor-promoting receptor that enhances angiogenesis and the motility of human CRC.
Endogenous expression of GPR120 was found in the intestines of humans and mice. Herein, we found that GPR120 was expressed in human normal colorectal epithelium. Strikingly, we detected significantly higher GPR120 expression in a large cohort of human CRC tissues and a panel of malignant CRC cell lines. A recent study showed that GPR120 expression in adipose tissue was significantly higher in obese individuals than in lean controls in human. However, one of nonsynonymous GPR120 variants lost the ability to transduce the signal of long-chain free fatty acids.9 This study prompted us to detect whether overexpressed GPR120 in CRC cells could respond to ligand stimulation, which was the basis of its biology. Overexpressed GPR120 in these CRC cells was functional and signaled via a Gαq/11-coupled pathway, similar to GPR120-expressing RAW 264.7 cells and mature adipocytes.8 In addition, GPR120 levels significantly correlated with clinical characteristics of CRC, including clinical stage, pathologic differentiation and lymph node metastasis. These observations prompted us to investigate the potential roles of GPR120-mediated signaling in the development of CRC. Interestingly, our findings are consistent with a recent study published by Mano’s group, who found that FFAR2 (also known as GPR43), a receptor for short-chain FAs, was increased and associated with malignant transformation in Gallbladder cancer.20
The growth and metastasis of CRC is dependent on the development of neo-vessels. Angiogenesis is regulated by a balance of proangiogenic and angiostatic factors.21, 22 Therefore, identification of proangiogenic genes and their products that lead to angiogenesis is critical for providing new potential therapeutic targets. In current oncological practice, the VEGF-targeted agent bevacizumab has been established as a first-line treatment for metastatic CRC,23, 24, 25 suggesting especially important roles for angiogenic factors in CRC progression. Here, we showed that GPR120 signaling promoted angiogenesis by inducing secretion of proangiogenic factors VEGF, IL-8 and COX-2-derived PGE2 in vitro and in xenograph mouse model. Although VEGF is known to be central and IL-8 and PGE2 are key regulators in angiogenesis, it is possible that activation of GPR120 may activate other cytokines to mediate angiogenesis, as a full proangiogenic signature was not analyzed. Furthermore, we found that GPR120 and VEGF positively correlated in CRC specimens, suggesting that GPR120 signaling might promote VEGF expression in vivo. All of these data raised the possibility that GPR120 signaling-induced VEGF, IL-8 and COX-2-derived PGE2 promoted tumor cell switching to an angiogenic phenotype, leading to tumor growth and progression.
Our results also revealed the molecular mechanisms underlying these proangiogenic effects of GPR120 signaling. It has been demonstrated that NF-κB has important roles in the development of malignant phenotypes, and aberrant activation of NF-κB is observed in a variety of cancer types.17, 26 The NF-κB pathway functions in cancer progression through mediating tumor-associated angiogenesis and inflammation.27, 28 Numerous proangiogenic and proinflammatory genes, such as VEGF, IL-8 and COX-2, are transcriptionally regulated by the NF-κB pathway.16 We found that GW9508 treatment elicited phosphorylated-IκBα at Ser32 in CRC cells, which is essential for the release of active NF-κB. However, blocking the activation of IκBα completely abrogated GPR120 signaling-induced production of VEGF, IL-8 and COX-2, and angiogenesis. On the other hand, although the IκB/NF-κB axis is subjected to activation by a variety of distinct upstream signals, our data suggested an involvement of the PI3K/Akt pathway, which was indeed activated by GW9508 stimulation. Suppression of PI3K/Akt signaling in CRC cells abrogated GW9508-induced effects on activation of NF-κB and subsequent inhibition of VEGF, IL-8 and COX-2 expression, and angiogenesis. This implied a seemingly linear relation of the two signaling molecules along the action axis. The results are consistent with the findings that the PI3K/Akt–NF-κB pathway has an important role in tumor-associated angiogenesis mediated by aberrant GPCR signaling.17, 18, 19
Migration and invasion are important prerequisites of tumor progression and metastasis. Although the mechanisms of migration are still poorly understood, EMT and mesenchymal–epithelial transition is a good model to explain how solid tumors metastasize from the site of origin to a new site.29,30,31 Herein, we showed that GPR120 signaling promoted migration and induced EMT of CRC cells in vitro and in xenograph mouse model. Furthermore, we found that expression of GPR120 and E-cadherin was inversely correlated in CRC specimens, suggesting that GPR120 might induce EMT in vivo. This model is similar to the transforming growth factor-β1-induced EMT process.32, 33 However, it has been reported that GPR120 signaling inhibited the ability of primary macrophages to migrate toward adipocyte CM.8 It seems a single GPCR can independently induce different effects in different cell types by different mechanisms. It would be of great interest to reveal the mechanistic differences in GPR120 signaling-induced effects in different cell types.
Although we showed that GPR120 signaling indeed induces angiogenesis in CRC cells in vivo and in vitro, it is possible that additional mechanisms of tumor promotion also exist in vivo. One possibility is that in vivo, activation of GPR120 induces the transdifferentiation of inflammatory M1 to anti-inflammatory M2 macrophages in the tumor microenviroment. Indeed, GPR120 increases the presence of anti-inflammatory M2 macrophages in adipose tissue in mice fed a high-fat diet.8 Here, we showed that GPR120 signaling promoted tumor growth in nude mice, but it is not clear whether GPR120 signaling induces the phenotype transition of macrophages, and whether this transition contributes to tumor progression. Given the importance of tumor-associated macrophages, especially M2 macrophages, in the regulation of tumor development, it is essential to perform further investigations.
It is well known that the endogenous ligands of GPR120 are ω-3 FAs such as docosahexaenoic acid (DHA) and eicosapentaenoic acid (EPA), which are mainly found in fish oil. Several studies have shown that DHA or EPA has anti-tumor effects.34, 35 However, the mechanisms underlying the effects of ω-3 FAs on tumor progression are complex. DHA is known to incorporate into biological membranes to alter membrane-domain organization and also to act as ligands of nuclear peroxisome proliferator-activated receptors.36,37 For these studies in vitro, researchers used ω-3 FAs dissolved in bovine serum albumin-containing vehicle. However, when ω-3 FAs were dissolved in bovine serum albumin-containing vehicle, they were not able to activate GPR120 in vitro7, 37 and protein-bound forms of ω-3 FAs are supposed to be more relevant in blood and exudates. Furthermore, DHA and EPA are believed to be conjugated to albumin in vivo. Therefore, it seems these anti-tumor effects are independent of GPR120 signaling because GPR120 in vitro is not activated by DHA in bovine serum albumin-containing media. However, through the action of lipoprotein lipase bound to the luminal surface of endothelial cells, ω-3 FAs are cleaved from circulating triglycerides, where they can act as ligands or be taken up by peripheral tissues.8,38 This small proportion (∼5%) of total plasma DHA in the FFA pool may trigger GPR120 signaling in CRC cells, resulting in tumor progression in vivo. More recently, a report showed that cis-platinum could induce poly-unsaturated FAs at the tumor sites, which protected tumor cells against a range of chemotherapeutics.39 This study implies that, in addition to dietary DHA and EPA, activated cells in the tumor microenviroment could also release poly-unsaturated FAs to modify tumor development through GPR120 signaling.
In conclusion, we established that GPR120 functioned as a tumor-promoting receptor in human CRC. After ligand stimulation, GPR120 signaling promoted angiogenesis mainly through regulating proangiogenic factors VEGF, IL-8 and COX-2-derived PGE2, mediated by the PI3K/Akt–NF-κB signal pathway. We also found that activation of GPR120 promoted migration and induced EMT of CRC cells. This discovery provides mechanistic insight into recent studies linking lipidomics to the development of cancers. Additionally, our discovery suggests a novel role for GPR120 as a target for treatment of CRC. Finally, our findings may have implications for the use of commercially available fish oil products or drugs targeting GPR120 signaling for treatment of metabolic and inflammatory diseases, such as obesity and type 2 diabetes in cancer patients.
Materials and methods
Patients and specimens
Paraffin-embedded CRC samples were collected from patients undergoing curative-intent surgery at the Department of Surgery, Renji Hospital, Shanghai Jiao Tong University School of Medicine between 2008 and 2011. There were also 90 normal colorectal tissue samples adjacent to CRC (used as controls). The histologic sections were reviewed by two expert pathologists to verify the histologic diagnosis. None of the patients had received any preoperative treatment. Tumors were staged according to the American Joint Committee on Cancer pathologic tumor–lymph node–metastasis classification. Informed consent was obtained from all study subjects before sample collection and these samples were used according to ethical standards.
Cell culture
All human CRC and normal colorectal cell lines were purchased from American type culture collection (ATCC, Manassas, VA, USA). These cell lines were routinely maintained in our laboratory according to the instructions from ATCC. Before GW9508 stimulation, cells were cultured in serum-free corresponding medium with antibiotics for 12 h to minimize the influence of FBS.
Cell line transfection and transduction
Lentiviral shRNA vectors (GenePharma, Shanghai, China) targeting human GPR120 were utilized for stable knockdown in CRC cells. Procedures were conducted according to the manufacturer’s protocol. SiRNA sequences (GPR120: 5′-GAGCAGCTTGCTTCTGAAG-3′; scramble: 5′-AGGACTGAGTGTACCGTCT-3′) were designed into shRNA and inserted into the vector PLVX-shRNA1 under U6 promoter. Cells resistant to puromycin (2 μg/ml) were selected and passaged for further study.
IHC, interpretation and evaluation of IHC results
Sections were subjected to routine IHC staining as described previously.40 IHC staining was independently examined by two clinical pathologists who were unaware of the patient outcome. Interpretation and evaluation of IHC results was as described previously.40
Cell migration assay
Twenty four-well transwell insert chambers (Merck KgaA, Darmstadt, Germany) were used for cell migration assy. One lakh cells (serum-starved overnight and then treated with or without GW9508 for 72 h before the assay) were added to the top chambers in serum-free medium (200 μl), and the bottom chambers were filled with medium containing 10% FBS. Cells were cultured for 24 h at 37 °C in a 5% CO2-humidified incubator. To quantify migration, cells were removed from the top-side of the membrane using a cotton-tipped swab, and migrating cells attached to the bottom of the membrane were fixed with 4% paraformaldehyde and stained with crystal violet solution. Cell number from five representative fields was counted for each insert using microscopy. The average cell number/field from the control group was set as the baseline (one fold), and was compared with the treatment groups (fold change=treatment group cells/field÷control group cells/field).
In vitro angiogenesis assay
ECMatrix (50 μl, Merck KGaA ) was distributed per well in a 96-well plate. HUVECs (ALLCELLS, Shanghai, China, 2 × 104 cells/well) suspended in 100 μl of medium supplemented with 0.5% FBS were added to each well and cultured in triplicate with 150 μl of CM from either Src or GPR120 KD cells at 37 °C. After 12 h, images were captured and branch points in three random view-fields per well were counted and the values were averaged.
Tumorigenicity assays with nude mice
Six-week old BALB/c (nu/nu) nude mice were purchased from Jackson ImmunoResearch Laboratories. Animals were housed in a specific pathogen-free facility at the Chinese Academy of Sciences. Animal protocols were approved by the Institutional Review Board of the Institute of Health Sciences, as previously described.41 Mice were injected subcutaneously into the flanks with 5 × 106 HCT 116 Src or GPR120 KD cells suspended in phosphate-buffered saline. Five animals were used in each group. Tumor volume was estimated by using the formula width2 × length × 0.52 in mm3. At day 30, mice were euthanized, and the tumors were removed for further experiments. IHC was performed on paraffin-embedded tumor sections using mouse anti-human Ki67 mAb (clone: MIB-1; Dako, Glostrup, Denmark). Ten random fields with the highest concentrations of Ki67-positive nuclei were used for counting the Ki67-positive cells. The Ki67 Labeling Index has been defined as the percentage of Ki67-positive cells to all nuclei.
Statistical analysis
Differences were evaluated using Statistical Package for Social Science software (SPSS, Version 17.0, Chicago, IL, USA). The association of staining intensity with clinicopathologic patterns was assessed using the χ2-test and two-sided Fisher’s exact test to determine the significance of the difference between the covariates. The correlations between expression of GPR120 and VEGF or E-cadherin were assessed with the χ2-test or the Spearman rank test. All measurement data are presented as mean±s.e.m. Statistical significance was evaluated by the Student’s t-test. Values of P<0.05 were considered to be statistically significant.
References
Jemal A, Siegel R, Ward E, Hao Y, Xu J, Murray T et al. Cancer statistics, 2008. CA Cancer J Clin 2008; 58: 71–96.
Taborga M, Corcoran KE, Fernandes N, Ramkissoon SH, Rameshwar P . G-coupled protein receptors and breast cancer progression: potential drug targets. Mini Rev Med Chem 2007; 7: 245–251.
Oh da Y, Lagakos WS . The role of G-protein-coupled receptors in mediating the effect of fatty acids on inflammation and insulin sensitivity. Curr Opin Clin Nutr Metab Care 2011; 14: 322–327.
Hara T, Hirasawa A, Ichimura A, Kimura I, Tsujimoto G . Free fatty acid receptors FFAR1 and GPR120 as novel therapeutic targets for metabolic disorders. J Pharm Sci 2011; 100: 3594–3601.
Oh da Y, Olefsky JM . Omega 3 fatty acids and GPR120. Cell Metab 2012; 15: 564–565.
Tanaka T, Katsuma S, Adachi T, Koshimizu TA, Hirasawa A, Tsujimoto G . Free fatty acids induce cholecystokinin secretion through GPR120. Naunyn Schmiedebergs Arch Pharmacol 2008; 377: 523–527.
Hirasawa A, Tsumaya K, Awaji T, Katsuma S, Adachi T, Yamada M et al. Free fatty acids regulate gut incretin glucagon-like peptide-1 secretion through GPR120. Nat Med 2005; 11: 90–94.
Oh DY, Talukdar S, Bae EJ, Imamura T, Morinaga H, Fan W et al. GPR120 is an omega-3 fatty acid receptor mediating potent anti-inflammatory and insulin-sensitizing effects. Cell 2010; 142: 687–698.
Ichimura A, Hirasawa A, Poulain-Godefroy O, Bonnefond A, Hara T, Yengo L et al. Dysfunction of lipid sensor GPR120 leads to obesity in both mouse and human. Nature 2012; 483: 350–354.
Itoh Y, Kawamata Y, Harada M, Kobayashi M, Fujii R, Fukusumi S et al. Free fatty acids regulate insulin secretion from pancreatic beta cells through GPR40. Nature 2003; 422: 173–176.
Briscoe CP, Peat AJ, McKeown SC, Corbett DF, Goetz AS, Littleton TR et al. Pharmacological regulation of insulin secretion in MIN6 cells through the fatty acid receptor GPR40: identification of agonist and antagonist small molecules. Br J Pharmacol 2006; 148: 619–628.
Briscoe CP, Tadayyon M, Andrews JL, Benson WG, Chambers JK, Eilert MM et al. The orphan G protein-coupled receptor GPR40 is activated by medium and long chain fatty acids. J Biol Chem 2003; 278: 11303–11311.
Kotarsky K, Nilsson NE, Flodgren E, Owman C, Olde B . A human cell surface receptor activated by free fatty acids and thiazolidinedione drugs. Biochem Biophys Res Commun 2003; 301: 406–410.
Fukata M, Chen A, Vamadevan AS, Cohen J, Breglio K, Krishnareddy S et al. Toll-like receptor-4 promotes the development of colitis-associated colorectal tumors. Gastroenterology 2007; 133: 1869–1881.
Wang D, Mann JR, DuBois RN . The role of prostaglandins and other eicosanoids in the gastrointestinal tract. Gastroenterology 2005; 128: 1445–1461.
Wang S, Liu Z, Wang L, Zhang X . NF-kappaB signaling pathway, inflammation and colorectal cancer. Cell Mol Immunol 2009; 6: 327–334.
Song L, Xiong H, Li J, Liao W, Wang L, Wu J et al. Sphingosine kinase-1 enhances resistance to apoptosis through activation of PI3K/Akt/NF-kappaB pathway in human non-small cell lung cancer. Clin Cancer Res 2011; 17: 1839–1849.
Cheng JC, Chou CH, Kuo ML, Hsieh CY . Radiation-enhanced hepatocellular carcinoma cell invasion with MMP-9 expression through PI3K/Akt/NF-kappaB signal transduction pathway. Oncogene 2006; 25: 7009–7018.
Kane LP, Shapiro VS, Stokoe D, Weiss A . Induction of NF-kappaB by the Akt/PKB kinase. Curr Biol 1999; 9: 601–604.
Hatanaka H, Tsukui M, Takada S, Kurashina K, Choi YL, Soda M et al. Identification of transforming activity of free fatty acid receptor 2 by retroviral expression screening. Cancer Sci 2010; 101: 54–59.
Sakurai T, Kudo M . Signaling pathways governing tumor angiogenesis. Oncology 2011; 81 (Suppl 1): 24–29.
Wang Y, Alam GN, Ning Y, Visioli F, Dong Z, Nor JE et al. The unfolded protein response induces the angiogenic switch in human tumor cells through the PERK/ATF4 pathway. Cancer Res 2012; 15: 5396–5406.
Yeung Y, Tebbutt NC . Bevacizumab in colorectal cancer: current and future directions. Expert Rev Anticancer Ther 2012; 12: 1263–1273.
Strickler JH, Hurwitz HI . Bevacizumab-based therapies in the first-line treatment of metastatic colorectal cancer. Oncologist 2012; 17: 513–524.
Koukourakis GV, Sotiropoulou-Lontou A . Targeted therapy with bevacizumab (Avastin) for metastatic colorectal cancer. Clin Transl Oncol 2011; 13: 710–714.
Romashkova JA, Makarov SS . NF-kappaB is a target of AKT in anti-apoptotic PDGF signalling. Nature 1999; 401: 86–90.
Strieter RM . Masters of angiogenesis. Nat Med 2005; 11: 925–927.
Greten FR, Eckmann L, Greten TF, Park JM, Li ZW, Egan LJ et al. IKKbeta links inflammation and tumorigenesis in a mouse model of colitis-associated cancer. Cell 2004; 118: 285–296.
Kalluri R . EMT: when epithelial cells decide to become mesenchymal-like cells. J Clin Invest 2009; 119: 1417–1419.
Zheng HX, Cai YD, Wang YD, Cui XB, Xie TT, Li WJ et al. Fas signaling promotes motility and metastasis through epithelial-mesenchymal transition in gastrointestinal cancer. Oncogene 2013; 32: 1183–1192.
Williams K, Ghosh R, Vummidi Giridhar P, Gu G, Case T, Belcher SM et al. Inhibition of Stathmin1 Accelerates the Metastatic Process. Cancer Res 2012; 72: 5407–5417.
Wendt MK, Schiemann BJ, Parvani JG, Lee YH, Kang Y, Schiemann WP . TGF-beta stimulates Pyk2 expression as part of an epithelial-mesenchymal transition program required for metastatic outgrowth of breast cancer. Oncogene 2013; 32: 2005–2015.
Wu YY, Peck K, Chang YL, Pan SH, Cheng YF, Lin JC et al. SCUBE3 is an endogenous TGF-beta receptor ligand and regulates the epithelial-mesenchymal transition in lung cancer. Oncogene 2011; 30: 3682–3693.
Habbel P, Weylandt KH, Lichopoj K, Nowak J, Purschke M, Wang JD et al. Docosahexaenoic acid suppresses arachidonic acid-induced proliferation of LS-174T human colon carcinoma cells. World J Gastroenterol 2009; 15: 1079–1084.
Hossain Z, Hosokawa M, Takahashi K . Growth inhibition and induction of apoptosis of colon cancer cell lines by applying marine phospholipid. Nutr Cancer 2009; 61: 123–130.
Turk HF, Barhoumi R, Chapkin RS . Alteration of EGFR spatiotemporal dynamics suppresses signal transduction. PLoS One 2012; 7: e39682.
Im DS . Omega-3 fatty acids in anti-inflammation (pro-resolution) and GPCRs. Prog Lipid Res 2012; 51: 232–237.
Polozova A, Salem N Jr . Role of liver and plasma lipoproteins in selective transport of n-3 fatty acids to tissues: a comparative study of 14C-DHA and 3H-oleic acid tracers. J Mol Neurosci 2007; 33: 56–66.
Roodhart JM, Daenen LG, Stigter EC, Prins HJ, Gerrits J, Houthuijzen JM et al. Mesenchymal stem cells induce resistance to chemotherapy through the release of platinum-induced fatty acids. Cancer Cell 2011; 20: 370–383.
Xu H, Wu Q, Dang S, Jin M, Xu J, Cheng Y et al. Alteration of CXCR7 expression mediated by TLR4 promotes tumor cell proliferation and migration in human colorectal carcinoma. PLoS One 2011; 6: e27399.
Zhao F, Zhang Y, Wang H, Jin M, He S, Shi Y et al. Blockade of osteopontin reduces alloreactive CD8+ T cell-mediated graft-versus-host disease. Blood 2011; 117: 1723–1733.
Acknowledgements
We thank Dr G Brewer (University of Medicine and Dentistry of New Jersey) for his critical review of the manuscript. This work was supported by the Ministry of Science and Technology of China (2011CB966200, 2010CB945600), the Strategic Priority Research Program of the Chinese Academy of Sciences (XDA01040000), the Program of Chinese Academy of Sciences (KSCX1-YW-22), the National Natural Science Foundation of China (81071748, 30873045, 81130057), the China Postdoctoral Science Foundation (2012M510906) and the Leading Academic Discipline Project of Shanghai Municipal Education Commission (J50207).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Oncogene website
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Wu, Q., Wang, H., Zhao, X. et al. Identification of G-protein-coupled receptor 120 as a tumor-promoting receptor that induces angiogenesis and migration in human colorectal carcinoma. Oncogene 32, 5541–5550 (2013). https://doi.org/10.1038/onc.2013.264
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2013.264
Keywords
This article is cited by
-
GPR120 prevents colorectal adenocarcinoma progression by sustaining the mucosal barrier integrity
Scientific Reports (2022)
-
New aspects of amino acid metabolism in cancer
British Journal of Cancer (2020)
-
Aberrant fatty acid profile and FFAR4 signaling confer endocrine resistance in breast cancer
Journal of Experimental & Clinical Cancer Research (2019)
-
GPR119 agonist enhances gefitinib responsiveness through lactate-mediated inhibition of autophagy
Journal of Experimental & Clinical Cancer Research (2018)
-
CD90 determined two subpopulations of glioma-associated mesenchymal stem cells with different roles in tumour progression
Cell Death & Disease (2018)