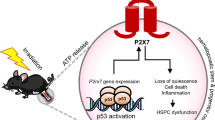
Abstract
Inadvertent mammalian tissue exposures to low doses of ionizing radiation (IR) after radiation accidents, remediation of radioactive-contaminated areas, space travel or a dirty bomb represent an interesting trauma to an organism. Possible low-dose IR-induced bystander effects could impact our evaluation of human health effects, as cells within tissue are not equally damaged after doses of IR ⩽10 cGy. To understand tissue responses after low IR doses, we generated a reporter system using the human clusterin promoter fused to firefly luciferase (hCLUp-Luc). Secretory clusterin (sCLU), an extracellular molecular chaperone, induced by low doses of cytotoxic agents, clears cell debris. Low-dose IR (⩾2 cGy) exposure induced hCLUp-Luc activity with peak levels at 96 h, consistent with endogenous sCLU levels. As doses increased (⩾1 Gy), sCLU induction amplitudes increased and time-to-peak response decreased. sCLU expression was stimulated by insulin-like growth factor-1, but suppressed by p53. Responses in transgenic hCLUp-Luc reporter mice after low IR doses showed that specific tissues (that is, colon, spleen, mammary, thymus and bone marrow) of female mice induced hCLUp-Luc activity more than male mice after whole body (⩾10 cGy) irradiation. Tissue-specific, non-linear dose- and time-responses of hCLUp-Luc and endogenous sCLU levels were noted. Colon maintained homeostatic balance after 10 cGy. Bone marrow responded with delayed, but prolonged and elevated expression. Intraperitoneal administration of α-transforming growth factor (TGF)β1 (1D11), but not control (13C4) antibodies, immediately following IR exposure abrogated CLU induction responses. Induction in vivo also correlated with Smad signaling by activated TGFβ1 after IR. Mechanistically, media with elevated sCLU levels suppressed signaling, blocked apoptosis and increased survival of TGFβ1-exposed tumor or normal cells. Thus, sCLU is a pro-survival bystander factor that abrogates TGFβ1 signaling and most likely promotes wound healing.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Goetz E, Shankar S, Zou Y, Morales X, Lou X, Araki S et al. ATM-dependent IGF-1 induction regulates secretory clusterin expression after DNA damage and in genetic instability. Oncogene 2011; 30: 3745–3754.
Alexander A, Cai SL, Kim J, Nanez A, Sahin M, MacLean KH et al. ATM signals to TSC2 in the cytoplasm to regulate mTORC1 in response to ROS. Proc Natl Acad Sci USA 2010; 107: 4153–4158.
Guo Z, Kozlov S, Lavin MF, Person MD, Paull TT . ATM activation by oxidative stress. Science 2010; 330: 517–521.
Sfeir A, Kabir S, van Overbeek M, Celli GB, de Lange T . Loss of Rap1 induces telomere recombination in the absence of NHEJ or a DNA damage signal. Science 2010; 327: 1657–1661.
Cornelissen B, Kersemans V, Darbar S, Thompson J, Shah K, Sleeth K . Imaging DNA damage in vivo using {gamma}H2AX-targeted immunoconjugates. Cancer Res 2011; 71: 4539–4549.
Redon CE, Dickey JS, Bonner WM, Sedelnikova OA . gamma-H2AX as a biomarker of DNA damage induced by ionizing radiation in human peripheral blood lymphocytes and artificial skin. Adv Space Res 2009; 43: 1171–1178.
Bhogal N, Kaspler P, Jalali F, Hyrien O, Chen R, Hill RP et al. Late residual gamma-H2AX foci in murine skin are dose responsive and predict radiosensitivity in vivo. Radiat Res 2010; 173: 1–9.
Lee TK, Allison RR, O’Brien KF, Naves JL, Karlsson UL, Wiley AL . Persistence of micronuclei in lymphocytes of cancer patients after radiotherapy. Radiat Res 2002; 157: 678–684.
Nachtrab U, Oppitz U, Flentje M, Stopper H . Radiation-induced micronucleus formation in human skin fibroblasts of patients showing severe and normal tissue damage after radiotherapy. Int J Radiat Biol 1998; 73: 279–287.
Lindholm C, Stricklin D, Jaworska A, Koivistoinen A, Paile W, Arvidsson E et al. Premature chromosome condensation (PCC) assay for dose assessment in mass casualty accidents. Radiat Res 2010; 173: 71–78.
Freund A, Patil CK, Campisi J . p38MAPK is a novel DNA damage response-independent regulator of the senescence-associated secretory phenotype. Embo J 2011; 30: 1536–1548.
Rodier F, Munoz DP, Teachenor R, Chu V, Le O, Bhaumik D et al. DNA-SCARS: distinct nuclear structures that sustain damage-induced senescence growth arrest and inflammatory cytokine secretion. J Cell Sci 2011; 124: 68–81.
Arufe MC, De la Fuente A, Mateos J, Fuentes I, De Toro FJ, Blanco FJ . Analysis of the chondrogenic potential and secretome of mesenchymal stem cells derived from human umbilical cord stroma. Stem Cells Dev 2011; 20: 1199–1212.
Criswell T, Beman M, Araki S, Leskov K, Cataldo E, Mayo LD et al. Delayed activation of insulin-like growth factor-1 receptor/Src/MAPK/Egr-1 signaling regulates clusterin expression, a pro-survival factor. J Biol Chem 2005; 280: 14212–14221.
Criswell T, Klokov D, Beman M, Lavik JP, Boothman DA . Repression of IR-inducible clusterin expression by the p53 tumor suppressor protein. Cancer Biol Ther 2003; 2: 372–380.
Cardona-Gomez GP, Mendez P, DonCarlos LL, Azcoitia I, Garcia-Segura LM . Interactions of estrogens and insulin-like growth factor-I in the brain: implications for neuroprotection. Brain Res Brain Res Rev 2001; 37: 320–334.
Chi KN, Hotte SJ, Yu EY, Tu D, Eigl BJ, Tannock I et al. Randomized phase II study of docetaxel and prednisone with or without OGX-011 in patients with metastatic castration-resistant prostate cancer. J Clin Oncol 2010; 28: 4247–4254.
Zoubeidi A, Chi K, Gleave M . Targeting the cytoprotective chaperone, clusterin, for treatment of advanced cancer. Clin Cancer Res 2010; 16: 1088–1093.
Sutton D, Kim S, Shuai X, Leskov K, Marques JT, Williams BR et al. Efficient suppression of secretory clusterin levels by polymer-siRNA nanocomplexes enhances ionizing radiation lethality in human MCF-7 breast cancer cells in vitro. Int J Nanomedicine 2006; 1: 155–162.
Zhang H, Kim JK, Edwards CA, Xu Z, Taichman R, Wang CY . Clusterin inhibits apoptosis by interacting with activated Bax. Nat Cell Biol 2005; 7: 909–915.
Araki S, Israel S, Leskov KS, Criswell TL, Beman M, Klokov DY et al. Clusterin proteins: stress-inducible polypeptides with proposed functions in multiple organ dysfunction. BJR Suppl 2005; 27: 106–113.
Shannan B, Seifert M, Leskov K, Willis J, Boothman D, Tilgen W et al. Challenge and promise: roles for clusterin in pathogenesis, progression and therapy of cancer. Cell Death Differ 2006; 13: 12–19.
Snyder AR . Review of radiation-induced bystander effects. Hum Exp Toxicol [Review] 2004; 23: 87–89.
Yang CR, Leskov K, Hosley-Eberlein K, Criswell T, Pink JJ, Kinsella TJ et al. Nuclear clusterin/XIP8, an X-ray-induced Ku70-binding protein that signals cell death. Proc Natl Acad Sci USA 2000; 97: 5907–5912.
Yang CR, Yeh S, Leskov K, Odegaard E, Hsu HL, Chang C et al. Isolation of Ku70-binding proteins (KUBs). Nucleic Acids Res 1999; 27: 2165–2174.
Araki S, Eitel JA, Batuello CN, Bijangi-Vishehsaraei K, Xie XJ, Danielpour D et al. TGF-beta1-induced expression of human Mdm2 correlates with late-stage metastatic breast cancer. J Clin Invest 2010; 120: 290–302.
Davis TW, Wilson-Van Patten C, Meyers M, Kunugi KA, Cuthill S, Reznikoff C et al. Defective expression of the DNA mismatch repair protein, MLH1, alters G2-M cell cycle checkpoint arrest following ionizing radiation. Cancer Res 1998; 58: 767–778.
Trougakos IP, Djeu JY, Gonos ES, Boothman DA . Advances and challenges in basic and translational research on clusterin. Cancer Res 2009; 69: 403–406.
Jin G, Howe PH . Transforming growth factor beta regulates clusterin gene expression via modulation of transcription factor c-Fos. Eur J Biochem 1999; 263: 534–542.
Nguyen DH, Oketch-Rabah HA, Illa-Bochaca I, Geyer FC, Reis-Filho JS, Mao JH et al. Radiation acts on the microenvironment to affect breast carcinogenesis by distinct mechanisms that decrease cancer latency and affect tumor type. Cancer Cell 2011; 19: 640–651.
Dasch JR, Pace DR, Waegell W, Inenaga D, Ellingsworth L . Monoclonal antibodies recognizing transforming growth factor-beta. Bioactivity neutralization and transforming growth factor beta 2 affinity purification. J Immunol 1989; 142: 1536–1541.
Doi S, Zou Y, Togao O, Pastor JV, John GB, Wang L et al. Klotho inhibits transforming growth factor-beta1 (TGF-beta1) signaling and suppresses renal fibrosis and cancer metastasis in mice. J Biol Chem 2011; 286: 8655–8665.
Kirshner J, Jobling MF, Pajares MJ, Ravani SA, Glick AB, Lavin MJ et al. Inhibition of transforming growth factor-beta1 signaling attenuates ataxia telangiectasia mutated activity in response to genotoxic stress. Cancer Res 2006; 66: 10861–10869.
Wang Y, Yu Y, Tsuyada A, Ren X, Wu X, Stubblefield K et al. Transforming growth factor-beta regulates the sphere-initiating stem cell-like feature in breast cancer through miRNA-181 and ATM. Oncogene 2011; 30: 1470–1480.
Cipriano R, Kan CE, Graham J, Danielpour D, Stampfer M, Jackson MW . TGF-{beta} signaling engages an ATM-CHK2-p53-independent RAS-induced senescence and prevents malignant transformation in human mammary epithelial cells. Proc Nat Acad Sci USA 2011; 108: 8668–8673.
He Q, Montalbano J, Corcoran C, Jin W, Huang Y, Sheikh MS . Effect of Bax deficiency on death receptor 5 and mitochondrial pathways during endoplasmic reticulum calcium pool depletion-induced apoptosis. Oncogene 2003; 22: 2674–2679.
Trougakos IP, Lourda M, Antonelou MH, Kletsas D, Gorgoulis VG, Papassideri IS et al. Intracellular clusterin inhibits mitochondrial apoptosis by suppressing p53-activating stress signals and stabilizing the cytosolic Ku70-Bax protein complex. Clin Cancer Res 2009; 15: 48–59.
Criswell T, Leskov K, Miyamoto S, Luo G, Boothman DA . Transcription factors activated in mammalian cells after clinically relevant doses of ionizing radiation. Oncogene 2003; 22: 5813–5827.
Garkavtsev I, Chauhan VP, Wong HK, Mukhopadhyay A, Glicksman MA, Peterson RT et al. Dehydro-{alpha}-lapachone, a plant product with antivascular activity. Proc Natl Acad Sci USA 2011; 108: 11596–115601.
Peretz S, Jensen R, Baserga R, Glazer PM . ATM-dependent expression of the insulin-like growth factor-I receptor in a pathway regulating radiation response. Proc Natl Acad Sci USA 2001; 98: 1676–1681.
Saatman KE, Contreras PC, Smith DH, Raghupathi R, McDermott KL, Fernandez SC et al. Insulin-like growth factor-1 (IGF-1) improves both neurological motor and cognitive outcome following experimental brain injury. Exp Neurol 1997; 147: 418–427.
Shahrabani-Gargir L, Pandita TK, Werner H . Ataxia-telangiectasia mutated gene controls insulin-like growth factor I receptor gene expression in a deoxyribonucleic acid damage response pathway via mechanisms involving zinc-finger transcription factors Sp1 and WT1. Endocrinology 2004; 145: 5679–5687.
Klokov D, Criswell T, Leskov KS, Araki S, Mayo L, Boothman DA . IR-inducible clusterin gene expression: a protein with potential roles in ionizing radiation-induced adaptive responses, genomic instability, and bystander effects. Mutat Res 2004; 568: 97–110.
Wagner MW, Li LS, Morales JC, Galindo CL, Garner HR, Bornmann WG et al. Role of c-Abl kinase in DNA mismatch repair-dependent G2 cell cycle checkpoint arrest responses. J Biol Chem 2008; 283: 21382–21393.
Li LS, Morales JC, Hwang A, Wagner MW, Boothman DA . DNA mismatch repair-dependent activation of c-Abl/p73alpha/GADD45alpha-mediated apoptosis. J Biol Chem 2008; 283: 21394–21403.
Acknowledgements
This work was supported by DOE Grant #DE-FG02-06ER64186 to DAB, a pilot grant from NASA to develop BLI imaging of hCLUp-Luc to DW and DAB, a DOD BCRP pre-doctoral fellowship (W81XWH-06-0748) to E.M.G and a DOD PCRP post-doctoral fellowship (X8IXWH-09-1-0168) to XL. We thank Ms Lakshmi Sampath and Mr Andrew Bruening for their help with this work. We are also grateful to Dr Mary Helen Barcellos-Hoff for her advice with the animal experiments. We are also grateful to the Robert B. and Virginia Payne Endowment to DAB. This is CSCN 065 and used the Flow Cytometry and Biostatistics Cores, Simmons Cancer Center.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Oncogene website
Rights and permissions
About this article
Cite this article
Klokov, D., Leskov, K., Araki, S. et al. Low dose IR-induced IGF-1-sCLU expression: a p53-repressed expression cascade that interferes with TGFβ1 signaling to confer a pro-survival bystander effect. Oncogene 32, 479–490 (2013). https://doi.org/10.1038/onc.2012.64
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2012.64
Keywords
This article is cited by
-
The emerging role of exosomes in radiotherapy
Cell Communication and Signaling (2022)
-
Cysteine protease cathepsin B mediates radiation-induced bystander effects
Nature (2017)
-
Metabolic reprogramming during TGFβ1-induced epithelial-to-mesenchymal transition
Oncogene (2015)