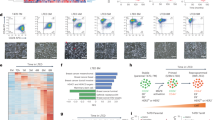
Abstract
Endocrine therapies targeting the proliferative effect of 17β-estradiol through estrogen receptor α (ERα) are the most effective systemic treatment of ERα-positive breast cancer. However, most breast tumors initially responsive to these therapies develop resistance through molecular mechanisms that are not yet fully understood. The long-term estrogen-deprived (LTED) MCF7 cell model has been proposed to recapitulate acquired resistance to aromatase inhibitors in postmenopausal women. To elucidate this resistance, genomic, transcriptomic and molecular data were integrated into the time course of MCF7–LTED adaptation. Dynamic and widespread genomic changes were observed, including amplification of the ESR1 locus consequently linked to an increase in ERα. Dynamic transcriptomic profiles were also observed that correlated significantly with genomic changes and were predicted to be influenced by transcription factors known to be involved in acquired resistance or cell proliferation (for example, interferon regulatory transcription factor 1 and E2F1, respectively) but, notably, not by canonical ERα transcriptional function. Consistently, at the molecular level, activation of growth factor signaling pathways by EGFR/ERBB/AKT and a switch from phospho-Ser118 (pS118)- to pS167-ERα were observed during MCF7–LTED adaptation. Evaluation of relevant clinical settings identified significant associations between MCF7–LTED and breast tumor transcriptome profiles that characterize ERα-negative status, early response to letrozole and tamoxifen, and recurrence after tamoxifen treatment. In accordance with these profiles, MCF7–LTED cells showed increased sensitivity to inhibition of FGFR-mediated signaling with PD173074. This study provides mechanistic insight into acquired resistance to endocrine therapies of breast cancer and highlights a potential therapeutic strategy.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Adelaide J, Finetti P, Charafe-Jauffret E, Wicinski J, Jacquemier J, Sotiriou C et al. (2008). Absence of ESR1 amplification in a series of breast cancers. Int J Cancer 123: 2970–2972.
Adler AS, Lin M, Horlings H, Nuyten DS, van de Vijver MJ, Chang HY . (2006). Genetic regulators of large-scale transcriptional signatures in cancer. Nat Genet 38: 421–430.
Ahn BY, Elwi AN, Lee B, Trinh DL, Klimowicz AC, Yau A et al. (2010). Genetic screen identifies insulin-like growth factor binding protein 5 as a modulator of tamoxifen resistance in breast cancer. Cancer Res 70: 3013–3019.
Alvarez MJ, Sumazin P, Rajbhandari P, Califano A . (2009). Correlating measurements across samples improves accuracy of large-scale expression profile experiments. Genome Biol 10: R143.
Balciunaite E, Spektor A, Lents NH, Cam H, Te Riele H, Scime A et al. (2005). Pocket protein complexes are recruited to distinct targets in quiescent and proliferating cells. Mol Cell Biol 25: 8166–8178.
Baselga J, Semiglazov V, van Dam P, Manikhas A, Bellet M, Mayordomo J et al. (2009). Phase II randomized study of neoadjuvant everolimus plus letrozole compared with placebo plus letrozole in patients with estrogen receptor-positive breast cancer. J Clin Oncol 27: 2630–2637.
Beeram M, Tan QT, Tekmal RR, Russell D, Middleton A, DeGraffenried LA . (2007). Akt-induced endocrine therapy resistance is reversed by inhibition of mTOR signaling. Ann Oncol 18: 1323–1328.
Benjamini Y, Hochberg Y . (1995). Controlling the false discovery rate: a practical and powerful approach to multiple testing. J Roy Statist Soc Ser B 57: 289–300.
Bouker KB, Skaar TC, Fernandez DR, O'Brien KA, Riggins RB, Cao D et al. (2004). Interferon regulatory factor-1 mediates the proapoptotic but not cell cycle arrest effects of the steroidal antiestrogen ICI 182 780 (faslodex, fulvestrant). Cancer Res 64: 4030–4039.
Bowie ML, Dietze EC, Delrow J, Bean GR, Troch MM, Marjoram RJ et al. (2004). Interferon-regulatory factor-1 is critical for tamoxifen-mediated apoptosis in human mammary epithelial cells. Oncogene 23: 8743–8755.
Brown LA, Hoog J, Chin SF, Tao Y, Zayed AA, Chin K et al. (2008). ESR1 gene amplification in breast cancer: a common phenomenon? Nat Genet 40: 806–807; author reply 810–2.
Bryne JC, Valen E, Tang MH, Marstrand T, Winther O, da Piedade I et al. (2008). JASPAR, the open access database of transcription factor-binding profiles: new content and tools in the 2008 update. Nucleic Acids Res 36: D102–D106.
Campbell RA, Bhat-Nakshatri P, Patel NM, Constantinidou D, Ali S, Nakshatri H . (2001). Phosphatidylinositol 3-kinase/AKT-mediated activation of estrogen receptor α: a new model for anti-estrogen resistance. J Biol Chem 276: 9817–9824.
Carroll JS, Meyer CA, Song J, Li W, Geistlinger TR, Eeckhoute J et al. (2006). Genome-wide analysis of estrogen receptor binding sites. Nat Genet 38: 1289–1297.
Chan CM, Martin LA, Johnston SR, Ali S, Dowsett M . (2002). Molecular changes associated with the acquisition of oestrogen hypersensitivity in MCF-7 breast cancer cells on long-term oestrogen deprivation. J Steroid Biochem Mol Biol 81: 333–341.
Chang JT, Nevins JR . (2006). GATHER: a systems approach to interpreting genomic signatures. Bioinformatics 22: 2926–2933.
Chia S, Gradishar W, Mauriac L, Bines J, Amant F, Federico M et al. (2008). Double-blind, randomized placebo controlled trial of fulvestrant compared with exemestane after prior nonsteroidal aromatase inhibitor therapy in postmenopausal women with hormone receptor-positive, advanced breast cancer: results from EFECT. J Clin Oncol 26: 1664–1670.
Chlebowski RT, Col N, Winer EP, Collyar DE, Cummings SR, Vogel III VG et al. (2002). American Society of Clinical Oncology technology assessment of pharmacologic interventions for breast cancer risk reduction including tamoxifen, raloxifene, and aromatase inhibition. J Clin Oncol 20: 3328–3343.
Clarke R, Liu MC, Bouker KB, Gu Z, Lee RY, Zhu Y et al. (2003). Antiestrogen resistance in breast cancer and the role of estrogen receptor signaling. Oncogene 22: 7316–7339.
Dey JH, Bianchi F, Voshol J, Bonenfant D, Oakeley EJ, Hynes NE . (2010). Targeting fibroblast growth factor receptors blocks PI3K/AKT signaling, induces apoptosis, and impairs mammary tumor outgrowth and metastasis. Cancer Res 70: 4151–4162.
Dowsett M, Martin LA, Smith I, Johnston S . (2005a). Mechanisms of resistance to aromatase inhibitors. J Steroid Biochem Mol Biol 95: 167–172.
Dowsett M, Nicholson RI, Pietras RJ . (2005b). Biological characteristics of the pure antiestrogen fulvestrant: overcoming endocrine resistance. Breast Cancer Res Treat 93 (Suppl 1): S11–S18.
Easton DF, Pooley KA, Dunning AM, Pharoah PD, Thompson D, Ballinger DG et al. (2007). Genome-wide association study identifies novel breast cancer susceptibility loci. Nature 447: 1087–1093.
EBCTCG (1998). Tamoxifen for early breast cancer: an overview of the randomised trials. Early Breast Cancer Trialists’ Collaborative Group. Lancet 351: 1451–1467.
Eeckhoute J, Keeton EK, Lupien M, Krum SA, Carroll JS, Brown M . (2007). Positive cross-regulatory loop ties GATA-3 to estrogen receptor α expression in breast cancer. Cancer Res 67: 6477–6483.
Ellis MJ, Tao Y, Young O, White S, Proia AD, Murray J et al. (2006). Estrogen-independent proliferation is present in estrogen-receptor HER2-positive primary breast cancer after neoadjuvant letrozole. J Clin Oncol 24: 3019–3025.
Galan-Caridad JM, Harel S, Arenzana TL, Hou ZE, Doetsch FK, Mirny LA et al. (2007). Zfx controls the self-renewal of embryonic and hematopoietic stem cells. Cell 129: 345–357.
Gautier L, Cope L, Bolstad BM, Irizarry RA . (2004). affy--analysis of Affymetrix GeneChip data at the probe level. Bioinformatics 20: 307–315.
Geisler J, Haynes B, Anker G, Dowsett M, Lonning PE . (2002). Influence of letrozole and anastrozole on total body aromatization and plasma estrogen levels in postmenopausal breast cancer patients evaluated in a randomized, cross-over study. J Clin Oncol 20: 751–757.
Gentleman RC, Carey VJ, Bates DM, Bolstad B, Dettling M, Dudoit S et al. (2004). Bioconductor: open software development for computational biology and bioinformatics. Genome Biol 5: R80.
Ghayad SE, Vendrell JA, Larbi SB, Dumontet C, Bieche I, Cohen PA . (2009). Endocrine resistance associated with activated ErbB system in breast cancer cells is reversed by inhibiting MAPK or PI3K/Akt signaling pathways. Int J Cancer 126: 545–562.
Gu Z, Lee RY, Skaar TC, Bouker KB, Welch JN, Lu J et al. (2002). Association of interferon regulatory factor-1, nucleophosmin, nuclear factor-kappaB, and cyclic AMP response element binding with acquired resistance to Faslodex (ICI 182 780). Cancer Res 62: 3428–3437.
Hoch RV, Thompson DA, Baker RJ, Weigel RJ . (1999). GATA-3 is expressed in association with estrogen receptor in breast cancer. Int J Cancer 84: 122–128.
Holst F, Stahl PR, Ruiz C, Hellwinkel O, Jehan Z, Wendland M et al. (2007). Estrogen receptor α (ESR1) gene amplification is frequent in breast cancer. Nat Genet 39: 655–660.
Horlings HM, Bergamaschi A, Nordgard SH, Kim YH, Han W, Noh DY et al. (2008). ESR1 gene amplification in breast cancer: a common phenomenon? Nat Genet 40: 807–808; author reply 810–2.
Hunter DJ, Kraft P, Jacobs KB, Cox DG, Yeager M, Hankinson SE et al. (2007). A genome-wide association study identifies alleles in FGFR2 associated with risk of sporadic postmenopausal breast cancer. Nat Genet 39: 870–874.
Iorns E, Turner NC, Elliott R, Syed N, Garrone O, Gasco M et al. (2008). Identification of CDK10 as an important determinant of resistance to endocrine therapy for breast cancer. Cancer Cell 13: 91–104.
Jelovac D, Sabnis G, Long BJ, Macedo L, Goloubeva OG, Brodie AM . (2005). Activation of mitogen-activated protein kinase in xenografts and cells during prolonged treatment with aromatase inhibitor letrozole. Cancer Res 65: 5380–5389.
Jeng MH, Shupnik MA, Bender TP, Westin EH, Bandyopadhyay D, Kumar R et al. (1998). Estrogen receptor expression and function in long-term estrogen-deprived human breast cancer cells. Endocrinology 139: 4164–4174.
Johnston S, Pippen Jr J, Pivot X, Lichinitser M, Sadeghi S, Dieras V et al. (2009). Lapatinib combined with letrozole versus letrozole and placebo as first-line therapy for postmenopausal hormone receptor-positive metastatic breast cancer. J Clin Oncol 27: 5538–5546.
Johnston SR, Martin LA, Head J, Smith I, Dowsett M . (2005). Aromatase inhibitors: combinations with fulvestrant or signal transduction inhibitors as a strategy to overcome endocrine resistance. J Steroid Biochem Mol Biol 95: 173–181.
Johnston SR, Saccani-Jotti G, Smith IE, Salter J, Newby J, Coppen M et al. (1995). Changes in estrogen receptor, progesterone receptor, and pS2 expression in tamoxifen-resistant human breast cancer. Cancer Res 55: 3331–3338.
Jonat W, Kaufmann M, Blamey RW, Howell A, Collins JP, Coates A et al. (1995). A randomised study to compare the effect of the luteinising hormone releasing hormone (LHRH) analogue goserelin with or without tamoxifen in pre- and perimenopausal patients with advanced breast cancer. Eur J Cancer 31A: 137–142.
Kanai M, Tashiro E, Maruki H, Minato Y, Imoto M . (2009). Transcriptional regulation of human fibroblast growth factor receptor 1 by E2F-1. Gene 438: 49–56.
Katzenellenbogen BS, Kendra KL, Norman MJ, Berthois Y . (1987). Proliferation, hormonal responsiveness, and estrogen receptor content of MCF-7 human breast cancer cells grown in the short-term and long-term absence of estrogens. Cancer Res 47: 4355–4360.
Knowlden JM, Hutcheson IR, Jones HE, Madden T, Gee JM, Harper ME et al. (2003). Elevated levels of epidermal growth factor receptor/c-erbB2 heterodimers mediate an autocrine growth regulatory pathway in tamoxifen-resistant MCF-7 cells. Endocrinology 144: 1032–1044.
Korc M, Friesel RE . (2009). The role of fibroblast growth factors in tumor growth. Curr Cancer Drug Targets 9: 639–651.
Kouros-Mehr H, Kim JW, Bechis SK, Werb Z . (2008). GATA-3 and the regulation of the mammary luminal cell fate. Curr Opin Cell Biol 20: 164–170.
Lannigan DA . (2003). Estrogen receptor phosphorylation. Steroids 68: 1–9.
Lewis-Wambi JS, Cunliffe HE, Kim HR, Willis AL, Jordan VC . (2008). Overexpression of CEACAM6 promotes migration and invasion of oestrogen-deprived breast cancer cells. Eur J Cancer 44: 1770–1779.
Ma XJ, Wang Z, Ryan PD, Isakoff SJ, Barmettler A, Fuller A et al. (2004). A two-gene expression ratio predicts clinical outcome in breast cancer patients treated with tamoxifen. Cancer Cell 5: 607–616.
Martin LA, Farmer I, Johnston SR, Ali S, Dowsett M . (2005). Elevated ERK1/ERK2/estrogen receptor cross-talk enhances estrogen-mediated signaling during long-term estrogen deprivation. Endocr Relat Cancer 12 (Suppl 1): S75–S84.
Martin LA, Farmer I, Johnston SR, Ali S, Marshall C, Dowsett M . (2003). Enhanced estrogen receptor (ER) α, ERBB2, and MAPK signal transduction pathways operate during the adaptation of MCF-7 cells to long term estrogen deprivation. J Biol Chem 278: 30458–30468.
Masamura S, Santner SJ, Heitjan DF, Santen RJ . (1995). Estrogen deprivation causes estradiol hypersensitivity in human breast cancer cells. J Clin Endocrinol Metab 80: 2918–2925.
Masri S, Phung S, Wang X, Wu X, Yuan YC, Wagman L et al. (2008). Genome-wide analysis of aromatase inhibitor-resistant, tamoxifen-resistant, and long-term estrogen-deprived cells reveals a role for estrogen receptor. Cancer Res 68: 4910–4918.
Massarweh S, Schiff R . (2006). Resistance to endocrine therapy in breast cancer: exploiting estrogen receptor/growth factor signaling crosstalk. Endocr Relat Cancer 13 (Suppl 1): S15–S24.
Massarweh S, Schiff R . (2007). Unraveling the mechanisms of endocrine resistance in breast cancer: new therapeutic opportunities. Clin Cancer Res 13: 1950–1954.
Matys V, Kel-Margoulis OV, Fricke E, Liebich I, Land S, Barre-Dirrie A et al. (2006). TRANSFAC and its module TRANSCompel: transcriptional gene regulation in eukaryotes. Nucleic Acids Res 34: D108–D110.
McClelland RA, Barrow D, Madden TA, Dutkowski CM, Pamment J, Knowlden JM et al. (2001). Enhanced epidermal growth factor receptor signaling in MCF7 breast cancer cells after long-term culture in the presence of the pure antiestrogen ICI 182 780 (Faslodex). Endocrinology 142: 2776–2788.
Meyer KB, Maia AT, O'Reilly M, Teschendorff AE, Chin SF, Caldas C et al. (2008). Allele-specific up-regulation of FGFR2 increases susceptibility to breast cancer. PLoS Biol 6: e108.
Michalides R, Griekspoor A, Balkenende A, Verwoerd D, Janssen L, Jalink K et al. (2004). Tamoxifen resistance by a conformational arrest of the estrogen receptor α after PKA activation in breast cancer. Cancer Cell 5: 597–605.
Miller WR, Larionov AA, Renshaw L, Anderson TJ, White S, Murray J et al. (2007). Changes in breast cancer transcriptional profiles after treatment with the aromatase inhibitor, letrozole. Pharmacogenet Genomics 17: 813–826.
Normanno N, Di Maio M, De Maio E, De Luca A, de Matteis A, Giordano A et al. (2005). Mechanisms of endocrine resistance and novel therapeutic strategies in breast cancer. Endocr Relat Cancer 12: 721–747.
Osborne CK, Shou J, Massarweh S, Schiff R . (2005). Crosstalk between estrogen receptor and growth factor receptor pathways as a cause for endocrine therapy resistance in breast cancer. Clin Cancer Res 11: 865s–8670s.
Pique-Regi R, Monso-Varona J, Ortega A, Seeger RC, Triche TJ, Asgharzadeh S . (2008). Sparse representation and Bayesian detection of genome copy number alterations from microarray data. Bioinformatics 24: 309–318.
Reis-Filho JS, Drury S, Lambros MB, Marchio C, Johnson N, Natrajan R et al. (2008). ESR1 gene amplification in breast cancer: a common phenomenon? Nat Genet 40: 809–810; author reply 810–2.
Rose C, Vtoraya O, Pluzanska A, Davidson N, Gershanovich M, Thomas R et al. (2003). An open randomised trial of second-line endocrine therapy in advanced breast cancer: comparison of the aromatase inhibitors letrozole and anastrozole. Eur J Cancer 39: 2318–2327.
Sabnis GJ, Jelovac D, Long B, Brodie A . (2005). The role of growth factor receptor pathways in human breast cancer cells adapted to long-term estrogen deprivation. Cancer Res 65: 3903–3910.
Sadler AJ, Pugazhendhi D, Darbre PD . (2009). Use of global gene expression patterns in mechanistic studies of oestrogen action in MCF7 human breast cancer cells. J Steroid Biochem Mol Biol 114: 21–32.
Santen R, Jeng MH, Wang JP, Song R, Masamura S, McPherson R et al. (2001). Adaptive hypersensitivity to estradiol: potential mechanism for secondary hormonal responses in breast cancer patients. J Steroid Biochem Mol Biol 79: 115–125.
Santen RJ, Song RX, Masamura S, Yue W, Fan P, Sogon T et al. (2008). Adaptation to estradiol deprivation causes up-regulation of growth factor pathways and hypersensitivity to estradiol in breast cancer cells. Adv Exp Med Biol 630: 19–34.
Santen RJ, Song RX, Zhang Z, Kumar R, Jeng MH, Masamura A et al. (2005). Long-term estradiol deprivation in breast cancer cells up-regulates growth factor signaling and enhances estrogen sensitivity. Endocr Relat Cancer 12 (Suppl 1): S61–S73.
Schild-Hay LJ, Leil TA, Divi RL, Olivero OA, Weston A, Poirier MC . (2009). Tamoxifen induces expression of immune response-related genes in cultured normal human mammary epithelial cells. Cancer Res 69: 1150–1155.
Schones DE, Smith AD, Zhang MQ . (2007). Statistical significance of cis-regulatory modules. BMC Bioinformatics 8: 19.
Shaw LE, Sadler AJ, Pugazhendhi D, Darbre PD . (2006). Changes in oestrogen receptor-α and -β during progression to acquired resistance to tamoxifen and fulvestrant (Faslodex, ICI 182 780) in MCF7 human breast cancer cells. J Steroid Biochem Mol Biol 99: 19–32.
Shen R, Chinnaiyan AM, Ghosh D . (2008). Pathway analysis reveals functional convergence of gene expression profiles in breast cancer. BMC Med Genomics 1: 28.
Shim WS, Conaway M, Masamura S, Yue W, Wang JP, Kmar R et al. (2000). Estradiol hypersensitivity and mitogen-activated protein kinase expression in long-term estrogen deprived human breast cancer cells in vivo. Endocrinology 141: 396–405.
Solé X, Bonifaci N, López-Bigas N, Berenguer A, Hernández P, Reina O et al. (2009). Biological convergence of cancer signatures. PLoS One 4: e4544.
Song RX, Fan P, Yue W, Chen Y, Santen RJ . (2006). Role of receptor complexes in the extranuclear actions of estrogen receptor α in breast cancer. Endocr Relat Cancer 13 (Suppl 1): S3–13.
Stamm S, Riethoven JJ, Le Texier V, Gopalakrishnan C, Kumanduri V, Tang Y et al. (2006). ASD: a bioinformatics resource on alternative splicing. Nucleic Acids Res 34: D46–D55.
Stephen R, Darbre PD . (2000). Loss of growth inhibitory effects of retinoic acid in human breast cancer cells following long-term exposure to retinoic acid. Br J Cancer 83: 1183–1191.
Stephen RL, Shaw LE, Larsen C, Corcoran D, Darbre PD . (2001). Insulin-like growth factor receptor levels are regulated by cell density and by long term estrogen deprivation in MCF7 human breast cancer cells. J Biol Chem 276: 40080–40086.
Subramanian A, Tamayo P, Mootha VK, Mukherjee S, Ebert BL, Gillette MA et al. (2005). Gene set enrichment analysis: a knowledge-based approach for interpreting genome-wide expression profiles. Proc Natl Acad Sci USA 102: 15545–15550.
Tashiro E, Minato Y, Maruki H, Asagiri M, Imoto M . (2003). Regulation of FGF receptor-2 expression by transcription factor E2F-1. Oncogene 22: 5630–5635.
Tomita S, Zhang Z, Nakano M, Ibusuki M, Kawazoe T, Yamamoto Y et al. (2009). Estrogen receptor α gene ESR1 amplification may predict endocrine therapy responsiveness in breast cancer patients. Cancer Sci 100: 1012–1017.
Turner N, Lambros MB, Horlings HM, Pearson A, Sharpe R, Natrajan R et al. (2010a). Integrative molecular profiling of triple negative breast cancers identifies amplicon drivers and potential therapeutic targets. Oncogene 29: 2013–2023.
Turner N, Pearson A, Sharpe R, Lambros M, Geyer F, Lopez-Garcia MA et al. (2010b). FGFR1 amplification drives endocrine therapy resistance and is a therapeutic target in breast cancer. Cancer Res 70: 2085–2094.
van de Vijver MJ, He YD, van't Veer LJ, Dai H, Hart AA, Voskuil DW et al. (2002). A gene-expression signature as a predictor of survival in breast cancer. N Engl J Med 347: 1999–2009.
Vincent-Salomon A, Raynal V, Lucchesi C, Gruel N, Delattre O . (2008). ESR1 gene amplification in breast cancer: a common phenomenon? Nat Genet 40: 809; author reply 810–2.
Vuaroqueaux V, Urban P, Labuhn M, Delorenzi M, Wirapati P, Benz CC et al. (2007). Low E2F1 transcript levels are a strong determinant of favorable breast cancer outcome. Breast Cancer Res 9: R33.
Welshons WV, Jordan VC . (1987). Adaptation of estrogen-dependent MCF-7 cells to low estrogen (phenol red-free) culture. Eur J Cancer Clin Oncol 23: 1935–1939.
Winer EP, Hudis C, Burstein HJ, Chlebowski RT, Ingle JN, Edge SB et al. (2002). American Society of Clinical Oncology technology assessment on the use of aromatase inhibitors as adjuvant therapy for women with hormone receptor-positive breast cancer: status report 2002. J Clin Oncol 20: 3317–3327.
Wolfer A, Wittner BS, Irimia D, Flavin RJ, Lupien M, Gunawardane RN et al. (2010). MYC regulation of a ‘poor-prognosis’ metastatic cancer cell state. Proc Natl Acad Sci USA 107: 3698–3703.
Xu X, Bieda M, Jin VX, Rabinovich A, Oberley MJ, Green R et al. (2007). A comprehensive ChIP-chip analysis of E2F1, E2F4, and E2F6 in normal and tumor cells reveals interchangeable roles of E2F family members. Genome Res 17: 1550–1561.
Yu JX, Sieuwerts AM, Zhang Y, Martens JW, Smid M, Klijn JG et al. (2007). Pathway analysis of gene signatures predicting metastasis of node-negative primary breast cancer. BMC Cancer 7: 182.
Yue W, Wang J, Li Y, Fan P, Santen RJ . (2005). Farnesylthiosalicylic acid blocks mammalian target of rapamycin signaling in breast cancer cells. Int J Cancer 117: 746–754.
Yue W, Wang JP, Conaway MR, Li Y, Santen RJ . (2003). Adaptive hypersensitivity following long-term estrogen deprivation: involvement of multiple signal pathways. J Steroid Biochem Mol Biol 86: 265–274.
Zhang Z, Chen D, Fenstermacher DA . (2007). Integrated analysis of independent gene expression microarray datasets improves the predictability of breast cancer outcome. BMC Genomics 8: 331.
Acknowledgements
This study was funded by the Spanish Ministry of Health CIBERESP and grant 06/0545 and the Ministry of Science and Innovation (MICINN) grant SAF06/05399. HA was supported by a MICINN postdoctoral fellowship and MAP was a ‘Ramón y Cajal’ Researcher with the MICINN.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Oncogene website
Rights and permissions
About this article
Cite this article
Aguilar, H., Solé, X., Bonifaci, N. et al. Biological reprogramming in acquired resistance to endocrine therapy of breast cancer. Oncogene 29, 6071–6083 (2010). https://doi.org/10.1038/onc.2010.333
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2010.333
Keywords
This article is cited by
-
Nucleosome destabilization by nuclear non-coding RNAs
Communications Biology (2020)
-
Molecular changes during extended neoadjuvant letrozole treatment of breast cancer: distinguishing acquired resistance from dormant tumours
Breast Cancer Research (2019)
-
The Eleanor ncRNAs activate the topological domain of the ESR1 locus to balance against apoptosis
Nature Communications (2019)
-
TNFAIP3 is required for FGFR1 activation-promoted proliferation and tumorigenesis of premalignant DCIS.COM human mammary epithelial cells
Breast Cancer Research (2018)
-
Endocrine therapy-resistant breast cancer model cells are inhibited by soybean glyceollin I through Eleanor non-coding RNA
Scientific Reports (2018)