Abstract
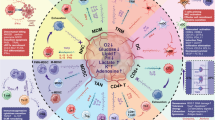
Immune escape is a critical gateway to malignancy. The emergence of this fundamental trait of cancer represents the defeat of immune surveillance, a potent, multi-armed and essential mode of cancer suppression that may influence the ultimate clinical impact of an early stage tumor. Indeed, immune escape may be a central modifier of clinical outcomes, by affecting tumor dormancy versus progression, licensing invasion and metastasis and impacting therapeutic response. Although relatively little studied until recently, immune suppression and escape in tumors are now hot areas with clinical translation of several new therapeutic agents already under way. The interconnections between signaling pathways that control immune escape and those that control proliferation, senescence, apoptosis, metabolic alterations, angiogenesis, invasion and metastasis remain virtually unexplored, offering rich new areas for investigation. Here, an overview of this area is provided with a focus on the tryptophan catabolic enzyme indoleamine 2,3-dioxygenase (IDO) and its recently discovered relative IDO2 that are implicated in suppressing T-cell immunity in normal and pathological settings including cancer. Emerging evidence suggests that during cancer progression activation of the IDO pathway might act as a preferred nodal modifier pathway for immune escape, for example analogous to the PI3K pathway for survival or the VEGF pathway for angiogenesis. Small molecule inhibitors of IDO and IDO2 heighten chemotherapeutic efficacy in mouse models of cancer in a nontoxic fashion and an initial lead compound entered phase I clinical trials in late 2007. New modalities in this area offer promising ways to broaden the combinatorial attack on advanced cancers, where immune escape mechanisms likely provide pivotal support.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Apetoh L, Ghiringhelli F, Tesniere A, Obeid M, Ortiz C, Criollo A et al. (2007). Toll-like receptor 4-dependent contribution of the immune system to anticancer chemotherapy and radiotherapy. Nat Med 13: 1050–1059.
Balkwill F, Charles KA, Mantovani A . (2005). Smoldering and polarized inflammation in the initiation and promotion of malignant disease. Cancer Cell 7: 211–217.
Ball HJ, Sanchez-Perez A, Weiser S, Austin CJ, Astelbauer F, Miu J et al. (2007). Characterization of an indoleamine 2,3-dioxygenase-like protein found in humans and mice. Gene 396: 203–213.
Banerjee T, DuHadaway JB, Gaspari P, Sutanto-Ward E, Munn DH, Mellor AL et al. (2008). Antitumor properties of chemopreventive natural product brassinin are based upon inhibition of indoleamine 2,3-dioxygenase (IDO). Oncogene (in press).
Bild AH, Turkson J, Jove R . (2002). Cytoplasmic transport of Stat3 by receptor-mediated endocytosis. EMBO J 21: 3255–3263.
Blank C, Kuball J, Voelkl S, Wiendl H, Becker B, Walter B et al. (2006). Blockade of PD-L1 (B7-H1) augments human tumor-specific T cell responses in vitro. Int J Cancer 119: 317–327.
Bronte V, Zanovello P . (2005). Regulation of immune responses by L-arginine metabolism. Nat Rev Immunol 5: 641–654.
Chang M, Boulden J, Katz JB, Wang L, Meyer TJ, Soler AP et al. (2007a). Bin1 ablation increases susceptibility to cancer during aging, particularly lung cancer. Cancer Res 67: 7605–7612.
Chang M, Boulden J, Sutanto-Ward E, Duhadaway JB, Soler AP, Muller AJ et al. (2007b). Bin1 ablation in mammary gland delays tissue remodeling and drives cancer progression. Cancer Res 67: 100–107.
Colombo MP, Piconese S . (2007). Regulatory-T-cell inhibition versus depletion: the right choice in cancer immunotherapy. Nat Rev Cancer 7: 880–887.
Coussens LM, Raymond WW, Bergers G, Laig-Webster M, Behrendtsen O, Werb Z et al. (1999). Inflammatory mast cells up-regulate angiogenesis during squamous epithelial carcinogenesis. Genes Dev 13: 1382–1397.
Curti A, Pandolfi S, Valzasina B, Aluigi M, Isidori A, Ferri E et al. (2007). Modulation of tryptophan catabolism by human leukemic cells results in the conversion of CD25- into CD25+ T regulatory cells. Blood 109: 2871–2877.
Curtis RE, Rowlings PA, Deeg HJ, Shriner DA, Socie G, Travis LB et al. (1997). Solid cancers after bone marrow transplantation. N Engl J Med 336: 897–904.
DuHadaway JB, Du W, Liu A-X, Baker J, Donover PS, Sharp DM et al. (2003). Transformation selective apoptosis by farnesyltransferase inhibitors requires Bin1. Oncogene 22: 3578–3588.
DuHadaway JB, Sakamuro D, Ewert DL, Prendergast GC . (2001). Bin1 mediates apoptosis by c-Myc in transformed primary cells. Cancer Res 16: 3151–3156.
Dunn GP, Old LJ, Schreiber RD . (2004). The immunobiology of cancer immunosurveillance and immunoediting. Immunity 21: 137–148.
Elliott K, Ge K, Du W, Prendergast GC . (2000). The c-Myc-interacting adapter protein Bin1 activates a caspase-independent cell death program. Oncogene 19: 4669–4684.
Elliott K, Sakamuro D, Basu A, Du W, Wunner W, Staller P et al. (1999). Bin1 functionally interacts with Myc in cells and inhibits cell proliferation by multiple mechanisms. Oncogene 18: 3564–3573.
Engels EA, Wu X, Gu J, Dong Q, Liu J, Spitz MR . (2007). Systematic evaluation of genetic variants in the inflammation pathway and risk of lung cancer. Cancer Res 67: 6520–6527.
Fallarino F, Grohmann U, Hwang KW, Orabona C, Vacca C, Bianchi R et al. (2003). Modulation of tryptophan catabolism by regulatory T cells. Nat Immunol 4: 1206–1212.
Fallarino F, Grohmann U, Vacca C, Bianchi R, Orabona C, Spreca A et al. (2002). T cell apoptosis by tryptophan catabolism. Cell Death Diff 9: 1069–1077.
Fallarino F, Grohmann U, You S, McGrath BC, Cavener DR, Vacca C et al. (2006). The combined effects of tryptophan starvation and tryptophan catabolites down-regulate T cell receptor zeta-chain and induce a regulatory phenotype in naive T cells. J Immunol 176: 6752–6761.
Friberg M, Jennings R, Alsarraj M, Dessureault S, Cantor A, Extermann M et al. (2002). Indoleamine 2,3-dioxygenase contributes to tumor cell evasion of T cell-mediated rejection. Int. J Cancer 101: 151–155.
Gabrilovich DI . (2007). Molecular mechanisms and therapeutic reversal of immune suppression in cancer. Curr Cancer Drug Targets 7: 1.
Galon J, Costes A, Sanchez-Cabo F, Kirilovsky A, Mlecnik B, Lagorce-Pages C et al. (2006). Type, density, and location of immune cells within human colorectal tumors predict clinical outcome. Science 313: 1960–1964.
Gaspari P, Banerjee T, Malachowski WP, Muller AJ, Prendergast GC, Duhadaway J et al. (2006). Structure-activity study of brassinin derivatives as indoleamine 2,3-dioxygenase inhibitors. J Med Chem 49: 684–692.
Ge K, DuHadaway J, Du W, Herlyn M, Rodeck U, Prendergast GC . (1999). Mechanism for elimination of a tumor suppressor: aberrant splicing of a brain-specific exon causes loss of function of Bin1 in melanoma. Proc Natl Acad Sci USA 96: 9689–9694.
Ge K, DuHadaway J, Sakamuro D, Wechsler-Reya R, Reynolds C, Prendergast GC . (2000a). Losses of the tumor suppressor Bin1 in breast carcinoma are frequent and reflect deficits in a programmed cell death capacity. Int. J Cancer 85: 376–383.
Ge K, Minhas F, DuHadaway J, Mao N-C, Wilson D, Sakamuro D et al. (2000b). Loss of heterozygosity and tumor suppressor activity of Bin1 in prostate carcinoma. Int J Cancer 86: 155–161.
Grohmann U, Volpi C, Fallarino F, Bozza S, Bianchi R, Vacca C et al. (2007). Reverse signaling through GITR ligands enables dexamethasone to activate IDO allergy. Nature Med 13: 579–586.
Hanahan D, Weinberg RA . (2000). The hallmarks of cancer. Cell 100: 57–70.
Hou DY, Muller AJ, Sharma MD, DuHadaway J, Banerjee T, Johnson M et al. (2007). Inhibition of indoleamine 2,3-dioxygenase in dendritic cells by stereoisomers of 1-methyl-tryptophan correlates with antitumor responses. Cancer Res 67: 792–801.
Huber S, Schramm C . (2006). TGF-beta and CD4+CD25+ regulatory T cells. Front Biosci 11: 1014–1023.
Hunter KW, Crawford NP . (2006). Germ line polymorphism in metastatic progression. Cancer Res 66: 1251–1254.
Iwai Y, Ishida M, Tanaka Y, Okazaki T, Honjo T, Minato N . (2002). Involvement of PD-L1 on tumor cells in the escape from host immune system and tumor immunotherapy by PD-L1 blockade. Proc Natl Acad Sci USA 99: 12293–12297.
Karni R, de Stanchina E, Lowe SW, Sinha R, Mu D, Krainer AR . (2007). The gene encoding the splicing factor SF2/ASF is a proto-oncogene. Nat Struct Mol Biol 14: 185–193.
Knoepfler PS, Zhang XY, Cheng PF, Gafken PR, McMahon SB, Eisenman RN . (2006). Myc influences global chromatin structure. EMBO J 25: 2723–2734.
Koebel CM, Vermi W, Swann JB, Zerafa N, Rodig SJ, Old LJ et al. (2007). Adaptive immunity maintains occult cancer in an equilibrium state. Nature 450: 903–907.
Lewis CE, Pollard JW . (2006). Distinct role of macrophages in different tumor microenvironments. Cancer Res 66: 605–612.
Lu LF, Lind EF, Gondek DC, Bennett KA, Gleeson MW, Pino-Lagos K et al. (2006). Mast cells are essential intermediaries in regulatory T-cell tolerance. Nature 442: 997–1002.
Machiels JP, Reilly RT, Emens LA, Ercolini AM, Lei RY, Weintraub D et al. (2001). Cyclophosphamide, doxorubicin, and paclitaxel enhance the antitumor immune response of granulocyte/macrophage-colony stimulating factor-secreting whole-cell vaccines in HER-2/neu tolerized mice. Cancer Res 61: 3689–3697.
Mehta RG, Liu J, Constantinou A, Thomas CF, Hawthorne M, You M et al. (1995). Cancer chemopreventive activity of brassinin, a phytoalexin from cabbage. Carcinogenesis 16: 399–404.
Mellor AL, Chandler P, Baban B, Hansen AM, Marshall B, Pihkala J et al. (2004). Specific subsets of murine dendritic cells acquire potent T cell regulatory functions following CTLA4-mediated induction of indoleamine 2,3 dioxygenase. Int Immunol 16: 1391–1401.
Mellor AL, Munn DH . (2004). IDO expression by dendritic cells: tolerance and tryptophan catabolism. Nat Rev Immunol 4: 762–774.
Mellor AL, Munn DH . (2008). Creating immune privilege: active local suppression that benefits friends, but protects foes. Nat Rev Immunol 8: 74–80.
Mellor AL, Sivakumar J, Chandler P, Smith K, Molina H, Mao D et al. (2001). Prevention of T cell-driven complement activation and inflammation by tryptophan catabolism during pregnancy. Nat. Immunol 2: 64–68.
Metz R, DuHadaway JB, Kamasani U, Laury-Kleintop L, Muller AJ, Prendergast GC . (2007). Novel tryptophan catabolic enzyme IDO2 is the preferred biochemical target of the antitumor IDO inhibitory compound D-1MT. Cancer Res 67: 7082–7087.
Miaczynska M, Christoforidis S, Giner A, Shevchenko A, Uttenweiler-Joseph S, Habermann B et al. (2004). APPL proteins link Rab5 to nuclear signal transduction via an endosomal compartment. Cell 116: 445–456.
Muller AJ, DuHadaway JB, Donover PS, Sutanto-Ward E, Prendergast GC . (2004). Targeted deletion of the suppressor gene Bin1/Amphiphysin2 enhances the malignant character of transformed cells. Cancer Biol Ther 3: 1236–1242.
Muller AJ, DuHadaway JB, Sutanto-Ward E, Donover PS, Prendergast GC . (2005a). Inhibition of indoleamine 2,3-dioxygenase, an immunomodulatory target of the tumor suppressor gene Bin1, potentiates cancer chemotherapy. Nature Med 11: 312–319.
Muller AJ, Malachowski WP, Prendergast GC . (2005b). Indoleamine 2,3-dioxygenase in cancer: targeting pathological immune tolerance with small-molecule inhibitors. Expert Opin Ther Targets 9: 831–849.
Muller AJ, Prendergast GC . (2007). Indoleamine 2,3-dioxygenase in immune suppression and cancer. Curr Cancer Drug Targets 7: 31–40.
Muller AJ, Scherle PA . (2006). Targeting the mechanisms of tumoral immune tolerance with small-molecule inhibitors. Nat Rev Cancer 6: 613–625.
Munn DH, Mellor AL . (2007). Indoleamine 2,3-dioxygenase and tumor-induced tolerance. J Clin Invest 117: 1147–1154.
Munn DH, Sharma MD, Baban B, Harding HP, Zhang Y, Ron D et al. (2005). GCN2 kinase in T cells mediates proliferative arrest and anergy induction in response to indoleamine 2,3-dioxygenase. Immunity 22: 633–642.
Munn DH, Sharma MD, Hou D, Baban B, Lee JR, Antonia SJ et al. (2004). Expression of indoleamine 2,3-dioxygenase by plasmacytoid dendritic cells in tumor-draining lymph nodes. J Clin Invest 114: 280–290.
Munn DH, Zhou M, Attwood JT, Bondarev I, Conway SJ, Marshall B et al. (1998). Prevention of allogeneic fetal rejection by tryptophan catabolism. Science 281: 1191–1193.
Muto S, Katsuki M, Horie S . (2007). Decreased c-kit function inhibits enhanced skin carcinogenesis in c-Ha-ras protooncogene transgenic mice. Cancer Sci 98: 1549–1556.
Obeid M, Tesniere A, Ghiringhelli F, Fimia GM, Apetoh L, Perfettini JL et al. (2007). Calreticulin exposure dictates the immunogenicity of cancer cell death. Nat Med 13: 54–61.
Popovic PJ, Zeh III HJ, Ochoa JB . (2007). Arginine and immunity. J Nutr 137: 1681S–1686 S.
Prendergast GC, Jaffee EM . (2007). Cancer immunologists and cancer biologists: why we didn′t talk then but need to now. Cancer Res 67: 3500–3504.
Ramalingam A, Farmer GE, Stamato TD, Prendergast GC . (2007). Bin1 interacts with and restrains the DNA end-binding protein complex Ku. Cell Cycle 6: 1914–1918.
Ramalingam A, Prendergast GC . (2007). Bin1 homolog hob1 supports a rad6-set1 pathway of transcriptional repression in fission yeast. Cell Cycle 6: 1655–1662.
Ren G, Vajjhala P, Lee JS, Winsor B, Munn AL . (2006). The BAR domain proteins: molding membranes in fission, fusion, and phagy. Microbiol Mol Biol Rev 70: 37–120.
Rose D, Sheff MD . (1967). Tryptophan metabolism in carcinoma of the breast. Lancet 1: 239–241.
Routhier EL, Donover PS, Prendergast GC . (2003). hob1+, the homolog of Bin1 in fission yeast, is dispensable for endocytosis but required for the response to starvation or genotoxic stress. Oncogene 22: 637–648.
Roy M, Xu Q, Lee C . (2005). Evidence that public database records for many cancer-associated genes reflect a splice form found in tumors and lack normal splice forms. Nucleic Acids Res 33: 5026–5033.
Sakamuro D, Elliott K, Wechsler-Reya R, Prendergast GC . (1996). BIN1 is a novel MYC-interacting protein with features of a tumor suppressor. Nature Genet 14: 69–77.
Schlee M, Schuhmacher M, Holzel M, Laux G, Bornkamm GW . (2007). c-MYC impairs immunogenicity of human B cells. Adv Cancer Res 97: 167–188.
Shankaran V, Ikeda H, Bruce AT, White JM, Swanson PE, Old LJ et al. (2001). IFNgamma and lymphocytes prevent primary tumour development and shape tumour immunogenicity. Nature 410: 1107–1111.
Sharma MD, Baban B, Chandler P, Hou DY, Singh N, Yagita H et al. (2007). Plasmacytoid dendritic cells from mouse tumor-draining lymph nodes directly activate mature Tregs via indoleamine 2,3-dioxygenase. J Clin Invest 117: 2570–2582.
Soucek L, Lawlor ER, Soto D, Shchors K, Swigart LB, Evan GI . (2007). Mast cells are required for angiogenesis and macroscopic expansion of Myc-induced pancreatic islet tumors. Nat Med 13: 1211–1218.
Swensen SJ, Jett JR, Hartman TE, Midthun DE, Mandrekar SJ, Hillman SL et al. (2005). CT screening for lung cancer: five-year prospective experience. Radiology 235: 259–265.
Tajiri T, Liu X, Thompson PM, Tanaka S, Suita S, Zhao H et al. (2003). Expression of a MYCN-interacting isoform of the tumor suppressor BIN1 is reduced in neuroblastomas with unfavorable biological features. Clin Cancer Res 9: 3345–3355.
Uyttenhove C, Pilotte L, Theate I, Stroobant V, Colau D, Parmentier N et al. (2003). Evidence for a tumoral immune resistance mechanism based on tryptophan degradation by indoleamine 2,3-dioxygenase. Nat Med 9: 1269–1274.
Wingender G, Garbi N, Schumak B, Jungerkes F, Endl E, von Bubnoff D et al. (2006). Systemic application of CpG-rich DNA suppresses adaptive T cell immunity via induction of IDO. Eur J Immunol 36: 12–20.
Xu Q, Lee C . (2003). Discovery of novel splice forms and functional analysis of cancer-specific alternative splicing in human expressed sequences. Nucleic Acids Res 31: 5635–5643.
Zou W . (2005). Immunosuppressive networks in the tumour environment and their therapeutic relevance. Nat Rev Cancer 5: 263–274.
Acknowledgements
I thank my colleagues and collaborators Alexander Muller, Lisa Laury-Kleintop and Laura Mandik-Nayak (Lankenau Institute for Medical Research (LIMR)); Richard Metz (LIMR Development Inc. (LDI)); David Munn and Andrew Mellor (Medical College of Georgia); and Charles Link, Mario Mautino and Nick Vahanian (New Link Genetics Corporation) for productive ongoing discussions of IDO and immune pathobiology in cancer and other settings. I acknowledge Richard Metz for contributing founding ideas about the function of IDO2 as discussed in our earlier publication and elaborated further in the model in Figure 5. My laboratory is supported by the National Cancer Institute R01 Grants CA82222, CA100123, CA109542 and by funds provided by the Lankenau Hospital Foundation. I declare competing interests as a consultant and major shareholder for New Link Genetics Corporation, which supports IDO and IDO2 research in my laboratory and is developing IDO and IDO2 related technology for the therapy of cancer and other chronic diseases associated with pathological immune suppression.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Prendergast, G. Immune escape as a fundamental trait of cancer: focus on IDO. Oncogene 27, 3889–3900 (2008). https://doi.org/10.1038/onc.2008.35
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2008.35
Keywords
This article is cited by
-
Roles of tumor-associated macrophages in anti-PD-1/PD-L1 immunotherapy for solid cancers
Molecular Cancer (2023)
-
Involvement of the kynurenine pathway in breast cancer: updates on clinical research and trials
British Journal of Cancer (2023)
-
A novel immunogenomic classification for prognosis in non-small cell lung cancer
Journal of Cancer Research and Clinical Oncology (2023)
-
Indoleamine 2,3-dioxygenase 2 immunohistochemical expression in medullary thyroid carcinoma: implications in prognosis and immunomodulatory effects
BMC Cancer (2022)
-
Association of PD-1 and PDL-1 gene polymorphisms with colorectal cancer risk and prognosis
Molecular Biology Reports (2022)