Abstract
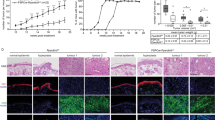
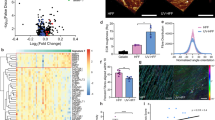
Xeroderma pigmentosum (XP) is a rare, recessively inherited genetic disease characterized by skin cancer proneness and premature aging in photoexposed area. The disease results from defective nucleotide excision repair of ultraviolet (UV)-induced DNA lesions. Reconstruction of group C (XP-C) skin in vitro previously suggested that patients' dermal fibroblasts might be involved in promoting skin cancer development, as they elicited microinvasions of both control and XP-C keratinocytes within dermal equivalents. Here we show that in the absence of UV exposure XP-C fibroblasts exhibit aged-like features such as an elongated and dendritic shape. We analysed the repertoire of expression of matrix metalloproteinases (MMPs) involved in skin aging and cancer. All XP-C fibroblasts tested in this study overexpressed specifically and significantly MMP1. MMP1 expression was also found increased in the dermis of XP-C skin sections suggesting the active contribution of XP-C mesenchymal cells to skin aging and exacerbated carcinogenesis. Increased MMP1 expression in cultured XP-C fibroblasts resulted from MMP1 mRNA accumulation and enhanced transcriptional activity of the MMP1 gene promoter. Deletion analysis revealed the essential role of AP-1 activation in constitutive MMP1 overexpression in XP-C primary fibroblasts. In parallel, levels of reactive oxygen species and FOSB DNA-binding activity were found increased in XP-C fibroblasts. Altogether, these observations suggest that beyond its role in nucleotide excision repair the XPC protein may be important in cell metabolism and fate in the absence of UV.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Airola K, Fusenig NE . (2001). Differential stromal regulation of MMP-1 expression in benign and malignant keratinocytes. J Invest Dermatol 116: 85–92.
Angel P, Baumann I, Stein B, Delius H, Rahmsdorf HJ, Herrlich P . (1987). 12-O-tetradecanoyl-phorbol-13-acetate induction of the human collagenase gene is mediated by an inducible enhancer element located in the 5′-flanking region. Mol Cell Biol 7: 2256–2266.
Arnaudeau-Begard C, Brellier F, Chevallier-Lagente O, Hoeijmakers J, Bernerd F, Sarasin A et al. (2003). Genetic correction of DNA repair-deficient/cancer-prone xeroderma pigmentosum group C keratinocytes. Hum Gene Ther 14: 983–996.
Asselineau D, Bernhard B, Bailly C, Darmon M . (1985). Epidermal morphogenesis and induction of the 67 kD keratin polypeptide by culture of human keratinocytes at the liquid–air interface. Exp Cell Res 159: 536–539.
Benbow U, Schoenermark MP, Mitchell TI, Rutter JL, Shimokawa K, Nagase H et al. (1999). A novel host/tumor cell interaction activates matrix metalloproteinase 1 and mediates invasion through type I collagen. J Biol Chem 274: 25371–25378.
Bernerd F, Asselineau D . (1997). Successive alteration and recovery of epidermal differentiation and morphogenesis after specific UVB-damages in skin reconstructed in vitro. Dev Biol 183: 123–138.
Bernerd F, Asselineau D, Frechet M, Sarasin A, Magnaldo T . (2005). Reconstruction of DNA repair-deficient xeroderma pigmentosum skin in vitro: a model to study hypersensitivity to UV light. Photochem Photobiol 81: 19–24.
Bernerd F, Asselineau D, Vioux C, Chevallier-Lagente O, Bouadjar B, Sarasin A et al. (2001). Clues to epidermal cancer proneness revealed by reconstruction of DNA repair-deficient xeroderma pigmentosum skin in vitro. Proc Natl Acad Sci USA 98: 7817–7822.
Bootsma D, Weeda G, Vermeulen W, van Vuuren H, Troelstra C, van der Spek P et al. (1995). Nucleotide excision repair syndromes: molecular basis and clinical symptoms. Philos Trans R Soc Lond B Biol Sci 347: 75–81.
Brenneisen P, Briviba K, Wlaschek M, Wenk J, Scharffetter-Kochanek K . (1997). Hydrogen peroxide (H2O2) increases the steady-state mRNA levels of collagenase/MMP-1 in human dermal fibroblasts. Free Radic Biol Med 22: 515–524.
Brinckerhoff CE, Rutter JL, Benbow U . (2000). Interstitial collagenases as markers of tumor progression. Clin Cancer Res 6: 4823–4830.
Cat B, Stuhlmann D, Steinbrenner H, Alili L, Holtkotter O, Sies H et al. (2006). Enhancement of tumor invasion depends on transdifferentiation of skin fibroblasts mediated by reactive oxygen species. J Cell Sci 119: 2727–2738.
Chung JH, Kang S, Varani J, Lin J, Fisher GJ, Voorhees JJ . (2000). Decreased extracellular-signal-regulated kinase and increased stress-activated MAP kinase activities in aged human skin in vivo. J Invest Dermatol 115: 177–182.
Chung JH, Seo JY, Choi HR, Lee MK, Youn CS, Rhie G et al. (2001). Modulation of skin collagen metabolism in aged and photoaged human skin in vivo. J Invest Dermatol 117: 1218–1224.
Collier IE, Smith J, Kronberger A, Bauer EA, Wilhelm SM, Eisen AZ et al. (1988). The structure of the human skin fibroblast collagenase gene. J Biol Chem 263: 10711–10713.
Comoglio PM, Trusolino L . (2005). Cancer: the matrix is now in control. Nat Med 11: 1156–1159.
D'Errico M, Parlanti E, Teson M, de Jesus BM, Degan P, Calcagnile A et al. (2006). New functions of XPC in the protection of human skin cells from oxidative damage. EMBO J 25: 4305–4315.
Del Rio M, Larcher F, Serrano F, Meana A, Munoz M, Garcia M et al. (2002). A preclinical model for the analysis of genetically modified human skin in vivo. Hum Gene Ther 13: 959–968.
DePinho RA . (2000). The age of cancer. Nature 408: 248–254.
Egeblad M, Werb Z . (2002). New functions for the matrix metalloproteinases in cancer progression. Nat Rev Cancer 2: 161–174.
Fisher GJ, Datta SC, Talwar HS, Wang ZQ, Varani J, Kang S et al. (1996). Molecular basis of sun-induced premature skin ageing and retinoid antagonism. Nature 379: 335–339.
Fligiel SE, Varani J, Datta SC, Kang S, Fisher GJ, Voorhees JJ . (2003). Collagen degradation in aged/photodamaged skin in vivo and after exposure to matrix metalloproteinase-1 in vitro. J Invest Dermatol 120: 842–848.
Fratelli M, Goodwin LO, Orom UA, Lombardi S, Tonelli R, Mengozzi M et al. (2005). Gene expression profiling reveals a signaling role of glutathione in redox regulation. Proc Natl Acad Sci USA 102: 13998–14003.
Frechet M, Bergoglio V, Chevallier-Lagente O, Sarasin A, Magnaldo T . (2006). Complementation assays adapted for DNA repair-deficient keratinocytes. Methods Mol Biol 314: 9–23.
Frisch SM, Reich R, Collier IE, Genrich LT, Martin G, Goldberg GI . (1990). Adenovirus E1A represses protease gene expression and inhibits metastasis of human tumor cells. Oncogene 5: 75–83.
Gray ST, Wilkins RJ, Yun K . (1992). Interstitial collagenase gene expression in oral squamous cell carcinoma. Am J Pathol 141: 301–306.
Inoue D, Kido S, Matsumoto T . (2004). Transcriptional induction of FosB/DeltaFosB gene by mechanical stress in osteoblasts. J Biol Chem 279: 49795–49803.
Jorissen HJ, Ulery PG, Henry L, Gourneni S, Nestler EJ, Rudenko G . (2007). Dimerization and DNA-binding properties of the transcription factor DeltaFosB. Biochemistry 46: 8360–8372.
Karin M, Liu Z, Zandi E . (1997). AP-1 function and regulation. Curr Opin Cell Biol 9: 240–246..
Kerkela E, Ala-aho R, Klemi P, Grenman S, Shapiro SD, Kahari VM et al. (2002). Metalloelastase (MMP-12) expression by tumour cells in squamous cell carcinoma of the vulva correlates with invasiveness, while that by macrophages predicts better outcome. J Pathol 198: 258–269.
Kerkela E, Saarialho-Kere U . (2003). Matrix metalloproteinases in tumor progression: focus on basal and squamous cell skin cancer. Exp Dermatol 12: 109–125.
Khorramizadeh MR, Tredget EE, Telasky C, Shen Q, Ghahary A . (1999). Aging differentially modulates the expression of collagen and collagenase in dermal fibroblasts. Mol Cell Biochem 194: 99–108.
Kraemer KH . (1997). Sunlight and skin cancer: another link revealed. Proc Natl Acad Sci USA 94: 11–14.
Milde-Langosch K, Roder H, Andritzky B, Aslan B, Hemminger G, Brinkmann A et al. (2004). The role of the AP-1 transcription factors c-Fos, FosB, Fra-1 and Fra-2 in the invasion process of mammary carcinomas. Breast Cancer Res Treat 86: 139–152.
Monhian N, Jewett BS, Baker SR, Varani J . (2005). Matrix metalloproteinase expression in normal skin associated with basal cell carcinoma and in distal skin from the same patients. Arch Facial Plast Surg 7: 238–243.
Mueller MM, Fusenig NE . (2004). Friends or foes—bipolar effects of the tumour stroma in cancer. Nat Rev Cancer 4: 839–849.
Nishigori C, Miyachi Y, Imamura S, Takebe H . (1989). Reduced superoxide dismutase activity in xeroderma pigmentosum fibroblasts. J Invest Dermatol 93: 506–510.
Otto AI, Riou L, Marionnet C, Mori T, Sarasin A, Magnaldo T . (1999). Differential behaviors toward ultraviolet A and B radiation of fibroblasts and keratinocytes from normal and DNA-repair-deficient patients. Cancer Res 59: 1212–1218.
Radisky DC, Levy DD, Littlepage LE, Liu H, Nelson CM, Fata JE et al. (2005). Rac1b and reactive oxygen species mediate MMP-3-induced EMT and genomic instability. Nature 436: 123–127.
Rhie G, Shin MH, Seo JY, Choi WW, Cho KH, Kim KH et al. (2001). Aging- and photoaging-dependent changes of enzymic and nonenzymic antioxidants in the epidermis and dermis of human skin in vivo. J Invest Dermatol 117: 1212–1217.
Rosenfeldt H, Lee DJ, Grinnell F . (1998). Increased c-fos mRNA expression by human fibroblasts contracting stressed collagen matrices. Mol Cell Biol 18: 2659–2667.
Rutter JL, Benbow U, Coon CI, Brinckerhoff CE . (1997). Cell-type specific regulation of human interstitial collagenase-1 gene expression by interleukin-1 beta (IL-1 beta) in human fibroblasts and BC-8701 breast cancer cells. J Cell Biochem 66: 322–336.
Shimizu Y, Iwai S, Hanaoka F, Sugasawa K . (2003). Xeroderma pigmentosum group C protein interacts physically and functionally with thymine DNA glycosylase. EMBO J 22: 164–173.
Shimokawa N, Kumaki I, Qiu CH, Ohmiya Y, Takayama K, Koibuchi N . (2005). Extracellular acidification enhances DNA binding activity of MafG-FosB heterodimer. J Cell Physiol 205: 77–85.
Shin MH, Rhie GE, Kim YK, Park CH, Cho KH, Kim KH et al. (2005). H2O2 accumulation by catalase reduction changes MAP kinase signaling in aged human skin in vivo. J Invest Dermatol 125: 221–229.
Stamenkovic I . (2003). Extracellular matrix remodelling: the role of matrix metalloproteinases. J Pathol 200: 448–464.
Stein B, Rahmsdorf HJ, Steffen A, Litfin M, Herrlich P . (1989). UV-induced DNA damage is an intermediate step in UV-induced expression of human immunodeficiency virus type 1, collagenase, c-fos, and metallothionein. Mol Cell Biol 9: 5169–5181.
Sternlicht MD, Werb Z . (2001). How matrix metalloproteinases regulate cell behavior. Annu Rev Cell Dev Biol 17: 463–516.
Tsukifuji R, Tagawa K, Hatamochi A, Shinkai H . (1999). Expression of matrix metalloproteinase-1, -2 and -3 in squamous cell carcinoma and actinic keratosis. Br J Cancer 80: 1087–1091.
Vandesompele J, De Preter K, Pattyn F, Poppe B, Van Roy N, De Paepe A et al. (2002). Accurate normalization of real-time quantitative RT-PCR data by geometric averaging of multiple internal control genes. Genome Biol 3: RESEARCH0034.
Varani J, Schuger L, Dame MK, Leonard C, Fligiel SE, Kang S et al. (2004). Reduced fibroblast interaction with intact collagen as a mechanism for depressed collagen synthesis in photodamaged skin. J Invest Dermatol 122: 1471–1479.
Vu TH, Werb Z . (2000). Matrix metalloproteinases: effectors of development and normal physiology. Genes Dev 14: 2123–2133.
Vuillaume M, Daya-Grosjean L, Vincens P, Pennetier JL, Tarroux P, Baret A et al. (1992). Striking differences in cellular catalase activity between two DNA repair-deficient diseases: xeroderma pigmentosum and trichothiodystrophy. Carcinogenesis 13: 321–328.
Wenk J, Brenneisen P, Wlaschek M, Poswig A, Briviba K, Oberley TD et al. (1999). Stable overexpression of manganese superoxide dismutase in mitochondria identifies hydrogen peroxide as a major oxidant in the AP-1-mediated induction of matrix-degrading metalloprotease-1. J Biol Chem 274: 25869–25876.
White LA, Brinckerhoff CE . (1995). Two activator protein-1 elements in the matrix metalloproteinase-1 promoter have different effects on transcription and bind Jun D, c-Fos, and Fra-2. Matrix Biol 14: 715–725.
Acknowledgements
Dr Asselineau and Dr J Leclaire are gratefully acknowledged for continuous support and encouragements. We are indebted to V Marty, C Pierrard and Dr C Marionnet for their expert help. We are also grateful to Dr A Jalil for confocal microscopy. We thank Professor P Herrlich and Professor CE Brinckerhoff for DNA reporter constructs. Many thanks to F Duvigneau for editing English usage in the article. TM gratefully acknowledges fundings from the Association pour la Recherche sur le Cancer (no. 3590), the Fondation de l'Avenir, the Société Française de Dermatologie, the Association Française contre les Myopathies. AS thanks the association ‘Les enfants de la Lune’ for its support.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Supplementary Information accompanies the paper on the Oncogene website (http://www.nature.com/onc).
Supplementary information
Rights and permissions
About this article
Cite this article
Fréchet, M., Warrick, E., Vioux, C. et al. Overexpression of matrix metalloproteinase 1 in dermal fibroblasts from DNA repair-deficient/cancer-prone xeroderma pigmentosum group C patients. Oncogene 27, 5223–5232 (2008). https://doi.org/10.1038/onc.2008.153
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2008.153