Abstract
Background:
Body mass index (BMI) may cluster in space among adults and be spatially dependent. Whether BMI clusters among children and how age-specific BMI clusters are related remains unknown. We aimed to identify and compare the spatial dependence of BMI in adults and children in a Swiss general population, taking into account the area’s income level.
Methods:
Geo-referenced data from the Bus Santé study (adults, n=6663) and Geneva School Health Service (children, n=3601) were used. We implemented global (Moran’s I) and local (local indicators of spatial association (LISA)) indices of spatial autocorrelation to investigate the spatial dependence of BMI in adults (35–74 years) and children (6–7 years). Weight and height were measured using standardized procedures. Five spatial autocorrelation classes (LISA clusters) were defined including the high–high BMI class (high BMI participant’s BMI value correlated with high BMI-neighbors’ mean BMI values). The spatial distributions of clusters were compared between adults and children with and without adjustment for area’s income level.
Results:
In both adults and children, BMI was clearly not distributed at random across the State of Geneva. Both adults’ and children’s BMIs were associated with the mean BMI of their neighborhood. We found that the clusters of higher BMI in adults and children are located in close, yet different, areas of the state. Significant clusters of high versus low BMIs were clearly identified in both adults and children. Area’s income level was associated with children’s BMI clusters.
Conclusions:
BMI clusters show a specific spatial dependence in adults and children from the general population. Using a fine-scale spatial analytic approach, we identified life course-specific clusters that could guide tailored interventions.
Similar content being viewed by others
Introduction
An increasing body of evidence shows that neighborhood socioeconomic context, measured by neighborhood deprivation, neighborhood segregation or population density, predicts the development of obesity and other related health outcomes.1, 2, 3 Poorer physical infrastructures and transports, worse housing conditions, fewer health and community services and lower stocks of social capital in poor neighborhoods are factors that have been proposed to explain how the place of residence might directly affect health.4 In addition, network phenomena, including social network, appear to be crucial factors in the biological and behavioral traits of obesity as it seems to spread through social ties.5
To best take into account the elements mentioned above, spatial analysis methods have been developed and introduced in epidemiological research to explore the link between the place of residence and health.6, 7 Spatial clusters of a trait can be determined by its spatial dependence (spatial autocorrelation), which is defined as a covariation of properties within a geographic space.
Among adults, diet-related factors such as body mass index (BMI), seem to be clustered in space and seem to be spatially dependent, according to community characteristics.8 The latter, such as BMI at proximal locations, may be correlated either positively or negatively.
Childhood excess weight is associated with an increased risk of obesity in adulthood, and corresponding increase in health risks.9 Geographical mapping of disease (for example, diabetes and leukemia) in children has been reported, but fine-scale spatial dependence analyses of BMI data in children are currently lacking. In addition, the relationship between BMI spatial clusters in adults and children is unknown. One might expect a correlation between BMI spatial clusters of adults and children due to common neighborhood-related risk factors of obesity.10 Among these risk factors, income level is thought to be of major importance and should therefore be considered when conducting BMI spatial dependence analyses.
It is important to understand the similarities and differences between age-specific BMI clusters within a given population, because spatial analyses of BMI are being increasingly proposed to identify specific areas to intervene (for example, specific local prevention campaigns, urban planning and food environment).11
Using geocoded measurements of BMI at the individual level, we aimed to identify and compare spatial dependence of BMI in adults and children from the general population. We then considered the effect of the area’s income level on age-specific BMI spatial dependence.
Subjects and methods
Adult participants
Data on adults were collected using the Bus Santé study.12 The Bus Santé study is a cross-sectional population-based study, which collects information on cardiovascular risk factors. Every year, a representative stratified sample of 500 men and 500 women from the population (∼5 00 000 inhabitants) of the State of Geneva (surface: 282.5 km2), Switzerland, is recruited and studied. Three stations receive participants. The first two stations are fixed and are based within the Geneva University Hospitals. The third station is a mobile medical unit, which visits three parts of the State of Geneva. Four trained collaborators interview and examine the participants. All procedures are reviewed and standardized across technicians on a regular basis.
Subjects are selected independently throughout each year to represent the State’s ∼1 00 000 male and 1 00 000 female non-institutionalized residents aged 35–74. Eligible subjects are identified using a standardized procedure using an annual residential list established by the local government. This listing includes all potentially eligible participants, except illegal immigrants. Stratified random sampling on the basis of the list by gender, within 10-year age strata, is proportional to the corresponding population distributions. Selected subjects are mailed an invitation to participate and, if they do not respond, up to seven telephone attempts are made at different times on various days of the week. If telephone contact is unsuccessful, two more letters are mailed. Subjects that are not reached are replaced using the same selection protocol. Subjects who refuse to participate are not replaced. Each participant receives several self-administered, standardized questionnaires covering the risk factors for the major lifestyle-chronic diseases. Geographic coordinates of the postal address is used for individual geographic information. For this analysis, data from 2001–2010 were used. The 2001–2010 mean participation rate was 60% (range: 55–65%).
Each participant brings along their filled-in questionnaires, which are checked for correct completion by trained interviewers. Body weight is measured with the subject lightly dressed, without shoes and using a medical scale (precision 0.5 kg), and standing height is measured using a medical gauge (precision 1 cm). BMI is calculated as weight (in kg)/height (in m2).
The Institutional Ethics Committee approved the study. All participants gave a written informed consent.
Children participants
Data on children were collected using the 2011 database from the School Health Service of Geneva (http://www.ge.ch/ssj/). The School Health Service of Geneva systematically conducts a medical visit for children entering the public school system in the State of Geneva. During this visit, weight and height are measured by school nurses using regularly calibrated scales. Weight was measured while the children were in their underclothes. BMI is calculated as weight (in kg)/height (in m2). In children, BMI typically varied with age and sex, and BMI is generally converted into a BMI z score when multiple age categories are compared. Because the children data were collected within a single-age category, we did not use the BMI z score. The effect of gender on BMI within the age 6–7 years is also very limited, as illustrated by the superposable curves of gender-specific BMI reported by the International Obesity Task Force.13 Geographic coordinates of the postal address were used for individual geographic information.
Adults and children with incomplete information on height, weight or addressses were excluded.
Area’s income level
Data on area’s income level were obtained from the 2009 Geneva Census (Office Cantonal de la Statistique, www.ge.ch/statistique). Information on median annual income in Swiss francs CHF (1 CHF≈1 US, November 2013) covered 475 areas (statistical subsectors) of the Geneva State. The income value was attributed to adult and child individuals on the basis of the inclusion of their postal address within the corresponding statistical subsector.
Spatial analysis
Local Indicators of Spatial Association (LISA)
Using the geographical coordinates of the postal address of the children and of the adults, we measured the spatial autocorrelation of BMI using the OpenGeoda software.14 A measure of local spatial autocorrelation has been carried out with LISA, developed by Anselin.15 LISA indicators are statistics that measure the spatial dependence and evaluate the existence of local clusters in the spatial arrangement of a given variable. They are based on a statistical index I developed by Moran16 to measure the global spatial autocorrelation of the overall clustering of the data in the area under investigation. Moran’s I ranges from 1 (negative spatial autocorrelation) to 1 (complete spatial dependence), with 0 indicating the absence of spatial dependence (that is, random distribution).
We used univariate LISA within a given spatial weighting scheme (spatial lag, described below). This index was used to identify local spatial autocorrelation clusters of BMI in adults’ and children’s data. For each participant, the relationship between BMI and the mean of BMI in a given neighborhood (spatial lag) was calculated. A standardized scattergram of this relation provides four distinct classes depending on the type of relationship between a participant’s BMI and the mean BMI of the participant’s nearest neighbors: (a) high BMI values associated with high BMI weighted values (high–high relationship), (b) low BMI values associated with low BMI weighted values (low–low relationship), (c) a low–high relationship and (d) a high–low relationship (Supplementary Figure S1). The attribution of individuals to these four classes depends on the results of a statistical significance test. This test consists in performing random Monte Carlo permutations among the sites located in the spatial lag to compare the observed LISA to the LISA corresponding to the random permutations.15 For this analysis, significance was calculated on the basis of a standard of 999 permutations corresponding to a pseudo P-value significance threshold of 0.01, and to a confidence level of 99%. If the test is significant—the observed LISA is statistically larger (or smaller in the case of a negative relationship) than the local indices resulting from all random permutations —an individual is attributed to one of the four classes. If the test is not significant, the individual remains in a neutral class (no spatial dependence). To assess the impact of area’s income level on BMI spatial dependence, we repeated the same analysis using BMI adjusted for area’s income level and compared results with and without adjustment for area’s income level. Median regression was used to obtain area’s income-adjusted BMI.17 To determine whether spatial dependence of BMI was stable during the 2001–2010 study periods and whether combining samples is appropriate, we compared Moran’s I for the 2001–2005 (n=3755) and the 2006–2010 (n=2908) periods using Kolmogorov–Smirnov tests.18 Comparison of Moran’s I for the 2001–2005 and for the 2006–2010 periods (Moran’s I for period 2001–2005 versus period 2001–2010, P-value=0.834; Moran’s I for period 2005–2010 versus period 2001–2010, P-value=0.653; Moran’s I for period 2001–2006 versus period 2001–2010, P-value=0.133) suggested that the distribution of the two adult samples was similar, allowing to combine BMI data of the two periods considered.
Maps
On the maps we produced, sampling sites which are statistically significant are displayed in colors, whereas sampling sites which are not are displayed in white. White dots show sampling places where the space is neutral (no spatial dependence). Red dots show clusters of locations where a participant’s high BMI value is spatially correlated with a high mean BMI value of the participant’s nearest neighbors. Blue dots show clusters of locations where a participant’s low BMI value is spatially correlated with a low mean BMI value of the participant’s nearest neighbors. Purple dots show low–high associations, and pink dots high–low associations. We presented maps derived from unadjusted (panel A) and area’s income-adjusted BMI (panel B), respectively.
Spatial lag
We decided to analyze the BMI in children and adults within 1800 m around each individual’s postal address. This choice was made on the basis of three criteria. First, the distance from which there is no neighborless individual is 1150 m in children and 1300 m in adults. Second, it was necessary to ensure that the density of points within spatial lags is sufficient (connectivity): in adults for 1800 m, the first percentile of the distribution contains 72 individuals that had between 2 and 22 neighbors; the class with the maximum number of neighbors was the one with percentile 100, with one individual having 2024 neighbors. In children, the first percentile contained 29 individuals that had between 2 and 11 neighbors; the class with the maximum number of neighbors was the one with percentile 100 with six individuals having between 969 and 979 neighbors. Finally, we produced a correlogram (Supplementary Figure S1) showing that the global Moran’s I is very low for both adults and children datasets, suggesting a low global spatial dependence. The correlogram also emphasizes the fact that, for a spatial lag of 1800 m, Moran’s I shows the same value for adults and children (Supplementary Figure S1).
Aggregated LISA and comparison of age-specific BMI clusters
In order to compare LISA indices characterizing age-specific BMI distributions over the study area, we first created a common geographical unit of reference. We built a regular grid composed of 3009 cells (59 × 51) of 500 × 500 m. This size represents a compromise in order to get the highest possible spatial resolution throughout the whole State of Geneva with a sufficient number of adult and child individuals per cell. The grid was superposed on the adult points contained within 526 cells, and on the children points contained within 419 cells. In adults, frequencies per cell ranged from 1 (in 34 cells) to 105, with a mean value of 16.6 and a median value of 9. In children, frequencies per cell range from 1 (in 81 cells) to 67, with a mean value of 9.2 and a median value of 5. We constituted the final working grid with the 172 cells containing at least five adults and five children.
We used SQL queries to count the number of individuals per cell, and to count the number of adult and child individuals belonging to each of the LISA cluster categories (one not significant and four significant classes). We then processed the different aggregated LISA indicators to characterize the compared spatial dependence of BMI in adults and children within the 384 cells. For each of the four classes, (n) is described previously ((1) high–high, (2) low–low, (3) low–high and (4) high–low), we calculated CLn indicators that allow the comparison of the ratio of the type of local spatial dependence between adults and children in each cell of the grid. For example, if CL1=1, then there is parity between adults and children for LISA class high–high in the cell; if CL1<1, then there are more children than adults for LISA class high–high in the cell and if CL1>1, then there are more adults than children for LISA class high–high in the cell. More details on the C indicators are available in the Supplementary Materials.
Results
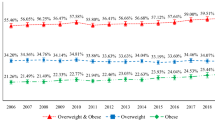
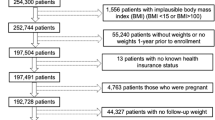
A total of 6663 adults and 3601 children were included in the analyses. In all, 146 adults and 69 children were excluded due to incomplete data. The mean age was 51.5 (s.d., 10.84) and 5.3 years (s.d., 0.47) for adults and children, respectively. The mean BMI was 25.1 (s.d., 4.23) kg/m2 and 15.6 (s.d., 1.69) kg/m2 for adults and children, respectively. 12.2% of the adults had a BMI of 30 kg/m2 or more (obesity), whereas 2.1% of the children had a BMI of 20 kg/m2 or more, suggesting obesity according to the International Obesity Task Force.13 Median (min–max range) area’s annual income level was 44 338CHF (6'562CHF–295'784CHF).
LISA clusters for the 6663 adults are shown in Figure 1, panel a. Within a 1800 m spatial lag, 3031 (45.5%) individuals presented no BMI spatial dependence, 864 (13.0%) had high BMI values significantly correlated with high neighborhood mean BMI values (high–high cluster class), 1087 (16.3%) showed low BMI values significantly correlated with low neighborhood mean BMI values (low–low cluster class), 911 (13.7%) belonged to the low–high cluster class and 770 (11.6%) belonged to the high–low cluster class.
LISA for the 6663 adults geo-referenced at their postal address, Bus Santé study, 2001–2010, panel a) unadjusted, panel b) adjusted for area’s income level. White dots show sampling places where the space is neutral (no spatial dependence). Red dots show clusters of high–high locations where an adult high BMI value is correlated with a high mean BMI value among the adults located within a radius of 1800 m (weighting scheme established on the basis of a Moran’s I correlogram). Blue dots show clusters of low–low locations where an adult low BMI value is correlated with a low mean BMI value the adults located within a radius of 1800 m. Purple dots show low–high associations, and pink dots high–low associations.
LISA clusters for the 3601 children are shown in Figure 2, panel a. Within a 1800 m spatial lag, 1923 (53.4%) individuals showed no BMI spatial dependence, 470 (13.0%) had high BMI values significantly correlated with high neighborhood mean BMI values (high–high cluster class), 410 (11.4%) showed low BMI values significantly correlated with low neighborhood mean BMI values (low–low cluster class), 563 (15.6%) belonged to the low–high cluster class and 235 (6.5%) belonged to the high–low cluster class.
LISA for the 3601 children geo-referenced at their postal address, Geneva School Health Service database, 2011, panel a) unadjusted, panel b) adjusted for area’s income level. White dots show sampling places where the space is neutral (no spatial dependence). Red dots show clusters of high–high locations where a child high BMI value is correlated with a high mean BMI value among the children located within a radius of 1800 m (weighting scheme established on the basis of a Moran’s I correlogram). Blue dots show clusters of low–low locations where a child low BMI value is correlated with a low mean BMI value among the children located within a radius of 1800 m. Purple dots show low–high associations, and pink dots high–low associations.
Both maps show clear BMI clusters with the high–high autocorrelation class predominantly on the right shore of the Lake Geneva and of the Rhone river, and the low–low autocorrelation class predominantly on the left shore of the Geneva lake and of the Rhone river.
Figure 3, panel a illustrates the CL1 indicator, comparing the ratio of adult and child individuals attributed to the high–high BMI LISA cluster class. We identified 28 areas (16.3% of the cells, dark orange), where the percentage of child individuals belonging to a high–high BMI cluster was higher than the percentage of adult individuals belonging to the same category. There were 51 cells (29.6% of the cells, purple), where the proportion of adults belonging to a high–high cluster was higher than the same class in children. There were 93 cells (54.1%, in pale yellow), where the spatial behavior of adult and children CL1 clusters was practically identical. Conversely, the Supplementary Figure S2 panel A illustrates the CL2 indicator comparing the ratio of adult and children individuals attributed to the low–low BMI LISA cluster class. Low–low BMI areas much predominant in children are shown in dark orange (24 cells, 14.0%), low–low BMI areas predominant in adults are shown in purple (38 cells, 22.1%). There were 110 cells (63.9%), where the spatial behavior of adult and children CL2 clusters was almost the same. These results suggested that both high–high and low–low BMI clustered differently in adults and children.
CL1 indicator comparing the ratio of adult and children individuals attributed to the high–high BMI LISA cluster class, panel a) unadjusted, panel b) adjusted for area’s income level. White cells (CL1≈1): there is parity between adults and children for LISA class high–high in the cell; orange cells (CL1<1): there are more children than adults for LISA class high–high in the cell; purple cells (CL1>1): there are more adults than children for LISA class high–high in the cell. The discretization method is based on equal intervals and adapted for comparison purpose, maximum CL1 index value=2, minimum CL1 value=0.5, range=1.5.
Impact of area’s income level on spatial dependence of BMI
LISA clusters adjusted for area’s annual income level in the 6663 adults are shown in Figure 1, panel b. While the number of individuals in each of the five categories slightly changed, cluster distribution obtained with and without adjustment for area’s annual income level remained very similar. Conversely, in the 3601 children, LISA clusters distribution was obtained using BMI adjusted for area’s annual income level Figure 2, panel b differed meaningfully from cluster distribution that was obtained using unadjusted BMI. Adjusting for area’s annual income level mainly mitigated the high–high cluster.
Adjustment for area’s annual income level neutralized the high–high BMI cluster areas, where the percentage of children individuals was higher than the percentage of adult individuals in unadjusted analysis (dark orange). Areas of high–high BMI clusters, where the percentage of adult individuals was higher than the percentage of children individuals (Figure 3 panel b) and areas of low–low BMI clusters (of both adults and children) were not affected by the adjustment for area’s annual income (Supplementary Figure S2 panel B).
Discussion
Using geo-referenced measurements of BMI at the individual level in both adults and children from the general population, we identified adult- and children-specific clusters highlighting a particular structure in the spatial distribution of high and low BMI values in the State of Geneva. In adults and children, BMI is not distributed at random and shows a spatial dependence. We found that, clusters of higher BMI in adults and children are located in close, yet different areas of the State. In addition, we found that area’s income level was associated with children’s BMI spatial dependence.
Previous reports have used spatial analyses to identify clusters of obesity and obesity-related factors among adult populations.19, 20, 21, 22 Studies specifically exploring the spatial distribution of BMI clusters in adults and children are, however, very limited.19 Our results clearly show that even within a relatively small region (282.5 km2), spatial dependence of BMI may vary significantly and may have opposite direction; high–high and low–low clusters coexist. Furthermore, we identified individuals who present opposite behavior (low–high and high–low classes). Overall, these observations underscore the need for collecting fine-scale information.
High–high clusters of children were found in certain areas of Geneva that were unmatched by high–high adult clusters. These unmatched clusters correspond to areas with higher proportion of children whose parents have a lower socioeconomic status than in other areas of the State.23 Compared with children whose parents have medium/high SES, children whose parents have low SES tend to have a higher prevalence of overweight in Switzerland and in the State of Geneva particularly.24 The fact that the adjustment for area’s income level clearly mitigates this high–high cluster in children, further suggests that neighborhood SES has an important role in children’s BMI.
The identification of clusters can guide local level interventions and might improve their efficacy, given that the interventions can then be tailored. Targeting of tailored interventions may even be more accurate on the basis of the value of LISA indices directly instead of cluster membership (maps not shown). The type of effective interventions, whether at the community, home/family or primary health care levels, varies across life course.25 Our cluster comparison analysis shows that BMI clusters in adults and children are geographically distinct and could therefore be used to tailoring interventions on the basis of the life course stage (for example, childhood and adulthood) in addition to tailoring intervention based on the geographical area.
Spatial-based information on health risk factors or disease is increasingly used and is being suggested as a tool to improve public health. Spatial-based information on BMI such as the present study can have both long-term and short-term impacts. In the long term, geo-referenced information on BMI could lead to specific recommendations for future healthy urban planning (type of housing, food environment and type of urban environment). In the short term, the use of spatial approaches can allow the identification of specific areas to intervene, to support specific prevention campaigns, for example. Models are being used in the UK to identify areas where anti-obesity policies should be implemented.26 But it was largely unknown whether areas to intervene are common in adults and children. Our results suggest that specific areas of high and low BMI in adults and children are not identical.
Generally, association studies on BMI did not account for spatial connections and assumed independence between observations. Our results clearly show that this assumption is not correct. This may explain some of the inconsistencies reported on the impact of social and built environment on obesity.26 In addition, because a potential reason for spatial clustering is shared predictor variables that cluster in space, this novel result suggests that predictor variables that cluster in space are different in adults and children. We identified an association of area’s income level with BMI in children. Further work should identify other social (for example, education) and environmental (for example, built area, green spaces and services) factors that would explain, at least in part, the observed spatial dependence.
Our study presents several strengths. Indeed, most studies defined neighborhoods by predefined unit (for example, census and counties). Because such studies focus on the internal characteristics of the unit, it has been suggested that this approach ignores any effect on individual health resulting from interactions between nearby neighborhoods.19 To identify clusters, we did not use a predefined unit but instead considered space as a continuum. Moreover, previous studies generally relied on self-reported height and weight, which is subject to reporting bias. Here, we calculated BMI based on the measured weight and height. Finally, we used the Moran’s I indicator, which has been shown to be a valid and robust indicator,27 and considered area’s income level in the analysis.
When interpreting the findings of this study, one also has to keep in mind its limitations. The study periods between the two databases are not the same. To allow a meaningful geographical coverage of the State of Geneva, data for the period 2001–2010 of the Bus Santé study were collected, whereas the data of the children were collected for the year 2011. We cannot exclude that adult clusters differ in 2001–2010 and 2011. The children attending private schools, 10% in the State of Geneva, were not included because the School Health Service of Geneva does not have the mandate to carry out health controls in private schools. As regards spatial statistic parameters, we chose to use a 1800-m spatial lag, but other choices may produce slightly different results. Yet, we tested the robustness of our findings using different spatial lag definitions (for example, different weighting distances, different numbers of neighbors) and found no meaningful difference in the results (that is, clusters). We lack information on the participants’ affiliation and cannot exclude that some participants were in some degrees affiliated. Because BMI in affiliated individuals has been shown to be correlated, this may have created clusters that would have been geographically superposed. Yet, we checked the adults’ and children’s addresses and found no overlap, which suggests, for children aged 6–7, a first degree affiliation is very unlikely. Because our outcome was BMI and not obesity, the identified clusters should not be interpreted as clusters of obesity. We limited our analyses to continuous BMI and avoided limitations of BMI categories, but we cannot exclude age-related variance in obesity prevalence as a limitation. We represented static points in time and no spatiotemporal information, which may be of interest. However, the number of observations needed in order to have sufficient data to conduct period specific analysis would have been meaningfully increased. While recruitment methods of the Bus Santé study aimed at collecting information on a representative sample of the general population, adult participants and non-participants to the Bus Santé study may differ and participation bias cannot be excluded. Of note to reduce the risk of participation bias, the Bus Santé study has—in addition to stationary clinics—a mobile examination unit that covers major area of the State. Among children, the fact that health exam in the Geneva public schools is mandatory mitigates the risk of participation bias.
This is the first study to compare adult and children spatial distribution of BMI at a fine geographic scale. Children’s BMI like adults’ BMI cluster in space yet in different area. Our approach identified areas where adults- and children-specific BMI-related health policies could be implemented.
References
Diez Roux AV . Investigating neighborhood and area effects on health. Am J Public Health 2001; 91: 1783–1789.
Ludwig J, Sanbonmatsu L, Gennetian L, Adam E, Duncan GJ, Katz LF et al. Neighborhoods, obesity and diabetes—a randomized social experiment. N Engl J Med 2011; 365: 1509–1519.
Rehkopf DH, Haughton LT, Chen JT, Waterman PD, Subramanian SV, Krieger N . Monitoring socioeconomic disparities in death: comparing individual-level education and area-based socioeconomic measures. Am J Public Health 2006; 96: 2135–2138.
Smith GD, Hart C, Watt G, Hole D, Hawthorne V . Individual social class, area-based deprivation, cardiovascular disease risk factors and mortality: the Renfrew and Paisley Study. J Epidemiol Community Health 1998; 52: 399–405.
Christakis NA, Fowler JH . The spread of obesity in a large social network over 32 years. N Engl J Med 2007; 357: 370–379.
Auchincloss AH, Gebreab SY, Mair C, Diez Roux AV . A review of spatial methods in epidemiology, 2000–2010. Annu Rev Public Health 2012; 33: 107–122.
Charreire H, Casey R, Salze P, Simon C, Chaix B, Banos A et al. Measuring the food environment using geographical information systems: a methodological review. Public Health Nutr 2010; 13: 1773–1785.
Chen S, Florax RJ, Snyder S, Miller CC . Obesity and access to chain grocers. Econ Geogr 2010; 86: 431–452.
Singh AS, Mulder C, Twisk JW, van Mechelen W, Chinapaw MJ . Tracking of childhood overweight into adulthood: a systematic review of the literature. Obes Rev 2008; 9: 474–488.
Black JL, Macinko J . Neighborhoods and obesity. Nutr Rev 2008; 66: 2–20.
Penney TL, Rainham DG, Dummer TJ, Kirk SF . A spatial analysis of community level overweight and obesity. J Hum Nutr Diet 2013. doi: 10.1111/jhn.12055.
Guessous I, Bochud M, Theler JM, Gaspoz JM, Pechere-Bertschi A . 1999-2009 Trends in prevalence, unawareness, treatment and control of hypertension in Geneva, Switzerland. PLoS One 2012; 7: e39877.
Cole TJ, Bellizzi MC, Flegal KM, Dietz WH . Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 2000; 320: 1240–1243.
Anselin L, McCann M . OpenGeoDa, open source software for the exploration and visualization of geospatial data. In: Proceedings of the 17th ACM SIGSPATIAL International Conference on Advances in Geographic Information Systems. New York, NY, USA: ACM, 2009. pp 550–551.
Anselin L . Local indicators of spatial association—LISA. Geographical Analysis 1995; 27: 93–115.
Moran PAP . Notes on continuous stochastic phenomena. Biometrika 1950; 37: 17–23.
Wei Y, Pere A, Koenker R, He X . Quantile regression methods for reference growth charts. Stat Med 2006; 25: 1369–1382.
Corder GW, Foreman DI . Non-parametric Statistics For Non-Statisticians: A Step-By-Step Approach. Hoboken, NJ, USA: Wiley, 2009.
Chen DR, Wen TH . Elucidating the changing socio-spatial dynamics of neighborhood effects on adult obesity risk in Taiwan from 2001 to 2005. Health Plac 2010; 16: 1248–1258.
Drewnowski A, Rehm CD, Solet D . Disparities in obesity rates: analysis by ZIP code area. Soc Sci Med 2007; 65: 2458–2463.
Pouliou T, Elliott SJ . An exploratory spatial analysis of overweight and obesity in Canada. Prev Med 2009; 48: 362–367.
Michimi A, Wimberly MC . Spatial patterns of obesity and associated risk factors in the conterminous U.S. Am J Prev Med 2010; 39: e1–12.
CATIGE. Cohésion sociale 2011. Available at http://www.unige.ch/ses/lea/publications/Autrespub/Cohesion_sociale_CATIGE_nov2011.pdf.
Promotion Santé Suisse. 2010. Available at http://www.unige.ch/ses/lea/publications/Autrespub/Cohesion_sociale_CATIGE_nov2011.pdf.
PANORG. Evidence update on obesity prevention across the life-course 2012. Available at http://sydney.edu.au/medicine/public-health/panorg/research-themes/intervention/Obesity%20Review_2%20May%202012_for%20website.pdf.
Edwards KL, Clarke GP, Ransley JK, Cade J . The neighbourhood matters: studying exposures relevant to childhood obesity and the policy implications in Leeds, UK. J Epidemiol Community Health 2010; 64: 194–201.
Moore DA, Carpenter TE . Spatial analytical methods and geographic information systems: use in health research and epidemiology. Epidemiol Rev 1999; 21: 143–161.
Acknowledgements
The authors thank the collaborators of the Unit of Population Epidemiology. The study was supported by University Hospitals of Geneva and the General Directorate of Health, Canton of Geneva, Switzerland. IG is supported by a Swiss National Science Foundation grant (SNF 33CM30-124087/1).
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
GIRAPH Group Dr Nicola Cantoreggi (University of Geneva), Dr Joël Chételat (MFSA, Saint-Sulpice), Dr Jean Simos (University of Geneva). Members of the GIRAPH (Geographic Information Research and Analysis in Public Health) Group are listed above the references.
Supplementary Information accompanies this paper on the Nutrition & Diabetes website
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Guessous, I., Joost, S., Jeannot, E. et al. A comparison of the spatial dependence of body mass index among adults and children in a Swiss general population. Nutr & Diabetes 4, e111 (2014). https://doi.org/10.1038/nutd.2014.8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nutd.2014.8
This article is cited by
-
Geographic footprints of life expectancy inequalities in the state of Geneva, Switzerland
Scientific Reports (2021)
-
Overlapping spatial clusters of sugar-sweetened beverage intake and body mass index in Geneva state, Switzerland
Nutrition & Diabetes (2019)
-
Prevalence of reported high blood pressure in Canada: investigation of demographic and spatial trends
Journal of Public Health (2017)
-
Finding big shots: small-area mapping and spatial modelling of obesity among Swiss male conscripts
BMC Obesity (2016)