Abstract
Background:
Lycium barbarum polysaccharides (LBPs) are antioxidant and neuroprotective derivative from Wolfberry. However, whether LBP has a protective effect in non-alcoholic steatohepatitis (NASH)-induced hepatic injury is still unknown.
Objective:
We aimed to study the possible hepatoprotective effects and mechanisms of LBP on a diet-induced NASH rat model.
Methods and Design:
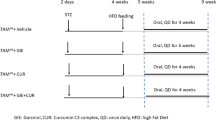
In this study, female rats were fed a high-fat diet to induce NASH with or without an oral 1 mg kg−1 LBP feeding daily for 8 weeks. After 8 weeks, blood serum and liver samples from each rat were subjected to histological analysis, biochemical and molecular measurements.
Results:
Compared with control rats, NASH rats showed typical NASH features including an increase in liver injury, lipid content, fibrosis, oxidative stress, inflammation and apoptosis. In contrast, NASH+LBP-co-treated rats showed (1) improved histology and free fatty acid levels; (2) re-balance of lipid metabolism; (3) reduction in profibrogenic factors through the TGF-β/SMAD pathway; (4) improved oxidative stress through cytochrome P450 2E1-dependent pathway; (5) reduction in hepatic pro-inflammatory mediators and chemokines production; and (6) amelioration of hepatic apoptosis through the p53-dependent intrinsic and extrinsic pathways. The preventive effects of LBP were partly modulated through the PI3K/Akt/FoxO1, LKB1/AMPK, JNK/c-Jun and MEK/ERK pathways and the downregulation of transcription factors in the liver, such as nuclear factor-κB and activator protein-1.
Conclusion:
LBP is a novel hepatoprotective agent against NASH caused by abnormal liver metabolic functions.
Similar content being viewed by others
Introduction
Non-alcoholic fatty liver disease (NAFLD) is a chronic metabolic liver disease that histologically resembles the alcohol-induced hepatic injury, but which is not from abuse of alcohol consumption (<20 g per day).1 In Western countries, NAFLD affects 20–40% of the adult populations and has the potential to be the most common liver disease.2, 3, 4 Non-alcoholic steatohepatitis (NASH), the extreme form of NAFLD, is characterized by an increase in fat deposition, fibrosis, oxidative stress and chronic inflammation in the liver. It is also the common cause of cirrhosis and could later progress to hepatocellular carcinoma, the life-threatening cancer.5 To date, the detailed mechanisms in the development of NASH remain not fully understood. However, a ‘multi-hit’ theory has been proposed to depict the key pathogenic processes of NASH development. In this theory, insulin resistance is thought to be the ‘first hit’ to the liver because it induces a net accumulation of lipid in hepatocytes that may cause the occurrence of following ‘hits’, such as oxidative stress, inflammation, fibrosis and apoptosis.6 Recently, some natural substances, including derivatives from foods or beverages, have been investigated for their protective effects in NAFLD/NASH-induced hepatic injury.7, 8
Lycium barbarum polysaccharides (LBPs) are the liquid fraction extracted from Wolfberry, the fruit of traditional Chinese medicinal plant L. barbarum, or Goji. In China, Goji has been used for centuries because it is believed to have positive effects on nourishing the liver and maintaining the health of the eyes.9 In the past decade, LBP has been studied for its therapeutic effects on human health. As a potent antioxidant, LBP enhances antioxidant biomarkers in human serum10 and protects the body from chemical- or exercise-induced toxicity through suppression of oxidative stress.11, 12, 13, 14 In cancer cell line, LBP treatment inhibited cell proliferation, arrested cell cycle in S phase, induced apoptosis and interrupted intracellular calcium balance.15 Finally, several reports demonstrated the anti-aging and neuroprotective properties of LBP both in vitro and in vivo.16, 17, 18 Although a recent study found that LBP attenuates alcohol-induced hepatic injury, lipid content and oxidative stress,19 the knowledge of the protective mechanisms of LBP on chronic liver diseases, particularly non-alcoholic liver diseases, is still inadequate.
In this study, we investigated the protective effects of LBP treatment along with the induction of NASH in a voluntary orally fed high-fat diet rat model. Co-treatment with LBP potently ameliorated the abnormal features in the NASH-damaged liver. Several molecular pathways, including MAPKs and LKB1/AMPK, linked the initial lipid imbalance and downstream effects. Thus, these data proved that LBP or Goji could be a useful food supplement in the prevention of chronic liver diseases.
Materials and methods
Rats and treatment
Eight-week healthy adult female Sprague–Dawley rats with body weight ranging from 195 to 200 g were purchased from the Laboratory Animal Unit, University of Hong Kong. Rats were kept under standard conditions for 3 days before the start of the experiment with free access to animal chow and tap water. The animals were divided into four groups (n=8 per group), namely: (1) control group; (2) NASH group; (3) vehicle-LBP group (1 mg kg−1 in 1 × phosphate-buffered saline; oral feeding; one time per day); and (4) NASH and LBP co-treatment group. The development of NASH in rats, including the recipe and preparation protocols of diet, was performed based on our previously described voluntary oral feeding NAFLD animal model.20, 21 Briefly, the diet provided 30% of its energy from fat, 35% from carbohydrate and 35% from protein with supplements of vitamins and minerals. After 8 weeks, rats were killed by an overdose of anesthesia (150 mg kg−1 pentobarbital, intraperitoneal injection) according to the protocols approved by the Committee of Animal Use for Research and Teaching at the University of Hong Kong. The Laboratory Animal Unit of the University of Hong Kong is accredited by the Association for Assessment and Accreditation of Laboratory Animal Care International. Blood and liver samples were collected for further analyses.
Processing of tissue and blood samples
Serum was collected by centrifugation of whole blood sample at 1000 × g for 10 min at 4 °C and stored at −80 °C. Liver tissue samples were fixed in 10% phosphate-buffered formalin, processed for histology and embedded in paraffin blocks. Five-micrometer tissue sections were cut and stained with hematoxylin and eosin, Sirius red and synaptophysin (DAKO, Glostrup, Denmark) for histological analysis under LEICA Qwin Image Analyser (Leica Microsystems Ltd., Milton Keynes, UK). The percentage area of the total amount of collagen was determined by the sum areas of Sirius red-positive stain divided by the sum areas of the reference field multiplied by 100. The NAFLD activity score of each group was calculated as previously described.22
Terminal deoxynucleotidyl transferase-mediated dUTP-nick end labeling assay
To demonstrate the apoptosis in the liver, the terminal deoxynucleotidyl transferase-mediated dUTP-nick end labeling (TUNEL) assay that detects 3′ hydroxyl ends in fragmented DNA as an early event in apoptotic cascade was used. After dewaxing and rehydration of the paraffin-embedded liver tissue sections, staining was performed according to the manufacturer’s instructions regarding the TUNEL assay by using the in situ cell death detection kit (Roche, Basel, Switzerland). DNase I recombinant in the sections was used as the positive control. Label solution without terminal transferase was used in place of TUNEL reaction mixture for negative control. The positive immunostaining of Fast Red of TUNEL was examined by light microscope (Zeiss Axiolab; Carl Zeiss Inc., Jena, Germany) and analyzed by ImageJ software (Bethesda, MD, USA).
Serum alanine aminotransferase assay
To evaluate the hepatic injury at the enzymatic level, serum alanine aminotransferase (ALT) level was measured by using ALT (SGPT) reagent set (Teco diagnostics, Anaheim, CA, USA) according to the manufacturer’s instructions.
Free fatty acid assay
To study the effect of LBP on lipid metabolism, blood serum free fatty acid (FFA) level of each rat was measured by using Cayman FFA assay kit (Cayman Chemical, Ann Arbor, MI, USA), and the final results were expressed as μM in the serum.
Measurement of malondialdehyde level
Levels of the end-product of lipid peroxidation (malondialdehyde (MDA)) in all liver tissue samples were determined by using a Bioxytech LPO-586 kit (Oxis Research, Portland, OR, USA). The reaction product was measured spectrophotometrically at 586 nm. Standard curves were constructed using 1,1,3,3-tetraethoxypropane as a standard. The MDA levels were normalized with corresponding protein amounts determined by a Bio-Rad Protein Assay Kit (Bio-Rad, Hercules, CA, USA) and expressed as percentage against the control level.
RNA extraction and reverse-transcription quantitative PCR
Total RNA of each rat was extracted from the liver sample by using illustra RNAspin mini kit (GE Healthcare, Buckinghamshire, UK). The preparation of the first-strand cDNA was conducted following the instruction of the SuperScript First-Strand Synthesis System (Invitrogen, Carlsbad, CA, USA).
The mRNA expression levels of target genes were measured by Takara SYBR premix Taq quantitative PCR system (Takara Bio Inc, Shiga, Japan) and in MyiQ2 real-time PCR machine (Bio-Rad). The primer sequences and annealing temperatures used in those real-time PCR reactions are listed in Supplementary Table S1. Parallel amplification of glyceraldehyde-3-phosphate dehydrogenase was used as the internal control. Relative quantification was done by using the 2−ΔΔCt method. The relative expression of the specific gene to the internal control was obtained and then expressed as percentage of the control value in the Figures. All real-time PCR procedures including the design of primers, validation of PCR environment and quantification methods were performed according to the MIQE guideline.23
Western blot analysis
Western blot analyses of liver tissue extracts were performed as previously described.24 The ratio of the optical density of the protein product to the internal control was obtained and was normalized as a percentage of the control value in the Figures.
Enzyme-linked immunosorbent assay measurement
To correlate the mRNA expression with protein expression of selected target genes in the liver, enzyme-linked immunosorbent assay measurements of tumor necrosis factor-α, interleukin-1β, monocyte chemoattractant protein-1 and transforming growth factor-β1 were performed by using corresponding enzyme-linked immunosorbent assay development kits from PeproTech (PeproTech Inc., Rocky Hill, NJ, USA) according to the user instructions.
Determination of DNA-binding activity of nuclear factor-κB and activator protein-1
Nuclear factor-κB (NF-κB) and activator protein-1 (AP-1) are the major transcription factors in the regulation of inflammation and oxidative stress. The DNA-binding activity of these factors was performed by electrophoretic mobility shift assay using the Gel Shift Assay Systems from Promega (Madison, WI, USA) as previously described.24
Statistical analysis
Data from each group were expressed as means±s.e.m. Statistical comparison between groups was done using the Kruskal–Wallis test followed by Dunn’s post hoc test to detect differences in all groups. A P-value <0.05 was considered to be statistically significant (Prism 5.0; Graphpad Software, Inc., San Diego, CA, USA).
Results
Addition of LBP showed no effect on the rat body weight and food intake
At week 8, the mean body weight of high-fat diet-induced NASH rats was significantly higher than that of the control rats (330.2±7.0 versus 297.0±5.1 g). Addition of LBP slightly reduced the mean body weight of NASH rats, although the change was not statistically significant (324.5±5.7 versus 330.2±7.0 g). There was no difference in high-fat diet intake between NASH rats and NASH+LBP-co-treated rats (89.7±2.2 versus 88.1±1.5 ml per day) (Table 1). Wet liver weight results also showed that NASH rats had heavier liver than control rats. Administration of LBP significantly reduced the liver weight of NASH rats without influencing that of control rats (Table 1).
LBP ameliorated NASH-induced liver injury, fat deposition and collagen formation
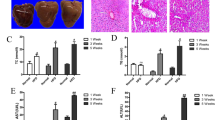
In high-fat diet-induced NASH rat, steatohepatitis caused a large number of fatty droplet accumulation and foci of inflammatory cell infiltration throughout the liver, as demonstrated by hematoxylin and eosin staining (Figure 1a). With the LBP co-treatment, both fat deposition and inflammation within the liver were significantly reduced (Figure 1d). LBP treatment also reduced the collagen formation around the centrolobular veins in the liver (Figures 1b and c). Serum ALT level was increased in NASH rats, but decreased by the co-treatment with LBP (Figure 1e). LBP treatment did not affect liver histology, fat deposition, serum ALT level and collagen formation of normal rats (Figures 1a–e).
Administration of LBP improved liver functions injured by NASH development. (a) Hematoxylin and eosin staining shows that high-fat diet-fed rats exhibit fat deposition and inflammatory foci in the liver. Administration of LBP reduced the injury without influencing healthy rat liver. Ctrl, control. (b) Sirius red staining shows the collagen formation in the NASH rat liver, which is significantly attenuated by LBP treatment. (c) Quantification of collagen formation, (d) NAFLD activity score and (e) serum ALT levels also indicate the improvement of liver function by LBP treatment. Data from each group were expressed as means±s.e.m. (n=8). Statistical comparison between groups was done using the Kruskal–Wallis test followed by Dunn’s post hoc test to detect differences between all groups. A P-value <0.05 was considered to be statistically significant with different letter labels. C, control; L, vehicle-LBP; N, NASH; N+L, NASH+LBP. Magnification: × 200. Bar: 20 μm.
Hepatic lipid metabolism was re-balanced by the administration with LBP
Lipogenic genes (sterol regulatory-element-binding protein-1c and peroxisome proliferator-activated receptor gamma 2) were upregulated, whereas lipolysis genes (adipose triglyceride lipase and adiponectin) were downregulated in high-fat diet fed NASH rats, which suggested a dysregulation of lipid metabolism in these rats (Figures 2a–d). As a result, serum FFA level was elevated in NASH rats (Figure 2e). Addition of 1 mg kg−1 LBP along with high-fat diet counteracted the NASH-induced effects on lipid metabolic genes and serum FFA level, without influencing their basal levels (Figures 2a–e).
LBP treatment re-balanced lipid metabolism in the liver. Real-time PCR results of (a,b) Lipogenic genes (sterol regulatory-element-binding protein-1c (SREBP1c) and peroxisome proliferator-activated receptor gamma 2 (PPARγ2)) and (c,d) lipolysis genes (adipose triglyceride lipase (ATGL) and adiponectin) exhibit accelerated lipid accumulation trends in the liver of NASH rats. LBP treatment has no significant impact on the healthy rat liver. (e) Serum level of FFAs further proves the anti-hyperlipidemic effects of LBP. Data from each group were expressed as means±s.e.m. (n=8). Statistical comparison between groups was done using the Kruskal–Wallis test followed by Dunn’s post hoc test to detect differences between all groups. A P-value <0.05 was considered to be statistically significant with different letter labels. C, control; L, vehicle-LBP; N, NASH; N+L, NASH+LBP.
LBP administration inhibited hepatic fibrosis through the TGF-β/SMAD pathway
During the development of NASH, the mRNA expression levels of TGF-β1, α-SMA and PC-1 and protein level of TGF-β1 were significantly upregulated in the liver, indicating an active status of hepatic fibrosis (Figures 3a–c). In line with the Sirius red staining results, daily administration of 1 mg kg−1 reduced the number of activated hepatic stellate cells (HSCs), which was significantly higher in the NASH group (Supplementary Figure S1). To further study the role of the TGF-β/SMAD pathway in fibrotic amelioration, the activity of both SMAD2 and SMAD4 was measured. The phosphorylation forms of SMAD2 and SMAD4 were induced in the NASH group but inhibited by LBP administration. Vehicle-LBP treatment did not influence the basal levels of the profibrogenic factors but slightly altered the activity of SMAD2 and SMAD4 (Figures 3d and e).
LBP treatment ameliorated fibrosis induced by NASH development. Expressional changes of (a) TGF-β1 mRNA and protein, (b) α-SMA mRNA and (c) PC-1 mRNA exhibit increased hepatic fibrosis in the liver of high-fat diet-fed rats, which is attenuated by LBP treatment. Western blot of phosphorylated and total forms of (d) SMAD2 and (e) SMAD4 indicate the contribution of the TGF-β/SMAD pathway in the anti-fibrosis effects of LBP. Data from each group were expressed as means±s.e.m. (n=8). Statistical comparison between groups was done using the Kruskal–Wallis test followed by Dunn’s post hoc test to detect differences between all groups. A P-value <0.05 was considered to be statistically significant with different letter labels. C, control; L, vehicle-LBP; N, NASH; N+L, NASH+LBP.
Antioxidant effects of LBP treatment on NASH-induced hepatic oxidative injury
To investigate the antioxidant properties of LBP treatment during the development of NASH, the formation of lipid peroxidation product—MDA and tyrosine nitration product—nitrotyrosine was measured in each group of rat. NASH development enhanced the formation of both MDA and nitrotyrosine in the liver, which was abolished by the addition of LBP (Figures 4a and b). Furthermore, the mRNA expression of antioxidant enzymes—catalase and glutathione peroxidase—was suppressed in the NASH group, when compared with that of control group. LBP co-treatment restored the level of these two enzymes as one of its antioxidant functions (Figures 4c and d). As a key enzyme mediating the production of reactive oxygen species in the liver, the protein expression level of CYP2E1 in NASH rats was upregulated to approximately 3.3-fold of the control level. LBP co-treatment also abolished such elevations without affecting its basal expression (Figure 4e).
LBP treatment reduced oxidative stress induced by NASH development. Expressional changes of (a) MDA formation, (b) nitrotyrosine formation, (c) catalase (CAT) mRNA, (d) glutathione peroxidase (GPx) mRNA and (e) CYP2E1 protein indicate an increased oxidative stress in the liver of high-fat diet-fed rats, which is attenuated by LBP treatment. Data from each group were expressed as means±s.e.m. (n=8). Statistical comparison between groups was done using the Kruskal–Wallis test followed by Dunn’s post hoc test to detect differences between all groups. A P-value <0.05 was considered to be statistically significant with different letter labels. C, control; L, vehicle-LBP; N, NASH; N+L, NASH+LBP.
Effects of LBP treatment on hepatic inflammation and chemoattraction
The concentrations of typical pro-inflammatory cytokines (tumor necrosis factor-α and interleukin-1β) and enzymes (iNOS and COX-2) were higher in the NASH rats than in the control rats, at both transcriptional and translational levels. After the daily co-treatment with LBP throughout the induction of NASH, the elevated expressions of these cytokines and enzymes were either abolished or significantly reduced (Figures 5a–f). The expressional change of inflammation inhibitor SOCS-3 also exhibited similar trends, at both mRNA and protein levels, showing a positively correlated inhibitory mechanism with the induction of hepatic inflammation (Figures 5g and h). Consistent with the changes of inflammatory mediators, the concentrations of typical chemokines also showed peak responses in NASH rats and attenuated levels in NASH+LBP rats, indicating a reduced chemoattraction in the liver (Supplementary Figure S2).
Addition of LBP alleviated hepatic inflammatory responses induced by NASH. Expressional changes of (a) tumor necrosis factor-α mRNA, (b) tumor necrosis factor-α protein, (c) interleukin-1β mRNA, (d) interleukin-1β protein, (e) iNOS mRNA, (f) COX-2 mRNA, (g) SOCS-3 mRNA and (h) SOCS-3 protein show that high-fat diet feeding in rats induces obvious inflammatory responses in the liver. Administration of LBP significantly attenuated such responses with minimal influence on the healthy rats. Data from each group were expressed as means±s.e.m. (n=8). Statistical comparison between groups was done using the Kruskal–Wallis test followed by Dunn’s post hoc test to detect differences between all groups. A P-value <0.05 was considered to be statistically significant with different letter labels. C, control; L, vehicle-LBP; N, NASH; N+L, NASH+LBP.
LBP attenuated hepatic apoptosis through the p53-dependent intrinsic and extrinsic pathways
To study the effects of LBP on NASH-induced hepatic apoptosis, we first measured the activity of terminal deoxynucleotidyl transferase (TdT), an enzyme that recognized the presence of nicks in the DNAs using TUNEL assay. By staining TdT with Fast Red reagent, the positive signal intensity was significantly higher in the NASH group than in the other three groups. Interestingly, both vehicle-LBP and NASH+LBP groups showed slightly higher signals of TdT than the control group, indicating that a slight degree of apoptosis had been induced in the healthy liver by LBP treatment (Figure 6a). To further characterize the signaling pathways that led to hepatic apoptosis, protein concentrations of key mediators in both the intrinsic and extrinsic apoptotic pathways had been quantified. In line with the TUNEL results, the concentrations of cleaved caspase-3 and phosphorylated p53 were highest in the NASH group and were slightly higher in the vehicle-LBP and NASH+LBP groups when compared with the control group. Three key members of the intrinsic pathway, cytochrome-c, Bcl-2 and Bax, exhibited significantly elevated protein concentrations in the NASH group and the control, showing comparable level to the vehicle-LBP and NASH+LBP groups. Key members for the extrinsic apoptotic pathway (Fas-associated death domain, Fas and cleaved caspase-8) revealed similar trends and results (Figures 6b and c).
LBP administration reduced hepatic apoptosis in NASH rats through the intrinsic and extrinsic pathways. (a) TUNEL results show that an increased TdT staining signal intensity in high-fat diet-fed rat livers. The apoptosis trend is attenuated by LBP treatment. Western blot results of key members in the (b) intrinsic apoptotic pathway and (c) extrinsic apoptotic pathway indicate that the anti-apoptotic effects of LBP are through both the pathways. Data from each group were expressed as means±s.e.m. (n=4–5). Statistical comparison between groups was done using the Kruskal–Wallis test followed by Dunn’s post hoc test to detect differences between all groups. A P-value <0.05 was considered to be statistically significant with different letter labels. C, control; L, vehicle-LBP; N, NASH; N+L, NASH+LBP. Bar: 20 μm.
LBP has hepatoprotective roles through modulating the kinase-dependent pathway and transcription factors
To further study the pathways linking upstream lipid dysfunction (‘first hit’) and downstream oxidative stress, inflammation and apoptosis (‘multi-hit’), several kinase-dependent pathways were characterized in different groups. In NASH rats, the hepatic activities of PI3K/Akt, LKB1/AMPK and MEK/ERK were inhibited, whereas the activities of FoxO1 and JNK/c-Jun were induced. Addition of LBP reversed the changes in the PI3K/Akt/FoxO1, LKB1/AMPK and JNK/c-Jun pathways but not in the MEK/ERK pathway (Figures 7a–c). NASH rats also showed increase activities of phosphorylated IκBα, NF-κB and AP-1, which were probably responsible for the occurrence of oxidative stress, inflammation and apoptosis in the liver. LBP counteracted such effects (Figure 7d). Supershift assay of NF-κB and AP-1 confirmed the specificity of gel-shift assay (data not shown).
LBP treatment ameliorated NASH-induced hepatic injury through the kinase- and transcription factor-related pathways. Western blot results of the (a) PI3K/Akt/FoxO1, (b) LKB1/AMPK, (c) MEK/ERK and JNK/c-Jun pathways show the involvements of these pathways in NASH development and LBP amelioration. (d) The results of IκBα and electrophoretic mobility shift assay results of NF-κB/AP-1 in different groups of rats show that the NASH development is accompanied by the activation of NF-κB and AP-1. Treatment with LBP reduces such induction. Data from each group were expressed as means±s.e.m. (n=4–5). Statistical comparison between groups was done using the Kruskal–Wallis test followed by Dunn’s post hoc test to detect differences between all groups. A P-value <0.05 was considered to be statistically significant with different letter labels. C, control; L, vehicle-LBP; N, NASH; N+L, NASH+LBP.
Discussion
To date, the main therapeutic strategies for NAFLD/NASH are weight control, abstinence from fatty food and maintenance of moderate intensity of exercise. Although several pharmaceutical therapies have been tested, none of them is accepted as a gold standard therapy.25 Because of their low toxicity and wide availability, several derivatives from natural herbs were used to control the pathological progression of NASH in animal studies, including aged garlic,24 coffee7 and green tea.26 In this study, we demonstrated that the polysaccharides part of Wolfberry ameliorated most typical NASH features in a high-fat diet rat model, from histological changes to apoptosis, with minimal perturbation in healthy rats. Because the effective dose of LBP in animal model is only 1 mg kg−1, which corresponds to about 0.25 g of dried Wolfberry for a 60-kg person,27 it is convenient and realistic for the daily consumption of Wolfberry to prevent early and middle stage of fatty liver disease.
The most direct evidence for the hepatoprotective property of LBP was the improvement of rat liver function. High-fat diet-fed rats showed typical NASH histology, such as intrahepatocyte lipid droplets, widespread inflammatory infiltration, perivenular fibrosis and increased serum ALT level (general index for hepatic injury/necrosis). Oral administration of LBP not only retarded the progression of NASH but also reversed the pathological changes. The histological and biochemical improvements from LBP were achieved by a sum of molecular events at different levels.
As the ‘first hit’ of NASH pathogenesis, dysregulated lipid metabolism was re-balanced by the co-treatment of LBP, leading to a reduction of lipid deposition in the liver. At the molecular level, LBP downregulated the intrahepatic expression of lipogenic genes and restored the level of lipolysis genes, contributing to accelerated lipid consumption rate (for example, β-oxidation) in the liver and reduced circulating level of FFAs (Figure 2). Because FFAs directly trigger the formation of oxidative stress and induce inflammation in the liver, the reduction of FFA levels by LBP partially alleviated hepatic reactive oxygen species formation and inflammatory infiltration.28 LBP treatment also restored the endogenous level of antioxidant enzymes, such as catalase and glutathione peroxidase, which further reduced the intracellular oxidative stress during the development of NASH. As a direct consequence, the increased hepatic apoptosis ratio in NASH rats, which was closely related to intracellular oxidative stress and inflammation, was significantly attenuated by LBP treatment, through the p53-dependent intrinsic and extrinsic apoptotic pathways. The activities of transcription factors NF-κB and AP-1, the master regulators of inflammation and apoptosis,29 were markedly higher in the NASH group than in the control, vehicle-LBP and NASH+LBP groups. Inhibition of NF-κB and AP-1 may partly explain the mechanisms for the antioxidant, anti-inflammatory and anti-apoptotic properties of LBP.
Under stressful conditions such as energy deprivation, the LKB1/AMPK pathway will respond to the stress by inhibiting the downstream apoptotic pathway through the AMPK-p53 axis.30 Consistent with increased hepatic apoptosis, the activities of both LKB1 and AMPK were suppressed in the NASH group (Figure 7b). Restoration of the LKB1/AMPK pathway by LBP co-treatment contributed to the improvement of hepatic functions.
A recent study demonstrated that during the pathogenesis of NASH, inhibition of the PI3K/Akt pathway and activation of transcription factor FoxO1 were crucial for the activation of HSCs, leading to the formation of ECM in the injured liver sites.31 Consistently, in the current study, NASH rats showed higher number of activated HSCs in the liver, as exhibited by synaptophysin staining (Supplementary Figure S1). Moreover, the phosphorylation form of PI3K/Akt was inhibited, whereas FoxO1 was promoted, which further supported the hypothesis that the anti-fibrogenic effect of LBP was partially through reduced activity of HSCs. As another important signaling contributor of fibrosis, the TGF-β/SMAD pathway was also induced by NASH development but attenuated by the administration of LBP, providing a different inhibitory mechanism of fibrosis.32, 33
The JNK/c-Jun pathway has an important role in FFA-induced insulin resistance and downstream pathological events, including inflammation and apoptosis.34, 35 In this study, high-fat diet feeding drastically increased the activities of both JNK and c-Jun, indicating their role in NASH development. LBP co-treatment effectively reduced the phosphorylations of these kinases to the control levels (Figure 7c). Unlike JNK/c-Jun, the MEK/ERK pathway, which beneficially accounts for cellular proliferation and oxidative stress formation after injury, is inhibited in NASH animals.36, 37 Consistent with these findings, high-fat diet-fed rats showed decreased MEK/ERK activities, indicating a suppressed proliferation status in the liver. However, LBP treatment further reduced instead of restoring the activities of MEK/ERK. We speculate that it may be related to the enhancement of autophagy/lipophagy in the liver after LBP treatment (data not shown).
In conclusion, consumption of LBP in a rat NASH model (1) improved liver function; (2) re-balanced lipid metabolism; (3) attenuated inflammation, oxidative stress and apoptosis through modulation of the kinase- and transcription factor-related pathways; and (4) reduced hepatic fibrosis via inhibition of HSC activity and the TGF-β/SMAD pathway. Considering its low effective dose, wide availability, and obvious improvement in NASH pathological features and minimal hepatic toxicity, LBP is a promising food supplement for the daily consumption in the prevention of NASH. Similar to other traditional Chinese medicinal herbal extracts, LBP is a mixture of several kinds of glycosidic monomers, including glucose, arabinose, galactose, mannose, xylose, rhamnose and β-carotene. The beneficial properties of LBP on the brain, neuron and liver probably rely on the intra-reactions or synergistic effects of the different monomers. Further studies by using specific monomer of these sugars in animal study and clinical trial are necessary.
References
Adams LA, Angulo P . Treatment of non-alcoholic fatty liver disease. Postgrad Med J 2001; 82: 315–322.
Williams CD, Stengel J, Asike MI, Torres DM, Shaw J, Contreras M et al. Prevalence of nonalcoholic fatty liver disease and nonalcoholic steatohepatitis among a largely middle-aged population utilizing ultrasound and liver biopsy: a prospective study. Gastroenterology 2011; 140: 124–131.
Farrell GC . The liver and the waistline: Fifty years of growth. J Gastroenterol Hepatol 2009; 24 (Suppl 3): S105–S118.
Youssef W, McCullough AJ . Diabetes mellitus, obesity, and hepatic steatosis. Semin Gastrointest Dis 2002; 13: 17–30.
Clark JM, Diehl AM . Nonalcoholic fatty liver disease: an underrecognized cause of cryptogenic cirrhosis. JAMA 2003; 289: 3000–3004.
Polyzos SA, Kountouras J, Zavos C 2009 Nonalcoholic fatty liver disease: the pathogenetic roles of insulin resistance and adipocytokines. Curr Mol Med 2009; 9: 299–314.
Vitaglione P, Morisco F, Mazzone G, Amoruso DC, Ribecco MT, Romano A et al. Coffee reduces liver damage in a rat model of steatohepatitis: the underlying mechanisms and the role of polyphenols and melanoidins. Hepatology 2010; 52: 1652–1661.
Vitaglione P, Morisco F, Caporaso N, Fogliano V . Dietary antioxidant compounds and liver health. Crit Rev Food Sci Nutr 2004; 44: 575–586.
Chang RC, So KF . Use of anti-aging herbal medicine, Lycium barbarum, against aging-associated diseases. What do we know so far? Cell Mol Neurobiol 2008; 28: 643–652.
Amagase H, Sun B, Borek C . Lycium barbarum (goji) juice improves in vivo antioxidant biomarkers in serum of healthy adults. Nutr Res 2009; 29: 19–25.
Xin YF, Wan LL, Peng JL, Guo C . Alleviation of the acute doxorubicin-induced cardiotoxicity by Lycium barbarum polysaccharides through the suppression of oxidative stress. Food Chem Toxicol 2011; 49: 259–264.
Wu HT, He XJ, Hong YK, Ma T, Xu YP, Li HH . Chemical characterization of Lycium barbarum polysaccharides and its inhibition against liver oxidative injury of high-fat mice. Int J Biol Macromol 2010; 46: 540–543.
Niu AJ, Wu JM, Yu DH, Wang R . Protective effect of Lycium barbarum polysaccharides on oxidative damage in skeletal muscle of exhaustive exercise rats. Int J Biol Macromol 2008; 42: 447–449.
Li XM . Protective effect of Lycium barbarum polysaccharides on streptozotocin-induced oxidative stress in rats. Int J Biol Macromol 2007; 40: 461–465.
Zhang M, Chen H, Huang J, Li Z, Zhu C, Zhang S . Effect of lycium barbarum polysaccharide on human hepatoma QGY7703 cells: inhibition of proliferation and induction of apoptosis. Life Sci 2005; 76: 2115–2124.
Ho YS, Yu MS, Yang XF, So KF, Yuen WH, Chang RC . Neuroprotective effects of polysaccharides from wolfberry, the fruits of Lycium barbarum, against homocysteine-induced toxicity in rat cortical neurons. J Alzheimers Dis 2010; 19: 813–827.
Li SY, Yang D, Yeung CM, Yu WY, Chang RC, So KF et al. Lycium barbarum polysaccharides reduce neuronal damage, blood-retinal barrier disruption and oxidative stress in retinal ischemia/reperfusion injury. PLoS One 2011; 6: e16380.
Chiu K, Chan HC, Yeung SC, Yuen WH, Zee SY, Chang RC et al. Erratum: modulation of microglia by wolfberry on the survival of retinal ganglion cells in a rat ocular hypertension model. J Ocul Biol Dis Infor 2009; 2: 127–136.
Cheng D, Kong H . The effect of Lycium barbarum polysaccharide on alcohol-induced oxidative stress in rats. Molecules 2011; 16: 2542–2550.
Tipoe GL, Ho CT, Liong EC, Leung TM, Lau TY, Fung ML et al. Voluntary oral feeding of rats not requiring a very high fat diet is a clinically relevant animal model of non-alcoholic fatty liver disease (NAFLD). Histol Histopathol 2009; 24: 1161–1169.
Tipoe GL, Liong EC, Leung TM, Nanji AA . A voluntary oral-feeding rat model for pathological alcoholic liver injury. Methods Mol Biol 2008; 447: 11–31.
Kleiner DE, Brunt EM, Van Natta M, Behling C, Contos MJ, Cummings OW et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology 2005; 41: 1313–1321.
Bustin SA, Benes V, Garson JA, Hellemans J, Huggett J, Kubista M et al. The MIQE guidelines: minimum information for publication of quantitative real-time PCR experiments. Clin Chem 2009; 55: 611–622.
Xiao J, Ching YP, Liong EC, Nanji AA, Fung ML, Tipoe GL . Garlic-derived S-allylmercaptocysteine is a hepato-protective agent in non-alcoholic fatty liver disease in vivo animal model. Eur J Nutr 2013; 52: 179–191.
Gossard AA, Lindor KD . Current therapies for nonalcoholic fatty liver disease. Drugs Today 2011; 47: 915–922.
Masterjohn C, Bruno RS . Therapeutic potential of green tea in nonalcoholic fatty liver disease. Nutr Rev 2012; 70: 41–56.
Yin G, Dang Y . Optimization of extraction technology of the Lycium barbarum polysaccharides by Box–Behnken statistical design. Carbohydr Polym 2008; 74: 603–610.
Cusi K . Role of insulin resistance and lipotoxicity in non-alcoholic steatohepatitis. Clin Liver Dis 2009; 13: 545–563.
Zima T, Kalousova M . Oxidative stress and signal transduction pathways in alcoholic liver disease. Alcohol Clin Exp Res 2005; 29 (Suppl 11): 110S–115S.
Filomeni G, Cardaci S, Da Costa Ferreira AM, Rotilio G, Ciriolo MR . Metabolic oxidative stress elicited by the copper (II) complex [Cu(isaepy)2] triggers apoptosis in SH-SY5Y cells through the induction of the AMP-activated protein kinase/p38MAPK/p53 signalling axis: evidence for a combined use with 3-bromopyruvate in neuroblastoma treatment. Biochem J 2011; 437: 443–453.
Adachi M, Osawa Y, Uchinami H, Kitamura T, Accili D, Brenner DA . The forkhead transcription factor FoxO1 regulates proliferation and transdifferentiation of hepatic stellate cells. Gastroenterology 2007; 132: 1434–1446.
Biernacka A, Dobaczewski M, Frangogiannis NG . TGF-beta signaling in fibrosis. Growth Factors 2011; 29: 196–202.
Tang LX, He RH, Yang G, Tan JJ, Zhou L, Meng XM et al. Asiatic acid inhibits liver fibrosis by blocking TGF-beta/Smad signaling in vivo and in vitro. PLoS One 2012; 7: e31350.
Hirosumi J, Tuncman G, Chang L, Görgün CZ, Uysal KT, Maeda K et al. A central role for JNK in obesity and insulin resistance. Nature 2002; 420: 333–336.
Schattenberg JM, Singh R, Wang Y, Lefkowitch JH, Rigoli RM, Scherer PE et al. JNK1 but not JNK2 promotes the development of steatohepatitis in mice. Hepatology 2006; 43: 163–172.
Czaja MJ, Liu H, Wang Y . Oxidant-induced hepatocyte injury from menadione is regulated by ERK and AP-1 signaling. Hepatology 2003; 37: 1405–1413.
Mebratu Y, Tesfaigzi Y . How ERK1/2 activation controls cell proliferation and cell death: is subcellular localization the answer? Cell Cycle 2009; 8: 1168–1175.
Acknowledgements
This work was supported by Small Project Funding, University Research Committee, HKU, General Research Fund, University Grant Council, Hong Kong SAR and the Azalea (1972) Endowment Fund to KFS and RCCC.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Nutrition & Diabetes website
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Xiao, J., Liong, E., Ching, Y. et al. Lycium barbarum polysaccharides protect rat liver from non-alcoholic steatohepatitis-induced injury. Nutr & Diabetes 3, e81 (2013). https://doi.org/10.1038/nutd.2013.22
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nutd.2013.22
Keywords
This article is cited by
-
Role of Oxidative Stress in the Occurrence and Development of Cognitive Dysfunction in Patients with Obstructive Sleep Apnea Syndrome
Molecular Neurobiology (2023)
-
Possible antioxidant effect of Lycium barbarum polysaccharides on hepatic cadmium-induced oxidative stress in rats
Environmental Science and Pollution Research (2017)
-
Lycium barbarum polysaccharide attenuates high-fat diet-induced hepatic steatosis by up-regulating SIRT1 expression and deacetylase activity
Scientific Reports (2016)
-
Bee’s honey attenuates non-alcoholic steatohepatitis-induced hepatic injury through the regulation of thioredoxin-interacting protein–NLRP3 inflammasome pathway
European Journal of Nutrition (2016)
-
Lycium barbarum polysaccharides therapeutically improve hepatic functions in non-alcoholic steatohepatitis rats and cellular steatosis model
Scientific Reports (2014)