Abstract
Objectives:
The objectives of the study were to test for spatial clustering of obesity in a cohort of young adults in the Philippines, to estimate the locations of any clusters, and to relate these to neighborhood-level urbanicity and individual-level socioeconomic status (SES).
Subjects:
Data are from a birth cohort of young adult (mean age 22 years) Filipino males (n=988) and females (n=820) enrolled in the Cebu Longitudinal Health and Nutrition Survey.
Methods:
We used the Kulldorff spatial scan statistic to detect clusters associated with unusually low or high prevalences of overweight or obesity (defined using body mass index, waist circumference and body fat percentage). Cluster locations were compared to neighborhood-level urbanicity, which was measured with a previously validated scale. Individual-level SES was adjusted for using a principal components analysis of household assets.
Results:
High-prevalence clusters were typically centered in urban areas, but often extended into peri-urban and even rural areas. There were also differences in clustering by both sex and the measure of obesity used. Evidence of clustering in males, but not females, was much weaker after adjustment for SES.
Similar content being viewed by others
Introduction
Urbanization, modernization and globalization have radically altered human environments, resulting in sweeping changes to the way we work, play and eat.1, 2 The most dramatic changes are taking place in the developing world, where the pace of urbanization has been especially rapid.3 In the wake of these environmental changes, obesity has emerged as a global public health problem,4, 5, 6 even in contexts where underweight is still prevalent.7
While it is broadly accepted that physical and social environments can promote obesogenic behaviors and limit healthy options,8, 9, 10, 11, 12, 13, 14, 15 more research on how they do so is needed to inform intervention efforts.15, 16 Responding to this need, researchers have spent the last two decades blending theoretical and methodological perspectives from various disciplines to identify environmental determinants of obesity (for example,17, 18). However, this growing area of research has almost exclusively focused on high-income countries, while related research in lower-income countries mostly consists of comparisons of urban vs rural obesity prevalences.
With this gap in mind, we employed the Kulldorff spatial scan statistic19 to detect clusters with unusually high or low prevalences of obesity among young adults living in a large metropolitan area in the Philippines. We then compared the locations of these spatial clusters with the urbanicity of the area, using a continuous scale measure of urbanicity that captures environmental heterogeneity between and within ‘urban’ and ‘rural’ areas.20 We also evaluated the degree to which any clusters were explained by the spatial distribution of individual-level socioeconomic status (SES).
Materials and Methods
Study site
Metro Cebu (pop 1.9 million), on the east coast of Cebu Island in the central Philippines, is composed of three cities and seven municipalities. It is further divided into 270 administratively defined neighborhoods called barangays (average area 2.65 km2) comprising a 720 km2 contiguous area. The study area includes densely populated urban centers, less dense peri-urban areas, rural towns and more isolated mountain and island areas.
Study design and sample
Data are from the Cebu Longitudinal Health and Nutrition Survey (CLHNS), a community based, one-year birth cohort.21 A single-stage cluster sampling procedure was used to randomly select 33 barangays. Pregnant women who gave birth between May 1, 1983 and April 30, 1984 were recruited from these barangays into the study. More than 95% of identified women agreed to participate. A baseline interview was conducted among 3327 women during their sixth or seventh month of pregnancy. Another survey took place immediately after birth. There were 3080 non-twin live births which make-up the CLHNS birth cohort. Subsequent surveys were conducted bi-monthly to age two years, then in 1991, 1994, 1998, 2002 and 2005.
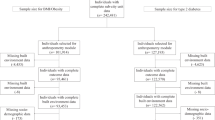
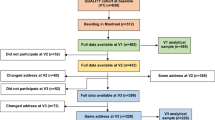
We used birth cohort data on barangay of residence and multiple adiposity measures collected in 2005 when the study participants were young adults (20–22 years of age). Women pregnant in 2005 were excluded (n=73). Anyone with missing data for barangay residence or any outcome measures were also dropped (n=7), resulting in a sample of 988 males and 820 females. By 2005, participants were living in 161 different barangays, though 77% of males and 76% of females were still located in the original 33 sample barangays (Supplementary Figure 1). Intra-barangay sample sizes were highly variable, ranging from 5 to 163 participants (mean: 43.8, s.d. 35.8) in the original 33 barangays; and sparse in the additional barangays, ranging from 1 to 15 (mean: 3.4 s.d. 2.8).
Barangay-level data were collected for each round of the survey. The surveys included information on physical characteristics, infrastructure and utilities, social services, community organizations, industrial and commercial establishments, labor markets and wage rates. Data were obtained from barangay officials or other key informants. Population sizes were taken from the year 2000 Filipino census.
Measures
Neighborhoods
Barangay of residence in 2005 was used to define participant neighborhoods. The assumptions implied are constant barangay-level effects across respondents in a given barangay, and that the barangay is a reasonable approximation of a person’s ‘activity space,’ defined as the set of locations a person encounters in the course of their daily activities.22, 23 These assumptions are common in health geography. Barangays have their own elected officials and budgets, community centers and so on, and Cebuanos can easily identify their barangay. Thus, barangay of residence is a better measure of neighborhood, one that encompasses social factors and not just space, than the administratively defined neighborhoods used in other contexts.
Urbanicity
While most research uses the urban–rural dichotomy to describe urbanicity, our research uses a continuous measure that captures a range of variation in urbanicity across a single dimension. The starting point for this measure is a previously designed urbanicity scale. Its description, rationale, and validation are given in Dahly and Adair.20
Briefly, the scale is made up of seven components derived from data collected for the CLHNS barangay-level surveys. The components are population size; population density; communications (availability of mail, telephone, internet, cable TV and newspaper services); transportation (paved road density and public transportation services); markets (presence of gas stations, drug stores, grocery stores and the number of small commercial kiosks); educational facilities; and health services. Theoretically, the scale represents an underlying latent construct labeled urbanicity that is imperfectly reflected in each of these seven components.
Since publishing the details of the scale’s creation, we’ve modified it by making the urbanicity value for a given barangay a function of its own score and the scores of surrounding barangays (for example, an urban barangay surrounded by other urban barangays will have a higher final score than an urban barangay with the same initial value that is bordered by more rural barangays). These values were created with the ESRI ArcMap inverse distance weighting interpolation tool, using the default settings. For more detail on inverse distance weighting, please see Waller and Gotway.24 A map of interpolated urbanicity values is given in Figure 1.
Urbanicity in Metro Cebu, 2005. To further validate that the urbanicity scale provides a valid description of the rural–urban gradient in Metro Cebu, we compared its spatial distribution to a Landsat 7 ETM+ image of the study area (http://landsat.gsfc.nasa.gov/), which is a false color composite that depicts vegetation as shades of red, while mixes of bare soil and impermeable land cover (buildings, roads and so on) appear green. We also compared our image with a SRTM elevation map (http://srtm.csi.cgiar.org/) because mountains constrain urban development to the northwest. The map depicts higher elevations as darker shades of blue, because mountains constrain urban development to the northwest.
Anthropometrics
We used three anthropometric measures to define overweight (OW) or obesity. They were body mass index (BMI), waist circumference (WC), and percent body fat (BF%). All anthropometrics were collected by trained field staff during in-home interviews using techniques described in Lohman et al.25 Weight was measured with calibrated portable scales to the nearest g. Height was measured with a folding stadiometer to the nearest tenth of a cm. BMI was calculated as measured weight (kg) divided by measured height (m) squared. BMI is the standard measure of adiposity for public health research26 because it is strongly correlated with both BF% and total fat mass,27 but it does not differentiate fat mass from lean mass. BMI was dichotomized as OW or obese based on respective cut points of ⩾23 kg m−2 and ⩾25 kg m−2, primarily based on evidence that lower cut points in Asian populations may be more appropriate for describing health risks (for example, Misra28 and Gallagher et al.29), and better reflect an important ‘public health action point’.30
WC was measured to the nearest mm, at the midpoint between the bottom of the ribs and the top of the iliac crest, using a measuring tape. WC is a measure of central obesity, which is thought to be an important driver for a number of important metabolic disorders31 compared with other patterns of fat distribution. High WC (HWC) was defined as WC>85 cm in males or >80 cm in females.32
BF% was calculated as described by Durnin and Wormersley33 using the sum of three skin folds (triceps, subscapular and suprailiac), measured to the nearest mm using Lange calipers. It is a more valid measure of adiposity than BMI, though it is typically measured less reliably. High BF% (HBF) was defined as BF% ⩾25 in the males, or ⩾38 in the females.34
Socioeconomic status
To capture SES, we used principal components analysis to evaluate a set of household assets measures (for example television, land and so on), a method commonly used with Demographic and Health Survey data. The measure used here is the first principal component (eigenvalue 4.2) from this analysis, and has been used in previous analyses.35, 36
Analytical methods
A spatial cluster can be defined as a contiguous geographic space for which the value of some characteristic is unusual when compared with the space surrounding it. The characteristic we are interested in is the prevalence of OW or obesity in our sample. To detect clusters, we used the spatial scan statistic as implemented by the software SaTScan and employed the Bernoulli model19, 37 for binary outcomes.
We derived Cartesian coordinates (x,y) for the center-point of each barangay using ArcGIS. Individuals in the study were assigned the location of their respective barangay’s center-point, resulting in a set of point locations characterized by the number of ‘cases’ of each outcome and the total number of study participants at that location.
For each of these locations, SaTScan draws all possible contiguous scan windows, centered on that point, that contain ⩽50% of the total study population. For each of these windows, a prevalence (p) is calculated as the number of observed cases divided by the total population residing within the window. This is compared with the observed prevalence (q) for participants residing outside the given window, resulting in a prevalence ratio (PR=p/q). The null hypothesis tested for each window is Ho: p/q=1. In this analysis, we set out to detect clusters of higher and lower than expected prevalence, thus the alternate hypothesis is H1: p/q≠1.
The goal is to identify the window with a prevalence ratio that is the least likely to occur given H0. To do this, a likelihood is calculated for each window. For the Bernoulli model detecting both high and low-prevalence clusters, the likelihood function is:

where c is the number of cases in the window, C is the total number of cases in the sample, n is the number of observations in the window, and N is the total number observations in the sample.19 The likelihood function is maximized over all the windows, and the one with the maximum likelihood is identified as the cluster that is least likely to have occurred by chance.19 This cluster is the ‘primary cluster.’
To obtain a P-value, the same analysis is repeated on 999 random replications of the data generated under the null hypothesis, and the maximum likelihood from the real data is ranked (R) along with maximum likelihoods from each of these Monte Carlo simulations.19 The P-value of the least likely cluster is given by R/1000. For this analysis we have elected to report all primary clusters for which H0 can be rejected at P<0.15, and any secondary clusters with P<0.15 that don’t geographically overlap with the primary cluster. Highly unusual clusters, given H0, are indicated by P<0.05.
The shape of the scan window used to detect clusters can take on a variety of forms. We chose to use an elliptical scan window38 because the urban core of Metro Cebu is elongated, running roughly southwest to northeast (see Figure 1). By hypothesizing that adiposity clusters will geographically coincide with the most urban areas of Metro Cebu, we are, in effect, hypothesizing that the clusters will be elliptical in nature. The elliptical scan window has slightly higher power for long narrow clusters, and slightly lower power for circular or more compact clusters.39 We used a medium strength non-compactness penalty which favors less eccentric clusters.39 In practice, this penalty helps prevent the detection of very long, thin clusters that are artifacts driven by high prevalences at the two ends of the ellipse.
We then repeated our analysis, adjusting for individual-level SES. The goal was to evaluate the degree to which spatial clusters of adiposity are explained by the spatial distribution of SES among study participants. In a previous analysis using generalized estimating equations, we found strong positive associations between adiposity and multiple indicators of SES in the males, but not in the females.35 The adjustment for SES was made by stratifying the samples by sex-specific tertiles of SES and using the multiple data sets option in SaTScan. More detail on how this adjustment is calculated can be found in the SaTScan user’s guide.39
Clusters are displayed by outlining the barangays that make-up the cluster (in red for high-prevalence clusters and in blue for low-prevalence clusters), then combining that information with urbanicity maps of the study area using ArcGIS. Urbanicity maps were created using the continuous urbanicity scale, as well as the barangays’ urban–rural designations from the 2000 Philippines census.
Results
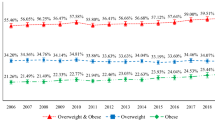
Table 1 summarizes the distribution of adiposity measures in our sample. The sample is lean overall, but characterized by wide variation in measures, indicative of a population suffering from a double burden of over- and under-nutrition (consistent with Pedro et al.40).
Among males (Table 2), there were high- and low-prevalence clusters detected for each outcome except HWC, for which there was only a high-prevalence cluster. Generally, the prevalence of a given outcome among males residing within a high-prevalence primary cluster was more than twice that of males living outside of the cluster. The high-prevalence clusters for OW and obese were highly unusual (P<0.05) given the null hypothesis of complete spatial randomness. Conversely, the high-prevalence clusters for HBF and HWC were not highly unusual (P=0.104 and 0.108, respectively). In every instance, these high-prevalence clusters were located in the urban core of Metro Cebu, with minor variations in the set of barangays contained within them (see Figure 2a). Low-prevalence clusters, where outcomes were virtually non-existent, occurred in the rural south or southwestern regions of Metro Cebu, though the low-prevalence cluster of HBF extended into some urban areas.
Like the males, a high-prevalence cluster was detected for all four outcome measures in females (Table 2), though the obese and HBF clusters were not highly unusual given the null hypothesis of complete spatial randomness (P=0.062 and 0.125, respectively). The prevalence of a given outcome among females living in the respective cluster was generally more than twice that of females living outside the cluster, but almost four times larger for the HWC cluster. Each of these high-prevalence clusters was located in the urban core of Metro Cebu (see Figure 2b). There were no low-prevalence clusters detected among the females.
To illustrate how informative the urban–rural dichotomy would be for describing cluster locations, we redisplayed the male clusters on a map of Metro Cebu barangays defined by the urban–rural dichotomy (Figure 3). For example, though the magnitude of the prevalence ratio comparing obesity in urban versus rural males (PR 1.71; 95% CI 1.05 to 2.79) is similar to that found in the high-prevalence obesity cluster (PR 2.33; 95% CI 1.56–3.47; top left, Figure 2a), if we only intervened in the urban barangays, we would be ignoring 18 rural barangays included in the obesity spatial cluster (a total population size of 96,472 according to the year 2000 Filipino census), and acting in 30 urban barangays not included in the spatial cluster (total population size 380,322). Furthermore, looking at the HBF clusters (bottom right, Figure 2a), intervening to reduce obesity in urban areas would target barangays that are in fact part of a low-prevalence cluster.
After adjustment for individual-level SES (Supplementary Table 1), there was no evidence of spatial clustering of obesity, HWC or HBF in the males. There was still strong evidence of a high-prevalence cluster of OW in the males, but no evidence for a low-prevalence cluster. Adjustment for SES did not appreciably impact the spatial clusters in the females.
Discussion
Motivated by the increasing prevalence of obesity in the Philippines,41, 42 and other lower-income countries,7 particularly in urban areas, we aimed to identify spatial clusters of obesity in Metropolitan Cebu. By identifying spatial clusters and relating them to the urbanicity of the study area, we hoped to facilitate further etiological research aimed at identifying environmental determinants of obesity in this study area. We also hoped to more directly inform public health practice by explicitly identifying areas where obesity is most common, and by evaluating how useful simple urban–rural classifications are for identifying these areas when spatial data are not available.
Cluster locations were consistent with the idea that urban areas are obesogenic. High-prevalence clusters were centered on the highly urban core of Metropolitan Cebu, and low-prevalence clusters were found in rural areas. However, high-prevalence clusters typically covered substantial proportions of the study area that included both urban and peri-urban areas. The observed scale of the clusters likely reflects the simple fact that barangay of residence is not a complete description of a person’s activity space. The lack of smaller clusters also suggests that there are not any environmental determinants of obesity that exert strong, highly localized influence.
Evidence of spatial clustering varied by sex and outcome measure. The most striking difference between the sexes was that evidence of clustering for HWC was very strong for females (P=0.010), but not for males (P=0.104). Furthermore, the female HWC cluster was characterized by a PR roughly twice that of the other high-prevalence clusters (PR ∼4 vs ∼2). These results are consistent with a previous analysis of the same sample in which we observed gender differences in intra-class correlations from multi-level models describing the proportion of variance in obesity and HWC described at the barangay level (males: 0.18 and 0.10, respectively; females: 0.05 and 0.18).35 These results raise the interesting possibility that central fat distribution and total adiposity each have unique environmental determinants that vary by gender.
High-prevalence clusters were not detected for all of the outcomes considered. In the males, there were clusters for both obesity and OW, but not HWC or HBF. We cannot rule out that these clusters are reflecting influences on both lean and fat mass. For females, a lack of clustering in HBF and obesity lead to similar reservations. While BF% is a more valid measure of adiposity than BMI, it is measured less reliably due to its reliance on skin folds, versus height and weight, which are measured much more accurately. Thus measurement error in BF% could have reduced our power to detect any such clusters. WC is also measured less reliably, though this did not prevent the detection of a high-prevalence cluster in the females.
We also cannot rule out that the existence of clusters are driven by compositional factors (that they disproportionately contain people more susceptible to obesity) rather than contextual causes. However, because the sample is a one-year birth cohort, confounding of the space-outcome relationship by age is not possible. Furthermore, the ethnic and cultural make-up of Cebu is fairly homogenous. Based on previous research on the socioeconomic determinants of obesity in this sample, we did adjust for a measure of household assets. We found that evidence for clustering in the males was much weaker after this adjustment, though there was no impact of the adjustment on the female results. This finding was consistent with a large body of evidence suggesting that SES is an important determinant of obesity in males but not females in lower-income contexts.43, 44, 45
In addition to gaining some etiological insight, understanding the spatial distribution of disease can also aid public health efforts by providing the best possible information on where to focus interventions. Unfortunately, the spatial data required to detect spatial clusters of obesity are often not available. In lower-income countries, this information is typically approximated by looking at obesity outcomes between areas defined as ‘urban’ or ‘rural.’ As obesity intervention efforts in developing countries increase, it seems likely they will rely on these urban–rural differences to target interventions.
Our results suggest that targeting obesity interventions in this manner should be done with caution. Though our study area is the second largest metropolitan area in the Philippines, there is a great deal of environmental heterogeneity in Metro Cebu and targeting interventions at the entire area could be inappropriate. Furthermore, targeting the administratively defined urban areas within Metro Cebu also seems problematic because this descriptor does not accurately describe where the highest prevalences of obesity are. This information is valuable because lower-income countries have fewer public health resources, but must contend with a greater variety of public health problems.
Strengths and limitations
For this analysis, we took an urban health perspective46 to clearly link our work to previous research in lower and middle income contexts that has focused on crude urban–rural comparisons of obesity prevalences (for example, Mendez et al.7). These studies have typically found that urbanites are more likely to be obese than their rural counterparts, though the degree of difference varies widely between studies (for example, Mendez et al.7). However, these studies often compare urban and rural areas that are located in completely different regions of a country; there are no consistently used definitions of urban and rural, and the use of the urban–rural dichotomy to describe environments likely obscures a great deal of environmental heterogeneity.20 To help overcome some of these limitations, we employed a previously developed continuous measure of urbanicity that better described the environmental heterogeneity in Metro Cebu.
While studies of the environmental determinants of obesity are becoming more common, most rely on multi-level models (for example, Rundle et al.47) that do not account for spatial dependencies at the higher level, or explicitly link outcomes to space (but rather to characteristics of space). This approach requires strong a priori hypotheses about which specific environmental characteristics you think are important, while our analysis was more exploratory. Given our goals, an explicitly spatial cluster analysis was more appropriate.
While there were many available cluster detection methods, the Kulldorff spatial scan statistic seemed ideal in that it both locates clusters and provides a statistical test of how unusual the clusters are given the null hypothesis of complete spatial randomness. Furthermore, the method accounts for multiple testing; it does not require a priori decisions regarding the scale of the clusters; the clusters are robust to the spatial distribution of cases and controls within them; it allows for covariate adjustment; and it is implemented with freely available software. Lastly, because clusters are based on the distribution of individual study participants, rather than barangay-level summary measures (for example, proportions), participants in sparsely populated barangays do not disproportionately contribute to the clusters. Additional methodological comparisons and references can be found in Kulldorff.39 Despite these strengths, we found few examples where the spatial scan statistic was used to identify obesity clusters (for example, Huang et al.48 and Edwards et al.49), and none that were relevant to the scale and context of our research.
This was the first survey in this cohort that we were able to assess adult obesity. Consequently, this analysis was limited by its cross-sectional nature. We were unable to evaluate the degree to which time spent in an urban area as an adult impacts obesity risk (such as Sobngwi et al.50). We tried to account for the possibility of residential selection by limiting our sample to individuals who still lived in the barangay they were born in. We found that this exclusion had no impact on our results (not reported). Another potential limitation of the study is that there are relatively few obese people in this sample of young adults. However, the mothers of this birth cohort underwent a remarkable sixfold increase in OW and obesity prevalence between 1983 and 2005.42 Space-time clustering of obesity in the cohort mothers will provide additional insights and help overcome these limitations.
Conclusions
Our analysis found evidence for spatial clusters of OW and obesity that varied by sex and outcome measure. Generally, high-prevalence clusters were centered on the urban core of Metropolitan Cebu, but extended into peri-urban areas. Low-prevalence clusters, where outcomes were virtually non-existent, were largely restricted to rural areas. The most striking result was the existence of a high-prevalence cluster of HWC in the females, characterized by a prevalence ratio of ∼4. This was contrasted by no evidence of clustering of HWC in the males. Sex differences were further highlighted by the result that adjustment for household assets explained spatial clustering of most outcomes among the males but not the females. Lastly, our results suggest that using simple urban–rural classifications to identify areas of greatest risk can possibly lead to substantial amounts of misclassification.
References
Popkin BM . The World is Fat: The Fads, Trends, Policies, and Products that are Fattening the Human Race. Avery: New York, NY, USA, 2008.
Swinburn BA, Sacks G, Hall KD, McPherson K, Finegood DT, Moodie ML et al. The global obesity pandemic: shaped by global drivers and local environments. Lancet 2011; 378: 804–814.
U.N. World Urbanization Prospects. The 2011 Revision. World Urbanization Prospects. United Nations Department of Economic and Social Affairs/Population Division: New York, NY, USA, 2011.
Popkin BM, Gordon-Larsen P . The nutrition transition: worldwide obesity dynamics and their determinants. Int J Obes Relat Metab Disord 2004; 28 (Suppl 3): S2–S9.
Popkin BM . Global nutrition dynamics: the world is shifting rapidly toward a diet linked with noncommunicable diseases. Am J Clin Nut 2006; 84: 289–298.
James WPT . WHO recognition of the global obesity epidemic. Int J Obes 2008; 32: S120–S126.
Mendez MA, Monteiro CA, Popkin BM . Overweight exceeds underweight among women in most developing countries. Am J Clin Nutr 2005; 81: 714–721.
Hill JO, Peters JC . Environmental contributions to the obesity epidemic. Science 1998; 280: 1371–1374.
Hill JO, Wyatt HR, Reed GW, Peters JC . Obesity and the environment: where do we go from here? Science 2003; 299: 853–855.
French SA, Story M, Jeffery RW . Environmental influences on eating and physical activity. Ann Rev Public Health 2001; 22: 309–335.
Booth KM, Pinkston MM, Poston WSC . Obesity and the built environment. J Am Diet Assoc 2005; 105: 110–117.
Lake A, Townshend T . Obesogenic environments: exploring the built and food environments. J R Soc Health 2006; 126: 262–267.
Macintyre S, Ellaway A, Cummins S . Place effects on health: how can we conceptualise, operationalise and measure them? Soc Sci Med 2002; 55: 125–139.
Entwisle B . Putting people into place. Demography 2007; 44: 687–703.
Giskes K, Van Lenthe F, Avendano-Pabon M, Brug J . A systematic review of environmental factors and obesogenic dietary intakes among adults: are we getting closer to understanding obesogenic environments? Obes Rev 2011; 12: e95–e106.
Huang TTK, Glass TA . Transforming research strategies for understanding and preventing obesity. JAMA 2008; 300: 1811–1813.
Feng J, Glass TA, Curriero FC, Stewart WF, Schwartz BS . The built environment and obesity: a systematic review of the epidemiologic evidence. Health & Place 2012; 16: 175–190.
Black JL, Macinko J . Neighborhoods and obesity. Nutr Rev 2008; 66: 2–20.
Kulldorff M . A spatial scan statistic. Communications in Statistics: Theory and Methods 1997; 26: 1481–1496.
Dahly DL, Adair LS . Quantifying the urban environment: A scale measure of urbanicity outperforms the urban-rural dichotomy. Social Science & Medicine 2007; 64: 1407–1419.
Adair LS, Popkin BM, Akin JS, Guilkey DK, Gultiano S, Borja J et al. Cohort profile: The Cebu Longitudinal Health and Nutrition Survey. Int J Epidemiol 2010; 40: 619–625.
Golledge RG, Stimpson RJ . Analytical Behavioural Geography. Croom Helm, Ltd.: London, UK, 1987.
Nemet GF, Bailey AJ . Distance and health care utilization among the rural elderly. Soc Sci Med 2000; 50: 1197–1208.
Waller LA, Gotway CA . Applied Spatial Statistics for Public Health Data. John Wiley & Sons: Hoboken, NJ, 2004.
Lohman T, Roche A, Martorell R . Anthropometric Standardization Reference Manual. Human Kinetics Books: Champaign, IL, USA, 1988.
Hall DMB, Cole TJ . What use is the BMI? Arch Dis Child 2006; 91: 283–286.
Hu FB . Obesity Epidemiology. Oxford University Press: New York, NY, USA, 2008.
Misra A . Revisions of cutoffs of body mass index to define overweight and obesity are needed for the Asian-ethnic groups. Int J Obes 2003; 27: 1294–1296.
Gallagher D, Heymsfield SB, Heo M, Jebb SA, Murgatroyd PR, Sakamoto Y . Healthy percentage body fat ranges: an approach for developing guidelines based on body mass index. Am J Clin Nutr 2000; 72: 694–701.
Barba C, Cavalli-Sforza T, Cutter J, Darnton-Hill I, Deurenberg P, Deurenberg-Yap M et al. Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet 2004; 363: 157–163.
Alberti K, Zimmet P, Shaw J . The metabolic syndrome—a new worldwide definition. The Lancet 2005; 366: 1059–1062.
Bei-Fan Z . Predictive values of body mass index and waist circumference for risk factors of certain related diseases in Chinese adults: study on optimal cut-off points of body mass index and waist circumference in Chinese adults. Asia Pacific J Clin Nutr 2002; 11: 685–693.
Durnin J, Womersley J . Body fat assessed from total body density and estimation from skinfolds thickness: measurements on 481 men and women aged from 16 to 72 years. British J Nutr 1974; 32: 77–97.
Chang CJ, Wu CH, Chang CS, Yao WJ, Yang YC, Wu JS et al. Low body mass index but high percent body fat in Taiwanese subjects: implications of obesity cutoffs. Int J Obes 2003; 27: 253–259.
Dahly DL, Gordon-Larsen P, Popkin BM, Kaufman JS, Adair LS . Associations between Multiple Indicators of Socioeconomic Status and Obesity in Young Adult Filipinos Vary by Gender, Urbanicity, and Indicator Used. J Nutr 2010; 140: 366–370.
Victora CG, Adair L, Fall C, Hallal PC, Martorell R, Richter L et al. Maternal and child undernutrition: consequences for adult health and human capital. Lancet 2008; 371: 340–357.
Kulldorff M, Nagarwalla N . Spatial disease clusters: detection and inference. Stat Med 1995; 14: 799–810.
Kulldorff M, Huang L, Pickle L, Duczmal L . An elliptic spatial scan statistic. Stat Med 2006; 25: 3929–3943.
Kulldorff M . SatScan user guide 2006.
Pedro MRA, Benavides RC, Barba CVC . Dietary changes and their health implications in the Philippines. FAO Food and Nutrition Paper. Food and Agriculture Organization: Rome, 2006.
Adair LS . Dramatic rise in overweight and obesity in adult Filipino women and risk of hypertension. Obes Res 2004; 12: 1335–1341.
Adair LS, Gultiano S, Suchindran C . 20-year trends in Filipino women’s weight reflect substantial secular and age effects. J Nutr 2011; 141: 667–673.
Sobal J, Stunkard AJ . Socioeconomic status and obesity: a review of the literature. Psychol Bulletin 1989; 105: 260–275.
McLaren L . Socioeconomic status and obesity. Epidemiologic Rev 2007; 29: 29–48.
Monteiro CA, Moura EC, Conde WL, Popkin BM . Socioeconomic status and obesity in adult populations of developing countries: a review. Bulletin of the World Health Organization 2004; 82: 940–946.
Vlahov D, Galea S . Urbanization, urbanicity, and health. J Urban Health 2002; 79: S1–S12.
Rundle A, Roux AV, Free LM, Miller D, Neckerman KM, Weiss CC . The urban built environment and obesity in New York City: a multilevel analysis. Am J Health Promotion 2007; 21: 326–334.
Huang L, Tiwari RC, Pickle LW, Zou Z . Covariate adjusted weighted normal spatial scan statistics with applications to study geographic clustering of obesity and lung cancer mortality in US. Stat Med 2010; 29: 2410–2422.
Edwards KL, Cade JE, Ransley JK, Clarke GP . A cross-sectional study examining the pattern of childhood obesity in Leeds: affluence is not protective. Arch Dis Child 2010; 95: 94–99.
Sobngwi E, Mbanya JC, Unwin NC, Porcher R, Kengne AP, Fezeu L et al. Exposure over the life course to an urban environment and its relation with obesity, diabetes, and hypertension in rural and urban Cameroon. Int J Epidemiol 2004; 33: 769–776.
Wilson EB . Probable inference, the law of succession, and statistical inference. J Am Stat Assoc 1927; 22: 209–212.
Newcombe RG . Two-sided confidence intervals for the single proportion: comparison of seven methods. Stat Med 1998; 17: 857–872.
Acknowledgements
Research supported by the NIH 1 R01 HL085144-03, a predoctoral traineeship at the Carolina Population Center T32-HD07168, and a Medical Research Council Population Health Scientist Fellowship G0902101. This research is facilitated by the Office of Population Studies, University of San Carlos, Cebu City, Philippines.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Nutrition & Diabetes website
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Dahly, D., Gordon-Larsen, P., Emch, M. et al. The spatial distribution of overweight and obesity among a birth cohort of young adult Filipinos (Cebu Philippines, 2005): an application of the Kulldorff spatial scan statistic. Nutr & Diabetes 3, e80 (2013). https://doi.org/10.1038/nutd.2013.21
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nutd.2013.21