Abstract
Background:
We examined the ability of the apolipoprotein AI mimetic peptide L-4F to improve the metabolic state of female and male ob mice and the mechanisms involved.
Methods:
Female and male lean and obese (ob) mice were administered L-4F or vehicle for 6 weeks. Body weight was measured weekly. Fat distribution, serum cytokines and markers of cardiovascular dysfunction were determined at the end of treatment.
Results:
L-4F significantly decreased serum interleukin (IL)-6, tumor necrosis factor-α and IL-1β. L-4F improved vascular function, and increased serum adiponectin levels and insulin sensitivity compared with untreated mice. In addition, L-4F treatment increased heme oxygenase (HO)-1, pAKT and pAMPK levels in kidneys of ob animals. pAKT and pAMPK levels were significantly reduced in the presence of an HO inhibitor. Interestingly, L4F did not alter body weight in female mice, but caused a significant reduction in males.
Conclusions:
L-4F treatments reduced cardiovascular risk factors and improved insulin sensitivity in female ob mice independent of body fat changes. Reduced inflammatory cytokine levels accompanied by increased HO activity, serum adiponectin and improved insulin sensitivity suggest that L-4F may promote the conversion of visceral fat to a healthier phenotype. Therefore, L-4F appears to be a promising therapeutic strategy for treating both cardiovascular risk factors and insulin resistance in obese patients of either gender.
Similar content being viewed by others
Introduction
Obesity affects over 72 million adults in the United States with a disproportionate prevalence in women.1, 2 Moderate to severe obesity is associated with increased risk for cardiovascular complications and insulin resistance in humans3, 4 and animals.5 In particular, intra-abdominal fat correlates with insulin resistance and is an important determinant of cardiovascular risk.6 Although men have received much attention for exhibiting such ‘android’ obesity, excess visceral fat deposition is present in 41% of women in Western countries (www.dh.gov.uk).
Visceral obesity creates a state of low-grade inflammation characterized by increased pro-inflammatory cytokine levels7, 8, 9 that contributes to insulin resistance10 and oxidative stress that impairs vascular and cardiac function.5 Indeed, mice lacking tumor necrosis factor (TNF)-α have significantly improved insulin sensitivity and glucose homeostasis in response to diet-induced obesity.11, 12, 13 In addition, ob mice overexpressing adiponectin have reduced inflammation and improved insulin sensitivity, accompanied by an increase in adipocyte number and smaller adipocyte size.14 These data suggest that promoting the expansion of adipocyte number may prevent or stave off the negative inflammatory effects of larger adipocytes. The increase in inflammatory cytokine production observed with obesity may result from an increase in reactive oxygen species.5, 15 It has been reported that reactive oxygen species produced by adipocytes increases the expression of MCP-1, a chemoattractant for macrophages, a key producer of such cytokines.5 This increase in reactive oxygen species contributes to progressive deterioration in vascular function.5
Abnormal high-density lipoprotein cholesterol (HDL-c) metabolism may also contribute to the increased cardiovascular disease risk caused by diabetes and obesity. The HDL-c particle distribution is abnormal in both types 1 and 2 diabetes, with decreases in the relative fraction of the large HDL-c particles believed to be cardioprotective.16 Apolipoprotein A-I (apoA-1) is the major protein component of HDL-c in plasma. The level of apoA-I is more closely correlated with the reduced risk of atherosclerosis than any other marker of HDL-c.17 ApoA-I prevents the oxidation and aggregation of pro-atherogenic low-density lipoprotein cholesterol (LDL-c) particles within the arterial wall and stimulates the mobilization of cholesterol from the same source.18 Infusion of apoA-I halts the progression of atherosclerosis and promotes its regression, reverses endothelial dysfunction, and induces lipid and macrophage efflux from established lesions in animals.19, 20, 21
Much effort has gone into designing peptide analogs of apoA-I that can promote the formation of HDL-c-like particles with improved potency or efficacy in vivo. L-4F, an apoA-1 mimetic peptide, improves insulin resistance in male ob mice, reduces inflammatory cytokines, reestablishes nitric oxide (NO)/superoxide ratios and reduces consequent cardiovascular risk.22, 23 Its enantiomer, D-4F, reduces atherosclerotic lesions,24 causes HDL-c to become anti-inflammatory, stimulates HDL-c-mediated cholesterol efflux and increases reverse cholesterol transport from macrophages.5, 24 In a phase 1 human trial, a single oral dose of D-4F improved HDL-c anti-inflammatory function.25 D-4F has also been shown to reduce the size of white adipose tissue stores (but not body weight) in male mice fed with a high-fat diet,26 and to decrease visceral fat in male ob mice.22, 23 L-4F is currently in clinical trials and has been hailed as being especially promising as a potential treatment for obesity and the metabolic syndrome.27 However, the actions of L-4F in female ob mice in addition to the efficacy of L-4F in improving markers of vascular function in obese mice remain to be examined.
Heme oxygenase 1 (HO-1) induction is known to suppress ROS production and promote increases in insulin sensitivity.5 In this study, we evaluated the mechanism by which L-4F affected HO-1 and subsequently, visceral and subcutaneous fat distribution in female and male ob mice. We then examined whether reduced visceral obesity is essential for the improved metabolic profile seen in L-4F-treated animals. Male and female ob mice treated with L-4F had significant improvements in insulin sensitivity and reduced inflammatory cytokine levels. However, we show for the first time that administration of L-4F in ob female mice decreases inflammatory cytokines and improves insulin responsiveness independent of changes in body weight. Furthermore, L-4F was effective in restoring HO-1 dependent increases in NO levels in female ob mice, indicating improved vascular function, and restored superoxide production and systolic blood pressure in male ob mice. Last, L-4F treatment resulted in a marked increase in heme oxygenase (HO) activity in both male and female ob mice. Therefore, L-4F has the potential to have a crucial therapeutic role in improving metabolic syndrome parameters and indices of vascular function-associated poor cardiovascular health.
Materials and methods
Animal care and L-4F administration
Male and female ob mice (B6v-Lep ob/J) were purchased from Harlan (Chicago, IL, USA) at the age of 6 weeks. Lean mice (age-matched B6.V, lean, Harlan) were used as control. Sex-matched lean and ob mice were fed a normal laboratory animal diet (Research diets, New Brunswick, NJ, USA) and had free access to water. Body weight of ob and lean mice were 34±5 g and 26±3 g, respectively, and glucose levels were 229±21 mg dl−1 and 154±9 mg dl−1, respectively, at the start of the experiments.
At 7 weeks of age, L-4F (2 mg kg−1 per day) or vehicle (ABCT: ammonium bicarbonate buffer at pH 7.4 containing 0.01% Tween-20), was administered intraperitoneally daily for 6 weeks to male and female ob and lean control mice. There were 10 groups of animals: (A) male lean, (B) male lean-L-4F, (C) male ob, (D) male ob-L-4F, (E) male ob-L-4F+SnMP (stannous mesoprophryin was given intraperitoneally 2 mg per 100 g body weight three times per week), (F) female lean, (G) female lean-L-4F, (H) female ob, (I) female ob-L-4F and (J) female ob-L-4F+SnMP. Systolic blood pressure was determined weekly by the tail-cuff method as previously described.28 The Animal Care and Use Committee of New York Medical College approved all experiments.
Effect on body weight, appearance and fat content
At the time of killing, the body weight of all mice was measured. The subcutaneous and visceral fat visible in the abdomen, mesenteric fat, fat around the liver, kidney, spleen, heart, ovaries and testes were dissected free, pooled for each mouse and weighed. Subcutaneous and visceral fat were weighed separately.
Glucose levels and insulin tolerance tests
Mouse blood glucose was determined by testing 5 μl of tail-vein blood using an Accu-Chek (Roche, Indianapolis, IN, USA) active blood glucose-monitoring system. After a 12 -h fast, mice were injected intraperitoneally with insulin (2.0 units kg−1). Blood samples were taken at 0 (basal), 30, 60, 75 and 90 min, and used to measure glucose levels.
LDL/VLDL and cytokine measurements
Serum LDL/VLDL (very low-density lipoprotein) cholesterol levels were measured in serum collected at the time of killing (24-h post previous injection) using LDL/VLDL Quantification Kits (Biovision, Mountainview, CA, USA). Adiponectin (high molecular weight), TNF-α, interleukin (IL)-1β and IL-6 were determined in mouse serum using an enzyme-linked immunosorbent assay assay (Pierce Biotechnology, Woburn, MA, USA). The assays were performed according to the manufacturer's guidelines.
Measurement of cardiac superoxide (O2−) levels
The hearts were placed in plastic scintillation minivials, containing 5 μmol l−1 lucigenin for the detection of O2−, in a final volume of 1 ml of air-equilibrated Krebs solution buffered with 10 mmol M−1 HEPES–NaOH (pH 7.4) as previously described.29 Lucigenin chemiluminescence was measured in a liquid scintillation counter (LS6000IC, Beckman Instruments, San Diego, CA, USA).
Determination of HO activity and NO levels
Aortic HO activity was assayed as described previously.30 Bilirubin, the end product of heme degradation, was extracted from chloroform, and its concentration was determined using the difference in absorbance between λ460 and λ530 nm with an absorption coefficient of 40 mM−1cm−1 (dual UV/VIS beam spectrophotometer lambda 25; PerkinElmer Life and Analytical Sciences, Wellesley, MA, USA). Under these conditions, HO activity was linear with protein concentration, time-dependent and substrate-dependent.31
For NO levels in whole kidney and aorta homogenate samples, 0.3 mg of protein were evaluated by measuring total nitrite and nitrate content in culture medium using the NO quantification kit and following the manufacturer's instructions (Active Motif, Carlsbad, CA, USA).
Western blot analysis of the kidney and aorta for HO-1, pAMPK and pAkt expression
At the time of killing, aorta and kidney were harvested, drained of blood and flash frozen in liquid nitrogen. Frozen aorta and kidney segments were pulverized and placed in a homogenization buffer as previously described.32 Homogenates (20–50 μg of protein) were examined by protein immunoblot. HO-1, HO-2,22 AMPK, pAMK, AKT and pAkt (Cell Signaling, Danvers, MA, USA) levels were determined as previously described.22
Statistical analyses
Statistical significance was determined by the Fisher method of analysis of multiple comparisons (P<0.05). For comparisons among treatment groups, the null hypothesis was tested by a two-factor analysis of variance for multiple groups or unpaired t-test for two groups. Data are presented as mean±s.e.
Results
Effects of L-4F on male and female body fat
L-4F treatment daily for 6 weeks prevented weight gain in ob male mice in accordance with previous findings (Figure 1a). Unexpectedly, ob female mice that received L-4F continued to gain weight at a rate similar to untreated ob mice (Figure 1a). Food intake in the male and female ob control and treated groups were comparable (ob male=3.66±0.35 g per day; ob male+L-4F=3.6±0.2 g per day; ob female=3.5±0.26 g per day; and ob female+L-4F=3.55±0.1 g per day). At the end of the 6-week treatment period, L-4F slightly decreased the ratio of subcutaneous fat to whole body weight in both males and females (Figure 1b). However, the ratio of visceral fat to whole body weight was decreased only in L-4F-treated males (Figure 1c). Female mice treated with L-4F showed a small but significant increase in the visceral fat to body weight ratio compared with controls (Figure 1c). The changes we measured in the fat to body weight ratio are consistent with the changes that were measured in body weight, which suggests that L-4F treatment may indeed cause sexually dimorphic responses.
Effect of L-4F on body composition in ob mice after 6 weeks of L-4F treatment (2 mg kg−1 per day) or control (a) Effect of L-4F treatment on body weight. ob male and female mice, respectively, were treated and weight determined (average of two independent experiments), n=10 for untreated and treated ob groups. Results are means±s.e. Levels of significance: *P<0.05 vs ob male+vehicle. (b) Effect of L-4F on subcutaneous fat to total body weight ratio. Levels of significance: *P<0.01 vs ob male and ***P<0.05 vs ob female. (c) Effect of L-4F on visceral fat to total body weight ratio. Levels of significance: *P< 0.05 vs ob male and #P<0.05 vs ob female.
Effects of L-4F on glucose levels and insulin tolerance tests
Chronic L-4F treatment reduced high fasting plasma glucose levels in ob males and females (Figure 2a). In addition, insulin administration to the L-4F-treated ob female mice resulted in a significant suppression of blood glucose levels but not in ob females receiving vehicle alone (Figure 2b). Last, the area under the curve determined for the data presented in Figure 2b was higher in vehicle compared with L-4F-treated ob females (Figure 2c). These results suggest that L-4F restores insulin sensitivity in female ob mice independent of changes in body weight (Figure 1a).
(a–c) Fasting glucose and insulin tolerance test. (a) Effect of L-4F treatment on glucose levels in ob male and female mice. The results are expressed as means±s.e.m., n=4. Levels of significance: *P<0.01 vs ob male and #P<0.05 vs ob female. (b) Intraperitoneal insulin tolerance test (IPGTT). The results are expressed as means±s.e.m., n=4. Levels of significance: *P<0.01 and ***P<0.001 vs ob female control. (c) Area under the curve for IPGTT. The results are expressed as means±s.e.m., n=4. Levels of significance: **P<0.005 vs ob female control.
Effects of L-4F on adiponectin and cytokine levels
It has been shown that overexpression of adiponectin in the ob mouse model leads to expansion of adipose tissue.33 We have previously shown that L-4F increases adiponectin levels in male mice.22 We therefore examined whether male and female mice show a difference in adiponectin responses to L-4F. L-4F produced a significant increase in plasma adiponectin levels in both ob female and male animals (Figure 3a). However, adiponectin levels in ob female mice were increased compared with ob male mice treated with L-4F, suggesting that adipose tissue maintenance and expansion in ob female mice may result from increased adiponectin levels.14
(a–d) Effect of L-4F on serum cytokines. L-4F was administered daily for 6 weeks and serum samples were obtained immediately before killing. (a) Effect of L-4F on serum adiponectin levels in ob male and female mice. The results are expressed as means±s.e., n=8–10. Levels of significance: *P<0.001 vs ob male, #P<0.05 vs ob male and **P<0.05 vs ob female. (b) Effect of L-4F on serum IL-6 levels in ob male and female mice. Levels of significance: *P<0.01 vs ob male, #P<0.05 vs ob male and **P<0.05 vs ob female. (c) Effect of L-4F on serum TNF-α levels in ob mice. Levels of significance: *P<0.01 vs ob male and #P<0.05 vs ob female. (d) Effect of L-4F on IL-1β serum levels in ob female mice. Levels of significance: *P<0.01 vs ob male and #P<0.05 vs ob female.
We also examined circulating levels of cytokines that are typically associated with obesity-mediated insulin resistance and vascular dysfunction. Female ob animals initially exhibited increased plasma IL-6 levels when compared with age-matched ob male mice (Figure 3b). L-4F produced a decrease in plasma IL-6 levels in both ob female and male mice when compared with untreated controls. Similar results were observed for plasma TNF-α and IL-1β levels (Figures 3c and d). Thus, although visceral fat is not lost in the female ob mice treated with L-4F, the inflammatory cytokine state is markedly improved, suggesting that the adipose tissue is healthier.14
Effects of L-4F on blood pressure and vascular function
In addition to metabolic defects, ob mice have altered cardiac function, which is a common consequence of obesity. Figure 4a shows that ob male mice are hypertensive compared with lean controls. L-4F treatment was highly successful in restoring systolic blood pressure to levels matching lean controls (Figure 4a). Additionally, ob male mice had significantly elevated cardiac superoxide levels, an indicator of oxidative stress (Figure 4b). Following L-4F treatment, superoxide production was normalized (Figure 4b). Aortic NO contributes to endothelial function and protects against hypertension. NO release from the aorta of ob female mice was reduced compared with lean female mice (Figure 4c). This decrease in NO was ameliorated by L-4F treatment (Figure 4c). These results indicate that L-4F may have a role in vascular protection in obese mice.
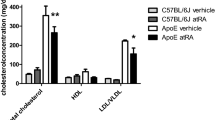
Effect of L-4F on blood pressure and vascular function. (a) Effect of L-4F on systolic blood pressure. Levels of significance: **P<0.01 vs ob vehicle and #P<0.05 vs ob vehicle. (b) Cardiac superoxide production. Levels of significance: *P<0.05 vs ob vehicle and #P<0.05 vs ob vehicle. (c) Effects of L-4F on NO levels. Levels of significance: *P<0.05 vs ob female and #P<0.05 vs ob female. (d) Effect of L-4F treatment on LDL/VLDL levels. Levels of significance: *P<0.01 vs ob male and #P<0.01 vs ob female.
Mice homozygous for the obese spontaneous mutation (ob mice) have elevated circulating free fatty acids, raised triglycerides, an increase in both low-density lipoprotein (LDL) and high-density lipoprotein (HDL) cholesterol and marked hepatic steatosis.34, 35, 36 In these mice, L-4F was effective in reducing the LDL/VLDL cholesterol ratio in both ob males and females (Figure 4e).
Effects of L-4F on HO-1 expression and HO activity
Obesity has been linked with increases in adipocyte oxidative stress, while HO-1 is strongly induced by oxidant stress and helps protect against oxidative insult in cardiovascular disease.5 Given that we have previously shown that administration of an HO-1 inducer increases serum adiponectin levels,29 we wanted to examine the possibility that L-4F increases adiponectin levels by raising HO-1 levels. Thus, we examined HO-1 levels in the kidneys and aortas of ob and lean mice. As in males, HO-1 in both the aortas (data not shown) and kidneys of ob females differed significantly from lean animals (Figures 5a and b). In addition, HO-1 levels were significantly lower in ob females compared with ob males (Figure 5b). We next compared the effect of L-4F on male and female HO-1 protein expression in renal and vascular tissue samples. L-4F increased HO-1 expression in both ob male and female animals (Figure 5c). In contrast to the effects on HO-1, HO-2 levels in renal and vascular tissue samples were unaffected by L-4F treatment in both male and female lean and ob animals (data not shown). L-4F increased HO activity in the aortic tissue samples of both ob male and female mice (Figure 5d). The increase in HO activity was inhibited by SnMP, an inhibitor of HO activity (Figure 5d). These results indicate that L-4F is an inducer of HO activity. Thus, the improvements in inflammatory cytokines and indices of cardiovascular function following L-4F treatment are likely mediated by L-4F-induced increases in HO activity.
(a–d) Effects of L-4F on levels of HO-1 and HO activity. Kidney samples were subjected to western blotting for the determination of HO-1 protein expression and densitometry analysis of HO-1/actin ratio. (a, b) Expression of HO-1 in the kidney of lean and ob male and female mice. Results are means±s.e., n=4. Levels of significance: *P<0.05 vs ob male. (c) Effect of L-4F on HO-1 expression in the kidneys of ob female and male mice. Results are means±s.e., n=4. Levels of significance: *P<0.05 vs ob male, **P<0.01 vs ob male and ***P<0.01 vs ob female. (d) Effect of L-4F and SnMP on HO activity in the aortas of ob male and female mice. Results are means±s.e., n=4. Levels of significance: *P<0.001 vs ob male, **P<0.001 vs ob male+L-4F, ***P<0.001 vs ob female and #P<0.01 vs ob female+L-4F.
To examine the contribution of vascular and renal AKT and AMPK pathways to the increase in HO-1 expression, we assessed vascular and renal expression of phosphorylated AMPK and AKT in L-4F-treated ob males and ob females. As seen in Figure 6, L-4F significantly increased basal renal AKT and AMPK phosphorylation in both ob males and females. Similar results were obtained with aortic tissue (data not shown). The addition of SnMP, a potent inhibitor of HO activity, to L-4F-treated animals reversed this effect in both ob males and females (Figures 6a–d). These results suggest that L-4F stimulation of AMPK and AKT pathways is involved in its ability to increase HO-1 expression and increase HO activity.
(a–d) Effect of L-4F and SnMP inhibition of HO activity on pAMPK, pAKT and α-actin in the kidneys of control and L-4F-treated ob males and females. All data are represented as phosphorylated/total. (a) Western blot and densitometry analysis of renal pAMPK protein in ob males. Results are means±s.e., n=4. *P<0.01 vs ob male and **P<0.001 vs ob male+L-4F. (b) Representative western blot and densitometry analysis of pAKT protein in ob male mice. Results are means±s.e., n=4. *P<0.05 vs ob male and **P<0.05 vs ob male+L-4F. (c) Representative western blot and densitometry analysis of pAMPK protein in ob females. Results are means±s.e., n=4. *P< 0.05 vs ob female and **P<0.05 vs ob female+L-4F. (d) Representative western blot and densitometry analysis of pAMPK protein in ob females. Results are means±s.e., n=4. *P<0.05 vs ob female and **P<0.01 vs ob female+L-4F.
Discussion
The metabolic syndrome is typically characterized by chronic, low-grade inflammation, excessive visceral fat, insulin resistance, abnormal cholesterol levels and increased blood pressure. The present study clearly shows for the first time that administration of the apoA-I mimetic L-4F ameliorates effects associated with the metabolic syndrome in female ob mice. Intriguingly, the positive effects of L-4F treatment on metabolic and vascular function in ob female mice were independent of changes in body weight. In fact, the visceral fat to body weight ratio increased in female ob mice treated with L-4F. We report that administration of L-4F to both ob female and male mice restored insulin sensitivity, increased serum adiponectin, decreased the LDL/VLDL cholesterol ratio and decreased serum pro-inflammatory cytokines (TNF-α, IL-6 and IL-1β). Moreover, in ob male mice, L-4F improved systolic blood pressure and reduced cardiac superoxide production. In female obese mice, L4F caused an increase in HO-1-mediated NO levels. These novel findings suggest that L-4F has the potential to be a key therapeutic agent in the treatment of both vascular diseases and insulin resistance in obese patients.
We have previously shown that L-4F administration reduces fat mass in male ob mice.22, 23 Recent studies suggest that this effect is mediated by enhanced energy expenditure resulting from upregulation of UCP1 expression in brown fat.26 In contrast, females treated with L-4F did not exhibit a decrease in visceral body fat over the time course measured (Figure 1c). These results are in line with the sexual dimorphism frequently observed in males and females in response to energetic challenges. Instead of primarily modulating food intake, females defend and build adipose stores by maintaining low rates of energy expenditure.37 Indeed, when overfed with a palatable high-fat diet, female rats gain more body weight than males because of a greater conservation of energy expenditure with lower activation of thermogenesis in brown adipose tissue.38, 39
Several factors may contribute to the observed differences in effect on body fat stores. Kim et al.14 demonstrated that overexpression of adiponectin in the ob mouse leads to increased adipocyte number. Importantly, the adipose expansion in ob mice overexpressing adiponectin is associated with increases in insulin sensitivity.14 More recently, overexpression of adiponectin was shown to promote a more metabolically flexible adipose tissue and prevented hepatic lipid accumulation in mice fed with a high-fat diet.33 The roughly 1.5-fold elevation of adiponectin seen in L-4F-treated female ob mice above that seen in males could therefore promote adipose tissue expansion in ob female mice. Adipose tissue expansion in the L-4F-treated ob females is currently being investigated and could explain the increased visceral fat to body weight ratio despite increased insulin sensitivity and reduced serum TNF-α, IL-6 and IL-1β in the present study. This would suggest that L-4F treatment converts the visceral fat in female ob mice to a healthier phenotype, which may prevent ectopic lipid accumulation in the liver and skeletal muscle. In addition, gender differences in HO-1 and sex hormone levels may favor female adiposity, as estradiol and HO-1 induction lead to an increase in proliferation of pre-adipocytes.40, 41 It is possible that female mice require a lengthier L-4F treatment period before decreases in weight gain are observed. Nevertheless, the retention of fat mass in the female animals did not impair the ability of L-4F to ameliorate the inflammatory cytokine and insulin resistant state of obese females.
HDL-c and apoA-1 have potent anti-inflammatory properties.42, 43 During atherogenesis, cholesterol accumulation in macrophage foam cells induces inflammatory responses, apoptosis and other adverse effects.44 One of the major functions of HDL-c is to transport cholesterol from these foam cells to the liver for elimination in the bile.45 Cells are able to export excess cholesterol to apoA-1 by virtue of specialized cell membrane transporters, such as ABCA1, that belong to a superfamily of ATP-binding cassette transporters (ABCs).46 Mice lacking ABCA1 in all tissues or specifically in macrophages have a heightened response to treatment with the inflammatory stimulus lipopolysaccaride,47 including increased inflammatory cytokines in the circulation, implying that macrophage ABCA1 has an anti-inflammatory function. 4F peptides can mimic apoA-I in removing cholesterol and phospholipids by the ABCA1 pathway.48, 49, 50, 51 We are currently perusing more in-depth studies to uncover the direct role of the ABCA1 pathway in the effects of apoA-1 mimetic treatment. In addition to this mechanism, L-4F may reduce inflammation by inhibiting cellular expression of VCAM-1 and ICAM-1 on coronary endothelial cells, reducing CD11b expression on circulating monocytes and/or reducing CD11b-dependent adhesion of leukocytes to fibrinogen.52
HO-1 is a stress response protein whose induction is associated with protection against oxidative stress with a concomitant increase in adiponectin. The current studies indicate that L-4F treatment decreases oxidative stress in female mice as previously seen in males.5, 22, 23, 32 Indeed, HO-1 was dramatically induced in male mice to levels nearly twofold above those seen in lean animals, and female increases were even larger. These effects may underlie many of the beneficial actions of L-4F. For example, treatment of obese mice with an NADPH oxidase inhibitor reduced reactive oxygen species production in adipose tissue, attenuated the dysregulation of adipocytokines, and improved diabetes, hyperlipidemia and hepatic steatosis.53 It has been shown that induction of HO-1 serves as an intrinsic protective factor against atherosclerotic lesion formation, possibly inhibiting lipid peroxidation and influencing the NO pathway.5 Indeed, ob female mice exhibited decreased NO levels and elevated LDL/VLDL cholesterol ratio compared with lean female mice. Additionally, ob male mice had elevated superoxide production. These findings are in line with previous data inducting that oxidative stress decreases the messenger RNA and protein expression of ABCA1 and cholesterol efflux.54, 55 L-4F administration, however, improved NO levels while decreasing the LDL/VLDL cholesterol ratio in ob female mice, and reduced superoxide production in ob male mice. Increases in HO-1 expression and HO activity have also been shown to suppress inflammatory cytokine production in adipose tissue.22 Thus, HO-1 actions may also account for the reduction in plasma concentration of TNF-α, IL-6 and IL-1β in L-4F-treated mice.
L-4F-treated females also showed a remarkable improvement in parameters of glucose regulation. There is mounting evidence that removal of excess cholesterol from pancreatic beta cells via the ABCA1 has a role in protecting beta cell function and preventing diabetes.56 Improvements in beta cell function may contribute to the beneficial effects of L4-F on glucose homeostasis. Apolipoprotein/ABCA1 interactions can also behave like a ligand/receptor system. HDL-c initiates a calcium-sensitive signaling cascade through ABCA1 that stimulates CaMKK, which phosphorylates and activates AMPK.57, 58 Thus, HDL-c has been shown to increase muscular glucose uptake in patients with type 2 diabetes mellitus by activating AMP-activated protein kinase in skeletal muscle in an ABCA1-dependent manner. The current studies confirm L-4F-induced phosphorylation of not only AMPK but also AKT in the kidney, suggesting L-4F can directly modulate insulin signaling and thereby improve glucose regulation. Finally, reductions in inflammatory cytokines and increases in adiponectin may also have a role in modulating insulin sensitivity and restoring glucose tolerance.29, 59, 60
In conclusion, we have demonstrated that targeting the apoA-I fraction of HDL-c with a mimetic not only reduces cardiovascular risk factors, but improves insulin sensitivity and vascular health in both male and female obese mice. L-4F increases pAKT and pAMPK in a manner dependent on HO activity. Furthermore, our results demonstrate that the positive effects of L-4F are independent of changes in body weight in ob female mice. We believe that the increase in visceral fat observed in female ob mice treated with L-4F is protective and may prevent the ectopic accumulation of lipids in other insulin-sensitive tissues, a hypothesis currently under investigation. Indeed, despite increased visceral fat, L-4F increased insulin sensitivity, reduced inflammatory cytokine levels and increased adiponectin levels. In addition, overexpression of adiponectin in obese mice promotes adipose tissue expansion, improved insulin and glucose tolerance and reduced hepatic lipid accumulation.33 If extrapolated to humans, these results suggest that L-4F offers a powerful pharmacological method of treating the metabolic syndrome that may compliment weight loss therapy. L-4F appears to be a promising therapeutic strategy for treating both cardiovascular disease and insulin resistance in obese patients of either gender.
References
Borkan GA, Hults DE, Gerzof SG, Robbins AH, Silbert CK . Age changes in body composition revealed by computed tomography. J Gerontol 1983; 38: 673–677.
Ogden CL, Carroll MD, Curtin LR, McDowell MA, Tabak CJ, Flegal KM . Prevalence of overweight and obesity in the United States, 1999–2004. JAMA 2006; 295: 1549–1555.
Kannel WB, D’Agostino RB, Cobb JL . Effect of weight on cardiovascular disease. Am J Clin Nutr 1996; 63: 419S–422S.
Larsson B . Obesity, fat distribution and cardiovascular disease. Int J Obes 1991; 15 (Suppl 2): 53–57.
Abraham NG, Kappas A . Pharmacological and clinical aspects of heme oxygenase. Pharmacol Rev 2008; 60: 79–127.
Mesch VR, Siseles NO, Maidana PN, Boero LE, Sayegh F, Prada M et al. Androgens in relationship to cardiovascular risk factors in the menopausal transition. Climacteric 2008; 11: 509–517.
Hotamisligil GS, Murray DL, Choy LN, Spiegelman BM . Tumor necrosis factor alpha inhibits signaling from the insulin receptor. Proc Natl Acad Sci USA 1994; 91: 4854–4858.
Hotamisligil GS, Peraldi P, Budavari A, Ellis R, White MF, Spiegelman BM . Irs-1-mediated inhibition of insulin receptor tyrosine kinase activity in TNF-alpha- and obesity-induced insulin resistance. Science 1996; 271: 665–668.
Pradhan AD, Manson JE, Rifai N, Buring JE, Ridker PM . C-reactive protein, interleukin 6, and risk of developing type 2 diabetes mellitus. JAMA 2001; 286: 327–334.
Gustafson B . Adipose tissue, inflammation and atherosclerosis. J Atheroscler Thromb 2010; 17: 332–341.
Hotamisligil GS . Mechanisms of TNF-alpha-induced insulin resistance. Exp Clin Endocrinol Diabetes 1999; 107: 119–125.
Peraldi P, Spiegelman B . TNF-alpha and insulin resistance: summary and future prospects. Mol Cell Biochem 1998; 182: 169–175.
Uysal KT, Wiesbrock SM, Marino MW, Hotamisligil GS . Protection from obesity-induced insulin resistance in mice lacking TNF-alpha function. Nature 1997; 389: 610–614.
Kim JY, van de Wall E, Laplante M, Azzara A, Trujillo ME, Hofmann SM et al. Obesity-associated improvements in metabolic profile through expansion of adipose tissue. J Clin Invest 2007; 117: 2621–2637.
Naha PC, Davoren M, Lyng FM, Byrne HJ . Reactive oxygen species (ROS) induced cytokine production and cytotoxicity of pamam dendrimers in j774a.1 cells. Toxicol Appl Pharmacol 2010; 246: 91–99.
Jenkins AJ, Lyons TJ, Zheng D, Otvos JD, Lackland DT, McGee D et al. Serum lipoproteins in the diabetes control and complications trial/epidemiology of diabetes intervention and complications cohort: associations with gender and glycemia. Diabetes Care 2003; 26: 810–818.
Maciejko JJ, Holmes DR, Kottke BA, Zinsmeister AR, Dinh DM, Mao SJ . Apolipoprotein A-I as a marker of angiographically assessed coronary-artery disease. N Engl J Med 1983; 309: 385–389.
Khoo JC, Miller E, McLoughlin P, Steinberg D . Prevention of low density lipoprotein aggregation by high density lipoprotein or apolipoprotein A-I. J Lipid Res 1990; 31: 645–652.
Chiesa G, Sirtori CR . Use of recombinant apolipoproteins in vascular diseases: the case of apoA-I. Curr Opin Investig Drugs 2002; 3: 420–426.
Shah PK, Kaul S, Nilsson J, Cercek B . Exploiting the vascular protective effects of high-density lipoprotein and its apolipoproteins: an idea whose time for testing is coming, part ii. Circulation 2001; 104: 2498–2502.
Shah PK, Nilsson J, Kaul S, Fishbein MC, Ageland H, Hamsten A et al. Effects of recombinant apolipoprotein A-I(milano) on aortic atherosclerosis in apolipoprotein E-deficient mice. Circulation 1998; 97: 780–785.
Peterson SJ, Drummond G, Kim DH, Li M, Kruger AL, Ikehara S et al. L-4f treatment reduces adiposity, increases adiponectin levels, and improves insulin sensitivity in obese mice. J Lipid Res 2008; 49: 1658–1669.
Peterson SJ, Kim DH, Li M, Positano V, Vanella L, Rodella LF et al. The l-4f mimetic peptide prevents insulin resistance through increased levels of ho-1, pampk, and pakt in obese mice. J Lipid Res 2009; 50: 1293–1304.
Navab M, Anantharamaiah GM, Reddy ST, Hama S, Hough G, Grijalva VR et al. Oral d-4f causes formation of pre-beta high-density lipoprotein and improves high-density lipoprotein-mediated cholesterol efflux and reverse cholesterol transport from macrophages in apolipoprotein E-null mice. Circulation 2004; 109: 3215–3220.
Rader DJ . Molecular regulation of HDL metabolism and function: implications for novel therapies. J Clin Invest 2006; 116: 3090–3100.
Ruan X, Li Z, Zhang Y, Yang L, Pan Y, Wang Z et al. Apolipoprotein A-I possesses an anti-obesity effect associated with increase of energy expenditure and up-regulation of ucp1 in brown fat. J Cell Mol Med 2011; 15: 763–772.
Sherman CB, Peterson SJ, Frishman WH . Apolipoprotein A-I mimetic peptides: a potential new therapy for the prevention of atherosclerosis. Cardiol Rev 2010; 18: 141–147.
Cao J, Sodhi K, Inoue K, Quilley J, Rezzani R, Rodella L et al. Lentiviral-human heme oxygenase targeting endothelium improved vascular function in angiotensin II animal model of hypertension. Hum Gene Ther 2011; 22: 271–282.
Li M, Kim DH, Tsenovoy PL, Peterson SJ, Rezzani R, Rodella LF et al. Treatment of obese diabetic mice with a heme oxygenase inducer reduces visceral and subcutaneous adiposity, increases adiponectin levels, and improves insulin sensitivity and glucose tolerance. Diabetes 2008; 57: 1526–1535.
Chernick RJ, Martasek P, Levere RD, Margreiter R, Abraham NG . Sensitivity of human tissue heme oxygenase to a new synthetic metalloporphyrin. Hepatology 1989; 10: 365–369.
Abraham NG, Jiang H, Balazy M, Goodman AI . Methods for measurements of heme oxygenase (ho) isoforms-mediated synthesis of carbon monoxide and ho-1 and ho-2 proteins. Methods Mol Med 2003; 86: 399–411.
Peterson SJ, Husney D, Kruger AL, Olszanecki R, Ricci F, Rodella LF et al. Long-term treatment with the apolipoprotein a1 mimetic peptide increases antioxidants and vascular repair in type I diabetic rats. J Pharmacol Exp Ther 2007; 322: 514–520.
Asterholm IW, Scherer PE . Enhanced metabolic flexibility associated with elevated adiponectin levels. Am J Pathol 2010; 176: 1364–1376.
Wiegman CH, Bandsma RH, Ouwens M, van der Sluijs FH, Havinga R, Boer T et al. Hepatic VLDL production in ob/ob mice is not stimulated by massive de novo lipogenesis but is less sensitive to the suppressive effects of insulin. Diabetes 2003; 52: 1081–1089.
Silver DL, Jiang XC, Tall AR . Increased high density lipoprotein (HDL), defective hepatic catabolism of apoa-I and apoa-II, and decreased apoa-I mRNA in ob/ob mice. Possible role of leptin in stimulation of HDL turnover. J Biol Chem 1999; 274: 4140–4146.
Silver DL, Wang N, Tall AR . Defective HDL particle uptake in ob/ob hepatocytes causes decreased recycling, degradation, and selective lipid uptake. J Clin Invest 2000; 105: 151–159.
Shi H, Strader AD, Woods SC, Seeley RJ . Sexually dimorphic responses to fat loss after caloric restriction or surgical lipectomy. Am J Physiol Endocrinol Metab 2007; 293: E316–E326.
Roca P, Rodriguez AM, Oliver P, Bonet ML, Quevedo S, Pico C et al. Brown adipose tissue response to cafeteria diet-feeding involves induction of the ucp2 gene and is impaired in female rats as compared to males. Pflugers Arch 1999; 438: 628–634.
Rodriguez E, Monjo M, Rodriguez-Cuenca S, Pujol E, Amengual B, Roca P et al. Sexual dimorphism in the adrenergic control of rat brown adipose tissue response to overfeeding. Pflugers Arch 2001; 442: 396–403.
Anderson LA, McTernan PG, Barnett AH, Kumar S . The effects of androgens and estrogens on preadipocyte proliferation in human adipose tissue: influence of gender and site. J Clin Endocrinol Metab 2001; 86: 5045–5051.
Macotela Y, Boucher J, Tran TT, Kahn CR . Sex and depot differences in adipocyte insulin sensitivity and glucose metabolism. Diabetes 2009; 58: 803–812.
Parker TS, Levine DM, Chang JC, Laxer J, Coffin CC, Rubin AL . Reconstituted high-density lipoprotein neutralizes gram-negative bacterial lipopolysaccharides in human whole blood. Infect Immun 1995; 63: 253–258.
Levine DM, Parker TS, Donnelly TM, Walsh A, Rubin AL . In vivo protection against endotoxin by plasma high density lipoprotein. Proc Natl Acad Sci USA 1993; 90: 12040–12044.
Tabas I . Consequences and therapeutic implications of macrophage apoptosis in atherosclerosis: the importance of lesion stage and phagocytic efficiency. Arterioscler Thromb Vasc Biol 2005; 25: 2255–2264.
Fielding CJ, Fielding PE . Molecular physiology of reverse cholesterol transport. J Lipid Res 1995; 36: 211–228.
Dean M, Hamon Y, Chimini G . The human ATP-binding cassette (ABC) transporter superfamily. J Lipid Res 2001; 42: 1007–1017.
Zhu X, Lee JY, Timmins JM, Brown JM, Boudyguina E, Mulya A et al. Increased cellular free cholesterol in macrophage-specific ABCA1 knock-out mice enhances pro-inflammatory response of macrophages. J Biol Chem 2008; 283: 22930–22941.
Mendez AJ, Anantharamaiah GM, Segrest JP, Oram JF . Synthetic amphipathic helical peptides that mimic apolipoprotein A-I in clearing cellular cholesterol. J Clin Invest 1994; 94: 1698–1705.
Remaley AT, Thomas F, Stonik JA, Demosky SJ, Bark SE, Neufeld EB et al. Synthetic amphipathic helical peptides promote lipid efflux from cells by an ABCA1-dependent and an ABCA1-independent pathway. J Lipid Res 2003; 44: 828–836.
Tang C, Vaughan AM, Anantharamaiah GM, Oram JF . Janus kinase 2 modulates the lipid-removing but not protein-stabilizing interactions of amphipathic helices with ABCA1. J Lipid Res 2006; 47: 107–114.
Yancey PG, Bielicki JK, Johnson WJ, Lund-Katz S, Palgunachari MN, Anantharamaiah GM et al. Efflux of cellular cholesterol and phospholipid to lipid-free apolipoproteins and class A amphipathic peptides. Biochemistry 1995; 34: 7955–7965.
Patel S, Drew BG, Nakhla S, Duffy SJ, Murphy AJ, Barter PJ et al. Reconstituted high-density lipoprotein increases plasma high-density lipoprotein anti-inflammatory properties and cholesterol efflux capacity in patients with type 2 diabetes. J Am Coll Cardiol 2009; 53: 962–971.
Furukawa S, Fujita T, Shimabukuro M, Iwaki M, Yamada Y, Nakajima Y et al. Increased oxidative stress in obesity and its impact on metabolic syndrome. J Clin Invest 2004; 114: 1752–1761.
Wang X, Liao D, Bharadwaj U, Li M, Yao Q, Chen C . C-reactive protein inhibits cholesterol efflux from human macrophage-derived foam cells. Arterioscler Thromb Vasc Biol 2008; 28: 519–526.
Marcil V, Delvin E, Sane AT, Tremblay A, Levy E . Oxidative stress influences cholesterol efflux in THP-1 macrophages: role of ATP-binding cassette A1 and nuclear factors. Cardiovasc Res 2006; 72: 473–482.
Brunham LR, Kruit JK, Verchere CB, Hayden MR . Cholesterol in islet dysfunction and type 2 diabetes. J Clin Invest 2008; 118: 403–408.
Han R, Lai R, Ding Q, Wang Z, Luo X, Zhang Y et al. Apolipoprotein A-I stimulates amp-activated protein kinase and improves glucose metabolism. Diabetologia 2007; 50: 1960–1968.
Drew BG, Duffy SJ, Formosa MF, Natoli AK, Henstridge DC, Penfold SA et al. High-density lipoprotein modulates glucose metabolism in patients with type 2 diabetes mellitus. Circulation 2009; 119: 2103–2111.
Jager J, Gremeaux T, Cormont M, Le Marchand-Brustel Y, Tanti JF . Interleukin-1beta-induced insulin resistance in adipocytes through down-regulation of insulin receptor substrate-1 expression. Endocrinology 2007; 148: 241–251.
Kern PA, Ranganathan S, Li C, Wood L, Ranganathan G . Adipose tissue tumor necrosis factor and interleukin-6 expression in human obesity and insulin resistance. Am J Physiol Endocrinol Metab 2001; 280: E745–E751.
Acknowledgements
This work was supported by National Institutes of Health grants DK-068134, HL-55601 and HL-34300 (NGA). We would like to thank Angela P Burgess, Dong Hyun Kim and Attallah Kappas for their insight during the preparation of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-No Derivative Works 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Marino, J., Peterson, S., Li, M. et al. ApoA-1 mimetic restores adiponectin expression and insulin sensitivity independent of changes in body weight in female obese mice. Nutr & Diabetes 2, e33 (2012). https://doi.org/10.1038/nutd.2012.4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nutd.2012.4
Keywords
This article is cited by
-
Correlation between heat shock proteins, adiponectin, and T lymphocyte cytokine expression in type 2 diabetics
Cell Stress and Chaperones (2018)
-
Low adiponectin is associated with diastolic dysfunction in women: a cross-sectional study from the Tromsø Study
BMC Cardiovascular Disorders (2017)
-
Clinical characteristics and outcomes of biopsy-proven diabetic nephropathy
Frontiers of Medicine (2017)
-
The importance of the cellular stress response in the pathogenesis and treatment of type 2 diabetes
Cell Stress and Chaperones (2014)