Abstract
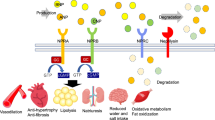
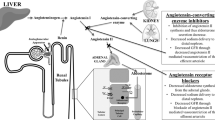
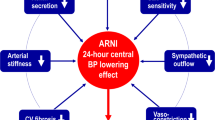
Angiotensin-converting-enzyme (ACE) inhibitors and angiotensin-receptor blockers (ARBs) have beneficial effects in patients with cardiovascular disease and in those with diabetes-related and diabetes-independent chronic kidney diseases. These beneficial effects are independent of the antihypertensive properties of these drugs. However, ACE inhibitors, ARBs, and combinations of agents in these two classes are limited in the extent to which they inhibit the activity of the renin–angiotensin–aldosterone system (RAAS). Angiotensin breakthrough and aldosterone breakthrough may be important mechanisms involved in limiting the effects of ACE inhibitors and ARBs. Whether direct renin inhibitors will overcome some of the limitations of ACE-inhibitor and ARB therapy by blocking the deleterious effects of the RAAS remains to be proven. This important area is, however, in need of further investigation.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Gerstein, H. C. et al. Rationale and design of a large study to evaluate the renal and cardiovascular effects of an ACE inhibitor and vitamin E in high-risk patients with diabetes: the MICRO-HOPE study. Microalbuminuria, cardiovascular, and renal outcomes. Heart Outcomes Prevention Evaluation. Diabetes Care 19, 1225–1228 (1996).
McPherson, E. A. et al. Chymase-like angiotensin II-generating activity in end-stage human autosomal dominant polycystic kidney disease. J. Am. Soc. Nephrol. 15, 493–500 (2004).
Chapman, A. B., Johnson, A., Gabow, P. A. & Schrier, R. W. The renin-angiotensin-aldosterone system and autosomal dominant polycystic kidney disease. N. Engl. J. Med. 323, 1091–1096 (1990).
Loghman-Adham, M., Soto, C. E., Inagami, T. & Cassis, L. The intrarenal renin-angiotensin system in autosomal dominant polycystic kidney disease. Am. J. Physiol. Renal Physiol. 287, 755–768 (2004).
Lewis, E. J. et al. Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N. Engl. J. Med. 345, 851–860 (2001).
Brenner, B. et al. Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N. Engl. J. Med. 345, 861–869 (2001).
Lewis, E. J., Hunsicker, L. G., Bain, R. P. & Rohde, R. D. The effect of angiotensin-converting-enzyme inhibition on diabetic nephropathy. N. Engl. J. Med. 329, 1456–1462 (1993).
Wolf, G. & Ritz, E. Combinatin therapy with ACE inhibitors and angiotensin II receptor blockers to halt progression of chronic renal disease: pathophysiology and indications. Kidney Int. 67, 799–812 (2005).
Nakao, N. et al. Combination treatment of angiotensin-II receptor blocker and angiotensin converting-enzyme inhibitor in non-diabetic renal disease (COOPERATE): a randomised controlled trial. Lancet 361, 117–124 (2003). Retraction in: Lancet 374, 1226 (2009).
Pfeffer, M. A. et al. Effects of candesartan on mortality and morbidity in patients with chronic heart failure: the CHARM-Overall programme. Lancet 362, 759–766 (2003).
Yusuf, S. et al. Telmisartan, ramipril, or both in patients at high risk for vascular events. N. Engl. J. Med. 358, 1547–1559 (2008).
Cohn, J. N. et al. Sustained reduction of aldosterone in response to the angiotensin receptor blocker valsartan in patients with chronic heart failure: results from the Valslartan Heart Failure Trial. Circulation 108, 1306–1309 (2003).
Yusuf, S. et al. Effects of an angiotensin-converting-enzyme inhibitor, ramipril, on cardiovascular events in high-risk patients. The Heart Outcomes Prevention Evaluation Study Investigators. N. Engl. J. Med. 342, 145–153 (2000).
Staessen, J., Lijnen, P., Fagard, R., Verschueren, L. J. & Amery, A. Rise in plasma concentration of aldosterone during long-term angiotensin II suppression. J. Endocrinol. 91, 457–465 (1981).
Bomback, A. S. & Klemmer, P. J. The incidence and implications of aldosterone breakthrough. Nat. Clin. Pract. Nephrol. 3, 486–492 (2007).
Schjoedt, K. J., Anderson, S., Rossing, P., Tarnow, L. & Parving, H. H. Aldosterone escape during blockade of the renin-angiotensin-aldosterone system in diabetic nephropathy is associated with enhanced decline in glomerular filtration rate. Diabetologia 47, 1936–1939 (2004).
Pitt, B. et al. The effect of spironolactone on morbidity and mortality in patients with severe heart failure. Randomized Aldactone Evaluation Study investigators. N. Engl. J. Med. 341, 709–717 (1999).
Pitt, B., Bakris, G., Ruilope, L. M., DiCarlo, L. & Mukherjee, R. Serum potassium and clinical outcomes in the Eplerenone Post-Acute Myocardial Infarction Heart Failure Efficacy and Survival Study (EPHESUS). Circulation 118, 1643–1650 (2008).
Schrier, R. W., Masoumi, A. & Elhassan, E. Aldosterone: role in edematous disorders, hypertension, chronic renal failure, and metabolic syndrome. Clin. J. Am. Soc. Nephrol. 5, 1132–1140 (2010).
Schrier, R. W. Aldosterone 'escape' vs 'breakthrough.' Nat. Rev. Nephrol. 6, 61 (2010).
Battenburg, W. W. & Jan Danser, A. H. The (pro)renin receptor: a new addition to the renin-angiotensin system? Eur. J. Pharmacol. 585, 320–324 (2008).
Lindenmeyer, M. T. et al. Interstitial vascular rarefaction and reduced VEGF-A expression in human diabetic nephropathy. J. Am. Soc. Nephrol. 18, 1765–1776 (2007).
Kang, J. J. et al. The collecting duct is the major source of prorenin in diabetes. Hypertension 51, 1597–1604 (2008).
Nguyen, G. et al. Pivotal role of the renin/prorenin receptor in angiotensin II production and cellular responses to renin. J. Clin. Invest. 109, 1417–1427 (2002).
Riccioni, O., Vitulano, N., D'Orazio, N. & Bellocci, F. Aliskiren, the first approved renin inhibitor: clinical application and safety in the treatment of hypertension. Adv. Ther. 26, 700–710 (2009).
Parving, H. H. et al. Aliskiren combined with losartan in type 2 diabetes and nephropathy. N. Engl. J. Med. 358, 2433–2446 (2008).
Parving, H. H. et al. Aliskiren Trial in Type 2 Diabetes Using Cardio-Renal Endpoints (ALTITUDE): rationale and study design. Nephrol. Dial. Transplant. 24, 1663–1671 (2009).
McMurray, J. J. et al. Effects of the oral direct renin inhibitor aliskiren in patients with symptomatic heart failure. Circ. Heart Fail. 1, 17–24 (2008).
Sanoski, C. A. Aliskiren: an oral direct renin inhibitor for the treatment of hypertension. Pharmacotherapy 29, 193–212 (2009).
Acknowledgements
The authors would like to thank Jan Darling for her editorial assistance.
Author information
Authors and Affiliations
Contributions
All authors researched the data for the article, provided a substantial contribution to discussion of content, and contributed to the review and/or editing of the manuscript before submission. R. W. Schrier and N. Nobakht contributed equally to writing the article.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Nobakht, N., Kamgar, M., Rastogi, A. et al. Limitations of angiotensin inhibition. Nat Rev Nephrol 7, 356–359 (2011). https://doi.org/10.1038/nrneph.2011.29
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrneph.2011.29
This article is cited by
-
The Role of Renin–Angiotensin–Aldosterone System and Its New Components in Arterial Stiffness and Vascular Aging
High Blood Pressure & Cardiovascular Prevention (2018)
-
Effects of pentoxifylline on proteinuria and glucose control in patients with type 2 diabetes: a prospective randomized double-blind multicenter study
Diabetology & Metabolic Syndrome (2015)
-
Glomerular hyperfiltration: definitions, mechanisms and clinical implications
Nature Reviews Nephrology (2012)