Key Points
-
The innate immune system has a series of conserved receptors, known as pattern-recognition receptors, which recognize specific pathogen-associated molecular patterns. The identification of Toll-like receptors (TLRs) that fulfil this role is an important advance in our understanding of the early events of host defence. Moreover, TLRs are potential regulators and controllers of an antigen-specific adaptive immune response.
-
TLRs are type I transmembrane proteins that are evolutionarily conserved between insects and humans. So far, ten TLRs have been identified. Consistent with their function as pathogen-recognition receptors, TLRs are expressed mainly in the cell types that are involved in the first line of defence. TLRs activate signalling pathways that are similar to those that are engaged by interleukin-1 (IL-1), leading to the nuclear translocation of nuclear factor-κB (NF-κB) and the subsequent transcriptional activation of numerous pro-inflammatory genes.
-
Blocking TLR function as a potential therapeutic strategy is obvious when bacteria and bacterial products, through exaggerated TLR responses, activate an uncontrolled network of host-derived mediators, as seen in sepsis or pathogen-induced disease exacerbations.
-
Allergic asthma is chosen as an example of a chronic, T-helper type 2 (TH2)-cell-driven inflammatory disease to show how TLR agonists or antagonists might offer possibilities for therapeutic intervention. The hygiene hypothesis proposes that the relatively sterile environment and increased use of antibiotics for childhood infections in Western countries has contributed to the recent epidemic of asthma. So, TLR-activating bacterial vaccines or selective TLR agonists that mimic host-defence-induced responses might have therapeutic benefit in atopic diseases.
-
In addition to the development of new therapies for diseases such as sepsis or disease-modifying therapies that result in immune deviation in asthma, reagents that enhance TLR-signalling pathways can be powerful adjuvants for fighting pathogens or cancer.
-
It has been shown that TLRs can be stimulated by endogenous ligands, such as heat-shock proteins, saturated and unsaturated fatty acids, hyaluronic-acid fragments, double-stranded DNA and surfactant protein-A. These observations and the discovery of low-molecular-mass synthetic compounds that activate TLRs raises interest in these receptors as being potential targets for the development of new therapies in multiple diseases.
Abstract
The family of Toll-like receptors (TLRs) is receiving considerable attention as potential regulators and controllers of the immune response through their ability to recognize pathogen-associated molecular patterns. The discovery that endogenous ligands, as well as microbial components, are recognized by TLRs, and that small-molecular-mass synthetic compounds activate TLRs, raised interest in these receptors as potential targets for the development of new therapies for multiple diseases. In this review, we discuss the current and future use of TLR agonists or antagonists in chronic inflammatory diseases and highlight potential problems that are associated with such approaches.
Similar content being viewed by others
Main
The immune system has been divided traditionally into an INNATE and ADAPTIVE component, each of which has different roles and functions in defending the organism against foreign agents, such as bacteria or viruses. The innate immune system has developed a series of conserved receptors, known as pattern-recognition receptors (PRRs), that recognize specific pathogen-associated molecular patterns (PAMPs), thereby allowing the innate immune system to distinguish self-molecules from pathogen-associated non-self structures and initiate the host defence response1. Recognition of PAMPs by PRRs results in the activation of signalling events that induce the expression of effector molecules, such as cytokines, chemokines and co-stimulatory molecules, which subsequently control the activation of an antigen-specific adaptive immune response. An important advance in our understanding of early events in microbial recognition and the subsequent development of immune responses has been the identification of Toll-like receptors (TLRs) as key PRRs of the innate immune system1.
The gene that encodes the Toll protein was shown to be involved in embryonic development in Drosophila, and was identified subsequently as being an essential molecule for driving the immune response. TLRs are mammalian homologues of this protein that can detect PAMPs2. The first report of a mammalian TLR and its involvement in host defence — TLR-4 as a receptor for LIPOPOLYSACCHARIDE (LPS)3 — was followed rapidly by the discovery that the human genome contains several TLRs — ten have been found so far, TLR-1–TLR-10. Members of the TLR family share characteristic extracellular and cytoplasmic domains. Their extracellular domains include several leucine-rich repeats (LRRs), whereas the cytoplasmic domain is similar to the cytoplasmic portion of the interleukin-1 receptor (IL-1R), which is commonly known as the Toll/IL-1R homologous region (TIR domain)4. Consistent with their function as PRRs, TLRs are expressed mainly in the cell types that are involved in the first line of defence, such as DENDRITIC CELLS, MACROPHAGES, NEUTROPHILS, mucosal epithelial cells and dermal endothelial cells5. Distinct subsets of dendritic cells and dendritic-cell precursors express different subsets of TLRs that enable them to induce specific patterns of immune response to different pathogens. For example, plasmacytoid dendritic cells strongly express TLR-9, whereas myeloid dendritic cells do not. Instead, they express other TLRs, including TLR-4, which cause them to be activated by a different set of PAMPs, including LPS6. Activation of dendritic cells by stimulation of TLRs results in the production of cytokines, such as IL-12, that induce T-helper type 1 (TH1) CELLS, which tends to direct the adaptive immune response to differentiate towards a TH1 phenotype6. The identification of TLRs as PRRs that are involved in controlling dendritic-cell activation led to substantial interest in these receptors as possible regulators of adaptive immune responses and, by inducing a specific cytokine environment, their involvement in the pathogenesis of several chronic inflammatory diseases. Therefore, we focus our discussion on the emerging role of TLRs in the pathogenesis of inflammatory diseases and how agonists or antagonists of these receptors might be used to treat various pathological conditions. We describe the basic mechanism of an allergic inflammatory response as an example to show how targeting TLRs might offer promising new therapeutic benefits. In addition, the current and future use of TLR agonists and antagonists in other chronic inflammatory diseases, and the activation of TLRs by exogenous or endogenous ligands are discussed.
TLRs: members and ligands
Several reviews describe elegantly the known members of the TLR family, their ligands and the signalling pathways that are induced by stimulation of the receptors4,5,6. Therefore, we summarize only briefly the current knowledge, focusing on the most important information that is required to understand the function of TLRs (Table 1). Different TLRs have been shown to be crucial for the selective recognition of specific PAMPs that are common to a range of either GRAM-NEGATIVE or GRAM-POSITIVE BACTERIA. The observation that a point mutation in the TIR domain of the mouse Tlr4 gene abolished the response to LPS provided the first evidence that this particular receptor might be involved in the innate immune response to Gram-negative bacteria3,7,8. By contrast, Tlr-2-deficient mice have a normal inflammatory response to LPS, but macrophages from these animals are less responsive to Gram-positive bacterial cell walls and PEPTIDOGLYCAN. Indeed, TLR-2 recognizes LPS from Porphyromonas gingivitis9 and Leptospira interrogans10, which differs in structure from the LPS of Gram-negative bacteria. These results are evidence of TLR selectivity in PAMP recognition, although other TLRs can recognize the same components of both Gram-negative and Gram-positive bacteria. Indeed, flagellin, the principal element of bacteria flagella, is a highly virulent molecule that is recognized by TLR-5 (Ref. 11), whereas TLR-9 is required for the inflammatory response that is triggered by hypomethylated bacterial DNA12. TLRs also trigger an innate immune response to viruses that produce double-stranded RNA, and a reduced response to the dsRNA analogue polyinosine–polycytidylic acid was observed in Tlr-3-deficient mice13. Recently, Takeuchi et al.14 showed that TLR-1 is involved in the recognition of mycobacterial lipoprotein and triacylated lipopetides. In addition, TLRs can form multimeric complexes (homodimers or heterodimers) to increase the spectrum of molecules that they recognize. For example, the cytoplasmic domain of TLR-2 can form functional pairs with TLR-6 and TLR-1, leading to signal transduction and cytokine expression after ligand activation4.
TLR signal transduction
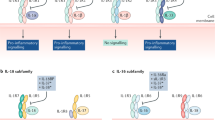
Different TLRs can exert distinct, but overlapping, sets of biological effects, and increasing evidence indicates that this can be attributed to both common and unique aspects of the signalling mechanisms (Fig. 1). TLRs activate signalling pathways that are similar to those engaged by IL-1 because of the presence of the TIR domain. The TIR domain can interact with the adaptor protein MYD88 (Ref. 15), and activation through TIR domains also leads to the activation of the IL-1R-associated kinase (IRAK)15,16, a serine kinase that activates another adaptor molecule; tumour-necrosis factor (TNF)-receptor-associated factor 6 (TRAF6)15,17. Recruitment of TRAF6 leads to the activation of inhibitor of NF-κB (IκB) kinase (IKK). This event frees NUCLEAR FACTOR-κB (NF-κB) from IκB, and allows its nuclear translocation and the subsequent transcriptional activation of many pro-inflammatory genes, which encode cytokines, chemokines, proteins of the complement system, enzymes such as cyclooxygenase-2 (COX-2) and the inducible form of nitric oxide synthase (iNOS), adhesion molecules and immune receptors. All of these molecules are involved in engaging and controlling the innate immune response, which is essential for pathogen elimination, and in orchestrating the transition to an adaptive immune response4.
The Toll-like receptor (TLR)-family members share many signalling components. These include the adaptor MYD88, the Toll-interacting protein (TOLLIP), interleukin (IL)-1-associated kinase (IRAK) and TRAF6 (tumour-necrosis factor (TNF)-receptor-associated factor 6). By contrast, recent evidence indicates that some TLRs might use other receptor-specific signalling components. For example, TLR-4 signals through another adaptor molecule known as MAL or TIRAP (Toll/IL-1 receptor (TIR)-domain-containing adaptor protein) that is not used by other TLRs. Protein kinase R (PKR) functions downstream of TIRAP, but its importance has not been established yet. IκB, inhibitor of NF-κB; NF-κB, nuclear factor-κB; NIK, NF-κB-inducing kinase.
Recently, another molecule, the Toll-interacting protein (TOLLIP), has been proposed to interact with the TIR signalling domains and participate in signal propagation18,19. Another TLR signalling pathway has been revealed by the observation that certain LPS-induced responses do not require MYD88. This MYD88-independent TLR-4 signalling was identified because NF-κB activation was delayed, but not absent, in MYD88-deficient cells, whereas it was completely suppressed in TLR-4-deficient cells20,21. These studies led to the identification of a new molecule known as the TIR-domain-containing adaptor protein (TIRAP, also known as MAL, for MYD88-adaptor-like protein), which interacts specifically with TLR-4 and not with other TLRs and is probably responsible for this MYD88-independent signalling. A biological consequence of this signalling pathway was found by Kaisho and co-workers22, who observed that the LPS-induced maturation of dendritic cells does not require MYD88 but does require TLR-4. These recent findings of differences in relation to the signalling proteins that are used after TLR stimulation could open up possibilities to selectively interfere with specific signalling components that are unique to particular TLR-family members.
TLRs as therapeutic targets in sepsis
Our current understanding of the pathogenesis of sepsis indicates that bacteria and bacterial products activate an uncontrolled network of host-derived mediators, such as pro-inflammatory cytokines, that can lead ultimately to multi-organ failure, cardiovascular collapse and death23,24,25. On the basis of the key role of TLRs in the recognition of microbial components, it is clear that an inappropriate TLR response to bacterial signals could have important consequences during infection, leading to exaggerated responses, such as sepsis23,24. Antagonists for TLR proteins might, therefore, be useful tools to counteract the harmful pro-inflammatory response that is associated with systemic microbial infections. Three basic strategies have been proposed that could reduce signal transduction through TLRs in sepsis26: first, soluble TLRs that bind and neutralize the microbial ligands; second, small molecules or antibodies that block the binding of ligands or protein–ligand complexes to the receptors; and third, specific small-molecular-mass inhibitors of the common signalling pathways that are induced by ligand–TLR interaction.
However, in addition to the potential therapeutic effect of blocking TLRs in sepsis, these receptors have also provided new opportunities to design therapeutics for the treatment of chronic inflammatory diseases or human diseases that are caused by dysregulation of the immune system. The development of TLR agonists or antagonists has the potential to create pharmacological tools to modulate these responses, and some examples of this role are discussed below.
TLRs as therapeutic targets in asthma
How do TLR-driven innate immune processes regulate and control a disease-associated adaptive immune response? Allergic asthma is chosen as an example of a chronic inflammatory disease that has a relatively well-understood adaptive immune response to show how TLR agonists or antagonists might offer possibilities for therapeutic intervention.
The initial acquired immune response that is responsible for the development of allergic diseases such as asthma is the generation of allergen-specific CD4+ TH2 CELLS (Fig. 2). Analysis of blood, bronchoalveolar lavages and bronchial mucosal biopsies from patients with allergic asthma showed a predominant activation of TH2-like T cells that produced IL-4, IL-13 and IL-5, but no IL-2 or interferon-γ (IFN-γ)27,28. IL-4 is required for TH2-cell development and, together with IL-13, is intimately involved in the regulation of IMMUNOGLOBULIN (Ig)E production, which is fundamental to the pathogenesis of allergic asthma29,30. IL-5 is the principal, and possibly the only, TH2 cytokine to be involved in the accumulation of EOSINOPHILS, another characteristic feature of asthma31. Crosslinking of allergen-specific IgE on MAST CELLS and activation of T cells and eosinophils during subsequent encounters with antigens stimulates the release of various preformed and newly synthesized products, including histamine, cytokines and chemokines, which together lead to characteristic airway changes that contribute to obstruction, airway hyperresponsiveness, goblet-cell metaplasia, mucus overproduction and mucosal oedema32,33,34. However, despite the relatively well characterized cellular mechanisms and the introduction of potent and effective drugs, the prevalence, severity and mortality rates of asthma have increased markedly over the past few decades and, so far, no effective preventive measure exists.
T-helper type 2 (TH2)-driven inflammation leads to characteristic airway changes that contribute to airway obstruction, airway hyperresponsiveness and mucus overproduction. Activation of Toll-like receptors (TLRs) by bacteria or bacterial products might shift the predominantly TH2-driven inflammation into a more protective TH1 response, or might lead to the induction of regulatory T cells, which subsequently might prevent the development of allergic asthma. By contrast, activation of TLRs by viruses or bacteria might induce disease exacerbations. APC, antigen-presenting cell; Ig, immunoglobulin; IL, interleukin.
The mechanism that underlies the preferential activation of TH2 cells in allergic asthma is still not known. However, the key event that determines the cytokine phenotype of allergen-specific T cells seems to occur early in life. The current view is that the divergence of pre-existing, foetally primed TH2 immunity towards TH1 fails in ATOPIC individuals, leading instead to the persistence and boosting of foetal TH2 responses after allergen contact35. Indeed, it has been shown that the rate of postnatal maturation of TH1 function is slower in children with a high genetic risk of atopy36. Moreover, it has been proposed that the increase in the incidence of atopic disorders is linked to a decrease in the prevalence of infections that induce TH1 responses early in life. This theory is referred to as the 'hygiene hypothesis', which proposes that the relatively sterile environment in industrialized western countries has contributed to the recent epidemic of asthma and atopy, and that the overall load of infectious agents encountered early in life is an important factor that influences the maturation of the immune system from a TH2 bias at birth towards a predominantly TH1-type response37,38,39. This is supported by recent reports that show a clear relationship between atopy and bacterial infection or antibiotic use40,41,42. It has been shown that certain mycobacterial strains can reduce the formation of specific IgE, eosinophilia and allergen-induced bronchial hyperresponsiveness, and increase IFN-γ production43, which is a powerful suppressor of TH2 activity44. So, exposure to TH1-inducing mycobacterial infections was proposed to cause a shift from TH2 to TH1 immune responses, which would subsequently prevent the development of allergy (Fig. 2). It is reasonable to believe that these bacterial infections are linked closely to the activation of several TLRs, as this family of receptors recognize conserved molecular patterns that are shared by large groups of microorganisms and might therefore have an essential role in the activation of the adaptive immune system. Moreover, the potential role of TLRs in the hygiene hypothesis is supported further by recent findings in Myd88-deficient mice, which showed that a lack of TLR signalling leads to a TH2 response with IgE production by default and no induction of TH1 responses45. However, the existence of PAMPs that are recognized by PRRs other than TLRs that actively stimulate TH2-type responses cannot be ruled out.
In addition to the potentially important role of TLRs in the induction phase of an allergic phenotype, a TLR-driven innate immune response might also have an essential role in disease exacerbations, which are episodes of worsening shortness of breath, coughing, wheezing or chest tightness associated with acute, mild-to-life-threatening airflow limitation. In addition to pollution, the main cause of exacerbations in asthma are viral or bacterial infections46 (Fig. 2). Virus infections are detected in up to 85% of such episodes. Rhinovirus is common in all age groups, whereas respiratory syncytial virus (RSV) is most important in infants and young children47. The innate immune response to the fusion protein of RSV is mediated by TLR-4 and CD14, and it has been shown that RSV persists longer in the lungs of infected Tlr-4-deficient mice than of normal mice48. Bacterial infections are also inducers of asthma exacerbation, and endotoxin is well known for its ability to exacerbate existing allergy and asthma symptoms49. The mechanisms of how viral or bacterial infections induce disease exacerbations are not well understood, but probably include the biased production and effector function of specific cytokines. For example, it has been shown that the exposure of peripheral-blood mononuclear cells from asthmatic individuals to rhinovirus induced a different cytokine pattern, with increased levels of IL-4 and lower levels of IL-12 and IFN-γ, compared with the exposure of cells from normal individuals50. Similarly, it was shown that Escherichia coli LPS — through the activation of TLR-4 — induced abundant IFN-γ, but little or no IL-13, IL-5 or IL-10 in vivo. By contrast, Porphyromonas gingivalis LPS — through the activation of TLR-2 — strongly induced IL-13, IL-5 and IL-10, but resulted in lower levels of IFN-γ, indicating that the production of a cytokine pattern that is compatible with the allergic phenotype might further amplify the underlying inflammatory response and thereby contribute to disease exacerbation51.
TLR-based treatment strategies in asthma
The above described observations associated with the hygiene hypothesis indicate that prospective human vaccines will probably aim to induce strong TH1 responses, leading to the induction of expression of cytokines such as IFN-γ, IL-12 and IL-18, and the induction of allergen-specific tolerance. The most promising approaches to achieve this objective include the induction of systemic or local immune responses through the use of bacterial vaccines, which probably activate several TLRs, or the use of selective TLR-specific ligands, such as CpG oligonucleotides. A different strategy needs to be applied when dealing with exacerbations in asthma, for which the selective induction of a TLR-mediated antiviral response or the blocking of TLR docking sites for viruses or bacteria might be more beneficial.
Bacterial vaccines. Mycobacteria are known to be highly immunostimulatory and, through recognition, uptake and presentation by macrophages and antigen-presenting cells, favour the (at least partly) TLR-dependent stimulation of TH1-type reponses by the production of IL-12 and IFN-γ52,53. The Mycobacterium bovis bacillus Calmette–Guerin (BCG) vaccination has been associated with a reduction in atopic diseases in Japan54. Moreover, BCG inoculation in mice administered 14 days before allergen sensitization reduced the formation of specific IgE in response to allergen, as well as the eosinophilic response and BHR responses, and increased the production of IFN-γ55,56. The application of heat-killed BCG to the lungs of mice inhibited the development of allergen-induced airway eosinophilia for up to two months after treatment57. However, other clinical studies have found no protective effect of BCG vaccination on the development of atopy. The reason for this discrepancy is not clear.
Similar results have been obtained in mice after a single injection of heat-killed Mycobacterium vaccae, another potent inducer of TH1 responses, and Listeria monocytogenes58. Indeed, there is some evidence that the fast-growing M. vaccae, which induces a vigorous cell-mediated immune response and shares several immunodominant epitopes with other mycobacteria, might be a potential candidate for an improved anti-asthma vaccine. Preliminary experiments with heat-killed M. vaccae in adults with asthma and rhinitis or in children with atopic dermatitis showed clinical benefits, as measured by a reduction in the use of rescue medication and severity of disease or inhibition of the allergen-induced, late-phase response59,60. By contrast, however, another study that used lower doses of M. vaccae in asthmatics failed to show any statistically significant beneficial clinical effects61. All patients in this study were prescribed inhaled GLUCOCORTICOSTEROIDS, and it is reasonable to speculate that the effector functions induced by M. vaccae treatment are suppressed by this treatment through antagonizing NF-κB function.
Targeting TLR-4: agonists or antagonists? Human studies have variously reported an association of LPS exposure with an increased risk of asthma-like respiratory symptoms or with a decreased risk of sensitization to aeroallergens62. In this regard, a promoter polymorphism in the human gene that encodes CD14 was found to correlate inversely with IgE levels, as individuals with low levels of IgE had high levels of CD14, and vice versa63. These data indicate that genetic variation in CD14 might modulate the effect that exposure to endotoxins has on the development of TH2 responses. Indeed, other studies have indicated that the CD14 polymorphism might result in the expression of a more severe allergic phenotype64,65. Taken together, these data support the use of TLR-4 agonists, rather than antagonists, for the treatment of asthma. Recently, several compounds, known as aminoacyl glucosaminide phosphates (AGPs), have been developed for monotherapeutic use in manipulating innate-immune mechanisms. These compounds can bind TLR-4 with agonist or antagonist characteristics, depending on the acyl-chain composition of the individual family member66. Several of these AGP TLR-4 agonists have shown pro-inflammatory activity profiles, including the induction of IFN-γ, TNF and IL-12, and activation of cytotoxic T lymphocytes. The ability of these compounds to activate TH1 responsiveness might, therefore, be useful for downregulating or dampening the characteristic TH2 response in atopic diseases such as asthma. By contrast, it has also been reported that allergic airway inflammation and production of IgE were enhanced when LPS was given after sensitization67. Moreover, some of the known disease-exacerbation-inducing stimuli, such as endotoxin or RSV, bind to TLR-4 (Ref. 48). These observations indicate that the development of TLR-4 antagonists might be more beneficial, in particular to prevent or treat episodes of asthma exacerbations.
Targeting TLR-7 and TLR-8. The natural ligands for TLR-7 and TLR-8 are not known. However, synthetic compounds with antiviral activities have now been described as ligands for both receptors68,69. These antiviral imidazoquinoline compounds, imiquimod (R-837) and resiquimod (R-848), are low-molecular-mass immune-response modifiers that can induce the synthesis of IFN-γ and other cytokines in various cell types (Fig. 3). Imiquimod has been used successfully for the local treatment of genital warts caused by human papilloma virus in the clinic. Resiquimod also shows promise for the treatment of genital herpes70. Recently, it has been shown that these compounds probably exert their antiviral properties by activating immune cells through the TLR-7 and TLR-8 signalling pathways. Macrophages from Myd88 or Tlr-7-deficient mice no longer respond to these imidazoquinolines, and both compounds could activate signalling pathways in Tlr-7- or Tlr-8-transfected cell lines68,69. Considering the role of viral infections in disease exacerbations of asthma, TLR-7 or TLR-8 agonists, such as imiquimod or resiquimod, could therefore be extremely valuable for the treatment of these conditions. In addition, the induction of a predominantly TH1-type cytokine profile by these compounds might have further benefits by redirecting the dominant TH2-type response in asthma to a more protective TH1 response.
Targeting TLR-9 by CpG oligonucleotides. Bacterial DNA, but not vertebrate DNA, has a direct immunostimulatory effect on immune cells in vitro71. The immunostimulatory effect is due to the presence of unmethylated CpG dinucleotides, which are under-represented and almost always methylated in vertebrate DNA72. Evidence from the literature shows that bacterial DNA containing unmethylated CpG motifs binds to TLR-9 and has a direct immunomodulatory effect on immune cells. It is well known that CpG DNA can induce the proliferation of almost all B cells and further protects B cells from apoptosis. It also triggers polyclonal immunoglobulin, IL-6 and IL-12 secretion from B cells. In addition to its effects on B cells, CpG DNA also directly activates dendritic cells to secrete IFN-α, IL-6, IL-12, granulocyte–macrophage colony-stimulating factor (GM-CSF), chemokines and TNF. These cytokines stimulate natural killer (NK) cells to secrete IFN-γ73. Overall, CpG DNA induces a TH1-like pattern of cytokine production that is dominated by IL-12 and IFN-γ, with little secretion of TH2 cytokines74. Indeed, treatment of immunized mice with CpG DNA, before or after the airway challenge, redirects the immune response from a TH2-like response towards a TH1-like response, leading to a reversal of established airway eosinophilia and bronchial hyperreactivity. More recently, Tighe et al.75 reported that the chemical conjugation of a CpG oligodeoxynucleotide to the short ragweed allergen Amb resulted in an enhanced immunotherapeutic effect compared with the CpG oligodeoxynucleotide alone. It was also reported that the allergen–CpG conjugate caused less histamine release from basophils than the allergen itself. So, these data indicate that CpG DNA, through activation of TLR-9, might be an effective new method of inducing prophylactic and therapeutic protection against atopic disorders. Furthermore, the combination of enhanced immunogenicity and reduced allergenicity observed for the allergen–CpG conjugate might offer a more effective and safer approach for allergen immunotherapy compared with conventional methods. Although most of the work on CpG DNA has been carried out in mice, it is clear that human cells respond in a similar manner. CpG oligonucleotides are now in clinical trials for various indications, including asthma and allergy, and it will be interesting to see whether the results that have been obtained in animal models can be confirmed in patients with atopic diseases. Moreover, patent applications indicate that several companies are developing TLR-9 agonists76.
In addition to asthma and allergic diseases, therapeutic applications of CpG DNA have been shown for the activation of innate immune defences against infections, as vaccine adjuvants and finally in DNA vaccines. Moreover, the efficacy of CpG DNA in preventing or treating tumour development or metastasis, as well as for tumour immunotherapy, has been shown in several experimental models, extending the potential for TLR-9 agonists far beyond their use in asthma77.
Issues associated with TH1-inducing strategies. Recent advances in our understanding of the hygiene hypothesis indicate that strategies to induce a strong TH1 response might be dangerous. Treatment that pushes responses non-specifically towards a TH1-type response are just as likely to initiate TH1-mediated pathology as to cure the allergy78. Moreover, although the reconstitution of the TH1/TH2 balance by bacterial vaccines is an attractive theory, it is unlikely to explain the whole story, as autoimmune diseases that are characterized by TH1 responses, such as type 1 diabetes, can also benefit from treatment with mycobacteria, and the prevalence of these diseases has increased in parallel with the prevalence of allergies79. This raised the question of whether mycobacteria modulate inflammatory responses through effects on REGULATORY T CELLS, which have been shown to have anti-inflammatory properties80,81. We have shown that treatment of mice with a heat-killed M. vaccae suspension can successfully induce the generation of allergen-specific regulatory T cells that can suppress the allergen-mediated inflammatory response82 (Fig. 2). It is, therefore, no longer reasonable to propose that a lack of exposure to TH1-inducing infectious agents leads to a bias towards TH2 responses. It seems more probable that a general deficiency of regulatory-cell activity is responsible for the increased prevalence of several groups of disease that involve immunodysregulation. However, it still remains to be shown whether activation of TLRs is one of the key elements in the induction of such allergen-specific regulatory T cells.
TLR agonists and antagonists in other diseases
As described for asthma, TLRs provide a mechanism by which exogenously generated signals can markedly affect the initiation, maintenance and progression of inflammatory diseases. This is a logical consequence of Janeway's 'extended self, non-self' theory, which predicts the interaction of the innate and acquired immune responses through the sensing of pathogen-derived motifs83,84. Similar arguments as for asthma can be made for another chronic respiratory disease, chronic obstructive pulmonary disease (COPD), for which LPS and bacterial infections are well known to induce disease exacerbations85, again indicating that TLR-4 or TLR-2 antagonists might have therapeutic benefits. Targeting of TLR-2 and TLR-4 can also be applied to other diseases, as an increased expression of TLR-2 and TLR-4 was observed in intestinal inflammation, indicating that the presence of TLRs might contribute to the inflammatory process observed in gastrointestinal diseases86. Finally, in acne lesions, TLR-2 is expressed on the cell surface of macrophages that surround pilosebaceous follicles, and these macrophages produce inflammatory cytokines after TLR-2 activation by Propionibacterium acnes. As such, TLR-2 could be a new target for the treatment of this common skin disease87.
A more subtle role for PRRs in chronic inflammatory disease is indicated by the role of NOD2 in Crohn's disease, in which polymorphisms in this intracellular LPS receptor lead to increased susceptibility to disease88,89. It has been proposed that NOD2, expressed in intestinal monocytes, acts as a negative regulator of inflammation, sensing the bacterial population of the gastrointestinal tract and possibly producing regulatory cytokines, such as IL-10 (Ref. 90), to dampen inflammatory responses and ensure that the normal commensal state in the gastrointestinal tract is maintained. The polymorphisms are believed to affect the expected signal from NOD2, either by reducing the association with LPS or decreasing the direct interaction of NOD2 with NF-κB88,89. This aberrant signalling stimulates an inflammatory response that leads to chronic inflammation in at least some patients with this disorder. So, PRR signalling can act as a factor to drive responses that occur in many diseases.
The extension of Janeway's original theory to the 'danger' theory of Matzinger91 gives the opportunity to broaden the origin of the stimulating factors. It is now proposed that, in addition to pathogen-derived signals, some of the endogenously released danger signals could interact directly with the PRRs that drive immune responses92. If these molecular danger signals are liberated by internal cellular activity at sites of tissue damage that are associated with inflammatory responses, then it is possible that the PRR-driven aspects of the innate immune response could be activated without pathogenic intervention. This implies that — in chronic diseases — there might be alternative stimuli maintaining or driving the responses that are seen. This hypothesis is dependent on crossreactivity of endogenously generated ligands for the various PRRs that are discussed in the introduction. Only a few endogenous ligands for PRRs have been identified so far. The mannose receptor and the scavenger receptor are good examples of PRRs that recognize exogenous and endogenous ligands. Some of the literature93,94,95,96,97,98,99 indicates that there are examples of endogenous stimulators of the TLRs in mammalian systems, which include HEAT-SHOCK PROTEINS (HSPs) 60 and 70, saturated and unsaturated fatty acids, hyaluronic-acid (HA) fragments, dsDNA, and surfactant protein-A (Table 1).
Role of endogenous TLR ligands. HSPs have a well-described role in stimulating various aspects of the acquired immune response100. Furthermore, theories have been advanced that propose that antibody crossreactivity between microbial and endogenous HSPs might have an important role in many inflammatory or autoimmune diseases101,102. Recent data show that HSPs can stimulate TLRs directly93,94,95, indicating alternative potential roles for these molecules in inflammatory events, with the potential for positive-feedback loops. An example of this inflammatory activation has been described after open-heart surgery103. Patients who undergo coronary-artery bypass grafting (CABG) by cardiopulmonary bypass are known to suffer an inflammatory response104,105. This is typified by the increased expression of HSP70 by myocardial cells106. Through protein-expression profiling, Dybdahl et al.103 showed elevated levels of HSP70 in the circulation of CABG patients. They also showed that expression of TLR-2 and TLR-4 on monocytes increased on days one and two after the operation. In a corresponding set of in vitro experiments, the ability of recombinant HSP70 to stimulate monocytes in a TLR-4/CD14-dependent manner was shown103. These data typify the extent of proof of concept of the endogenous activation of TLRs in inflammatory conditions. However, there are other concerns related to these types of study. In a recent review of HSP activation of the innate immune response, Wallin107 discussed several confounding factors that could influence the conclusions regarding the involvement of TLR-2 and TLR-4 in the process. They specifically discuss the potential for LPS contamination of recombinant protein preparations, the potential for certain HSPs to act as LPS-binding proteins, and that polymyxin B does not neutralize all species of LPS. These are all issues that need to be considered when interpreting the results.
The ability of fatty acids to induce the expression of COX-2 through TLR-4-mediated activation of the NF-κB pathway has been comprehensively reviewed by Hwang108. One of the most interesting points about fatty-acid activation of TLRs is that saturated and unsaturated fatty acids have different properties. Lauric acid, a saturated fatty acid that is structurally similar to the lipid A component that is found in LPS of the Gram-negative bacterium E. coli105, is a strong stimulator of TLR-4 (Ref. 96). By contrast, long-chain, unsaturated fatty acids, such as docosahexaenoic acid, not only fail to stimulate COX-2 induction, but also inhibit LPS-induced COX-2 induction, indicating that such fatty acids might be antagonists of TLR-4-mediated lipid signalling108. These functional differences between the fatty-acid ligands need to be understood with respect to the structure–activity relationships (SARs) that are being developed for LPS binding to TLR-2 and TLR-4. It has been proposed that the conformation of the lipid A component explains which TLR is favoured or even whether the LPS molecule is antagonistic109,110. The above observations set out the potential for endogenously derived fatty acids to modulate inflammatory responses. Perhaps of more significance to disease management is the opportunity to modify inflammatory responses through the provision of exogenous fatty acids or their derivatives in dietary or therapeutic regimens, providing the receptor–ligand SAR can be understood and exploited.
HA is a principal component of the extracellular matrix, which can be degraded at sites of inflammation111,112. Furthermore, the low-molecular-mass products of this degradation are pro-inflammatory and activate macrophages113,114. Termeer et al.97 have extended their previous observations on the maturation of human dendritic cells by HA fragments115 to show that HA fragments act through TLR-4 both in vitro and in vivo.
The synthesis of autoreactive antibodies specific for DNA or the nucleosome is a hallmark of some autoimmune diseases116. It has been shown recently in a mouse model that B cells can be directly stimulated to proliferate in response to immune complexes isolated from the sera of autoimmune mice117. This observation has been refined to show that Myd88−/− animals are unresponsive, indicating that autoimmune serum stimulates a TLR, which was identified as TLR-9 (Ref. 98), the hypomethylated DNA receptor77. Interestingly, this observation, although in an animal model, points to several aspects of autoimmune disease: first, the dual stimulation of the TLR and the B-cell receptor provides a mechanism for direct antigen stimulation of autoreactive B cells118; second, autoantibodies specific for DNA or the nucleosome are a feature of systemic lupus erythematosus (SLE)116; and third, the inhibition of the process by chloroquine (an endosome inhibitor that is assumed to disrupt the presentation of DNA to TLR-9) is mirrored by its use as a therapeutic for the treatment of SLE119.
So, there are data to indicate that HSPs, fatty acids, HA fragments and endogenous DNA can act as endogenous ligands for TLRs, and thereby modulate the inflammatory response by inducing inflammatory mediators108, sensitizing or activating cells such as monocytes103 or dendritic cells97, or stimulating mature immune cells, such as antibody-producing B cells98. The importance of these pathways in specific diseases is unknown, and, therefore, the potential for targeting them in therapeutic interventions has not yet been validated. However, it is reasonable to speculate that more evidence for a role of endogenous TLR ligands in the pathogenesis of autoimmune diseases, transplant rejection and many chronic inflammatory diseases will accumulate in the near future, showing the real potential of TLRs as therapeutic targets in these (chronic) inflammatory diseases.
Conclusion
The discovery of TLRs has provided us with an important insight into the mechanisms whereby the innate immune system senses and responds to pathogens and how an adaptive immune response is controlled. These new insights not only provide a basis for the development of new therapies for diseases such as sepsis, but also offer the potential to develop disease-modifying therapies that result in immune deviation from a TH2-to a TH1-dominated immune response or the induction of regulatory T cells (Table 2). Moreover, reagents that enhance TLR signalling pathways can be powerful adjuvants for fighting pathogens or cancer. More recent data extend the role of TLRs by showing that, in addition to pathogen-derived signals, endogenous ligands, such as surfactant protein-A, HSPs, HA fragments and dsDNA, can activate TLRs. These data indicate that these receptors might also have an important role in the maintenance of the inflammatory process that leads to chronic inflammation. Together with the emerging data on the role of TLRs in chronic inflammation, there are equally fascinating insights to show that molecules that are tractable to the pharmaceutical industry, such as oligonucleotides, fatty acids and imidazoquinolines, can elicit responses at various TLRs. Indeed, the demonstration that low-molecular-mass compounds, such as resiquimod, bind to TLR-7 and TLR-8 and have antiviral and anti-allergic properties, supports the concept that targeting TLRs could offer a promising new therapeutic strategy for the treatment of human inflammatory diseases that are caused by dysregulation of the immune system. However, the potential for adverse effects when targeting such fundamental pathways of the host defence mechanism needs to be carefully assessed, especially for diseases that are not usually life-threatening. Nevertheless, the data that are available at present clearly indicate that, in the near future, it is possible that TLRs will offer validated druggable targets for anti-inflammatory therapeutics.
References
Janeway, C. A. & Medzhitov, R. Innate immune recognition. Annu. Rev. Immunol. 20, 197–216 (2002).
Lemaitre, B., Nicolas, E., Michaut, L., Reichhart, J. M. & Hoffman, J. A. The dorsoventral regulatory gene cassette spatzle/Toll/cactus controls the potent antifugal response in Drosophila adults. Cell 86, 973–983 (1996).
Poltorak, A. et al. Defective LPS signalling in C3H/Hej and C57BL/10ScCr mice: mutations in TLR-4 gene. Science 282, 2085–2088 (1998).The first report to show that mammalian TLRs are involved in host defence.
Medzhitov, R. Toll-like receptors and innate immunity. Nature Immunol. 1, 135–145 (2001).
Imler, J. L. & Hoffmann, J. A. Toll-like receptors in innate immunity. Trends Cell Biol. 11, 304–311 (2001).
Akira, S., Takeda, K. & Kaisho, T. Toll-like receptors: critical proteins linking innate and acquired immunity. Nature Immunol. 2, 675–680 (2001).
Hoshino, K. et al. Cutting edge: Toll-like receptor-4 (TLR-4)-deficient mice are hyporesponsive to lipopolysaccharide: evidence for TLR-4 as the LPS gene product. J. Immunol. 162, 3749–3752 (1999).
Underhill, D. M. & Ozinsky, A. Toll-like receptors: key mediators of microbe detection. Curr. Opin. Immunol. 14, 103–110 (2002).
Wertz, C. et al. Leptospiral lipopolysaccharide activates cells through a TLR-2-dependent mechanism. Nature Immunol. 2, 346–352 (2001).
Hirschfeld, M. et al. Signalling by Toll-like receptor 2 and 4 agonists results in differential gene expression in murine macrophages. Infect. Immun. 69, 1477–1482 (2001).
Hayashi, F. et al. The innate immune response to bacterial flagellin is mediated by Toll-like receptor 5. Nature 410, 1099–1103 (2001).
Hemmi, H. et al. A Toll-like receptor recognises bacterial DNA. Nature 408, 740–745 (2000).This study reports for the first time that bacterial DNA containing unmethylated CpG motifs binds to TLR-9 and has a direct immunomodulatory effect on immune cells in vitro.
Alexopoulou, L., Czopik-Holt, A., Medzhitov, R. & Flavell, R. Recognition of double stranded RNA and activation of NFκB by Toll-like receptor 3. Nature 413, 696–712 (2001).
Takeuchi, O. et al. Cutting edge: role of Toll-like receptor 1 in mediating immune response to microbial lipoproteins. J. Immunol. 169, 10–14 (2002).
Medzhitov, R. et al. MyD88 is an adaptor protein in the hToll/IL-1 receptor family signalling pathways. Mol. Cell 2, 253–258 (1998).
Cao, Z., Henzel, W. J. & Gao, X. IRAK: a kinase associated with the interleukin-1 receptor. Science 271, 1128–1131 (1996).
Cao, Z., Xiong, J., Takeuchi, M., Kurama, T. & Goeddel, D. V. TRAF6 is a signal transducer for interleukin-1. Nature 383, 443–446 (1996).
Bulut, Y., Faure, E., Thomas, L., Equils, O. & Arditi, M. Cooperation of Toll-like receptor 2 and 6 for cellular activation by soluble tuberculosis factor and Borrelia burgdorferi outer surface protein A lipoprotein: role of Toll-interacting protein and IL-1 receptor signaling molecules in Toll-like receptor 2 signaling. J. Immunol. 167, 987–994 (2001).
Fitzgerald, K. A. et al. Mal (MyD88-adapter-like) is required for Toll-like receptor-4 signal transduction. Nature 413, 78–83 (2001).
Kawai, T., Adachi, O., Ogawa, T., Takeda, K. & Akira, S. Unresponsiveness of MyD88-deficient mice to endotoxin. Immunity 11, 115–122 (1999).
O'Neill, L. A. J. Toll-like receptor signal transduction and the tailoring of innate immunity: a role for Mal. Trends Immunol. 23, 296–300 (2002).
Kaisho, T., Takeuchi, O., Kawai, T., Hoshino, K. & Akira, S. Endotoxin-induced maturation of MyD88-deficient dendritic cells. J. Immunol. 166, 5688–5694 (2001).
Gutierrez-Ramos, J. C. & Bluethmann, H. Molecules and mechanisms operating in septic shock: lessons from knockout mice. Immunol. Today 18, 329–334 (1997).
Warren, H. S. Strategies for the treatment of sepsis. New Engl. J. Med. 336, 952–953 (1997).
Knuefermann, P. et al. Cardiac inflammation and innate immunity in septic shock. Is there a role for Toll-like receptors? Chest 121, 1329–1336 (2002).
Opal, S. M. & Huber, C. E. Bench-to-bedside review: Toll-like receptors and their role in septic shock. Crit. Care 6, 125–136 (2002).
Anderson, G. P. & Coyle, A. J. TH2 and TH2-like cells in allergy and asthma: pharmacological perspectives. Trends Pharmacol. Sci. 15, 324–332 (1994).
Robinson, D. R. et al. Predominant TH2-like bronchoalveolar lavage T-lymphocyte population in atopic asthma. New Engl. J. Med. 326, 298–304 (1992).
Corry, D. B. & Kheradmand, F. Induction and regulation of the IgE response. Nature 402, B18–B23 (1999).
Bacharier, L. B. & Geha, R. S. Molecular mechanisms of IgE regulation. J. Allergy Clin. Immunol. 105, S547–S558 (2000).
Sanderson, C. J. IL-5, eosinophils and disease. Blood 79, 3101–3109 (1992).
Bousquet, J., Jeffery, P. K., Busse, W. W., Johnson, M. & Vignola, A. M. Asthma. From bronchoconstriction to airways inflammation and remodeling. Am. J. Respir. Crit. Care Med. 161, 1720–1745 (2000).
Lemanske, R. F. & Busse, W. W. Asthma. JAMA 278, 1855–1873 (1997).
Wills-Karp, M. Immunologic basis of antigen-induced airway hyperresponsiveness. Annu. Rev. Immunol. 17, 255–281 (1999).
Holt, P. G. et al. The role of allergy in the development of asthma. Nature 402, B12–B17 (1999).
Holt, P. G. et al. Genetic risk for atopy is associated with delayed postnatal maturation of T cell competence. Clin. Exp. Allergy 22, 1093–1099 (1992).
Martinez, F. D. & Holt, P. G. Role of microbial burden in aetiology of allergy and asthma. Lancet 354 (Paediatrics Suppl. 2), 12–15 (1999).
Matricardi, P. M. et al. Exposure to foodborne and orofecal microbes versus airborne viruses in relation to atopy and allergic asthma: epidemiologic study. BMJ 320, 412–417 (2000).
Illi, S. et al. Early childhood infectious diseases and the development of asthma up to school age: a birth cohort study. BMJ 322, 390–395 (2001).
Shirakawa, T., Enomoto, T., Shimazu, S. & Hopkin, J. M. The inverse association between tuberculin responses and atopic disorder. Science 275, 77–79 (1997).
von Mutius, E. et al. Frequency of infections and risk of asthma, atopy and airway hyperresponsiveness in children. Eur. Respir. J. 14, 4–11 (1999).
Wickens, K., Pearce, N., Crane, J. & Beasley, R. Antibiotic use in early childhood and the development of asthma. Clin. Exp. Allergy 29, 766–771 (1999).
Erb, K. J., Holloway, J. W., Sobeck, A., Moll, H. & Le Gros, G. Infection of mice with Mycobacterium bovis Bacillus Calmette–Guerin (BCG) suppresses allergen-induced airway eosinophilia. J. Exp. Med. 187, 561–569 (1998).
Gajewski, T. F. & Fitch, F. W. Anti-proliferative effect of IFN-γ in immune regulation: IFN-γ inhibits the proliferation of TH2 but not TH1 murine helper T lymphocyte clones. J. Immunol. 140, 4245–4252 (1988).
Schnare, M. et al. Toll-like receptors control activation of adaptive immune responses. Nature Immunol. 2, 947–950 (2001).This paper shows that in Myd88-deficient mice, the lack of TLR signalling leads to a T H 2 response with IgE production by default, with no induction of a T H 1 response.
Johnston, S. L. Mechanisms of asthma exacerbation. Clin. Exp. Allergy 28, 181–186 (1998).
Message, S. D. & Johnston, S. L. Viruses in asthma. Br. Med. Bull. 61, 29–43 (2002).
Kurt-Jones, E. A. et al. Pattern recognition receptors TLR-4 and CD14 mediate response to respiratory syncytial virus. Nature Immunol. 1, 398–401 (2000).
Holla, A. D., Roy, S. R. & Liu, A. H. Endotoxin, atopy and asthma. Curr. Opin. Allergy Clin. Immunol. 2, 141–145 (2002).
Papadopoulos, N. G., Stanciu, L. A., Papi, A., Holgate, S. T. & Johnston, S. L. A defective type 1 response to rhinovirus in atopic asthma. Thorax 57, 328–332 (2002).
Pulendran, B. et al. Lipopolysaccharides from distinct pathogens induce different classes of immune responses in vivo. J. Immunol. 167, 5067–5076 (2001).
Orme, I. M. et al. Cytokine secretion by CD4+ T lymphocytes aquired in response to Mycobacterium tuberculosis infection. J. Immunol. 151, 518–525 (1993).
von Hertzen, L. C. & Haahtela, T. Could the risk of asthma and atopy be reduced by a vaccine that induces a strong T-helper type 1 response? Am. J. Respir. Cell Mol. Biol. 22, 139–142 (2000).
Shirakawa, T. et al. The inverse association between tuberculin responses and atopic disorder. Science 275, 77–79 (1997).
Erb, K. J. et al. Infection of mice with Mycobacterium bovis Bacillus Calmette–Guerin (BCG) suppresses allergen-induced airway eosinophilia. J. Exp. Med. 187, 561–569 (1998).
Herz, U. et al. BCG infection suppresses allergic sensitisation and development of increased airway reactivity in an animal model. J. Allergy Clin. Immunol. 102, 867–874 (1998).
Wohlleben, G. & Erb, K. L. Atopic disorders: a vaccine around the corner? Trends Immunol. 22, 618–625 (2001).
Wang, C. C. & Rook, G. A. Inhibition of an established allergic response to ovalbumin in Balb/c mice by killed Mycobacterium vaccae. Immunology 93, 307–313 (1998).
Hopkins, J. M. in New Drugs For Asthma, Allergy and COPD (eds Hansel, T. T. & Barnes, P. J.) 226–228 (Karger, Basel, Switzerland, 2001).
Arkwright, P. D. & David, T. J. Intradermal administration of a killed Mycobacterium vaccae suspension (SRL172) is associated with improvement in atopic dermatitis in children with moderate-to-severe disease. J. Allergy Clin. Immunol. 107, 531–534 (2001).
Shirtcliffe, P. M. et al. The effect of delipidated deglycolipidated (DDMV) and heat-killed Mycobacterium vaccae in asthma. Am. J. Respir. Crit. Care Med. 163, 1410–1414 (2001).
Park, J. H., Gold, D. R., Spiegelman, D. L., Burge, H. A. & Milton, D. K. House dust endotoxin and wheeze in the first year of life. Am. J. Respir. Crit. Care Med. 163, 322–328 (2001).
Gereda, J. E. et al. Relation between house dust endotoxin exposure, type 1 T cell development and allergen sensitiation in infants at high risk of asthma. Lancet 355, 1680–1683 (2000).
Vercelli, D. et al. CD14: a bridge between innate immunity and adaptive IgE responses. J. Endotoxin Res. 7, 45–48 (2001).
Koppelman, G. H. et al. Association of a promoter polymorphism of the CD14 gene and atopy. Am. J. Respir. Crit. Care Med. 163, 965–969 (2001).
Persing, D. H. et al. Prophylactic and therapeutic treatment of infectious and other diseases with mono- and disaccharide-based compounds. US Patent Application WO 01/90129 A2/ (2002).
Slater, J. E. et al. Lipopolysaccharide augments IgG and IgE responses of mice to the latex allergen Hev b5. J. Allergy Clin. Immunol. 102, 977–983 (1998).
Hemmi, H. et al. Small anti-viral compounds activate immune cells via the TLR-7 MyD88-dependent signaling pathway. Nature Immunol. 3, 196–200 (2002).The first demonstration of synthetic low-molecular-mass compounds as TLR agonists.
Jurk, M. et al. Human TLR7 or TLR8 independently confer responsiveness to the antiviral compound R-848. Nature Immunol. 3, 499 (2002).
Berman, B. Imiquimod: a new immune response modifier for the treatment of external genital warts and other diseases in dermatology. Int. J. Dermatol. 29, 7–11 (2002).
Tokunaga, T. et al. Antitumor activity of deoxyribonucleic acid fraction from Mycobacterium bovis BCG. I. Isolation, physicochemical characterisation and antitumor activity. J. Natl Cancer Inst. 72, 955–962 (1998).
Davis, H. L. Use of CpG DNA for enhancing specific immune responses. Curr. Top. Microbiol. Immunol. 247, 171–183 (2000).
Klinman, D. M. et al. CpG motifs present in bacteria DNA rapidly induce lymphocyte to secrete IL-6, IL-12, and IFN-γ. Proc. Natl Acad. Sci. USA 93, 2879–2883 (1996).
Krieg, A. M. Mechanisms and applications of immune stimulatory CpG oligodeoxynucleotides. Biochim. Biophys. Acta 1489, 107–116 (1999).
Tighe, H. et al. Conjugation of immunostimulatory DNA to the short ragweed allergen Amb a 1 enhances its immunogenicity and reduces its allergenicity. J. Allergy Clin. Immunol. 106, 124–134 (2000).
Lewis, A. P. & Ray, K. P. Toll-like receptor. US Patent application WO 01/55386 A1 (2001).
Krieg, A. M. CpG motifs in bacterial DNA and their immune effects. Annu. Rev. Immunol. 20, 709–760 (2002).
Wohlleben, G. & Erb, K. J. Atopic disorders: a vaccine around the corner? Trends Immunol. 22, 618–625 (2001).
Martins, T. C. & Aguas, A. P. A role for CD45RB(low) CD38+ T cells and costimulatory pathways of T-cell activation in protection of non-obese diabetic (NOD) mice from diabetes. Immunology 96, 600–605 (1999).
Roncarolo, M. G. & Levings, M. K. The role of different subsets of T regulatory cells in controlling autoimmunity. Curr. Opin. Immunol. 12, 676–683 (2000).
Maloy, K. J. & Powrie, F. Regulatory T cells in the control of immune pathology. Nature Immunol. 2, 816–822 (2001).
Zuany-Amorim, C. et al. Suppression of airway eosinophilia by killed Mycobacterium vaccae-induced allergen-specific regulatory T cells. Nature Med. 8, 625–629 (2002).
Janeway, C. A. Jr. Approaching the asymptote? Evolution and revolution in immunology. Cold Spring Harb. Symp. Quantit. Biol. 54, 1–13 (1989).
Janeway, C. A. Jr. The immune system evolved to discriminate infectious nonself from noninfectious self. Immunol. Today 13, 11–16 (1992).
Wedzicha, J. A. Exacerbations: etiology and pathophysiologic mechanisms. Chest 121, 136S–141S (2002).
Hausmann, M. et al. Toll-like receptors 2 and 4 are up-regulated during intestinal inflammation. Gastroenterology 122, 1987–2000 (2002).
Kim, J. et al. Activation of Toll-like receptor 2 in acne triggers inflammatory cytokine responses. J. Immunol. 169, 1535–1541 (2002).
Hugot, J. P. et al. Association of NOD2 leucine-rich repeat variants with susceptibility to Crohn's disease. Nature 411, 599–603 (2001).
Ogura, Y. et al. A frameshift mutation in NOD2 associated with susceptibility to Crohn's disease. Nature 411, 603–606 (2001).References 88 and 89 show, through genetic-linkage analysis, that the LPS-binding protein NOD2 is associated with susceptibility to Crohn's disease. These data present more evidence for the involvement of PRRs in chronic inflammatory diseases.
Berg, D. J. et al. Enterocolitis and colon cancer in interleukin-10-deficient mice are associated with abberant cytokine production and CD4+ TH1 responses. J. Clin. Invest. 98, 1010–1020 (1996).
Matzinger, P. Tolerance, danger, and the extended family. Annu. Rev. Immunol. 12, 991–1045 (1994).
Matzinger, P. The danger model: a renewed sense of self. Science 296, 301–305 (2002).
Ohashi, K. et al. Cutting edge: heat shock protein 60 is a putative endogenous ligand of the Toll-like-receptor-4 complex. J. Immunol. 164, 558–561 (2000).
Vabulas, R. M. et al. HSP70 as endogenous stimulus of the Toll/interleukin-1 receptor signal pathway. J. Biol. Chem. 277, 15107–15112 (2002).
Asea, A. et al. Novel signal transduction pathway utilised by extracellular HSP70: role of Toll-like receptor (TLR)2 and TLR4. J. Biol. Chem. 277, 15028–15034 (2002).
Lee, J. Y. et al. Saturated fatty acids, but not unsaturated fatty acids, induce the expression of cyclooxygenase-2 mediated through Toll-like receptor 4. J. Biol. Chem. 276, 16683–16689 (2001).
Termeer, C. et al. Oligosaccharides of hyaluronan activate dendritic cells via Toll-like receptor-4. J. Exp. Med. 195, 99–111 (2002).
Leadbetter, E. A. et al. Chromatin–IgG complexes activate B-cells by dual engagement of IgM and Toll-like receptors. Nature 416, 603–607 (2002).An elegant demonstration that — in the mouse — endogenous DNA is presented to B cells by TLR-9. Includes extrapolation and discussion of the relevance of the observation to autoimmune diseases.
Guillot, L. et al. Cutting edge: the immunostimulatory activity of the lung surfactant protein-A involves Toll-like receptor 4. J. Immunol. 168, 5989–5992 (2002).
Singh-Jasuja, H. et al. The role of heat shock proteins and their receptors in the activation of the immune system. Biol. Chem. 382, 629–636 (2001).
Mollenhauer, J. & Schulmeister, A. The humoral immune response to heat shock proteins. Experientia 48, 644–649 (1992).
Schultz, D. R. & Arnold, P. I. Heat shock (stress) proteins and autoimmunity in rheumatic diseases. Semin. Arthritis Rheum. 22, 357–374 (1993).
Dybdahl, B. et al. Inflammatory response after open heart surgery: release of heat-shock protein 70 and signaling through Toll-like receptor-4. Circulation 105, 685–690 (2002).
Kirklin, J. K. et al. Cardiopulmonary bypass: studies on its damaging effects. Blood Purif. 5, 168–178 (1987).
Cremer, J. et al. Systemic inflammatory response syndrome after cardiac operations. Ann. Thorac. Surg. 61, 1714–1720 (1996).
Demidov, O. N. et al. Heat shock proteins in cardiosurgery patients. Eur. J. Cardiothorac. Surg. 16, 444–449 (1999).
Wallin, R. P. Heat-shock proteins as activators of the innate immune system. Trends Immunol. 23, 130–135 (2002).Extensive and critical review of heat-shock proteins and their ability to activate the innate immune response.
Hwang, D. Modulation of the expression of cyclooxygenase-2 by fatty acids mediated through Toll-like receptor 4-derived signaling pathways. FASEB J. 15, 2556–2564 (2001).
Raetz, C. R. Biochemistry of endotoxins. Annu. Rev. Biochem. 59, 129–170 (1990).
Netea, M. G. et al. Does the shape of lipid A determine the interaction of LPS with Toll-like receptors? Trends Immunol. 23, 135–139 (2002).
Agren, U. M. et al. Reactive oxygen species contribute to epidermal hyaluronan catabolism in human skin organ culture. Free Radic. Biol. Med. 23, 996–1001 (1997).
Weigel, P. H. et al. A model for the role of hyaluronic acid and fibrin in the early events during the inflammatory response and wound healing. J. Theor. Biol. 119, 219–234 (1986).
Laurent, T. C. & Fraser, J. R. Hyaluronan. FASEB J. 6, 2397–2404 (1992).
Noble, P. W. et al. Hyaluronan fragments activate an NF-κB/I-κB auto-regulatory loop in murine macrophages. J. Exp. Med. 183, 2373–2378 (1996).
Termeer, C. J. et al. Oligosaccharides of hyaluronan are potent activators of dendritic cells. J. Immunol. 165, 1863–1870 (2000).
Tan, E. Antinuclear antibodies: diagnostic markers for autoimmune diseases and probes for cell biology. Adv. Immunol. 44, 93–151 (1989).
Rifkin, I. R. et al. Immune complexes present in the sera of autoimmune mice activate rheumatoid factor B cells. J. Immunol. 165, 1626–1633 (2000).
Shlomchik, M. J. et al. The role of clonal selection and somatic mutation in autoimmunity. Nature 328, 805–811 (1987).
The Canadian Hydroxychloroqine Study Group. A randomised study on the effect of withdrawing hydroxychloroquine in systemic lupus erythematosus. N. Engl. J. Med. 324, 150–154 (1991).
Author information
Authors and Affiliations
Corresponding author
Related links
Related links
DATABASES
FlyBase
InterPro
LocusLink
OMIM
Glossary
- INNATE IMMUNITY
-
The early response of a host to infections by pathogens, such as bacteria and viruses, before the antigen-specific, adaptive immune response is induced.
- ADAPTIVE IMMUNITY
-
Also known as acquired immunity. Host defence that is mediated by B and T cells after exposure to antigen and which shows specificity, memory and self/non-self recognition.
- LIPOPOLYSACCHARIDE
-
(LPS). A lipopolysaccharide comprises three regions: a branched core oligosaccharide, linked to a lipid component and an O-linked oligosaccharide. The exact composition differs between Gram-negative bacteria. LPS induces an acute inflammatory reaction both in vitro and in vivo.
- DENDRITIC CELL
-
A bone-marrow-derived leukocyte that is specialized for the uptake, transport, processing and presentation of antigens to T cells.
- MACROPHAGE
-
A large, myeloid cell derived from a monocyte in the circulation that functions in phagocytosis, antigen processing and presentation, secretion of cytokines and antibody-dependent, cell-mediated cytotoxicity.
- NEUTROPHIL
-
A circulating granulocyte that can phagocytose pathogens, such as bacteria, and release proteolytic enzymes.
- TH1 CELL
-
A terminally differentiated subclass of T-helper cell that secretes a restricted repertoire of cytokines, including IL-2 and IFN-γ.
- GRAM-NEGATIVE BACTERIA
-
Bacteria that do not retain a basic blue dye during the Gram stain procedure. Their cell walls are thin, consisting of a layer of lipopolysaccharide outside of a peptidoglycan layer.
- GRAM-POSITIVE BACTERIA
-
Bacteria that retain a basic blue dye during the Gram-stain procedure. Their cell wall is thicker than that of Gram-negative bacteria, containing more peptidoglycan.
- PEPTIDOGLYCAN
-
Peptide–saccharide conjugates that are constituents of the bacterial cell wall.
- NUCLEAR FACTOR-κB
-
(NF-κB). A transcription factor that is important for pro-inflammatory and anti-apoptotic responses.
- TH2 CELLS
-
A terminally differentiated subclass of T-helper cells that secretes a restricted repertoire of cytokines, including IL-4, IL-5, IL-9 and IL-13.
- IMMUNOGLOBULIN E (Ig)E
-
A subtype of immunoglobulins that is associated with allergy. Elevated levels are the hallmark of the atopic state. Cells that are activated by allergen-specific IgE to release inflammatory products contribute to allergic diseases, such as asthma, allergic rhinitis and anaphylaxis.
- EOSINOPHIL
-
An allergic effector cell (granulocyte) that is strongly associated with allergic inflammation. Secreted products of eosinophils might contribute to airway obstruction, bronchial hyperresponsiveness and other pathologies in allergic asthma.
- MAST CELLS
-
A type of leukocyte that has large secretory granules that contain histamine and various other preformed protein mediators. Mast cells release these proteins after ligation and crosslinking of allergen-specific IgE bound to high-affinity IgE receptors that are expressed on these cells.
- ATOPY
-
The propensity to develop hypersensitivity reactions, such as asthma, which is strongly linked to TH2 cells and IgE.
- CpG DNA
-
A region of DNA that has patterns of CpG motifs (cytosine–guanine repeats). These motifs can be methylated (on cytosine) — an event that is rare in bacteria — giving rise to hypermethylated CpG regions.
- GLUCOCORTICOSTEROID
-
A natural or synthetic molecule that influences carbohydrate and protein metabolism. An important drug target, as the mechanism also produces an anti-inflammatory effect.
- REGULATORY T CELLS
-
Lymphocytes that can suppress the activity of naive or effector T cells, either by cell–cell contact or by producing cytokines, such as TGF-β or IL-10.
- NOD2
-
An intracellular protein that contains the leucine-rich repeat (LRR) structural element (similar to TLRs) and can bind lipopolysaccharides and regulate NF-κB function.
- HEAT-SHOCK PROTEINS
-
(HSPS). A ubiquitous group of intracellular proteins that have a range of functions; for example, as chaperones. Many HSPs are found in normal cells, and some are induced by stress conditions, such as heat.
Rights and permissions
About this article
Cite this article
Zuany-Amorim, C., Hastewell, J. & Walker, C. Toll-like receptors as potential therapeutic targets for multiple diseases. Nat Rev Drug Discov 1, 797–807 (2002). https://doi.org/10.1038/nrd914
Issue Date:
DOI: https://doi.org/10.1038/nrd914
This article is cited by
-
Prognostic significance of crown-like structures to trastuzumab response in patients with primary invasive HER2 + breast carcinoma
Scientific Reports (2022)
-
A cell-penetrating peptide blocks Toll-like receptor-mediated downstream signaling and ameliorates autoimmune and inflammatory diseases in mice
Experimental & Molecular Medicine (2019)
-
The Traditional Chinese Medicine MLC901 inhibits inflammation processes after focal cerebral ischemia
Scientific Reports (2018)
-
Molecular Cloning, Domain Analysis and Homology Modeling of Toll-Like Receptor 3 from Barilius bendelisis (Ham.)
Proceedings of the National Academy of Sciences, India Section B: Biological Sciences (2017)
-
Integrative analysis of genetic data sets reveals a shared innate immune component in autism spectrum disorder and its co-morbidities
Genome Biology (2016)