Key Points
-
Alzheimer's disease (AD), including both early-onset familial and late-onset senile dementia of the Alzheimer type, accounts for the major proportion of dementia cases and neurodegenerative diseases.
-
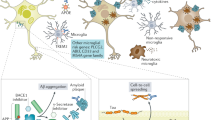
AD is characterized by progressive cognitive, functional and behavioural impairment, evolving into a dramatic loss of most cortical and subcortical functions, and ultimately death. The major pathological hallmarks include amyloid plaques, neurofibrillary tangles and neuronal cell loss.
-
Valid animal models for AD could help to further unravel underlying degenerative processes and discover therapeutic strategies to alleviate and/or prevent this devastating condition. We describe the major rodent models of AD and evaluate their effectiveness for drug discovery research.
-
For a therapeutic intervention to slow down or halt disease progression — that is, to be disease-modifying — it must interfere with a central pathophysiological pathway.
-
Rodent models have acquired a strong position in the evaluation of the preventive and disease-modifying efficacy of potential therapeutics because they rapidly develop symptoms and/or pathology, allow the assessment of large groups of subjects, improve accessibility to early-stage CNS changes and enable time-linked observations.
-
Non-cognitive symptoms represent a major source of physical and psychological caregiver burden often motivating institutionalization of the patient. Animal models mimicking these symptoms are indispensable tools for evaluating new psychopharmacological strategies
-
We empahsize the need for validation of all new models and thorough standardization of procedures, good knowledge of strains, compounds and paradigm characteristics, and skilled personnel.
-
The implementation of a multidisciplinary approach combining valid animal models with new technologies improving biomarker profiling and early diagnosis of dementia subtypes, as well as prediction of patient-specific treatment outcome, will create new paths for improved treatment and prevention of AD.
Abstract
Recent advances in the understanding of the pathophysiological mechanisms underlying Alzheimer's disease have pointed to novel strategies for drug development. Animal models have contributed considerably to these advances, and will have a key role in the evaluation of therapeutics that could have the potential not just to alleviate the dementia associated with Alzheimer's disease, but to modify the disease process. Here, we summarize and critically evaluate current rodent models of dementia, and discuss their role in drug discovery and development.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Wimo, A., Winblad, B., Aguero-Torres, H. & von Strauss, E. The magnitude of dementia occurrence in the world. Alzheimer Dis. Assoc. Dis. 17, 63–67 (2003). Provides a detailed estimate of current and future impact of dementia, based on worldwide demographics and age-dependent prevalence and incidence figures of dementia.
De Deyn, P. P., D'Hooge, R. & van Zutphen, L. F. M. Animal models of human disorders — general aspects. Neurosci. Res. Commun. 26, 141–148 (2000).
Cummings, B. J., Head, E., Ruehl, W., Milgram, N. W. & Cotman, C. W. The canine as an animal model of human aging and dementia. Neurobiol. Aging 17, 259–268 (1996).
Head, E. et al. β-amyloid deposition and tau phosphorylation in clinically characterized aged cats. Neurobiol. Aging 26, 749–763 (2005).
Uchida, K. et al. Senile plaques and other senile changes in the brain of an American black bear. Vet. Pathol. 32, 412–414 (1995).
Braak, H., Braak, E. & Strothjohann, M. Abnormally phosphorylated tau protein related to the formation of neurofibrillary tangles and neuropil threads in the cerebral cortex of sheep and goat. Neurosci. Lett. 171, 1–4 (1994).
Gearing, M., Tigges, J., Mori, H. & Mirra, S. S. β-amyloid (Aβ) deposition in the brains of aged orangutans. Neurobiol. Aging 18, 139–146 (1997).
Gearing, M., Rebeck, G. W., Hyman, B. T., Tigges, J. & Mirra, S. S. Neuropathology and apolipoprotein E profile of aged chimpanzees: implications for Alzheimer's disease. Proc. Natl Acad. Sci. USA 91, 9382–9386 (1994).
Sani, S. et al. Distribution, progression and chemical composition of cortical amyloid-β deposits in aged rhesus monkeys: similarities to the human. Acta Neuropathol. (Berlin) 105, 145–156 (2003).
Erickson, C. A. & Barnes, C. A. The neurobiology of memory changes in normal aging. Exp. Gerontol. 38, 61–69 (2003).
Sherman, K. A. & Friedman, E. Pre- and post-synaptic cholinergic dysfunction in aged rodent brain regions: new findings and an interpretive review. Int. J. Dev.Neurosci. 8, 689–708 (1990).
Butterfield, D. A. & Poon, H. F. The senescence-accelerated prone mouse (SAMP8): a model of age-related cognitive decline with relevance to alterations of the gene expression and protein abnormalities in Alzheimer's disease. Exp. Gerontol. 40, 774–783 (2005).
Ebert, U. & Kirch, W. Scopolamine models of dementia: electroencephalogram findings and cognitive performance. Eur. J. Clin. Invest. 28, 944–949 (1998).
Toledano, A. & Alvarez, M. I. Lesions and dysfunctions of the nucleus basalis as Alzheimer's disease models: general and critical overview and analysis of the long-term changes in several excitotoxic models. Curr. Alzheimer Res. 1, 189–214 (2004).
Gray, J. A. & McNaughton, N. Comparison between the behavioural effects of septal and hippocampal lesions: a review. Neurosci. Biobehav. Rev. 7, 119–188 (1983).
Jarrard, L. E. On the role of the hippocampus in learning and memory in rat. Behav. Neural Biol. 60, 9–26 (1993).
Sloan, H. L., Good, M. & Dunnett, S. B. Double dissociation between hippocampal and prefrontal lesions on an operant delayed matching task and a water maze reference memory task. Behav. Brain Res. 171, 116–126 (2006).
Harkany, T. et al. β-amyloid neurotoxicity is mediated by a glutamate-triggered excitotoxic cascade in rat nucleus basalis. Eur. J. Neurosci. 12, 2735–2745 (2000).
Harkany, T. et al. β-amyloid(Phe(SO3H)24)25–35 in rat nucleus basalis induces behavioral dysfunctions, impairs learning and memory and disrupts cortical cholinergic innervation. Behav. Brain Res. 90, 133–145 (1998).
Yamada, M. et al. Implanted cannula-mediated repetitive administration of Aβ25–35 into the mouse cerebral ventricle effectively impairs spatial working memory. Behav. Brain Res. 164, 139–146 (2005).
Nakamura, S., Murayama, N., Noshita, T., Annoura, H. & Ohno, T. Progressive brain dysfunction following intracerebroventricular infusion of β1–42-amyloid peptide. Brain Res. 912, 128–136 (2001).
Olariu, A., Yamada, K., Mamiya, T., Hefco, V. & Nabeshima, T. Memory impairment induced by chronic intracerebroventricular infusion of β-amyloid (1–40) involves downregulation of protein kinase C. Brain Res. 957, 278–286 (2002).
Nag, S., Yee, B. K. & Tang, F. Reduction in somatostatin and substance P levels and choline acetyltransferase activity in the cortex and hippocampus of the rat after chronic intracerebroventricular infusion of β-amyloid (1–40). Brain Res. Bull. 50, 251–262 (1999).
Vickers, J. C. et al. The cause of neuronal degeneration in Alzheimer's disease. Prog. Neurobiol. 60, 139–165 (2000).
Hauss-Wegrzyniak, B., Dobrzanski, P., Stoehr, J. D. & Wenk, G. L. Chronic neuroinflammation in rats reproduces components of the neurobiology of Alzheimer's disease. Brain Res. 780, 294–303 (1998).
Wenk, G. L., McGann, K., Hauss-Wegrzyniak, B. & Rosi, S. The toxicity of tumor necrosis factor-α upon cholinergic neurons within the nucleus basalis and the role of norepinephrine in the regulation of inflammation: implications for Alzheimer's disease. Neuroscience 121: 719–729 (2003).
Melov, S. Modeling mitochondrial function in aging neurons. Trends Neurosci. 27, 601–606 (2004).
Nitsch, R. & Hoyer, S. Local action of the diabetogenic drug, streptozotocin, on glucose and energy metabolism in rat brain cortex. Neurosci. Lett. 128, 199–202 (1991).
Games, D. et al. Alzheimer-type neuropathology in transgenic mice overexpressing V717F β-amyloid precursor protein. Nature 373, 523–527 (1995).
Hsiao, K. et al. Correlative memory deficits, Aβ elevation, and amyloid plaques in transgenic mice. Science 274, 99–102 (1996).
Stürchler-Pierrat, C. et al. Two amyloid precursor protein transgenic mouse models with Alzheimer disease-like pathology. Proc. Natl Acad. Sci. USA 94, 13287–13292 (1997).
McGowan, E., Eriksen, J. & Hutton, M. A decade of modeling Alzheimer's disease in transgenic mice. Trends Genet. 22, 281–289 (2006).
Huber, G. et al. Characterization of transgenic mice expressing apolipoprotein E4(C112R) and apolipoprotein E4(L28P;C112R). Neuroscience 101, 211–218 (2000).
Freichel, C. et al. Age-dependent cognitive decline and amygdala pathology in α-synuclein transgenic mice. Neurobiol. Aging 2006 July 25 [epub ahead of print].
Andreasson, K. I. et al. Age-dependent cognitive deficits and neuronal apoptosis in cyclooxygenase-2 transgenic mice. J. Neurosci. 21, 8198–8209 (2001).
Capsoni, S. et al. Alzheimer-like neurodegeneration in aged antinerve growth factor transgenic mice. Proc. Natl Acad. Sci. USA 97, 6826–6831 (2000).
Iwata, N. et al. Metabolic regulation of brain Aβ by neprilysin. Science 292, 1550–1552 (2001).
Farris, W. et al. Insulin-degrading enzyme regulates the levels of insulin, amyloid β-protein, and the β-amyloid precursor protein intracellular domain in vivo. Proc. Natl Acad. Sci. USA 100, 4162–4167 (2003).
Götz, J., Schild, A., Hoerndli, F. & Pennanen, L. Amyloid-induced neurofibrillary tangle formation in Alzheimer's disease: insight from transgenic mouse and tissue-culture models. Int. J. Dev.Neurosci. 22, 453–465 (2004).
Perez, M. et al. Accelerated amyloid deposition, neurofibrillary degeneration and neuronal loss in double mutant APP/tau transgenic mice. Neuroscience 130, 339–347 (2005).
Oddo, S., Caccamo, A., Kitazawa, M., Tseng, B. P. & LaFerla, F. M. Amyloid deposition precedes tangle formation in a triple transgenic model of Alzheimer's disease. Neurobiol. Aging 24, 1063–1070 (2003).
Oddo, S. et al. Triple-transgenic model of Alzheimer's disease with plaques and tangles: intracellular Aβ and synaptic dysfunction. Neuron 39, 409–421 (2003)
Janelsins, M. C. et al. Early correlation of microglial activation with enhanced tumor necrosis factor-α and monocyte chemoattractant protein-1 expression specifically within the entorhinal cortex of triple transgenic Alzheimer's disease mice. J. Neuroinflammation 2, 23 (2005).
Billings, L. M., Oddo, S., Green, K. N., McGaugh, J. L. & LaFerla, F. M. Intraneuronal Aβ causes the onset of early Alzheimer's disease-related cognitive deficits in transgenic mice. Neuron 45, 675–688 (2005).
De Deyn, P. P. Dementie: Medisch, Psychosocial, Ethisch en Preventief [In Dutch] (Kluwer, Mechelen, Belgium, 2004).
Sarter, M. Animal cognition: defining the issues. Neurosci. Biobehav. Rev. 28, 645–650 (2004).
Pellow, S. & File, S. E. Anxiolytic and anxiogenic drug effects on exploratory activity in an elevated plus-maze: a novel test of anxiety in the rat. Pharmacol. Biochem. Behav. 24, 525–529 (1986).
Bensadoun, J. C., Brooks, S. P. & Dunnett, S. B. Free operant and discrete trial performance of mice in the nine-hole box apparatus: validation using amphetamine and scopolamine. Psychopharmacology (Berlin). 174, 396–405 (2004).
D'Hooge, R. & De Deyn, P. P. Applications of the Morris water maze in learning and memory. Brain Res. Rev. 36, 60–90 (2001).
Klapdor, K. & van der Staay, F. J. The Morris-water maze task in mice: strain differences and effects of intra-maze contrast and brightness. Physiol. Behav. 60, 1247–1254 (1996).
Van Dam, D., Lenders, G. & De Deyn, P. P. Effect of Morris water maze diameter on visual-spatial learning in different mouse strains. Neurobiol. Learn. Mem. 85, 164–172 (2006).
Wahlsten, D. Standardizing tests of mouse behaviour: Reasons, recommendations, and reality. Physiol. Behav. 73, 695–704 (2001).
Janas, A. M. et al. The cholinesterase inhibitor, phen-serine, improves Morris water maze performance of scop-olamine-treated rats. Life Sci. 76, 1073–1081 (2005).
Crawley, J. N. What's Wrong With My Mouse? Behavioral Phenotyping of Transgenic and Knockout Mice (Wiley-Liss, USA, 2000). Written by an expert in the field, this book provides an excellent introduction to the cognitive and behavioural phenotyping of genetically engineered mouse models.
Tokita, K. et al. FK962, a novel enhancer of somatostatin release, exerts cognitive enhancing actions in rats. Eur. J. Pharmacol. 527, 111–120 (2005).
Stäubli, U., Izreal, Z. & Xu, F. Remembrance of odors past: Enhancement by central facilitation of AMPA receptors. Behav. Neurosci. 110, 1067–1073 (1996).
Patel, N. V. et al. Caloric restriction attenuates Aβ-deposition in Alzheimer transgenic models. Neurobiol. Aging 26, 995–1000 (2005).
De Deyn, P. P. et al. A randomized trial of risperidone, placebo, and haloperidol for behavioral symptoms of dementia. Neurology 53, 899–901 (1999).
De Deyn, P. P., Katz, I. R., Brodathy, H., Lyons, B., Greenspan, A. & Burns, A. Management of agitation, aggression, and psychosis associated with dementia: a pooled analysis including three randomized, placebo-controlled double-blind trials in nursing home residents treated with risperidone. Clin. Neurol. Neurosurg. 107, 497–508 (2005).
Navarro, J. F. & Manzaneque, J. M. Acute and subchronic effects of tiapride on isolation-induced aggression in male mice. Pharmacol. Biochem. Behav. 58, 255–259 (1997).
Chourbaji, S. et al. Learned helplessness: validity and reliability of depressive-like states in mice. Brain Res. Protoc. 16, 70–78 (2005).
Sanchis-Segura, C., Spanagel, R., Henn, F. A. & Vollmayr, B. Reduced sensitivity to sucrose in rats bred for helplessness: a study using the matching law. Behav. Pharmacol. 16, 267–270 (2005).
Gelinas, D. S., DaSilva, K., Fenili, D., St. George-Hyslop, P. & McLaurin, J. Immunotherapy for Alzheimer's disease. Proc. Natl Acad. Sci. USA 101, 14657–14662 (2004).
DeMattos, R. B., Bales, K. R., Cummins, D. J., Dodart, J.-C., Paul, S. M. & Holtzman, D. M. Peripheral anti-Aβ antibody alters CNS and plasma Aβ clearance and decreases brain Aβ burden in a mouse model of Alzheimer's disease. Proc. Natl Acad. Sci. USA 98, 8850–8855 (2001).
Dodart, J.-C. et al. Immunization reverses memory deficits without reducing brain Aβ burden in Alzheimer's disease model. Nature Neurosci. 5, 452–457 (2002).
Chishti, M. A. et al. Early-onset amyloid deposition and cognitive deficits in transgenic mice expressing a double mutant form of amyloid precursor protein 695. J. Biol. Chem. 276, 21562–21570 (2001).
Gervais, F., Garceau, D., Aisen, P. & Gauthier, S. in Alzheimer's Disease and Related Disorders Annual 5 (eds Gauthier, S., Scheltens, P. & Cummings, J.) 63–72 (Taylor & Francis, London, 2005).
Eriksen, J. L. et al. NSAIDs and enantiomers of flurbiprofen target γ-secretase and lower Aβ 42 in vivo. J. Clin. Invest. 112, 440–449 (2003).
Migliore, L. et al. Searching for the role and the most suitable biomarkers of oxidative stress in Alzheimer's disease and in other neurodegenerative diseases. Neurobiol. Aging 26, 587–595 (2005).
Sung, S. et al. Early Vitamin E supplementation in young but not aged mice reduces Aβ levels and amyloid deposition in a transgenic model of Alzheimer's disease. FASEB J. 18, 323–325 (2004).
McGeer, E. G. & McGeer, P. L. Inflammatory processes in Alzheimer's disease. Prog. Neuropsychopharmacol. Biol. Psychiatry 27, 741–749 (2003).
Heneka, M. T. et al. Acute treatment with the PPARγ agonist pioglitazone and ibuprofen reduces glial inflammation and Aβ1–42 levels in APPV717I transgenic mice. Brain 128, 1442–1453 (2005).
Stackman, R. W., Eckenstein, F., Frei, B., Kulhanek, D., Nowlin, J. & Quinn, J. F. Prevention of age-related spatial memory deficits in a transgenic mouse model of Alzheimer's disease by chronic Ginkgo biloba treatment. Exp. Neurol. 184, 510–520 (2003).
Van Dam, D. & De Deyn, P. P. Cognitive evaluation of disease-modifying efficacy of galantamine and memantine in the APP23 model. Eur. Neuropsychopharmacol. 16, 59–69 (2006). This paper proposes a treatment schedule based on a clinical-withdrawal design for the analysis of disease-modifying efficacy in a transgenic mouse model with age-dependent development of cognitive/behavioural alterations.
Van Dam, D., Abramowski, D., Staufenbiel, M. & De Deyn, P. P. Symptomatic effect of donepezil, rivastigmine, galantamine and memantine on cognitive deficits in the APP23 model. Psychopharmacology 180, 177–190 (2005).
Schenk, D. et al. Immunization with amyloid-β attenuates Alzheimer-disease-like pathology in the PDAPP mouse. Nature 400, 173–177 (1999).
Monsonego, A. & Weiner, H. L. Immunotherapeutic approaches to Alzheimer's disease. Science 302, 834–838 (2003).
Furlan, R. et al. Vaccination with amyloid-β peptide induces autoimmune encephalomyelitis in C57/BL6 mice. Brain 126, 285–291 (2003).
Crentsil, V. The pharmacogenomics of Alzheimer's disease. Ageing Res. Rev. 3, 153–169 (2004).
Squire, L. R. & Kandel, E. R. Memory. From mind to molecules. Scientific American Library, New York, United States of America (2000).
Engelborghs, S. et al. Neuropsychiatric symptoms of dementia: cross-sectional analysis from a prospective, longitudinal Belgian study. International Journal of Geriatric Psychiatry. 20, 1028–1037 (2005).
St George-Hyslop, P. H. Molecular genetics of Alzheimer's disease. Biol. Psychiatry 47, 183–199 (2000).
Brunkan, A. L. & Goate, A. M. Presenilin function and γ-secretase activity. J. Neurochem. 93, 769–792 (2005).
Lacor, P. N. et al. Synaptic targeting by Alzheimer's-related amyloid β oligomers. J. Neurosci. 24, 10191–10200 (2004).
Moreira, P. I., Smith, M. A., Zhu, X., Nunomura, A., Castellani, R. J. & Perry, G. Oxidative stress and neurodegeneration. Ann. NY Acad. Sci. 1043, 545–552 (2005).
Smith, M. A., Casadesus, G., Joseph, J. A. & Perry, G. Amyloid-β and tau serve antioxidant functions in the aging and Alzheimer brain. Free Radic. Biol. Med. 33, 1194–1199 (2002).
Akiyama, H. et al. for the Neuroinflammation Working Group. Inflammation and Alzheimer's disease. Neurobiol. Aging 21, 383–421 (2000).
Aisen, P. S. et al. A randomized controlled trial of prednisone in Alzheimer's disease. Alzheimer's disease Cooperative study. Neurology 54, 588–593 (2000).
Van Gool, W. A., Weinstein, H. C., Scheltens, P. & Walstra, G. J. Effect of hydroxychloroquine on progression of dementia in early Alzheimer's disease: an 18-month randomised, double-blind, placebo-controlled study. Lancet 358, 455–460 (2001).
Weggen, S. A subset of NSAIDs lower amyloidogenic Aβ42 independently of cyclooxygenase activity. Nature 414, 212–216 (2001).
Poirier, J. Apolipoprotein E, cholesterol transport and synthesis in sporadic Alzheimer's disease. Neurobiol. Aging 26, 355–361 (2005).
Sparks, D. L., Scheff, S. W., Hunsaker, J. C. 3rd, Liu, H., Landers, T. & Gross, D. R. Induction of Alzheimer-like β-immunoreactivity in the brains of rabbits with dietary cholesterol. Exp. Neurol. 126, 88–94 (1994).
Fassbender, K. et al. Simvastatin strongly reduces levels of Alzheimer's disease β-amyloid peptides Aβ42 and Aβ40 in vitro and in vivo. Proc. Natl Acad. Sci. USA 98, 5856–5861 (2001).
Coleman, P., Federoff, H., Kurlan, R. A focus on the synapse for neuroprotection in Alzheimer disease and other dementias. Neurology 63, 1155–1162 (2004).
Seabrook, T. J., Iglesias, M., Bloom, J. K., Spooner, E. T. & Lemere, C. A. Differences in the immune response to long term Aβ vaccination in C57BL/6 and B6D2F1 mice. Vaccine 22, 4075–4083 (2004).
Van Dam, D., D'Hooge, R., Staufenbiel, M., Van Ginneken, C., Van Meir, F. & De Deyn, P. P. Age-dependent cognitive decline in the APP23 model precedes amyloid deposition. Eur. J. Neurosci. 17, 388–396 (2003).
Acknowledgements
This work was financed by the Fund for Scientific Research–Flanders, Agreement between the University of Antwerp and the Institute Born-Bunge, Neurosearch Antwerp, the Antwerp Medical Research Foundation, and the Thomas Riellaerts Research fund.
Author information
Authors and Affiliations
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Related links
Glossary
- Anomia
-
Impaired recall of words with no impairment of comprehension or the capacity to repeat the words.
- Aphasia
-
Loss or impairment of the ability to produce and/or comprehend language.
- Perseveration
-
Uncontrollable repetition of a particular response — for example, a word, phrase or gesture — despite the absence or cessation of a stimulus.
- Paraphasia
-
The production of unintended syllables, words or phrases during the effort to speak.
- Agnosia
-
Loss of ability to recognize objects, persons, sounds, shapes or smells while the specific sense is not defective.
- Prosopganosia
-
Disorder of face perception with impairment of the ability to recognize faces.
- Apraxia
-
Loss of the ability to execute or carry out learned movements, despite having the desire and the physical capacity to perform the movements.
- Nucleus basalis of Meynert
-
Basal forebrain cholinergic neurons that primarily project to the cerebral cortex and amygdala.
- Early-onset Alzheimer's disease
-
(EOAD). Refers to cases of AD in which disease onset occurs before the age of 65. EOAD represents approximately 5% of all AD cases.
- Cholinomimetic
-
Having an action similar to that of acetylcholine.
- Amyloid-derived diffusible ligands (ADDLs)
-
Soluble Aβ oligomers that directly inhibit long-term potentiation, and therefore synaptic plasticity, and which have been linked to synaptic loss and reversible memory failure in trangenic animal models.
- Disease-modifying therapy
-
Therapy that can slow or halt the progression of a disease by interacting with a central pathophysiological pathway(s).
- Memory consolidation
-
Molecular memory consolidation refers to molecular processes by which long-term conductivity of synapses is affected by training. Network consolidation describes the idea that episodic memories are initially stored in the hippocampus and are slowly moved to the neocortex.
- Procedural memory
-
Refers to the memory for skills and procedures that are often not easily put into words and can be used without conscious recollection (for example, learning to ride a bike or touch typing).
- Declarative memory
-
The aspect of (human) memory that stores facts and events that can be consciously recalled. It includes episodic memory and semantic memory, which refer to the memory of personal events and the memory of facts, meanings and understanding, respectively.
- Theranostics
-
The identification and prediction of specific phenotypic characteristics associated with well-characterized biomarker profiles and monitoring or even prediction of the efficacy of disease-modifying drugs for a specific human condition.
Rights and permissions
About this article
Cite this article
Van Dam, D., De Deyn, P. Drug discovery in dementia: the role of rodent models. Nat Rev Drug Discov 5, 956–970 (2006). https://doi.org/10.1038/nrd2075
Issue Date:
DOI: https://doi.org/10.1038/nrd2075
This article is cited by
-
Characterization of aged male BALB/ccenp mice as a model of dementia
Laboratory Animal Research (2020)
-
The brains of aged mice are characterized by altered tissue diffusion properties and cerebral microbleeds
Journal of Translational Medicine (2020)
-
Tacrine(10)-hupyridone, a dual-binding acetylcholinesterase inhibitor, potently attenuates scopolamine-induced impairments of cognition in mice
Metabolic Brain Disease (2018)
-
Sex hormone-related neurosteroids differentially rescue bioenergetic deficits induced by amyloid-β or hyperphosphorylated tau protein
Cellular and Molecular Life Sciences (2016)
-
Battling Alzheimer’s Disease: Targeting SUMOylation-Mediated Pathways
Neurochemical Research (2016)