Abstract
The management of pericardial diseases is largely empirical because of the relative lack of randomized trials that involve patients with these conditions. A first attempt to bring together and organize current knowledge resulted in the publication of the first guidelines on the management of pericardial diseases. Nevertheless, a number of observational studies and the first randomized trials are moving the management of pericardial diseases towards evidence-based medicine, particularly for pericarditis. Emerging data indicate that management can be tailored to the individual patient and, although the optimal duration of treatment is not clearly established, some recommendations can be formulated to guide management and follow-up.
Key Points
-
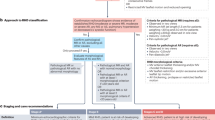
The clinical diagnosis of pericarditis is confirmed when at least two of four clinical criteria are present—typical chest pain, pericardial friction rub, widespread ST-segment elevation, and pericardial effusion
-
Tests for pericarditis include electrocardiography, echocardiography, chest radiography and measurement of markers of inflammation (C-reactive protein, erythrocyte sedimentation rate) and myocardial lesions (troponin); etiology searches and hospitalization are restricted to high-risk patients
-
High-risk features for pericarditis (predictive of nonviral, nonidiopathic etiologies and complications) include fever >38 °C, a subacute course, large pericardial effusion or cardiac tamponade, and failure of aspirin or NSAIDs
-
Pericardiocentesis is indicated for cardiac tamponade, high suspicion of tuberculous, purulent or neoplastic pericarditis and can also be considered for large or symptomatic effusions refractory to medical treatment
-
Pericardial biopsy is indicated in patients with persistent, worsening illness without a definite diagnosis despite medical therapy (diagnostic) and with relapsing tamponade or large effusions with severe symptoms (therapeutic)
-
Pericardiectomy is essentially recommended for persistent constriction; patients with newly diagnosed constriction who are hemodynamically stable can be given a trial of anti-inflammatory therapy for 2–3 months before pericardiectomy
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Shabetai, R. Recurrent pericarditis: recent advances and remaining questions. Circulation 112, 1921–1923 (2005).
Shabetai, R. Corticosteroids for recurrent pericarditis: on the road to evidence-based medicine. Circulation 118, 612–613 (2008).
Sagristá Sauleda, J. et al. The clinical practice guidelines of the Sociedad Espanola de Cardiologia on pericardial pathology [Spanish]. Rev. Esp. Cardiol. 53, 394–412 (2000).
Maisch, B. et al. Guidelines on the diagnosis and management of pericardial diseases executive summary: the task force on the diagnosis and management of pericardial diseases of the European Society of Cardiology. Eur. Heart J. 25, 587–610 (2004).
Imazio, M. et al. Day-hospital treatment of acute pericarditis: a management program for outpatient therapy. J. Am. Coll. Cardiol. 43, 1042–1046 (2004).
Artom, G. et al. Pretreatment with corticosteroids attenuates the efficacy of colchicine in preventing recurrent pericarditis: a multi-center all-case analysis. Eur. Heart J. 26, 723–727 (2005).
Imazio, M. et al. Management, risk factors, and outcomes in recurrent pericarditis. Am. J. Cardiol. 96, 736–739 (2005).
Imazio, M. et al. Colchicine in addition to conventional therapy for acute pericarditis: results of the COlchicine for acute PEricarditis (COPE) trial. Circulation 112, 2012–2016 (2005).
Imazio, M. et al. Colchicine as first choice therapy for recurrent pericarditis: results of the CORE (COlchicine for REcurrent pericarditis) trial. Arch. Intern. Med. 165, 1987–1991 (2005).
Brucato, A. et al. Long-term outcomes in difficult-to-treat patients with recurrent pericarditis. Am. J. Cardiol. 98, 267–271 (2006).
Imazio, M. et al. Indicators of poor prognosis of acute pericarditis. Circulation 115, 2739–2744 (2007).
Imazio, M. et al. Prognosis of idiopathic recurrent pericarditis as determined from previously published reports. Am. J. Cardiol. 100, 1026–1028 (2007).
Permanyer-Miralda, G. Acute pericardial disease: approach to the aetiologic diagnosis. Heart 90, 252–254 (2004).
Imazio, M. & Trinchero, R. Triage and management of acute pericarditis. Int. J. Cardiol. 118, 286–294 (2007).
Spodick, D. H. Risk prediction in pericarditis: who to keep in hospital? Heart 94, 398–399 (2008).
Troughton, R. W., Asher, C. R. & Klein, A. L. Pericarditis. Lancet 363, 717–727 (2004).
Imazio, M. et al. Myopericarditis versus viral or idiopathic acute pericarditis. Heart 94, 498–501 (2008).
Permanyer-Miralda, G., Sagristá- Sauleda, J. & Soler-Soler, J. Primary acute pericardial disease: a prospective series of 231 consecutive patients. Am. J. Cardiol. 56, 623–630 (1985).
Zayas, R. et al. Incidence of specific etiology and role of methods for specific etiologic diagnosis of primary acute pericarditis. Am. J. Cardiol. 75, 378–382 (1995).
Seferovi´c, P. M. et al. Management strategies in pericardial emergencies. Herz. 31, 891–900 (2006).
Mayosi, B. M. Contemporary trends in the epidemiology and management of cardiomyopathy and pericarditis in sub-Saharan Africa. Heart 93, 1176–1183 (2007).
Maisch, B., Risti´c, A. D., Rupp, H. & Spodick, D. H. Pericardial access using the PerDUCER and flexible percutaneous pericardioscopy. Am. J. Cardiol. 88, 1323–1326 (2001).
Seferovi´c, P. M. et al. Diagnostic value of pericardial biopsy: improvement with extensive sampling enabled by pericardioscopy. Circulation 107, 978–983 (2003).
Imazio, M. et al. Aetiological diagnosis in acute and recurrent pericarditis: when and how. J. Cardiovasc. Med. (Hagerstown) 10, 217–230 (2009).
Seidenberg, P. H. & Haynes, J. Pericarditis: diagnosis, management, and return to play. Curr. Sports Med. Rep. 5, 74–79 (2006).
Soler-Soler, J., Sagristà-Sauleda, J. & Permanyer-Miralda, G. Relapsing pericarditis. Heart 90, 1364–1368 (2004).
Imazio, M., Trinchero, R. & Shabetai, R. Pathogenesis, management, and prevention of recurrent pericarditis. J. Cardiovasc. Med. (Hagerstown) 8, 404–410 (2007).
Lange, R. A. & Hillis, D. H. Clinical practice: acute pericarditis. N. Engl. J. Med. 351, 2195–2202 (2004).
Imazio, M. et al. Corticosteroids for recurrent pericarditis: high versus low doses: a nonrandomized observation. Circulation 118, 667–671 (2008).
Marcolongo, R., Russo, R., Laveder, F., Noventa, F. & Agostini, C. Immunosoppressive therapy prevents recurrent pericarditis. J. Am. Coll. Cardiol. 26, 1276–1279 (1995).
Adler, Y. et al. Colchicine for large pericardial effusion. Clin. Cardiol. 21, 143–144 (1998).
Brucato, A., Brambilla, G., Adler, Y. & Spodick, D. H. Colchicine for recurrent acute pericarditis. Arch. Intern. Med. 166, 696 (2006).
Imazio, M., Brucato, A., Trinchero, R., Spodick, D. & Adler, Y. Colchicine for pericarditis: hype or hope? Eur. Heart J. 30, 532–539 (2009).
Maisch, B. Recurrent pericarditis: mysterious or not so mysterious? Eur. Heart J. 26, 631–633 (2005).
Corey, G. R. et al. Etiology of large pericardial effusions. Am. J. Med. 95, 209–213 (1993).
Sagristà-Sauleda, J., Mercé, J., Permanyer-Miralda, G. & Soler-Soler, J. Clinical clues to the causes of large pericardial effusions. Am. J. Med. 109, 95–101 (2000).
Levy, P. Y. et al. Etiologic diagnosis of 204 pericardial effusions. Medicine (Baltimore) 82, 385–391 (2003).
Imazio, M. et al. Relation of acute pericardial disease to malignancy. Am. J. Cardiol. 95, 1393–1394 (2005).
Sagristà-Sauleda, J., Angel, J., Permanyer-Miralda, G. & Soler-Soler, J. Long-term follow-up of idiopathic chronic pericardial effusion. N. Engl. J. Med. 341, 2054–2059 (1999).
Spodick, D. H. The Pericardium: A Comprehensive Textbook (Fundamental and Clinical Cardiology) (Marcel Dekker, New York, 1997).
Little, W. C. & Freeman, G. L. Pericardial disease. Circulation 13, 1622–1632 (2006).
Talreja, D. R. et al. Constrictive pericarditis in 26 patients with histologically normal pericardial thickness. Circulation 108, 1852–1857 (2003).
Sagristà-Sauleda, J., Permanyer-Miralda, G., Candell-Riera, J., Angel, J. & Soler-Soler, J. Transient cardiac constriction: an unrecognized pattern of evolution in effusive acute idiopathic pericarditis. Am. J. Cardiol. 59, 961–966 (1987).
Haley, J. H. et al. Transient constrictive pericarditis: causes and natural history. J. Am. Coll. Cardiol. 43, 271–275 (2004).
Cameron, J., Oesterle, S. N., Baldwin, J. C. & Hancock, E. W. The etiologic spectrum of constrictive pericarditis. Am. Heart J. 113, 354–360 (1987).
Ling, L. H. et al. Constrictive pericarditis in the modern era: evolving clinical spectrum and impact on outcome after pericardiectomy. Circulation 100, 1380–1386 (1999).
Bertog, S. C. et al. Constrictive pericarditis: etiology and cause-specific survival after pericardiectomy. J. Am. Coll. Cardiol. 43, 1445–1452 (2004).
Mayosi, B. M., Burgess, L. J. & Doubell, A. F. Tuberculous pericarditis. Circulation 112, 3608–3616 (2005).
Sagristà-Sauleda, J., Angel, J., Sánchez, A., Permanyer-Miralda, G. & Soler-Soler, J. Effusive-constrictive pericarditis. N. Engl. J. Med. 350, 469–475 (2004).
Hancock, E. W. A clearer view of effusive-constrictive pericarditis. N. Engl. J. Med. 350, 435–437 (2004).
DeValeria, P. A. et al. Current indications, risks, and outcome after pericardiectomy. Ann. Thorac. Surg. 52, 219–224 (1991).
Chowdhury, U. K. et al. Pericardiectomy for constrictive pericarditis: a clinical, echocardiographic, and hemodynamic evaluation of two surgical techniques. Ann. Thorac. Surg. 81, 522–529 (2006).
Clare, G. C. & Troughton, R. W. Management of constrictive pericarditis in the 21st century. Curr. Treat. Options Cardiovasc. Med. 9, 436–442 (2007).
Ha, J. W. et al. Impact of left ventricular function on immediate and long-term outcomes after pericardiectomy in constrictive pericarditis. J. Thorac. Cardiovasc. Surg. 136, 1136–1141 (2008).
Schwefer, M., Aschenbach, R., Heidemann, J., Mey, C. & Lapp, H. Constrictive pericarditis, still a diagnostic challenge: comprehensive review of clinical management. Eur. J. Cardiothorac. Surg. 36, 502–510 (2009).
Halphen, C., Haiat, R., Clément, F. & Michelon, B. Silent pericardial effusion in late pregnancy: echocardiographic detection in the third trimester of pregnancy [French]. J. Gynecol. Obstet. Biol. Reprod. (Paris) 11, 245–248 (1982).
Brucato, A., Imazio, M., Curri, S., Palmieri, G. & Trinchero, R. Medical treatment of pericarditis during pregnancy. Int. J. Cardiol. doi:10.1016/j.ijcard.2009.03.028.
Tsang, T. S. et al. Consecutive 1127 therapeutic echocardiographically guided pericardiocenteses: clinical profile, practice patterns, and outcomes spanning 21 years. Mayo Clin. Proc. 77, 429–436 (2002).
Østensen, M. et al. Anti-inflammatory and immunosuppressive drugs and reproduction. Arthritis Res. Ther. 8, 209 (2006).
American Academy of Pediatrics Committee on Drugs. The transfer of drugs and other chemicals into human milk. Pediatrics 108, 776–789 (2001).
Beitins, I. Z., Bayard, F., Ances, I. G., Kowarski, A. & Migeon, C. J. The transplacental passage of prednisone and prednisolone in pregnancy near term. J. Pediatr. 81, 936–945 (1972).
Acknowledgements
Désirée Lie, University of California, Orange, CA is the author of and is solely responsible for the content of the learning objectives, questions and answers of the MedscapeCME-accredited continuing medical education activity associated with this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Imazio, M., Brucato, A., Trinchero, R. et al. Diagnosis and management of pericardial diseases. Nat Rev Cardiol 6, 743–751 (2009). https://doi.org/10.1038/nrcardio.2009.185
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrcardio.2009.185